Ὁ λύχνος τοῦ σώματός ἐστιν ὁ ὀφθαλμός. ἐὰν οὖν ᾖ ὁ ὀφθαλμός σου ἁπλοῦς, ὅλον τὸ σῶμά σου φωτεινὸν ἔσται ἐὰν. δὲ ὁ ὀφθαλμός σου πονηρὸς ᾖ, ὅλον τὸ σῶμά σου σκοτεινὸν ἔσται. εἰ οὖν τὸ φῶς τὸ ἐν σοὶ σκότος ἐστίν, τὸ σκότος πόσον.
Introduction
Both immediate and delayed presentations exist for eye problems in burned patients. Accordingly, in burns, the structure and function of a normal eye can be disrupted by blunt or penetrating injury, electrical current, thermal energy, or chemical agents. After the initial insult, foreign bodies, ongoing chemical injury, deterioration of the facial burn wound, infection, and environmental exposure can cause additional damage or progression of existing pathology. Although many providers may view comprehensive eye examination as an esoterica outside their skill set and purview, the frequency and acuity of sight-threatening complications necessitate that the burn team learn the basics of eye evaluation and management.
Selected anatomy
The organ of sight arises through reciprocal interaction between the optic vesicle (neuroectoderm) and the lens placode (facial ectoderm). The full-thickness neuroectoderm protrudes toward the surface, inducing the primordial lens, and invaginating to form the optic cup. The lens vesicle, separating from the surface ectoderm, induces corneal development. The upper and lower eyelids develop from primordial eyelid folds, fusing transversely from 8 weeks to 5 months, protecting the nascent ocular surface from initial environmental exposure as the fetal urinary system begins to contribute to the amniotic fluid composition. ,
Eyelids are layered structures of skin, orbicularis muscle, tarsus with fibrous septae, and palpebral conjunctiva. Subcutaneous, pre- and postseptal adipose tissues are present. The skin of the eyelids is thin and elastic in the normal state. Upper eyelid skin folds are formed from terminal skin attachments of underlying levator muscle, which functions with Müller’s muscle to open the upper eyelid. The inferior rectus muscle provides analogous function via the capsulopalpebral fascia and inferior tarsus, retracting the lower lid with down-gaze. , The orbicularis muscle can be divided into pretarsal, preseptal, and orbital segments based on the structure they overlie: tarsus, orbital septum, or orbital rim. The pretarsal and preseptal parts are used in blinking and voluntary winking, whereas the orbital segments are used in forced closure; this anatomy has implications for use of botulinum toxin in the treatment of burn scars (discussed later). Orbicularis motor innervation is via the zygomatic and temporal branches of the facial nerve. Epidermal appendages, including follicular sebaceous glands (of Zeiss), modified apocrine sweat glands (of Moll), and eyelashes, are located at the anterior margin of the mucocutaneous junction. Posteriorly, the fibrous tarsi harbor the Meibomian glands (about 50 in the upper lid and 25 in the lower lid) that secrete lipid-rich material into the tear film.
The tear film is a trilaminar structure; moving from the ocular surface externally, there is mucus on the cornea and conjunctiva, covered by an aqueous layer, with a lipid layer most externally. A healthy tear film remains stable for at least 10 seconds and maintains more than 300 μm of meniscus height. The lacrimal gland, located laterally and superiorly in the orbit, produces the aqueous phase of the tear film, along with accessory lacrimal glands (of Krause and Wolfring) located in the superior and inferior fornices. The lipid layer is secreted by the Meibomian glands, stabilizing the tear film and reducing evaporative loss. A complex protein mixture within the tear film confers antimicrobial, inflammatory, and antiinflammatory properties and regulates corneal epithelial cell function.
The conjunctiva covers the inner surface of the eyelids and the anterior sclera, reflecting between the two at the superior and inferior fornices. It is composed of stratified nonkeratinized squamous and columnar cells interspersed with goblet cells upon a continuous basement membrane and lamina propria. Other tissues include accessory lacrimal glands and immune surveillance cells; the lymphatic drainage of the conjunctiva is via the submandibular, parotid, and preauricular nodes. The limbus is the border between the conjunctiva and corneal epithelia. Circumscribing the limbus, the palisades of Vogt harbor the corneal epithelial stem cell niche. ,
The corneal epithelium is approximately six to seven cell layers (50 μm) tall and composed of stratified squamous epithelium with minimal keratinization. The basal layer is mitotically active and replenishes the more external layers as they are continuously sloughed. The corneal epithelial stem cell niche, at the limbus within the palisades of Vogt, allows reepithelialization when the entire basal layer is lost, as in severe burn injuries or toxic epidermal necrolysis. This mechanism requires cell proliferation and migration from the limbus to the center of the cornea and can take weeks to fully reepithelialize the cornea, compared with days when the basal corneal epithelial layer remains intact. The corneal epithelium produces and rests upon a basement membrane. The layers deep to this basement membrane constitute the corneal stroma. The first 8 to 12 μm of stroma is called Bowman’s membrane and is composed of randomly oriented collagen fibers. The stroma is approximately 500 μm (0.5 mm) thick. Precise arrangement of about 200 collagenous lamellae confers transmittance of visible light. Fibroblasts, nerve fibers, and immune surveillance cells populate the stroma. A deep layer, Descemet’s membrane, about 10 μm in thickness, provides posterior structural integrity. Upon this membrane rests the corneal endothelium, rich in mitochondria and nonproliferative, which maintains corneal dehydration (and transparency) via active transport of solute into the aqueous. The cornea provides about two-thirds of the refractive power of a normal eye, approximately +40 diopters.
Examination
Eye examination in a burn intensive care unit requires several modifications from the standard eye clinic setting. Clinicians must adapt to the patient condition and support machinery, which may include multiple intravenous and enteral access lines, ventilator and dialysis support, bulky wound dressings, difficult patient positioning, and, frequently, severe comorbid injuries and burns of the face. This is not the comfort zone for the ophthalmologist, but the frequency and acuity of comorbid eye involvement necessitate adaptation and innovation. An assessment of visual function in each eye can be made with a near vision card, finger counting, or, at a minimum, light perception. Patients with endotracheal tubes can generate various responses, head nod or hand signal, to visual acuity testing under appropriately permissive sedative/analgesic conditions. There are a variety of portable slit lamps that can be employed. Our preference is a handheld lens (20 diopter or panretinal) and penlight. With practice, the penlight may be axially directed through the lens or shone indirectly upon the ocular surface to section through the anterior segment, thereby providing fine detail of stromal and corneal epithelial problems. Loupes provide additive magnification when used with a handheld lens. Topical ocular surface anesthesia is usually employed.
If the injury was associated with an explosion, flying debris, or blunt/penetrating trauma to the eye and periorbita, an open globe injury may be present. In this situation, examination must be performed without pressure on the globe until corneal or scleral perforation can be excluded. Pressure applied to an open globe could cause (further) herniation of intraocular contents and detract from potential recovery. If an open globe-suspect injury is identified, pupillary light response and visual acuity should be grossly documented (at least light perception/hand motion/finger counting), photographs obtained, and a shield placed over the eye sufficient to transmit any applied pressure to the osseous orbital rim rather than the eye and orbital contents. Immediate ophthalmologic consultation is indicated to evaluate a possible open globe.
Once an open globe injury is excluded, cotton swabs, Desmarres retractors, or an eyelid speculum are useful and often necessary because of facial burns and lid edema. Swelling should never be an excuse to defer examination of the ocular surface because it is expected and any delay in the recognition of significant injuries subjects a patient’s visual recovery to avoidable jeopardy. Superficial foreign bodies can usually be removed by saline irrigation alone if identified quickly postburn. Fluorescein dye (strips or solution) should be available in the burn unit and used if there is any suspicion of corneal or conjunctival pathology. The ocular surface should be irrigated to remove any discharge or ointment. A normal healthy cornea should appear clear and glassy with a sharp light reflex. A hazy light reflex can usually be appreciated in early-stage keratopathies. We generally apply dye in a balanced salt solution to the lateral canthus/inferior fornix and then have the patient blink a few times. Next, the eye is opened and examined for epithelial irregularities and negative staining. Excess dye is then rinsed away with balanced salt solution. A normal healthy cornea will wash itself clean and be devoid of stain; dye retention signifies pathology. Areas of confluent, homogeneous stain signify epithelial defect ( Fig. 37.1 C). Lacy staining patterns usually signify epithelial keratopathy (see Fig. 37.1 B). Early-stage epithelial lesions of exposure and herpetic keratopathies are often difficult to appreciate without the assistance of dye. Adjustable-intensity pocket LED flashlights often have fairly cool light, which sufficiently highlights fluorescein; otherwise, a cobalt-blue filter or near-ultraviolet handheld light can be used. Photographs of findings often allow more comprehensive review while minimizing patient discomfort.
Spectrum of exposure-related ocular surface disease encountered in the burn unit. (A) Lagophthalmos and cicatricial ectropion; (B) Exposure keratopathy; (C) Epithelial defect; (D) Herpetic keratitis; (E) Corneal ulcer; (F) Same, with hypopyon; (G) Descemetocele; (H) Corneal perforation.
Indirect ophthalmoscopy via a dilated pupil is occasionally useful and indicated in the burn unit. In cases of nonaccidental trauma, distinctive retinal lesions may be observed and should be documented with fundus photography for potential medicolegal review. In the first 48 to 96 hours after carbon monoxide intoxication, cerebral swelling and herniation syndromes are frequently causes of death. Fundoscopy may show papilledema, which can be graded in severity. In cases where persistently positive blood cultures raise clinical concern for hematogenous seeding, infectious microemboli can occasionally be visualized on thorough funduscopy. Similarly there is a spectrum of retinal findings with disseminated candidiasis, defined as Candida isolated from three or more sites (urine, sputum, mucosa, wound, blood, or eye). Because choroidal blood flow is much higher than retinal blood flow, these hematogenous lesions more frequently occur within the choroid and are initially observed underlying the retinal layers as gray-white round lesions, rather than occlusive lesions within the retinal vessels proper. These lesions, termed chorioretinitis, enlarge as the infection progresses and may erupt into the vitreous. This distinction is important because the stage/level of involvement determines treatment choices (ranging from intravenous antimicrobial therapy, intravitreal antimicrobial instillation, to vitrectomy for significant vitreitis).
Applied pathology
Thermal injuries to the eye concurrent with the burning event are fortunately rare. The typical presentation is flash-type mechanism, decreased vision, eye pain/foreign body sensation, perilimbal hyperemia, and epithelial defect with fluorescein staining. Outside the burn unit, this type of injury is frequently seen in welders without adequate protective equipment. If detected early, a corneal epithelial lesion, analogous to a blister, may be present and is usually translucent to opaque. Upon sloughing, an underlying epithelial defect of varying depth is apparent. In the setting of closed-space (house) fires, it is difficult to determine whether a corneal injury is thermal or (gaseous) chemical in nature, and copious irrigation is recommended. In addition to tissue destruction, eyelid burns compromise the skin barrier function and predispose to burn wound cellulitis and infection. Development of a preseptal inflammatory process (eyelid swelling, hyperemia, and pain) is frequent after eyelid burn injury, and microbiologic cultures help in determining whether this process is sterile or infectious. If infected, it is termed preseptal cellulitis. When observed, it is important to evaluate extraocular muscle mobility and function. If the orbital septum is compromised, an orbital cellulitis or abscess may develop, which can be an eye-threatening emergency. Typical presentation of orbital cellulitis or abscess includes reduced extraocular movements and pain on extraocular muscle testing. Ophthalmologic consultation, systemic antimicrobial therapy, and frequent reexamination are indicated. Surgical drainage and debridement may be needed for orbital abscess.
Chemical eye injuries are a true ophthalmologic emergency. Frequent and copious eye irrigation is generally indicated. Solid chemical particles should be removed by irrigation as rapidly as possible with upper and lower lid eversion and examination. Alkali injuries may need prolonged irrigation, up to several hours. Wound pH can be litmus tested, preferably 2 to 5 minutes after cessation of irrigation as early false-normal results may occur. Insertion of an irrigation aid, such as Morgan lenses, can provide continuous irrigation for several hours; these can also be useful for continuous antibiotic delivery in cases of refractory bacterial keratitis.
Patients with Stevens-Johnson syndrome/toxic epidermal necrolysis (TEN) are treated in the burn unit, and eye involvement is seen in more than 60% of these cases. At worst, they present with complete corneal slough, membranous conjunctivitis, and lash autoepilation (see Fig. 37.1 C). The natural history is scar formation at involved areas, symblepharon, forniceal shortening, corneal opacification/scarring, mucocutaneous junction loss/keratinization, entropion, and chronic, severe, dry-eye symptoms. Mounting evidence indicates that ocular surface recovery may be hastened, with improvement in vision, by prompt coverage of the ocular surface with amniotic membrane. Patients with these conditions should receive definitive treatment at burn units where amniotic membrane transplantation is available and applied immediately when ocular surface involvement is apparent. ,
Electrical injury
As with the systemic response, there are a number of unique ocular aspects of electrical burn injury. Cataract formation after electrical injury has been recognized for more than a half a century. Although the mechanism is not fully understood, within the lens (and other ocular tissues) there is substantial intercellular electrical coupling. These reports note that electrical cataract tends to present within 12 months of the electrical burn event and that visual outcome after cataract extraction can be good in the absence of other eye pathology. Other findings, such as chorioretinal atrophy, are seen less frequently. , For both patient care and medicolegal reasons, electrical injury patients should be evaluated for cataract via dilated exam at admission, discharge, and 6 and 12 months postinjury.
Exposure keratitis and eyelid burns
Eyelid burns and singed eyelashes identify a group of patients at high risk for ocular surface problems, with likelihood ratios (LR+), if present, for the development of corneal ulceration of 12 and 6.9, respectively. Punctate epitheliopathy, or keratopathy, is usually the earliest stage of per se corneal injury, and, if present, it confers an LR+ for the development of corneal ulceration of 6.4. These subtle irregularities on the normally glassy corneal surface can be discerned with magnification and are accentuated by the application of fluorescein dye (see Fig. 37.1 B). The severity of epitheliopathy ranges from scattered, superficial submillimeter dots to a homogeneous area of abnormal epithelium, confluent keratopathy. The latter is essentially an epithelial defect before sloughing of the diseased epithelium. Although keratopathy may be caused by direct thermal or chemical injury of the eye, it is much more frequently observed with corneal exposure resulting from the contraction of eyelid burn wounds and scars. It generally develops around 1 week postburn, and careful observation of the sleeping patient demonstrates incomplete resting eyelid closure, with scleral or corneal show (see Fig. 37.1 A). Any patient with incomplete lid closure, best observed while asleep, should undergo detailed examination of the ocular surface. Bell’s phenomenon, up-gaze with lid closure, is absent in 25% of patients and does not reliably protect the ocular surface when present; however, an intact Bell’s phenomenon may somewhat mitigate the severity of exposure keratopathy.
Epithelial defects
An epithelial defect is present when an area of the cornea has lost epithelium (see Fig. 37.1 C). It is denoted by a subtle ridge where epithelium remains and by a solid area of fluorescein staining. This can be either full or partial thickness. Partial-thickness epithelial defects can heal rapidly from the remaining basal layers, whereas full-thickness injuries must heal by keratinocyte migration from the periphery. Other than observing time to healing/reepithelialization, it is somewhat difficult to otherwise discern the depth/thickness of a corneal epithelial defect. If the basement and Bowman’s membranes are disrupted, keratinocyte migration will be further delayed, and more aggressive eyelid closure techniques (discussed later) should be considered in the interim. Typically the epithelial defect seen from incomplete eyelid closure (exposure) is transverse, linear, and centered over the inferior third of the cornea. Careful daily examination of epithelial defects is required in burn patients, as is correction of underlying causes. If magnified examination reveals stromal opacification (i.e., any finding other than clear cornea at and around the epithelial defect), then a corneal ulcer is present and there is a high risk of vision loss. All indicated diagnostic and therapeutic maneuvers should be employed without delay.
Corneal ulcer
We define a corneal ulcer as an epithelial defect with any associated stromal infiltrate (see Fig. 37.1 E). Corneal transparency, or lack thereof, is an important finding with histopathologic correlates. Transparency is lost when the stroma becomes hydrated. In burns, this is typically in response to injury or infection. This occurs when the keratinocyte basement membrane has been compromised, a process that can develop independent of phagocytic cells via production of active matrix metalloproteinase-9 (MMP-9) and then MMP-2 by corneal cells. The active forms of these enzymes have also been observed in the tear fluid from ocular burn and infectious ulceration patients. Altered capillary permeability and the evolving wound-healing response occur in a manner akin to skin wound healing. This includes phagocytic infiltration, tissue destruction and pathogen clearance, reepithelialization, and myofibroblast-mediated scar formation. The disorganized collagen formed as part of scar formation lacks the regular arrangement and spacing of a healthy, clear corneal stroma. As a result, it appears white or gray and reflects, rather than transmits, visible light, causing vision loss. Transparency can also be lost as a result of corneal endothelial dysfunction. Impaired function of the endothelial adenosine triphosphate (ATP)-dependent transport of solute from the stroma into the aqueous humor causes abnormally increased hydration of stromal proteins. The associated epithelial defect should be measured daily at a minimum on magnified exam because stability (nonenlargement of the defect) followed by reepithelialization (decreasing size of the remaining defect) indicate treatment response. Inhibition of serine proteases may slow epithelial migration, although inhibition of MMPs may actually facilitate reepithelialization. A key point is that the majority of corneal ulcers can be prevented in burned patients via early release and skin grafting of deep partial- and full-thickness eyelid burns. The majority of corneal ulcers in burned patients are sterile, but bacterial superinfection is not uncommon. For this reason, and because treatment of infectious corneal ulcers is aided by the provision of directed antibiotics, swab or scraping culture of corneal ulcers is a routine part of our diagnostic protocol. Corneal scraping is accomplished with ophthalmic tetracaine drops, sedation (usually intravenous ketamine), loupe magnification, adequate lighting, and either a #69 or the rounded belly of a #15 blade. Carefully, the margin of the corneal ulcer is scraped, maintaining the edge of the blade almost parallel to the corneal surface to avoid any penetrating injury. The specimen, often visible only with loupes, is plated on blood and chocolate agars (for the broadest spectrum of bacterial growth), Sabouraud’s agar (for fungal organisms), and several glass slides, for Gram stain (for bacteria), Giemsa stain (for cellular features and viral cytopathic effect), and potassium hydroxide stain (for fungal elements). Rapid review of the slide specimens, if positive, enables immediate initiation of directed topical antimicrobial agents. Initial response to treatment is nonprogression (stabilization) in the size of the epithelial defect and underlying stromal infiltrate. With continued healing, these gradually become smaller. Therefore every follow-up examination should scrupulously document (and/or photograph) the sizes of the epithelial defect and stromal infiltrate.
Bacterial keratitis
Bacterial corneal ulcers can occur in otherwise healthy patients, as with prolonged use of contact lenses, but burned patients are at particular risk because of lost eyelid function, ocular surface exposure, local contamination from colonized/infected skin wounds, and disruption of host immunity, among other factors. Acinetobacter spp. have been reported, as well as Staphylococcus spp. and Pseudomonas spp. , Pathogen virulence factors play important roles in the outcome of these infections, and more virulent bacteria may be selected during the recovery of severely burned patients. Bacterial keratitis typically follows a more fulminant course than sterile corneal ulcers caused by exposure (see Fig. 37.1 F).
Fungal keratitis
Burn patients are at risk for developing secondary infections of persistent exposure-related epithelial lesions. Not infrequently, fungal organisms are isolated as colonizers or active pathogens from burn wounds of the face and eyelids; thus facial wound microbiology determines the risk of secondary infection at ocular surface lesions. We have seen secondary Candida keratitis (ulcer) arising in this manner. Fungal keratitis is typically more indolent and is unresponsive to antibacterial treatment. With magnification, satellite lesions may be observed around the primary lesion. Diagnosis can be made through scraping, potassium hydroxide prep, and fungal culture. A corneal biopsy is rarely necessary to establish the diagnosis if a high clinical suspicion for fungal keratitis exists while cultures remain negative. In refractory cases, debridement and corneal transplant may be necessary.
Viral (herpetic) keratitis
The systemic response to burn injury entails profound alterations in host immunity, including markedly reduced novel immunoglobin generation and adaptive cell-mediated immunity. Type 1 T-helper (T H 1) cellular response, activated macrophage cell killing, is associated with clearance of systemic virus and survival in animal models. Elegant studies by Suzuki et al . demonstrated that, postburn, chemokine CCL2 (a.k.a. monocyte chemoattractant protein-1) stimulates a subset of natural killer T cells to produce interleukin-4, an early signal in a cascade ultimately producing T H 2 cytokines and abolishing the beneficial T H 1 response. This situation leads to increased susceptibility to Herpesviridae. Herpetic keratitis (reactivation) in burned patients is both a sight-threatening problem and a marker of profoundly altered immunity. Dendritic (branching) epithelial defects and stromal infiltrates are typical of herpetic keratopathy (see Fig. 37.1 D). Allowed to progress, these enlarge forming a “geographic” corneal ulcer with an irregular border. Real-time polymerase chain reaction testing of corneal swab specimens is invaluable for diagnosis, providing rapid (within hours) information about the presence and type of Herpesviridae infection. Although tear specimens have also been studied, the diagnostic yield is substantially lower.
Orbital compartment syndrome
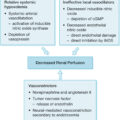
Orbital compartment syndrome (OCS) occurs when the globe is compressed by swelling of the orbital contents and is unable to decompress itself. The natural variation in eyelid laxity provides a variable individual susceptibility to this problem; if the globe is able to move anteriorly to accommodate the swelling, intraocular hypertension may not develop. Acute intraocular hypertension can lead to anterior ischemic optic neuropathy (AION), with loss of vision. In the setting of severe burns, it can rapidly cause complete loss of vision bilaterally. Decreased arterial pressure further compounds the risk of AION infarction. Orbital compartment syndromes are occasionally observed in the first 24 to 96 hours after severe burn injury requiring large-volume resuscitation. The development of compartment syndromes in unburned extremities or abdomen should prompt evaluation of the intraocular pressure; urgency is increased if there is concomitant arterial hypotension. Burns of the face and periorbita can lead to prodigious swelling and OCS in the absence of massive fluid resuscitation. Full-thickness flame burns (charring) and eschar of the periorbital skin can prevent the normal swelling of the underlying tissues, thus facilitating OCS. Intraocular pressure can be evaluated grossly by direct palpation of the globe, by evaluating the mobility of the globe against the lower lid (the globe is tightly pressed against the conjunctival surface of the lower lid in OCS), or more exactly with a Tono-Pen or Schioetz tonometer. Intraocular pressure is sensitive to extrinsic forces, so it is essential that the technique used to open the lids not compress the globe or a falsely elevated intraocular pressure reading may result. Measured at the cornea, intraocular pressures of 20 mm Hg or higher are cause for concern and frequent reevaluation. Avoiding excessive fluid/volume expansion and elevation of the head of the bed can help reduce intraocular pressure. If the globe is hard on palpation, the lower lid is tightly apposed to the globe, or intraocular pressure remains at 30 mm Hg or higher, release of OCS is indicated to preserve vision and prevent AION. The intraocular pressure threshold for release should be somewhat lower when patients have shock with ongoing arterial hypotension because tissue perfusion is a balance between arterial and tissue hydrostatic pressures.
Amblyopia
Amblyopia is concerning in the burn unit primarily when prolonged eyelid closure or near-closure is requisite to treat ocular surface lesions in prepubertal children. Loss of visual stimuli leads to loss of capacity to perceive visual stimuli. Amblyopia presents with decreased visual acuity in the absence of structural or refractive lesions. In practice, it is better to treat both eyes equally (e.g., tarsorrhaphy) if eyelid destruction and ocular surface exposure are present. In cases where vision is unilaterally affected, it is possible to intermittently patch, or treat with cycloplegics, the “good” eye, in an attempt to prevent amblyopia. Involving an ophthalmology consultant is prudent when vision-preserving eyelid procedures raise concerns for iatrogenic amblyopia.
Descemetocele, corneal perforation, and open globe
The posterior 50 μm of corneal stroma is Descemet’s membrane. This posterior layer of corneal stroma, although thin, possesses a high degree of strength. When stromal destruction is near full thickness, the aqueous humor of the anterior chamber may be contained by this structure alone. Termed a descemetocele , it is a sign of an impending corneal perforation (see Fig. 37.1 G). Often an aqueous leak can be appreciated if fluorescein dye is applied over the area; the leaking aqueous humor dilutes and carries the dye into the tear lake (positive Seidel test). Corneal perforations (see Fig. 37.1 H) and lacerations ( Fig. 37.2 ) can be similarly recognized if the aqueous leak is not massive. With a massive loss of aqueous humor, the eye loses intraocular pressure, becoming “flat.” Loss of intraocular pressure, or marked intraocular hypotension below 8 mm Hg, can result in choroidal detachment and loss of retinal function. Early application of tissue adhesive to descemetocele or acute perforation reduces the rate of eventual enucleation. ,
(A) Corneal laceration; (B) Scleral laceration.
Interventions
Topical lubricants provide protection to an at-risk ocular surface. We generally prefer petroleum-based or water-based ointments. The preservative present (a mild chemical toxin) in multidose artificial tear formulations can cause or exacerbate corneal injury if used more frequently than four times a day.
Topical antimicrobials are recommended if clinical findings or confirmatory microbiologic evidence exists of ocular surface infection. For limited burns, erythromycin ointment provides antimicrobial coverage and lubrication. In major burns or with severe associated facial burns, high colony count, not infrequently gram-negative, colonization often occurs of the eyelids and surrounding skin. In these patients, our first-line preference is bacitracin/polymyxin B ointment. We provide empiric coverage of corneal ulcers and significant epithelial defects with quinolone drops (moxifloxacin is preferred but more expensive) while culture data are pending. Fortified antibiotics (vancomycin, ceftazidime, or tobramycin) are used on a case-by-case basis, generally when positive culture data are available or pending, and clinical progression is observed while on empiric treatment. Fungal keratitis occurs infrequently, but, in severe burns, when culture data suggest yeast colonization of facial wounds near the eyes, we provide natamycin prophylaxis. Voriconazole eyedrops can similarly be compounded to fortified antibiotic drops and may be useful in the treatment of documented fungal keratitis. Herpetic keratitis in burned patients is treated with systemic antivirals; topical antivirals (ganciclovir or trifluridine) can be added to more quickly halt the progression of corneal injury. A direct comparison between systemic and topical treatments has not, to our knowledge, been performed in burn patients. Because of altered host immunity discussed earlier, burn patients are in jeopardy of developing disseminated Herpesviridae, and topical monotherapy is not generally employed.
Bandage contact lens
Lenses useful as corneal bandages are characterized by low diopteric power, soft structure, and high gas permeability, and are often labeled extended wear (e.g., Bausch and Lomb Night and Day or Acuvue Oasis). These are occasionally useful in facilitating reepithelialization and protecting corneas damaged by exposure. Once in place, these lenses should be evaluated frequently and discontinued or replaced when no longer effective. Because of risk of infection and other complications, it is prudent to involve an ophthalmology consultant when bandage contact lenses are employed.
Lateral canthotomy
Lateral canthotomy should be performed in cases of OCS, described earlier. Structure is provided to the lids by the canthal tendons, inserting on the upper and lower tarsi medially and laterally. The lateral origin is palpable as a bony prominence at the lateral orbital rim, called Whitnall’s tubercle. Lateral canthotomy is performed by dividing the skin and lateral canthal tendon, freeing the lower lid from its bony attachment. Lidocaine 1% or 2% with epinephrine is infiltrated lateral to the lateral canthus and the skin is clamped parallel to the palpebral fissure, then divided with scissors anteroposteriorly. The lower lid is grasped and pulled away from the globe, placing the lateral canthal tendon on stretch, making it easier to locate and divide. The canthal tendon is divided with scissors anteriorly to Whitnall’s tubercle on the orbital rim. , A successful lateral canthotomy leaves the lower lid freely mobile and no longer apposed to the globe. Afterward, the intraocular pressure should be reevaluated.
Eyelid closure and reconstruction
Because the vast majority of burn-related eye disease results from exposure of the ocular surface, techniques facilitating eyelid closure are of central import. Temporary closure can be accomplished with wound closure strips and cyanoacrylate skin adhesive; this closure may last 24 to 48 hours. Cyanoacrylate adhesive can also be used to temporarily close the lids by joining the lashes and eyelid margins of the lateral parts of lids; in practice, this method of temporary eyelid closure lasts a few days. A temporary suture tarsorrhaphy can be constructed either with bedside sedation and local anesthesia or in the operating room. Tarsorrhaphy increases the rate of corneal epithelial wound healing. , Several techniques have been described; some permit facile reopening and reclosure if frequent eye examination is deemed necessary. Chromic gut sutures often do not require removal and are occasionally used in our practice. A tarsorrhaphy becomes progressively more “permanent” as deepithelialized surfaces of the eyelids are apposed. Several methods exist to create what we term semipermanent tarsorrhaphy; these are indicated when large areas of full-thickness injury to the eyelids necessitate multiple reconstructive operations or after the failure of previous temporary suture tarsorrhaphy. Less durable outcomes are associated with mattress sutures or bolster techniques than an internal fixation technique by which the gray line is split in the region of the planned tarsorrhaphy and the posterior and anterior laminae of the upper and lower lids are sutured to each other. It is vitally important to avoid placing knots in contact with the corneal surface because these can cause abrasion injuries and corneal ulcers.
The forces of scar contraction powerfully influence eyelid function and, when tarsorrhaphy (including temporary) is indicated, often eyelid release and tissue interposition will also be required to preserve sight ( Fig. 37.3 ). Essentially the procedure is a reverse blepharoplasty: the skin and scar of the lid is incised in the tarsal crease, and the upper lid mobilized inferiorly. Overcorrection is needed at the time of surgery because recurrent contraction in 2 to 3 weeks is the rule. The resulting defect can be covered with a split-thickness skin graft and secured with a combination of fibrin glue, sutures, or cyanoacrylate adhesive. If necessary, a secondary procedure is employed for the lower lids, although full-thickness skin autografts may be substituted to close the defect after release. Although release and skin graft interposition may protect a fresh tarsorrhaphy from disruption caused by scar contraction at the eyelids, these grafts eventually contract despite all efforts at preservation. Contraction and recurrence of cicatricial ectropion necessitate a series of repeated releases until both ocular surface and eyelid function stabilize. In cases of massive burns, when eyelid release is required and no sufficient donor site for sheet grafting of the upper lids can be spared, it is possible, despite burned skin, to mobilize the midportion of the brow and upper lid inferiorly from the medial and lateral brow in a myocutaneous V-Y inferior advancement flap, akin to this flap’s utilization in oncologic reconstruction. This procedure may provide the release needed to allow formation of a stable tarsorrhaphy for ocular surface protection in critically injured patients.
(A) Upper eyelid release, grafting, and lateral tarsorrhaphy; (B) Follow-up.
Huang et al. suggest use of local skin flaps, when possible, to overcome the difficulty of autograft contraction and recurrent cicatricial ectropion. The lower lid may be treated with a superomedially based island pedicle flap from the nasolabial fold ( Fig. 37.4 ). This flap is quite durable, and the donor site heals with little morbidity. If burn scar of the skin surrounding the donor site precludes closure, a split-thickness autograft can be used. Flaps available for the upper lid include paramedian forehead flap and orbicularis oculi myocutaneous flap from the lower lid with a laterally based pedicle ( Fig. 37.5 ). , The lower lid donor site defect of the latter may be closed with the previously discussed nasolabial fold island pedicle flap. Occasionally, the tissue destruction resulting from burn injury is so severe that the structural integrity of the tarsal plate is compromised. This leads to lid dysfunction often recalcitrant to the preceding methods of treatment. To address this, tarsal compromise must first be recognized. It can be replaced using suitable cartilage, often harvested from the conchal bowl. Placed in a preseptal location during eyelid contracture release and covered with a skin flap, this technique can be used in cases of subtotal eyelid loss so long as intact palpebral conjunctiva remains. Replacing lost conjunctival tissue is infrequently necessary postburn. This deformity can present with entropion and significant ocular surface injury and is frequently seen after Stevens-Johnson syndrome or TEN. We have successfully employed the technique of preseptal cartilage graft with skin resection (blepharoplasty) to rotate the lash line and scarred/keratinized mucocutaneous junction away from the corneal surface. We have not yet had occasion to resort to conjunctival replacement procedures, such as buccal or nasal mucosal free grafts or nasal septal composite cartilage-mucosa grafts. ,
Cicatricial ectropion of the lower lid; reconstruction with nasolabial island pedicle flap. (A) Flap dissection; (B) Flap inset; (C) Follow-up.
Cicatricial ectropion; reconstruction with myocutaneous orbicularis flap and nasolabial flap. (A) Flap dissection; (B) Flaps inset; (C) Follow-up.
Conjunctival (gundersen) flaps
When corneal ulceration and epithelial loss are catastrophic and refractory to the previously described therapeutic measures, it is possible to mobilize the bulbar conjunctiva over the cornea ( Fig. 37.6 ). These flaps provide a supply of vascularized tissue to create scar, deliver systemic antimicrobial therapy to the wound, and stabilize an impending perforation (e.g., descemetocele). A fornix flap is constructed by suture of the mobile conjunctiva in the inferior and superior fornices. This flap may last 1 to 2 weeks before retracting and does not require any dissection. If small strips of apposing conjunctiva are excised, a more durable fornix flap may be held in place by adhesions similar to those formed via semipermanent tarsorrhaphy. Khodadoust described a microsurgical conjunctival flap, but its placement is more demanding than other options. The classic Gundersen flap mobilizes the superior bulbar conjunctiva over the entire corneal surface, beginning through a transverse incision of the conjunctiva in the superior fornix. After the superior bulbar conjunctival flap is raised, a perilimbal peritomy is performed, the cornea deepithelialized, and the flap brought down over the cornea by securing its inferior edge between the 4 and 7 o’clock positions of the periotomy. , The superior aspect of the flap is sutured to Tenon’s capsule between the 10 and 2 o’clock positions of the peritomy, and the entire superior surface of the globe is left denuded of conjunctiva, which rapidly reepithelializes. This flap is useful if performed with scrupulous avoidance of “buttonholing,” as holes created in the flap invariably expand and allow corneal exposure. The goal of a Gundersen flap is to provide long-term corneal coverage, prevent perforation, and preserve an intact globe for later vision restoration.
Gundersen (conjunctival) flap.
Reconstruction of the lacrimal apparatus
Rarely, burn injury or resulting scarring compromises the normal flow of tears through the lacrimal system. Although a Jones tube or lacrimal stent may be useful in other settings, in the burned patient, scarring and markedly abnormal function of the eyelids combined with discharge caused by chronic conjunctivitis render these tubes prone to clogging. The foreign body may also trigger local infectious complications. Instead we employ a conjunctival mucosal flap to create a fistulous tract for tear drainage. In cases where the punctum and upper lacrimal drainage apparatus are destroyed, this flap can be placed within the lacrimal sac, termed mucosal conjunctivodacryocystostomy. When the upper and lower lacrimal drainage structures are dysfunctional, the mucosal flap can be drained directly into the nasal or maxillary sinus cavities, mucosal conjunctivorhinostomy, and mucosal conjunctivoantrostomy, respectively. Refractory epiphora has been amenable to these treatments in 16 of 17 reported cases.
Corneal transplantation
A stable ocular surface is generally requisite to achieve a successful corneal transplant. , Eyelid malposition must be corrected and epithelial defects and corneal ulcers closed and in a stable, if scarred, state. Corneal neovascularization frequently follows the healing of corneal ulcers. If present, it will increase the risk of corneal allograft rejection, as does the presence of nonnative immune surveillance (Langerhans) cells. Herpetic keratopathy is a further risk factor for rejection. Thus a lamellar graft (partial-thickness corneal allograft) is preferred, because it preserves the patient’s native endothelium from graft rejection. Lamellar grafts are also more tolerant of elevated intraocular pressure, although they can undergo epithelial or stromal rejection. As a salvage procedure, tectonic grafts can be used in the setting of frank perforation or descemetocele. The purpose of these procedures is to maintain a closed globe and intraocular pressure. Amniotic membrane multilayer grafts may be useful as a temporizing measure and may play an antiinflammatory role in decreasing the rate of rejection of allografts placed in an emergent setting. Rarely, destruction of the eyelids, ocular surface, and/or ocular surface may lead to the situation in which the potential for vision exists, but no native reconstructive options exist. These cases may benefit from evaluation by centers experienced in the performance of and postoperative care for keratoprosthesis surgery.
References
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree