The brow and forehead complex is very intriguing, in that it not only conveys the aesthetics of youth and aging but is also essential in communication. The mimetic upper facial muscles and periorbital region convey diverse nonverbal communication. We frequently “talk” with our brows and forehead. Raising the brow can signal a question or surprise; contracting and depressing the brow and forehead can signal aggression or displeasure; raising a single brow can question sincerity, etc. Changing the brow and forehead complex with surgery or neuromodulators can either enhance aesthetics or make a person look unnatural. I believe that fewer browlifts are being performed today because of the over-corrected “deer in the headlights” look seen with so many celebrities. A subtle brow and forehead lift can make a patient look younger and refreshed, while an overdone browlift can look hideous. Patients are aware of this and many are reticent to undergo browlift, as an over-corrected brow is one the worst cosmetic deformities.
The idea that all beautiful women have elevated brows is a fallacy. Look at any fashion or model magazine and you will see beautiful women with elevated brows and low-sitting brows. Not every patient with low brows looks “better” with them elevated. The brow and forehead region thus must be carefully diagnosed in consultation.
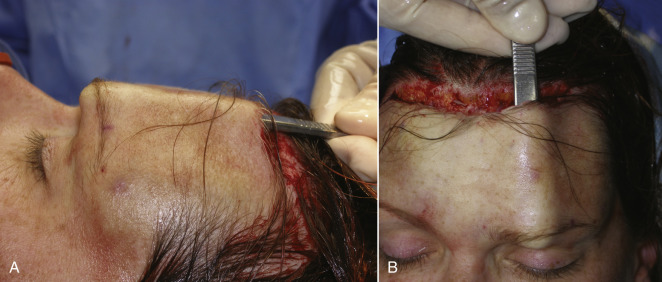
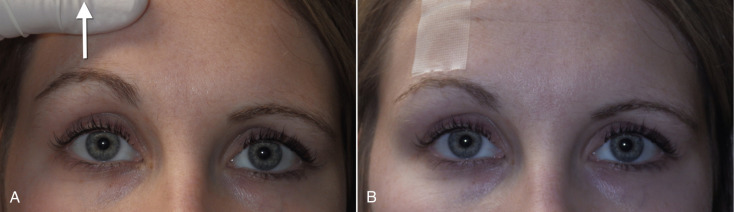
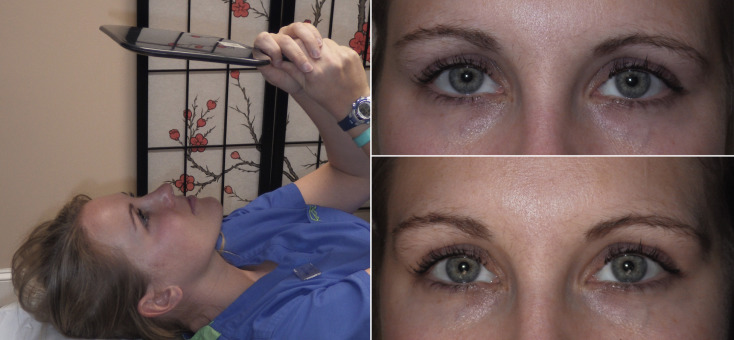
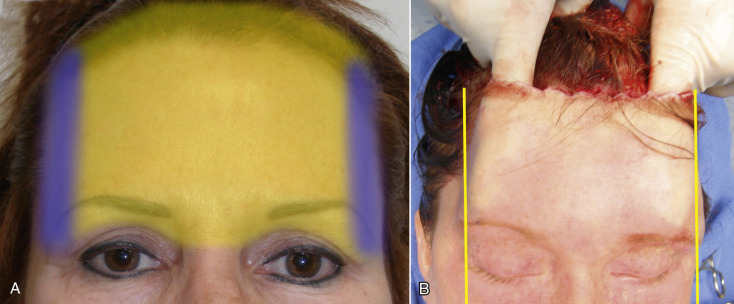
To give the patient (and surgeon) a chairside prediction of the possible result, the brow can be simply elevated with the surgeon’s finger, while the patient looks in the mirror. Using clear tape on the brow and forehead to lift the brow is another way to convey a result ( Fig. 4.1 ). Lying the patient horizontal in a reclining chair will usually serve to position the brows in the position very similar to a natural browlift and is a means of showing the patient an anticipated result ( Fig. 4.2 ). Digital imaging can also be used for prediction.
Whatever method is used to show a patient a possible result, is not as important as the moment when the patient looks in the mirror. In my experience, patients will either say, “Oh my God, I look unnatural, “like a deer in the headlights,” or they will say, “Wow doc, that looks great, that is how I used to look, I love it!” The latter is the response that validates the proposed procedure. In consultation, I lift the patient’s brows and I am honest with them if it looks natural or not. I also involve my staff on this opinion and it is helpful to have the patient’s spouse or significant other present to view the prediction to add their input. Many patients do not have a good understanding of what a browlift does and most conservative patients do not want a browlift. Educating the patient and showing what a result may do is essential. If a patient is undecided about a browlift procedure, then do not perform it. Most browlift techniques are not reversible and this can make a patient very unhappy for a very long time.
During a consultation, it can be impossible to get a female to relax her brows to a neutral position. Experienced surgeons know that if you hand a woman a mirror, 99% of them will automatically raise their brows. This is probably an involuntary learned posture that is gradually adapted with aging and related brow descent. As we age, the forehead, brows, and upper lids become ptotic and it can affect form and function. People may raise their forehead to make their upper-lid complex look younger, or some may do it to improve their visual field. Chronic brow elevation will increase frontalis wrinkling as proof of this habit. On a side note, it is this type of patient that becomes very unhappy with neurotoxin treatment to their forehead, which inactivates the frontalis function. This can produce an inability to raise their brow, hence their upper lids have more redundancy and patients can become very disturbed by this.
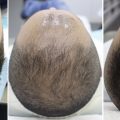
I have performed many female browlifts, but only a handful of male browlifts. I have colleagues who have done many male browlifts, but personally I feel that almost any browlift feminizes male patients and frequently they look unnatural. Also, and perhaps because of my own bald head, I am sensitive to scarring the scalp of males with unstable hairlines.
Brow and Forehead Anatomy
Male brows are usually less peaked and sit at the level of the orbital rim in youth and descend with age. The youthful female brow generally sits above the level of the superior orbital rim ( Fig. 4.3 ).
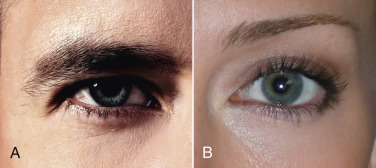
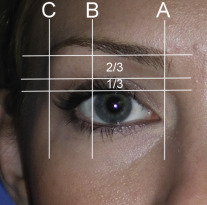
The youthful female brow is a delicate structure that tapers from a thicker and squarer medial portion to a fine point laterally. Classical proportions dictate the tail of the brow tapers at the lateral orbital rim, the peak of the brow at the lateral limbus, and the medial brow at the medical canthus. Classical proportions show the region of the youthful female brow between the lash and the brow to be one-third the distance below the crease and two-thirds the distance above the crease ( Fig. 4.4 ).
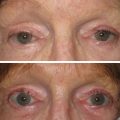
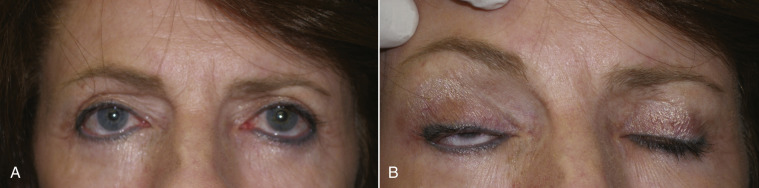
Discussing a browlift procedure with patients is less straightforward. Many patients are browlift candidates but they may still not look natural when the brow is elevated. Similarly, the patient may look very pleasing to the surgeon and staff when the brows are elevated, but the patient may not agree. The bottom line is that the beauty of the browlift is truly in the eye of the beholder. Having said this, it is extremely important and ethical to inform all patients that have ptotic brows that they are candidates for a browlift procedure, whether they desire the procedure or not. This is important because many patients who are browlift candidates undergo aggressive blepharoplasty without ever being counseled about the possibility of brow and forehead lift. Every year I see a number of patients that have ptotic brows and desire browlift, but unfortunately they have had several upper-lid blepharoplasties without ever being offered the option of browlift and, now, a browlift is impossible as the patient would not be able to close their eyelids due to the previous aggressive removal of upper-eyelid skin ( Fig. 4.5 ). This not only robs the patient of contemporary rejuvenation but may be grounds for a lawsuit from previous misdiagnosis. The take home message here is that if a patient has ptotic eyelids or an aging forehead, they need to be offered the option of brow and forehead lift. If the diagnosing surgeon does not possess that skillset, then ethics dictate referring the patient to a surgeon proficient in brow and forehead lift.
Numerous factors dissuade patients from brow and forehead lift. These include a misunderstanding of the procedure, failure of the surgeon to discuss the procedure, fear of an unnatural appearance, and finances. The optimum policy is to discuss browlift and blepharoplasty with all appropriate patients and document this information in the medical record.
In addition to actually elevating the brow, a brow and forehead lift can improve horizontal forehead rhytids (depending on the type of lift performed), open up the eye/orbit complex, giving a more alert and youthful appearance, improve lateral brow hooding that blepharoplasty does not address, and lift and thin glabellar ptosis and fullness seen with aging.
Types of Browlifts
Elevating the ptotic brow and forehead complex is an important part of cosmetic facial surgery and a plethora of techniques has been described. As with many cosmetic procedures, there is no right and wrong technique and the best procedure is the one that produces natural and long-lasting results with low complications and happy patients. Some patients are very pleased with a 2-mm brow elevation from neurotoxin and nonsurgical skin tightening devices. My practice, on the other hand, is surgical and my patients expect and demand more dramatic results. The happy patient with a 2-mm brow from the office next door, might demand a refund for such a small result at my office. In my experience, the commonest type of browlift being performed today is endoscopic, with conservative open procedures running a close second. I know very few surgeons that still perform classic coronal brow and forehead lift.
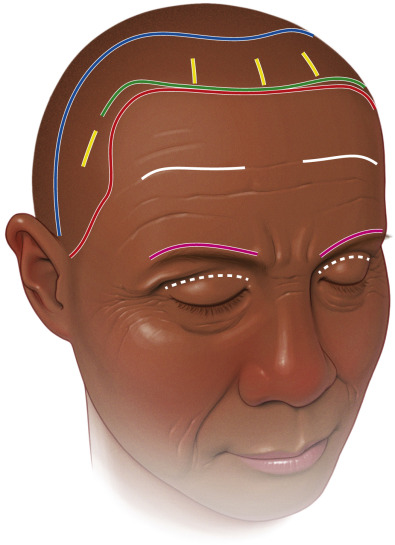
The coronal browlift is an aggressive open technique that utilizes a trauma-type incision from ear to ear across the scalp. Coronal browlifting was once the most popular technique but has fallen out of popularity owing to drawbacks, such as over-elevated hairline, hair loss, nerve damage, and the sheer aggressiveness of the procedure. It is simply too aggressive and the scar and related problems can be significant. Some of the more common approaches for coronal lift are shown in Fig. 4.6 .
Conservative browlifts are described in all shapes and forms in the literature and involve remote small incisions in the hairline and attempt to raise the brow with these tiny skin excisions and or with suture suspension through the incision. Although these lifts come in and out of favor, they are not known for their efficacy or longevity.
Direct browlifts are performed by removing a horizontal ellipse of forehead skin at some position above the eyebrow. Basically, the surgeon is taking a pleat out of the forehead and sewing the edges back, which lifts the brow. Although moderately effective, they do not address the entire forehead and leave noticeable scars. Older patients with deep horizontal wrinkles may tolerate such a scar.
Transblepharoplasty browlift involves performing routine upper-lid blepharoplasty and attempting to suspend the eyebrow to the periosteum to raise it. Although this remains popular with some surgeons, it does not have a great track record for efficacy or longevity. More recently, this approach has been modified with resorbable plastic tine devices that are anchored in the skull and support the elevated brow. This, I feel, fails to address the entire brow and forehead.
Suture suspension browlifting has wafted in and out of popularity for almost 30 years. It is a technique that appeals to non-surgeons, as it is simple to perform. It involves securing the brow with a suture and suspending it higher on the forehead or using barbed sutures to suspend the brows. This is one of the least effective procedures in cosmetic surgery and I do not perform it. The “thread lift” craze of the early 2000s was met with extremely disappointing results.
Laser skin resurfacing brow and forehead lifts are promoted by some doctors. When aggressive laser or chemical peeling is performed on the forehead, the skin tightens and can elevate the brow, but the net result and longevity cannot compare with a surgical browlift. Radiofrequency, ultrasonic, and other noninvasive devices are also used to tighten the forehead skin to raise the brow but produce clinically minor results compared with surgery.
Injectable filler browlifts are performed by some doctors and can be effective for minimal improvement of brow aesthetics (see Chapter 10 ). Filler is injected in multiplanes beneath the eyebrow and the effect is more of a projection than a lift. When done properly by an experienced injector, it can improve brow aesthetics, but only produces a minor change.
Although the endoscopic brow and forehead lift (EBFL) is a high-tech procedure, there are numerous disadvantages to the technique. First of all, it requires a good deal of expensive and specialized equipment, including camera, light source, monitor, along with significant hand instrumentation. Second, there is a steep learning curve for competency. Just because something is new, does not mean it is better. Many surgeons feel that EBFL is not a stable procedure and is more prone to relapse. I have personally seen more postoperative change with this technique than I have with my transfollicular technique. When any surgeon reviews, studies, analyzes, or criticizes someone else’s technique, it is very important to be open-minded. If a given surgeon is using a different technique with safe and repeatable, long-lasting outcomes and happy patients, then their technique can be validated, even if it may not be effective in the hands of other surgeons. I do still perform endoscopic brow and forehead lift in my practice. As with many procedures, I may feel a certain technique is better suited for a given patient, or a patient may request a given approach. In reality, there are numerous techniques that I use for multiple operations and they all basically have the same safe and predictable outcome, or I would not use them. It is important for the reader to understand that when I endorse or downplay any procedure, it is based not only on my personal experience, but also I try to take into account the basic “gestalt” of the contemporary multispecialty cosmetic surgery community.
Transfollicular Subcutaneous Brow and Forehead Lift
Transfollicular Subcutaneous Procedure
The transfollicular subcutaneous browlift has become my “go-to” procedure and the biggest reason is simplicity. It only requires several instruments, does not necessitate cameras or scopes, is a direct vision technique, is more stable because skin is removed, and it DOES NOT raise the hairline. This section is devoted to the transfollicular subcutaneous brow and forehead lift (TFSBFL), which I also refer to as the “mini open browlift.”
A discussion of terminology plays an important role in understanding (or misunderstanding) surgical procedures. Incisions made in front of hair follicles are termed trichophylic (hair-loving) or pretrichial (in front of the follicles) because the follicles are not disturbed. Incisions that transect intact hair follicles (transfollicular) have been termed trichophytic , tricho meaning “hair” and phytic either from the Greek phynai , “to be born,” or phyein , “to produce.” I have seen these terms misquoted, misused, and used interchangeably in articles, textbooks, and lectures. This browlift uses an incision that transects the hair follicles and for accuracy will henceforth be referred to as the “transfollicular approach.” Since this lift is performed in the subcutaneous plane, the formal name is the “transfollicular subcutaneous brow and forehead lift” or TFSBFL.
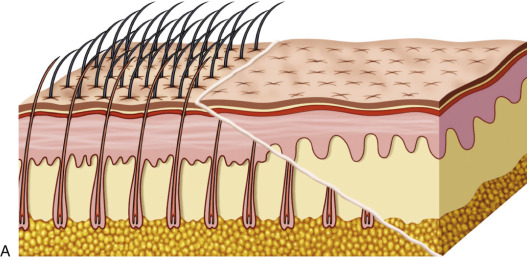
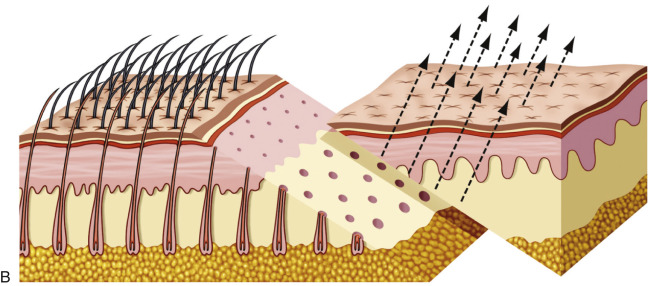
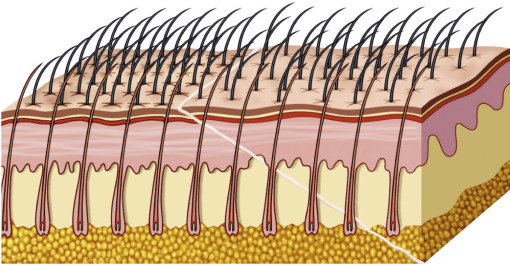
An important factor to keep in mind when choosing a browlift technique is whether or not it elevates the patient’s hairline. A long forehead and high hairline are not considered aesthetic for females. Coronal and endoscopic browlift approaches will both elevate the anterior hairline along with the brows. The endoscopic approach separates the deep tissue planes and elevates the brow and forehead by lifting the redundant skin and repositioning it posteriorly ( Fig. 4.7 ). The TFSBFL does not raise the hairline when lifting the brow and forehead.
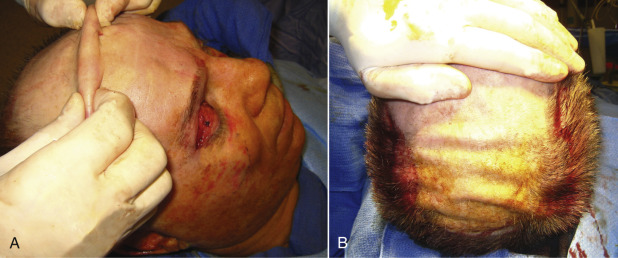
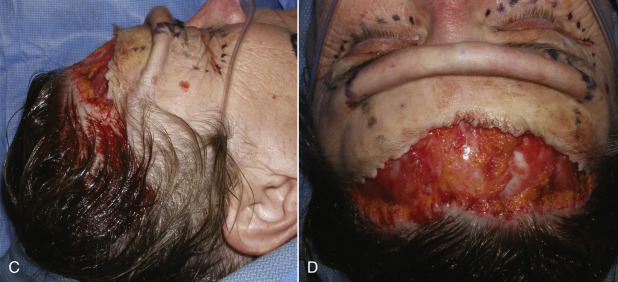
Perhaps the biggest advantage of the TFSBFL is that does not elevate the anterior hairline, which is of tremendous importance. For patients with a low hairline, virtually any browlift procedure is acceptable, as nominal hairline elevation is not critical ( Fig. 4.8 ). For patients with higher hairlines (longer foreheads), no extra increase in the anterior hairline is acceptable, so patients with elevated hairlines are optimum candidates for TFSBFL. This approach does not raise the hairline (when properly performed) but with additional distal scalp undermining and release, a patient’s hairline can actually be lowered.
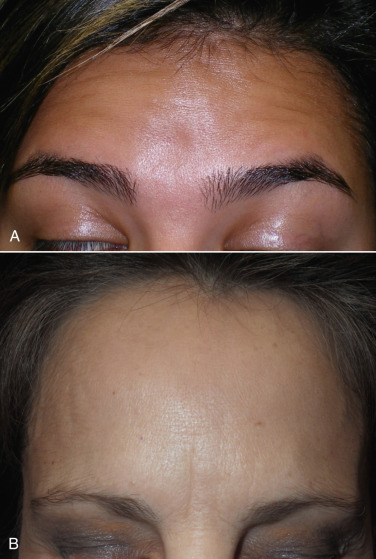
The learning curve is less complex than the EBFL, and this approach is very similar to facelift surgery, in that it involves dissection and skin excision. The TFSBFL is simply a facelift for the forehead and brow. Subcutaneous dissection, flap development, skin excision, and resuturing techniques are virtually identical to rhytidectomy ( Fig. 4.9 ).
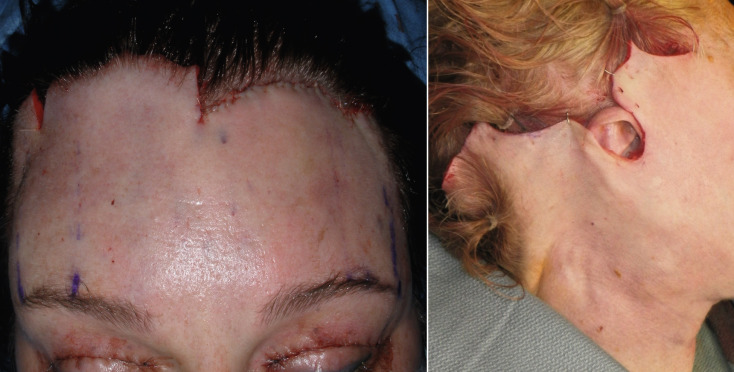
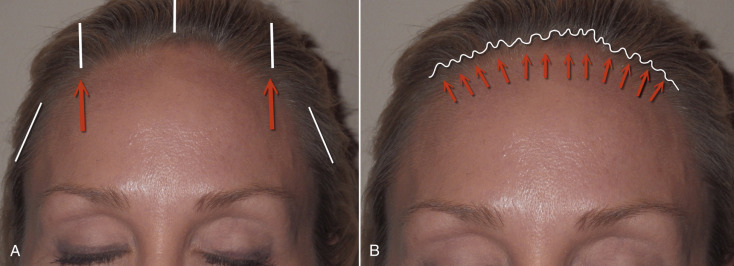
Being a subcutaneous procedure, there is less edema and ecchymosis compared with other browlift techniques. Since this is a skin excision technique, stability is excellent, and the result is immediately evident. As the skin is excised all across the horizontal hairline and the area resutured, the suspension is dispersed across the entire brow hairline ( Fig. 4.10A ). This is in extreme opposition to the EBFL, which only has several fixation points that are suspended with extreme tension in selected regions ( Fig. 4.10B ). An additional advantage is that TFSBFL, being a subcutaneous technique, will have an impressive effect on the effacement of vertical and horizontal forehead rhytids. This is possible because the skin is dissected from the underlying frontalis muscle and then tightened, which significantly improves horizontal wrinkles ( Fig. 4.11 ). Subperiosteal browlifts are not nearly as effective at improving horizontal forehead wrinkles, because they cannot effectively be addressed from the subperiosteal plane. Direct access to the brow depressors is another advantage when compared with endoscopic access; the treatment of these muscles is easier under direct vision.
There is no need for osseous fixation with the TFSBFL, which is an advantage for both the surgeon and the patient, as many patients are averse to having holes and hardware in their skull. Finally, there is no need for over-correction with the subcutaneous skin excision technique and much less chance of frontal nerve injury. Box 4.1 shows the relative advantages of TFSBFL compared with the endoscopic technique.
| Subcutaneous mini open brow and forehead lift (TFSBFL) | Endoscopic brow and forehead lift (EBFL) |
|---|---|
|
|
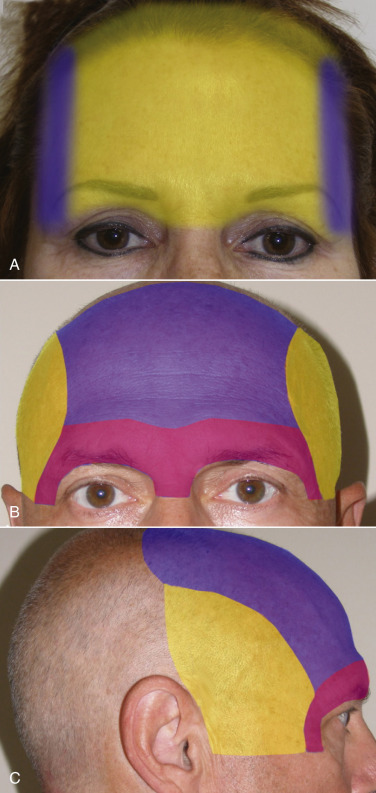
A relative disadvantage is that the TFSBFL is not reversible, insofar as it is a skin excision technique. An over-corrected endoscopic brow and forehead lift could be reversed in the first several weeks by releasing the fixation and redissecting the pockets. There is no easy means of reversing TFSBFL after the skin has been removed. Another relative disadvantage is the public or collegial perception, that open browlifts are excessive or antiquated. Endoscopic proponents claim that the endoscopic technique is a minimally invasive procedure. This is not true. Only the actual incisions are minimally invasive. In reality, the endoscopic technique is the most aggressive browlift technique, traversing numerous tissue planes on the majority of the skull, and necessitating the use of cranial fixation ( Fig. 4.12 ). The EBFL is definitely more high-tech and the small incisions are attractive to patients, especially when over-touted by surgeons that do not possess the skillset for the transfollicular subcutaneous technique. Comparatively, TFSBFL is a very conservative procedure. There is a visible incision for several weeks, but when this procedure is performed correctly, the incision is rarely a concern.
Diagnosis
Although I promote the transfollicular approach first, any browlift that has natural results, low complications, and happy patients is a good procedure. The diagnosis for TFSBFL is the same as for other browlift techniques. Once it is determined that a patient wants a browlift, a decision is made as to what technique to employ. When deciding which technique to use, several factors should be considered. First, the position of the patient’s hairline: if the patient already has a naturally high hairline with a long forehead, the TFSBFL is preferable, as no patient with a high hairline wants it higher. Another scenario is a patient with a significantly rounded frontal bone or frontal bossing. This exaggerated frontal curvature makes an endoscopic technique more difficult because the surgeon is working tangential to the curved bone, making it difficult to position the tip of the scope. Also, the need for drilling into the skull and using some type of retention system is a negative for many patients. It is important to let patients know preoperatively if drill holes and or hardware will be used, to ensure accurate informed consent.
Patients with permanently tattooed eyebrows can be problematic, especially if the tattoos are not symmetric or extremely peaked. When the skin is excised and the forehead retracted, an unnatural result can occur. Any patient with permanent tattooed brows should be closely evaluated for result when the brows are manually lifted, and the problem discussed while the patient looks in a mirror. Some patients have virtually no eyebrow hair and draw them on daily. This is not a problem, as they can be drawn at any height postoperatively by the patient. This type of patient is actually the best browlift candidate, as the operation improves their periorbital aging and the brows can be drawn anywhere the patient desires.
Also germane with choosing a brow technique is the use of simultaneous laser resurfacing. The endoscopic technique is subperiosteal and can be aggressively lasered in the same manner as the rest of the face. The transfollicular subcutaneous technique is a much thinner flap and more prone to devitalization. When I laser an endoscopic forehead, I use the same settings as the face, but when I laser a transfollicular subcutaneous browlift, I reduce the power or the density of the laser in the same manner that I do with facelift flaps.
For younger surgeons, it is sometimes difficult to determine which patients are appropriate (or inappropriate) candidates for brow and forehead lift. Box 4.2 shows some of the various diagnostic indications and contraindications for brow and forehead lift.
| Indications | Contraindications |
|---|---|
|
|
Transfollicular Subcutaneous Brow and Forehead Lift: Surgical Technique
Patients are instructed to wash their hair for several days before surgery and the day of surgery with an antibacterial soap.
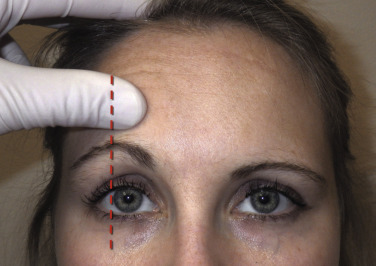
As with blepharoplasty, the TFSBFL success revolves around proper preoperative incision markings, which must be precise and accurate. After photographs are taken, the patient is marked preoperatively. The area of maximum brow elevation is decided with the patient looking in the mirror. When in doubt, it is always better to be conservative. The area of maximum brow elevation is generally at the junction of the central and lateral thirds of the eyebrow, which usually coincides with an imaginary vertical line at the lateral limbus ( Fig. 4.13 ). This is a guideline and may differ in some patients, but is generally accurate. Some older females literally have no eyebrow hairs and draw them in daily, which as stated above, is a safe situation. Care must be exercised not to over-elevate the medial brows, as this can produce an unnatural and quizzical appearance. Fig. 4.14 shows the typical markings for the TFSBFL.
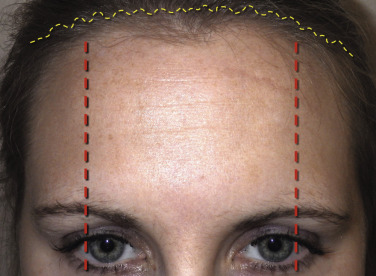
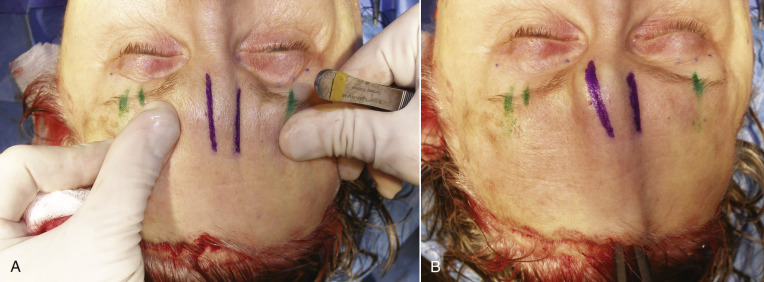
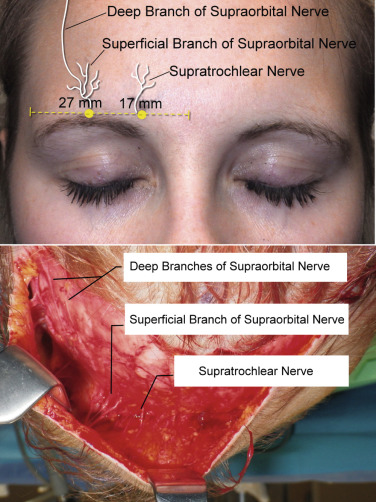
Additional markings commonly used include the supratrochlear nerves, which are located approximately 17 mm from the midline and the supraorbital nerves, which are approximately 27 mm from the midline ( Fig. 4.15 ). Marking the neurovascular bundles allows the surgeon to be mindful of significant anatomy. Blepharoplasty markings are also performed if planned at the same procedure.
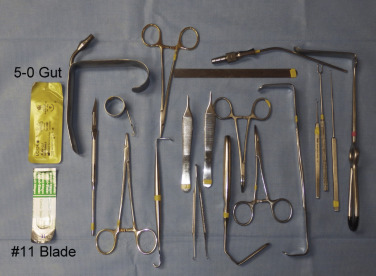
The instrumentation for TFSBFL is minimal and similar to facelift surgery ( Fig. 4.16 ). Most commonly used instruments include:
- •
Round scalpel handles
- •
No.11 scalpel blades
- •
Fine pickups
- •
Comb
- •
Marking pen
- •
Suction
- •
Retractors (lighted are preferable)
- •
Radiowave or electrosurgical unit for hemostasis
- •
4-0 gut, 5-0 gut, and/or 6-0 nylon sutures.
The TFSBFL can be performed with local or tumescent anesthesia, but is most commonly performed with intravenous (IV) sedation, as other simultaneous procedures are frequently included.
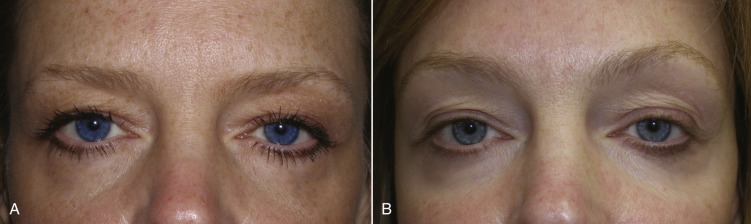
Regardless of the browlift technique utilized, I personally do a simultaneous blepharoplasty in almost every case. I feel that most patients that are in need of a browlift are also in need of some upper-lid skin reduction. Obviously, eyelid closure must remain functional, so discretion is required. If the upper lids are not addressed, the patient may be left with a perfectly elevated brow but redundant upper-lid skin that detracts from the result ( Fig. 4.17 ). Also, in the event the brow is not elevated enough or minor relapse occurs, the combination of blepharoplasty and browlift provide a combined change that will usually satisfy the patient.
When performing simultaneous blepharoplasty with browlift, a much more conservative blepharoplasty procedure is invoked. Less skin is removed and the outline of the blepharoplasty incision is different from conventional blepharoplasty. When performing conventional blepharoplasty, most surgeons use an upswept incision at the lateral portion of the eyelid. This is done to assist with lateral hooding. When performing browlift surgery, the lateral hooding is automatically corrected, so there is no need to perform the upswept lateral blepharoplasty incision. The “bleph with brow” incision is tapered on both ends ( Fig. 4.18 ). Whereas a traditional blepharoplasty may dictate a 10-mm skin excision, the blepharoplasty done with browlift requires only 3–4 mm of skin excision. When combining simultaneous blepharoplasty and browlift, novice surgeons should perform the browlift first, as the amount of eyelid skin excision is more easily determined. Experienced surgeons can perform the blepharoplasty first by taking 3–4 mm of skin at the beginning of the procedure. Additionally, elevating the brow will reposition the eyelid tissues so significant muscle or fat removal is not generally necessary and simple skin excision is usually sufficient for most cases. I have never experienced a problem lagophthalmos when combining these procedures.
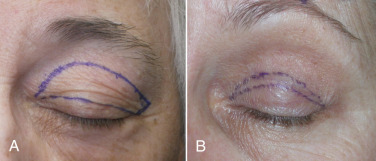
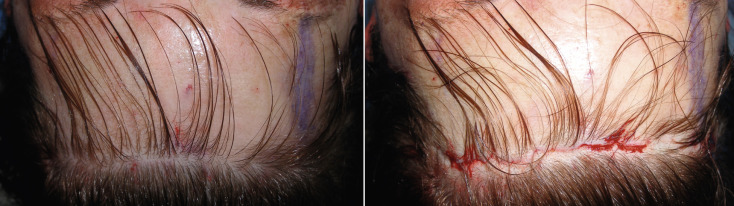
When performing blepharoplasty before the browlift, the lid incisions are closed before scalp excision is performed. The surgeon can therefore decide how much excess forehead skin can be removed without producing significant lagophthalmos. Enough skin must remain to close the lids, and this is taken into account during excess scalp excision ( Fig. 4.19 ). Novice surgeons should avoid simultaneous blepharoplasty or perform it at the end of the case to avoid significant lagophthalmos.
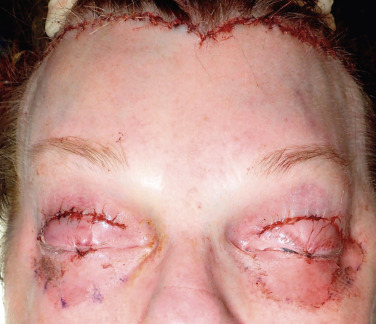
Crafting the Incision
There are few surgeries totally defined by a specific incision, but this is one of them. The technicality and quality of the transfollicular incision can make or break the aesthetic success of this browlift procedure. There are two basic principles of this lift. The first critical principle is to craft a precision incision to allow hair regrowth through the surgical scar, thus camouflaging it. The second principle is to elevate the brow and forehead without raising the hairline.
The incision pattern is also very critical for a naturally appearing hairline scar. First, the incision should never be made anterior to the hairline. To avoid old terminology confusion, we will refer to incisions anterior to the hairline simply as “prefollicular” hairline incisions. They are also referred to as “trichophytic” or “pretrichial” and this incision totally avoids any hair follicles. This may sound good in theory and will definitely be easier to incise and close, but the aesthetics are frequently unacceptable and produce a straight line, often hypopigmented scar ( Fig. 4.20 ). I frequently hear surgeons advocate the prefollicular hairline incision but continually see patients in my office who were operated elsewhere and have unacceptably visible scars. Even geometric, random incisions performed anterior to the hairline can heal with a very unnatural appearance ( Fig. 4.21 ).
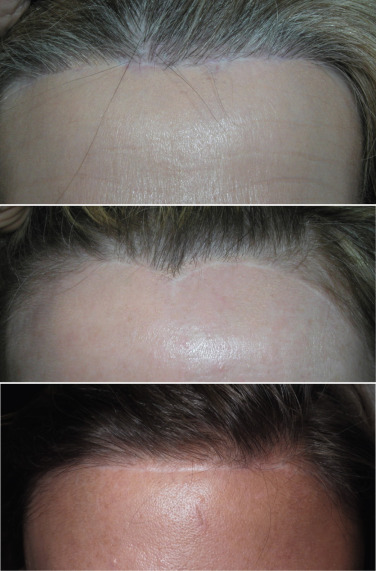
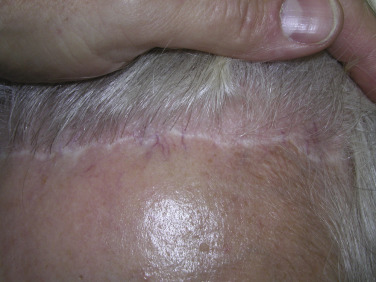
As there are very few straight lines in human anatomy, these prefollicular scars can look unnatural. Also important is the fact that there is no such thing as a “natural hairline.” Normal hairlines are not lines at all, but very incidental and random patterns of follicles. Only a toupée or a poor hair transplant produces a true “hairline.” Making a straight line prefollicular incision on a patient’s forehead can make them look unnatural, with a visible and often hypopigmented scar ( Fig. 4.22 ).
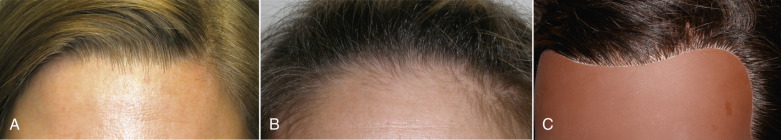
The transfollicular incision is unique in design. First, the incision is designed to transect the existing hair shafts and follicles at a steep bevel. This incision is intentionally placed about 5 mm posterior to the true hairline. The optimum placement of this incision is at the region of the follicular density change from the thin, sparse anterior hairs to the denser follicles of the “actual” hairline ( Fig. 4.23 ). The incision has to be placed posteriorly enough to allow the scalpel to transect enough hair shafts and follicles to regrow through the thin scar edges.
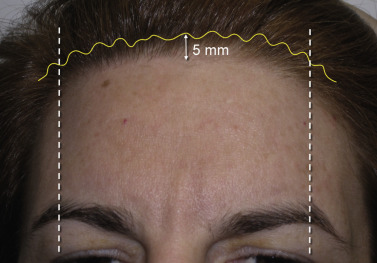
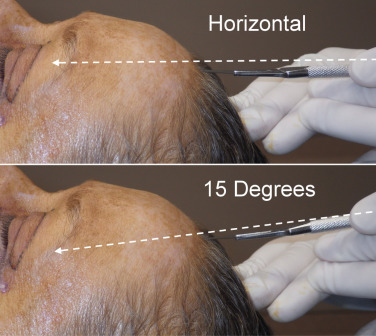
The bevel of the incision is critical and must transect several rows of hair shafts and follicles at different heights. In order for this to occur, the scalpel with a No.11 blade must be held about 10–20 degrees above the horizontal plane, as shown in Fig. 4.24 . This angle and scalpel movement is similar to filleting a fish, except the blade is not totally horizontal. The reciprocal motion of filleting a fish is used when the incision is made.
This extreme bevel has numerous functions. First, it allows the angled transection of hair shafts and follicles, which encourages hair regrowth through the scar. Second, this extreme bevel produces a very thin skin incision edge. Whereas an incision made perpendicular to the skin surface will produce the thickest skin edges, the more angled the scalpel is held, the thinner the skin flap edges will be. This very thin epidermal/dermal interface contributes to the excellent aesthetics of this type of skin incision. This thin interface also makes it easier for the underlying hair follicles to grow through the thin flap. When the surgeon appreciates these characteristics and can predictably perform this incision, repeatable outcomes are accomplished with this approach.
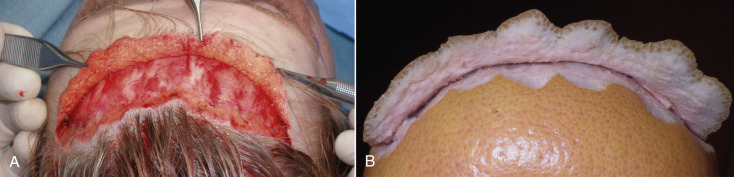
To illustrate this transition, Fig. 4.25 shows a beveled incision on a grapefruit peel; the white region corresponds to the dermis, and the yellow region corresponds to the epidermis.
Incision Geometry
Keeping with incision design, the next aspect to be addressed is incision geometry. Understanding that the incision is placed about 5 mm into the hairline, the configuration can be regular with large or small triangles or irregular with random undulating geometry. Different surgeons prefer one of these configurations over the others. Proponents of large triangular incisions say that the incision, skin excision, and reapproximation of the trimmed flap is less laborious. My experience with the larger triangular configured flaps has been that the larger regular triangles show more intentional geometry, which is obvious after healing ( Fig. 4.26 ). Other surgeons prefer very tiny triangles and this is not only more labor intensive to cut and sew, but the smaller the triangles, the more the final incision resembles a straight line ( Fig. 4.27 ).
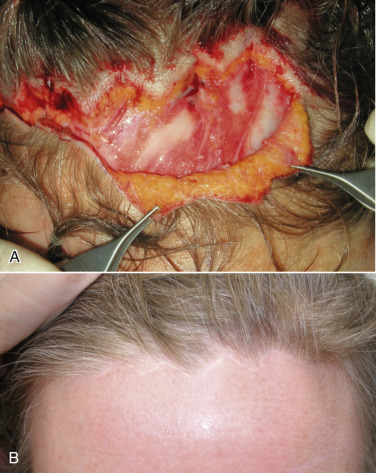
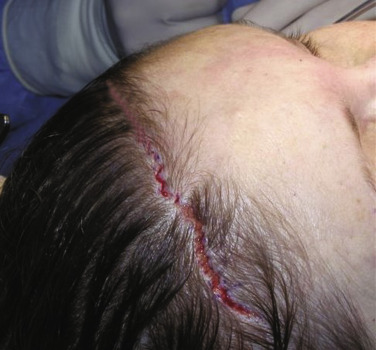
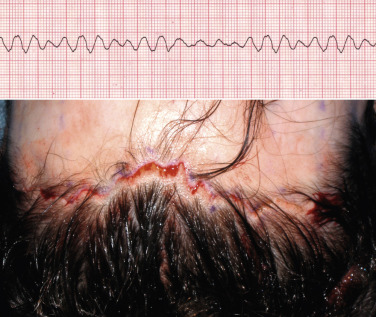
After experimenting with all the common geometric incision patterns, experience has shown that a random, irregular, undulating incision pattern produces the best postoperative scar. As stated earlier, this incision is made by using the scalpel at about a 10–20 degree angle from horizontal in a reciprocating manner like filleting a fish. The pattern is basically irregular and reminiscent of ventricular fibrillation on an electrocardiogram ( Fig. 4.28 ). The incision pattern and the angle of the cut are both critical factors in the success of this technique.
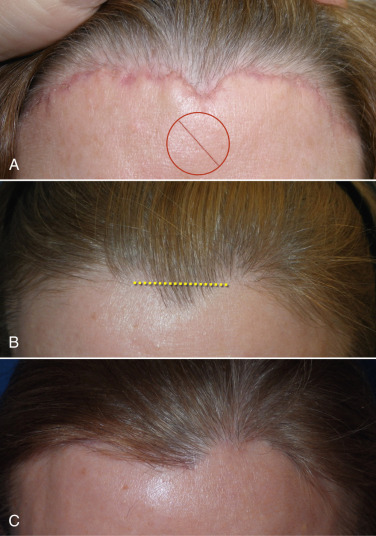
If a patient has a prominent widow’s peak, it is better to cut through the lower-third of the apex instead of following the distinct “V” shape of the peak. Otherwise the angles are too conspicuous with the final scar ( Fig. 4.29 ).
Similar to blepharoplasty, correctly marking this browlift incision is critical. Marking the incision 5 mm posterior to the hairline with a conventional “Magic Marker” type felt marker with an angled tip, provides a basis for the incision outline. The marker is used to mark triangles by rotating the tip while marking. The first mark is made with the tip held at a 45-degree angle to the left, then the marker is rotated 45 degrees to the right to make the corresponding angle. This is repeated 5 mm behind the hairline across the scalp ( Fig. e4.1 ![]() ). Although triangles are drawn, the incision is not angular and the peaks of the triangles are rounded with the scalpel. The triangles are only used as a general guide.
). Although triangles are drawn, the incision is not angular and the peaks of the triangles are rounded with the scalpel. The triangles are only used as a general guide.
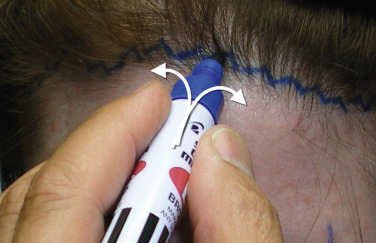
Transfollicular Incision and Healing
The reason this incision heals so well when performed properly is that the transected hair follicles can regrow through the incision and camouflage the scar. In order for this to occur, the bevel of the incision must transect the hair shafts and follicles at various angles. The most anterior and usually fine vellus hairs may be totally excised and be lost. Generally, this small amount of hair loss is negligible and not noticeable in the final result. The next rows of follicles are transected close to the hair bulb and these are the hairs that will regrow through the scar. The posterior-most hair shafts will be transected towards the top of the shaft and these will also grow back ( Fig. 4.30 ).
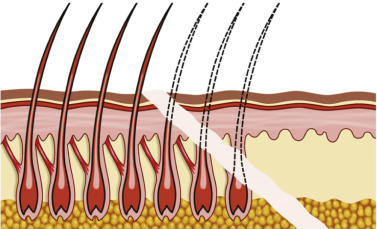
Although some hair may be excised when trimming the flap, it should be negligible if the incision is made correctly ( Fig. 4.31 ). It may appear that more hair is lost when incising, but it is important to remember that some of the rows of follicles that appear to be cut will actually regrow through the scar; in effect these hairs are cut but not lost.
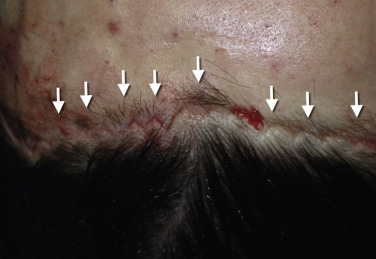
As with any surgical procedure, a learning curve is associated with this technique but when mastered, the postoperative scar and hairline can be virtually undetectable ( Fig. 4.32 ).
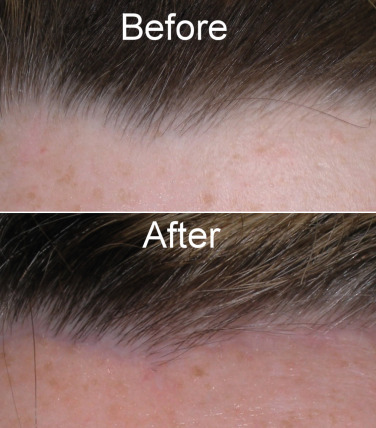
The reason that the incision cannot be made more posteriorly than 5 mm is that if the incision is made more posteriorly, more hair will be removed during flap trimming and the hairline will be elevated, which is counterintuitive to this hair-sparing technique. The further back the incision is made on the scalp, the more the procedure resembles a coronal lift and elevates the hairline. In some patients, the incision may be slightly posterior, such as 7 mm, but beyond that, excessive anterior hair will be lost during skin excision. When the incision is close to the hairline, the excised tissue will be forehead skin and not hair. The incision does need to be posterior enough to accept a long bevel with the No.11 scalpel blade and 5–6 mm is generally adequate. Patients with thick straight hairlines across the entire forehead are the easiest candidates for novice surgeons. For patients that have do not have a distinct, straight hairline, or have lateral hair recession, the incision must be modified to accommodate the follicular density as it curves around the hairline ( Fig. 4.33 ).
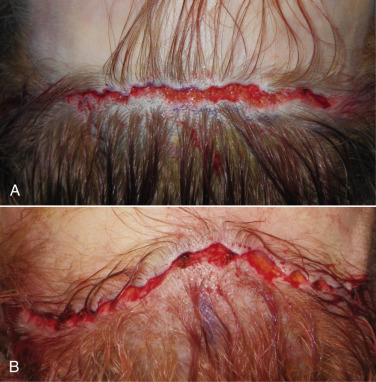
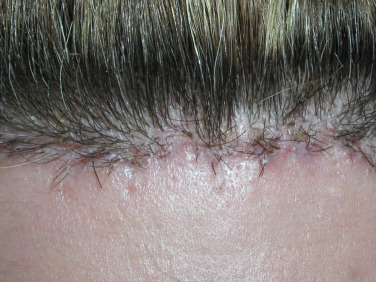
After the initial hyper-beveled incision is made and dissection completed, the excess forehead skin will be retracted towards the scalp and also trimmed with the same angle bevel as the initial incision. The feather-edged forehead skin flap will then lie on the feather-edged scalp flap to create a very thin epidermal/dermal interface ( Fig. 4.34 ). It is this thin skin interface, which lies over the transected hair shafts and follicles, that allows the hair to regrow through the skin and camouflage the scar ( Fig. 4.35 ). When these incisions are properly performed, new hair regrowth can be seen in the first several weeks after the procedure ( Fig. 4.36 ).
Step-by-Step Operative Technique
Simultaneous Blepharoplasty
I believe that almost any patient that needs a browlift also needs blepharoplasty. I perform simultaneous blepharoplasty with almost all browlifts (endoscopic and transfollicular). The only exceptions are patients that do not have dermatochalasis, or patients that have had previous aggressive upper-lid skin resection. To determine this, I manually elevate the brow to the desired position. If there is redundant lid skin (which there generally is), then I will perform simultaneous blepharoplasty. Another means of estimating the need for blepharoplasty is to lie the patient back in the chair. This automatically places the brows in an elevated position. If there is still excess upper-lid skin in this position, a blepharoplasty is warranted.
After the surgical prep is completed, the incision marking is visualized and several rows of hair are combed forward to expose the scalp where the incision will be made ( Fig. 4.37 ).
Anesthesia
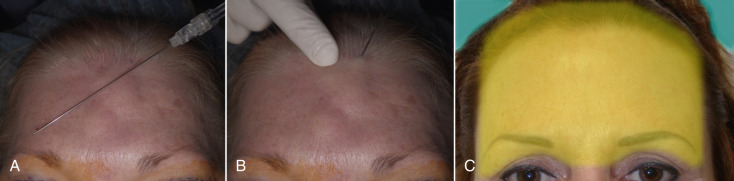
As stated earlier, this procedure can be performed with tumescent anesthesia only but is more commonly done with sedation. For tumescent technique, the entire brow and forehead is injected with typical Klein’s solution (0.1% lidocaine with 1 : 1 million epinephrine) with a 23-gauge spinal needle. The tumescent solution is injected from the hairline to the superior orbital rims and laterally to the temporal crests. It is critical that the local anesthesia is injected in the subcutaneous plane, as this is where the dissection will occur. The tumescent solution also produces hydrodissection between the dermis and frontalis, which aids in the actual surgical dissection. The actual hairline where the scalpel incision occurs is injected with 2% lidocaine 1 : 100,000 epinephrine. If the surgeon does not want to use tumescent anesthesia, the entire brow can be injected with the standard 2% lidocaine with epinephrine. Again it is important to infiltrate from just above the planned incision to the superior orbital rims and the entire forehead between the temporal crests ( Fig. 4.38 ). Unlike liposuction, excessive volume of tumescent is unnecessary and only enough fluid to provide anesthesia and hemostasis is used.
Dissection
Just as a precision incision is required for this procedure to be successful, the dissection is equally important. Unlike many browlift procedures, this is a subcutaneous dissection. The proper dissection plane is below the dermis (including some subcutaneous fat) and above the frontalis muscle. This plane is similar to facelift surgery and the proper plane must be followed for success with this procedure.
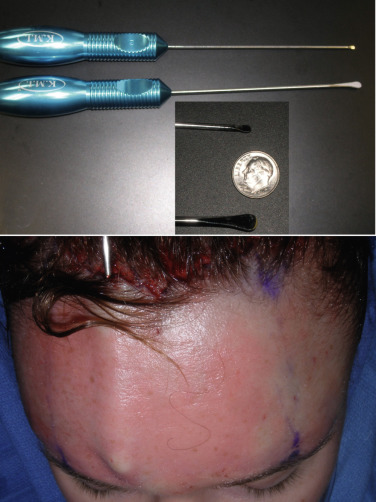
Some surgeons prefer to pretunnel or predissect the subcutaneous flap with blunt dissectors ( Fig. 4.39 ) as similarly performed in facelift surgery. Although this is not a necessary step, it is very helpful, especially for novice surgeons, to find and stay in the correct surgical plane and avoid trauma to the thin frontalis muscle complex.
After the pretunneling maneuver, the actual flap dissection is begun. Again, this is a subcutaneous dissection made below the dermis and above the frontalis muscle. The dissection is performed with facelift scissors, and it is imperative to remain in the subcutaneous plane and not damage the frontalis muscle or the sensory nerves that lie over it. The surgeon must remain cognizant that long branches of the supratrochlear and supraorbital nerves course from the superior orbital rim to the scalp ( Fig. 4.40 ).
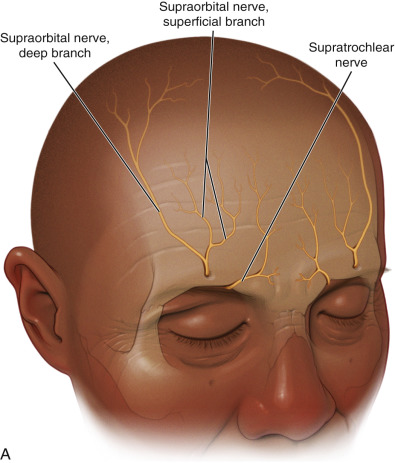
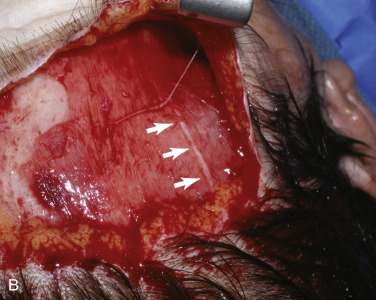
Scissors dissection is begun at the incision line as the scissors enter the subcutaneous plane. If the flap has been pretunneled, this dissection is easy and can be accomplished by “nipping,” pushing, and spreading with the scissors ( Fig. 4.41 ). This initial scissor dissection can be performed “blindly” (indirect vision) to a point several centimeters above the orbital rim to prevent damage to the supratrochlear and supraorbital nerve branches. Distal to this, all dissection must be completed with direct vision, as the neurovascular bundles are easily visualized. A lighted fiber optic retractor greatly facilitates the surgery. In the midline glabellar region, blunt or sharp dissection can be performed to the nasal radix without fear of nerve injury.
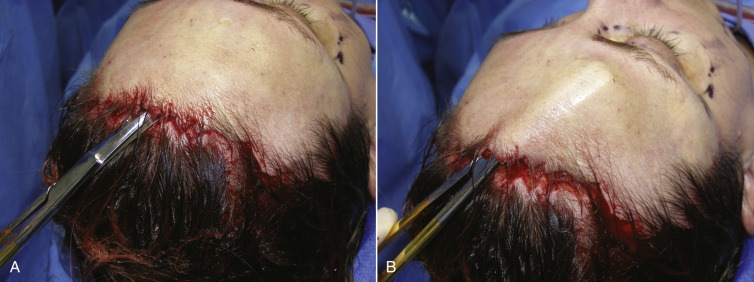
As the flap is developed, bleeding will occur at the incision site. Minor bleeding will subside but given the vascular nature of the scalp, larger areas of bleeding must be cauterized. Very fine tip bipolar forceps are used and extreme care is exercised not to damage exposed hair follicles ( Fig. 4.42 ). The surgeon must always keep in mind that it is the hair follicles and cut hair shaft that regrow through the scar and any damage to these structures can compromise the result.
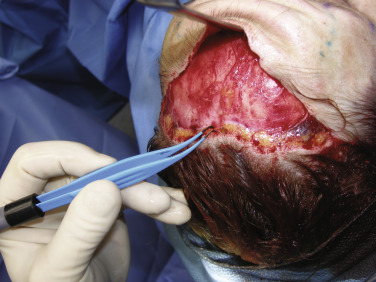
After the initial flap is developed, it is completed to the required extent. This can be variable depending on the age of the patient and amount of brow and lid ptosis. In most cases, the lateral extent of the dissection extends just past the brow tail to the point needed to fully elevate the brow ( Fig. 4.43 ). In older patients, or those with extreme ptosis or hooding, the dissection can proceed more laterally, just up to the temporal crest (conjoined tendon) but never exceeds this region laterally ( Fig. 4.44 ). Again, the advantage of this procedure is simplicity. Staying medial to the temporal crest region also prevents damage to the frontal nerve.
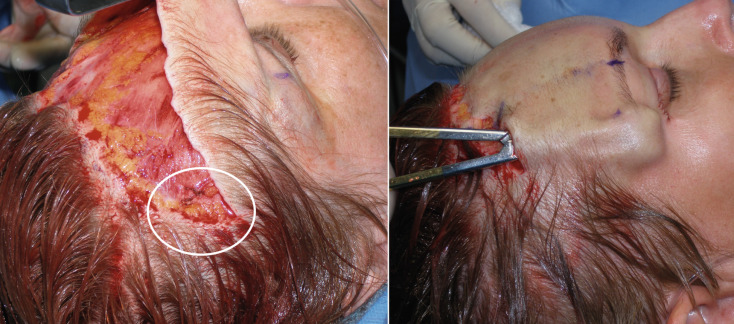
It is imperative to remember that this is lipocutaneous flap performed in a plane above the frontalis muscle. The flap should have adequate fat on the dermal surface ( Fig. 4.45 ). The frontalis muscle is very thin in some females and sometimes translucent. Gentle dissection in the subdermal, premuscular plane above the muscle is essential to preventing injury.
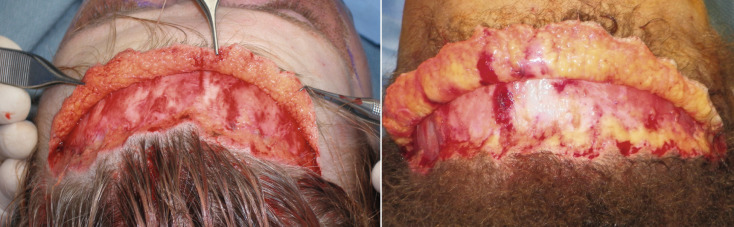
Once enough inferior dissection has been performed to accommodate retractors, the remainder of the procedure is performed with direct vision ( Fig. 4.46 ). As the direct vision dissection approaches the superior orbital rims, the anterior flap can be folded inferiorly to facilitate vision. This may not be possible with a small flap on a younger patient, but may be performed with a larger lateral dissection on a patient with increased aging and ptosis ( Fig. 4.47 ).
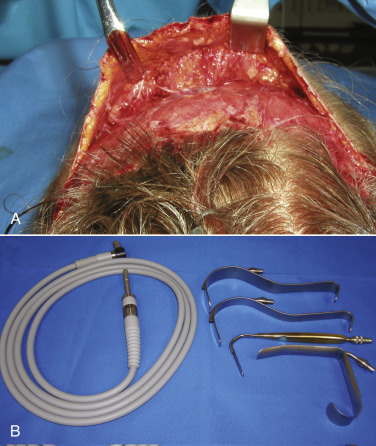
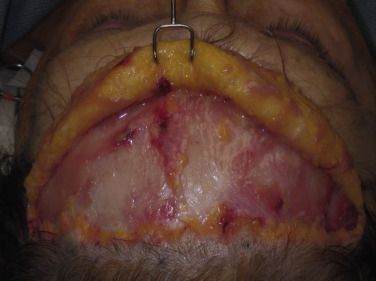
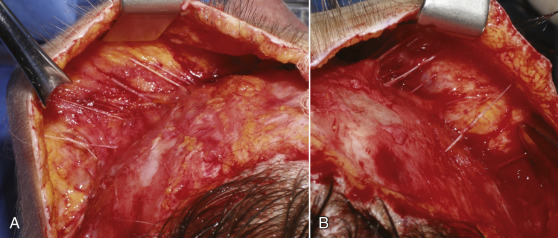
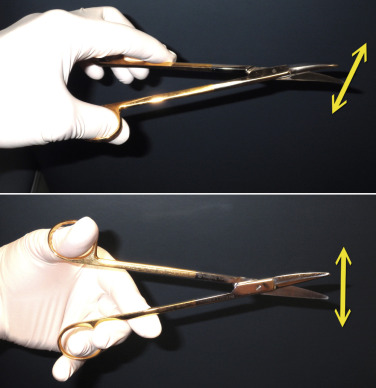
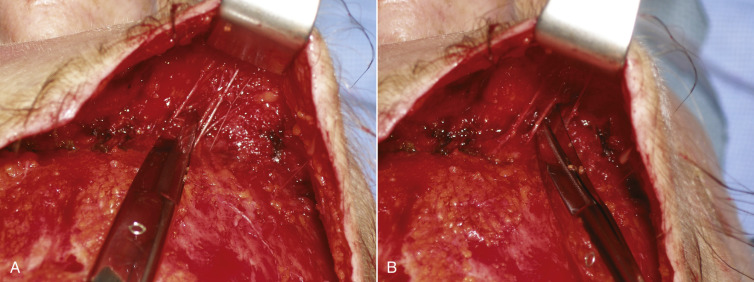
As the dissection continues, the neurovascular bundles of the supratrochlear and supraorbital nerves will be encountered. The advantage of a direct vision approach is the excellent visualization of these structures ( Fig. 4.48 ). As the dissection nears the orbital rims, and hence the neurovascular bundles, judicious and precise surgery is required to prevent nerve injury. In the area of the neurovascular bundles, direct vision should always be used. Blunt facelift scissors are used to gently spread the perineural tissues without disrupting the nerves and vessels. The initial approach is with the scissors used horizontally. The bundles can actually be dissected further by turning the scissors vertically and gently stretching between the bundles for additional release and dissection ( Fig. 4.49 ). The neurovascular bundles can be gently stretched without permanent damage, while dissecting in the subcutaneous plane ( Fig. 4.50 ). This is preferable to having them tethered to the flap, which will later be stretched.
For surgeons used to endoscopic or coronal approaches, the nerve bundle in these approaches are subperiosteal and the nerve exits a foramen or notch as a distinct single bundle ( Fig. 4.51 ). Damaging this main branch can cause considerable damage. In the subcutaneous approach, the nerve has branched from the bundle, so main trunk damage is less risky.
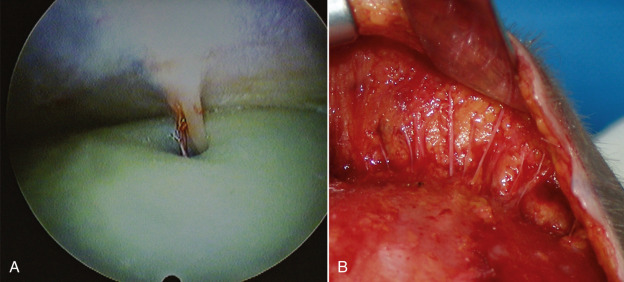
As the inferior dissection proceeds, nerves are gently freed from the surrounding tissues or avoided altogether if it is not an obstacle or not interfering with the lift. It is imperative to release the eyebrows completely for effectiveness and stability of the lift, so the surgeon must dissect inferior to the brows and into the upper lids ( Fig. 4.52 ). Since the patient is in the supine position, the brow will almost self-elevate when the appropriate adhesions and tethers are released with the scissors. When the brow is passively released and elevated to the proper arch, the dissection is sufficient. This will differ from patient to patient. Younger patients may only need dissection and elevation to the area of maximum arch but older patients may need dissection to the lateral orbital rim ( Fig. 4.53 ).