Key Points
- ▪
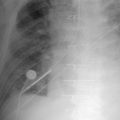
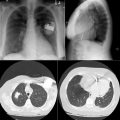
Calcification may occur within numerous structures within the heart and also within the great blood vessels.
- ▪
Greater penetration and optimal “windowing” favor depiction of the calcification. Often the lateral radiograph favors depiction of calcification by avoiding superimposition of the heart onto the spine.
- ▪
The significance of the presence of calcification depends widely depending on the location and cause, as well as other factors. For example, pericardial calcification may or may not be associated with constrictive physiology, whereas myocardial calcification is synonymous with myocardial dysfunction.
Technical Issues
Cardiac and vascular calcifications are always signs of disease and are therefore noteworthy.
Cardiac and vascular calcification is often better appreciated with an overexposed radiograph and is best appreciated when seen on a tangential plane, thus rendering the calcification very dense and therefore visually more obvious. When seen en-face, a layer of calcification is visible at its thinnest and is therefore least apparent. Superimposition of other shadows (the heart itself, or in particular, the spine) often, if not usually, obscures calcification that would be apparent if projected free of other structures. Areas to scrutinize are those with greater likelihood to calcify (the aortic and mitral valves and annuli, the left ventricular walls, the diaphragmatic pericardial surface, and atrioventricular grooves), and those areas where calcification is most readily appreciated.
Sites of Cardiac Calcification
Pericardial Calcification
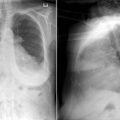
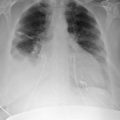
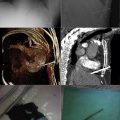
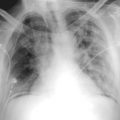
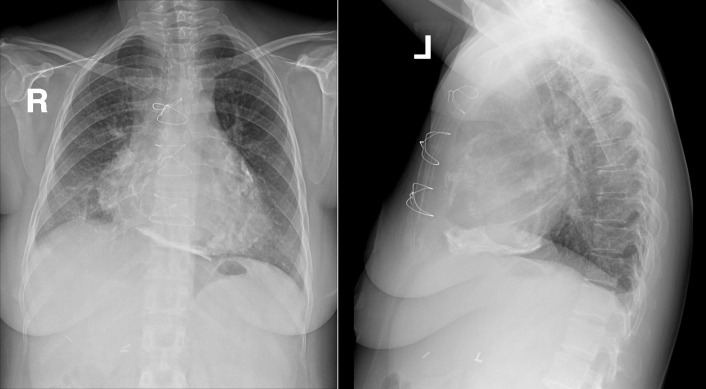
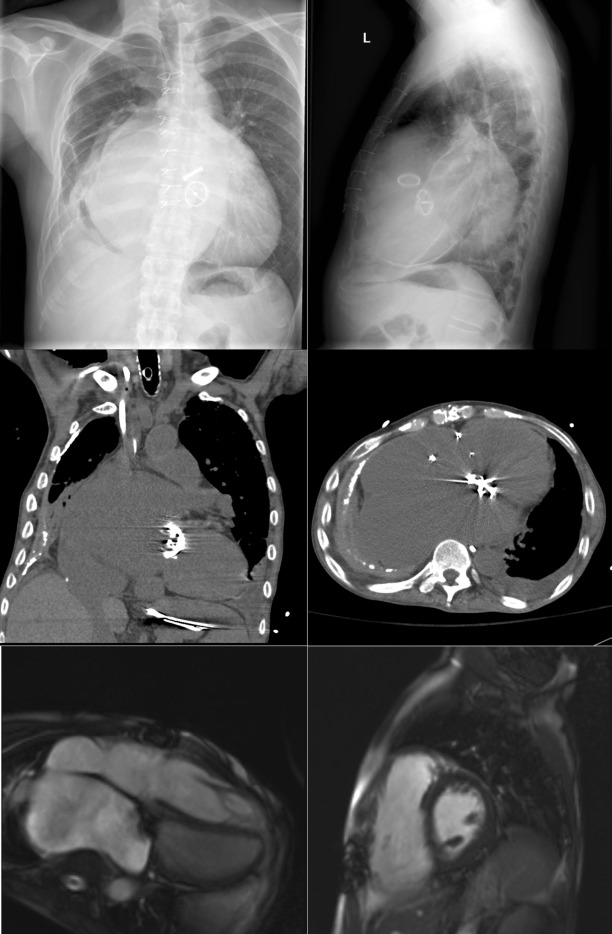
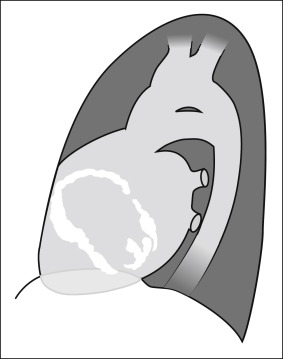
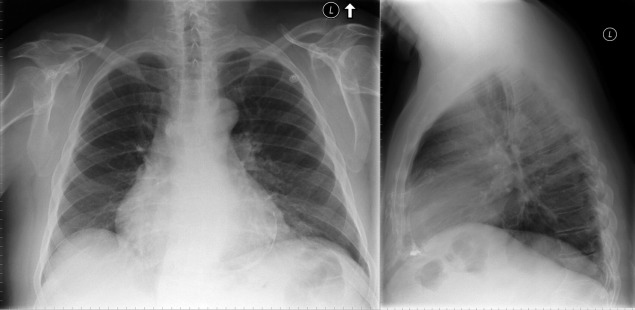
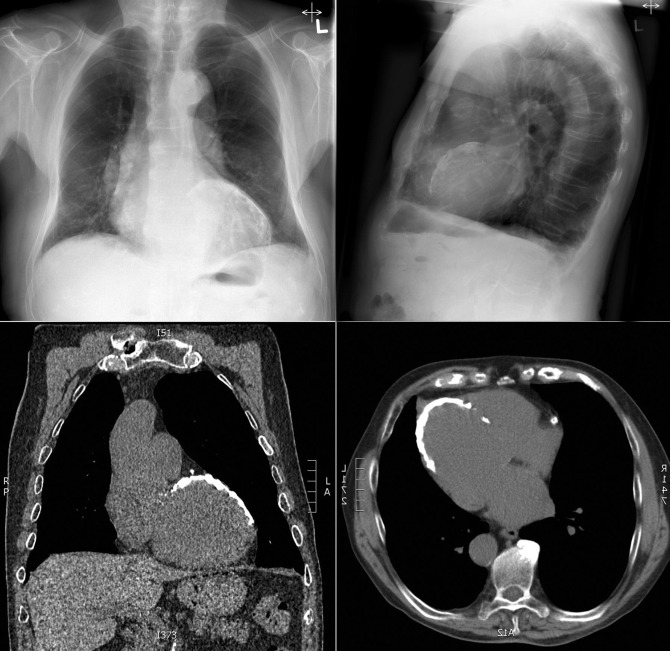
Pericardial calcification ( Figs. 27-1 to 27-4 ) is most prominent in the interventricular and atrioventricular grooves, and lateral to the right atrial and ventricular walls ( Graphic 27-1 ). When looking for pericardial calcification, it is necessary to scrutinize the lateral chest radiograph well, particularly the diaphragmatic surface. Pericardial calcification does not usually involve the left heart as much the right heart, and it does not often involve the apex (which, if calcified, is far more often due to prior infarction). Pericardial calcification should prompt serious consideration of the diagnosis of constrictive pericarditis, and clinicians should seek other radiographic and clinical features of constriction.
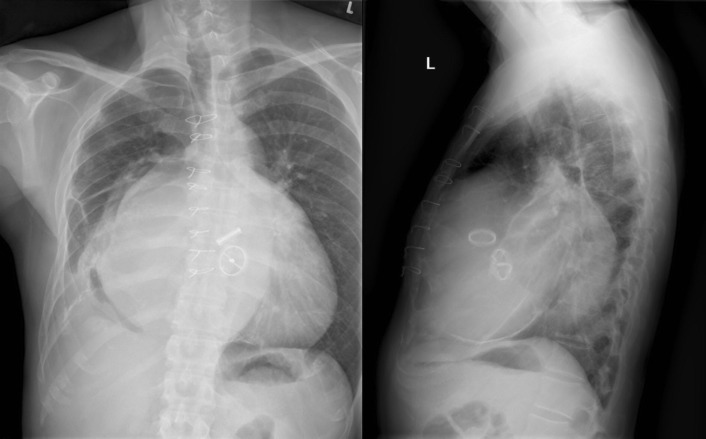
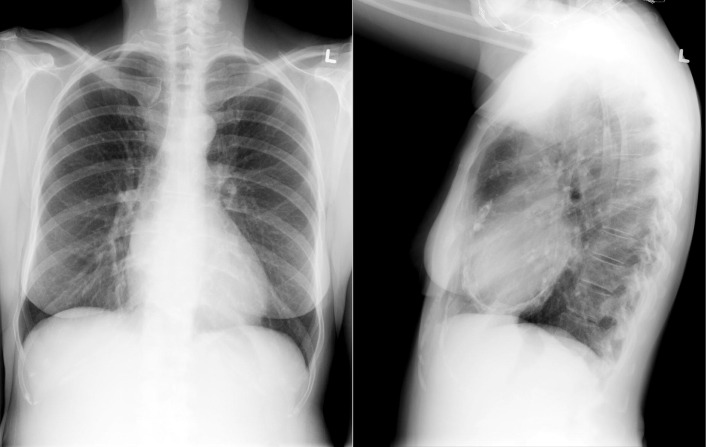
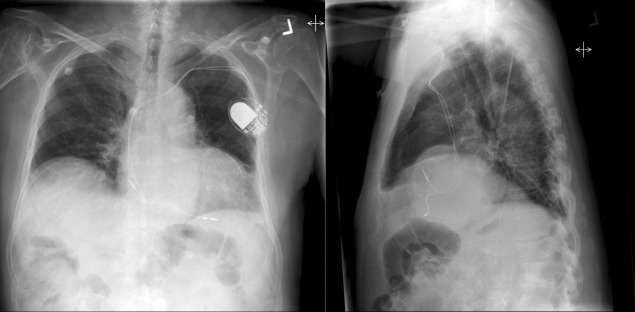
Myocardial Calcification ( Figs. 27-5 to 27-9 )
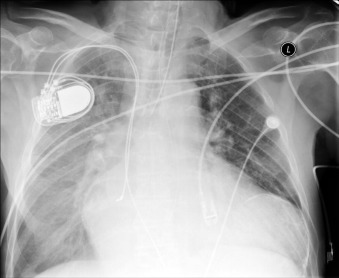
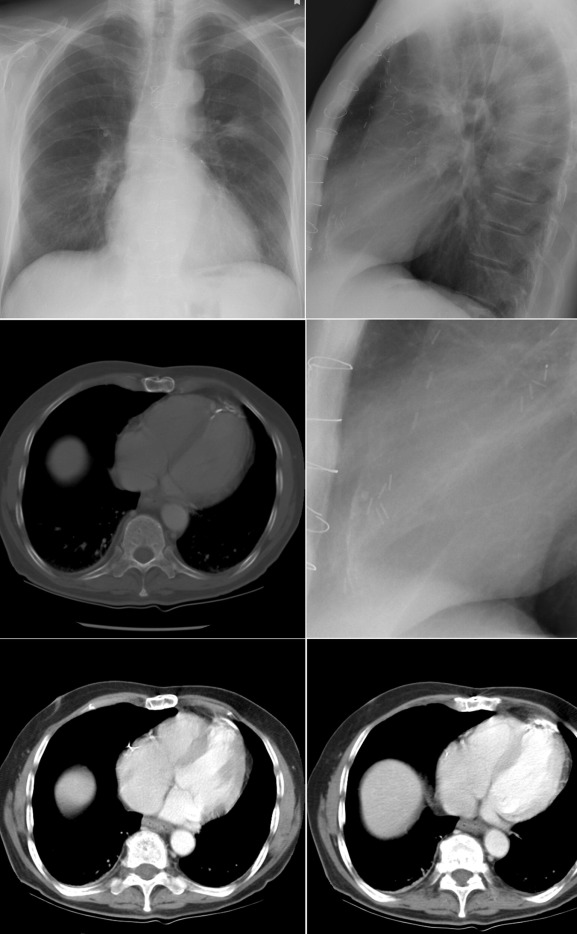
A calcified ventricular aneurysm is seen as a fine dense line when viewed on edge and is consistent with an old transmural infarction. On the frontal chest radiograph, an anterolateral, or apical, calcified aneurysm may be visible. Rarely, a calcified septal aneurysm may be seen on a lateral chest radiograph. Myocardium may calcify following traumatic injury as well as postinfarction.

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree