Atopic Dermatitis
Lauren Fried
Gabriela A. Cobos
David Cohen
BACKGROUND
Atopic dermatitis (AD) is a chronic and relapsing condition associated with pruritus and inflammation. The pathophysiology of AD is complex and involves both overactivity of the immune system and epidermal barrier dysfunction.
AD is the most common chronic inflammatory skin disease. It affects 15% to 30% of children and 1% to 3% of adults in the United States, and the prevalence is increasing.1,2 AD most often presents within the first 5 years of life, with 10% to 30% of cases persisting into adulthood. However, it may have a later onset, with about 20% of cases first presenting in adulthood.3
PRESENTATION
Patients may present with an acute or chronic report of pruritic, red papules or plaques. In young children, the affected areas typically include the face, hands, and extensors. In older children and adults, flexural regions, such as the antecubital fossae, are often involved.
DIAGNOSIS
Clinical Diagnosis
AD generally follows a relapsing and remitting course characterized by dry, pruritic, inflamed skin. Individual presentation may appear on a continuum between acute and chronic. Acute AD classically presents with edematous papules and plaques, vesiculation, oozing, and crusting, whereas the chronic disease presents with xerotic, lichenified plaques with pigmentary alteration. Distribution can follow age-specific patterns. In infants and young children, it is often red, scaly, blistering, or crusted, most often affecting the face, hands, or extensors. Older children more often show facial, neck, and extensor involvement, and adult AD is characterized by
patches of localized, lichenified eczema, particularly in flexural areas and also on the face, neck, and hands.4 Flexural lesions can occur in any age group.5 Diagnosis of AD is based on history and physical findings and includes pruritus, chronic eczematous dermatitis, personal or family history of atopy, and many other associated cutaneous stigmata.
patches of localized, lichenified eczema, particularly in flexural areas and also on the face, neck, and hands.4 Flexural lesions can occur in any age group.5 Diagnosis of AD is based on history and physical findings and includes pruritus, chronic eczematous dermatitis, personal or family history of atopy, and many other associated cutaneous stigmata.
Histopathology
Histology of acute AD demonstrates epidermal spongiosis, with mild dermal edema. There may be vesiculation due to marked spongiosis. The inflammatory infiltrate consists of perivascular lymphocytes and eosinophils, which can be occasionally found in the epidermis. In subacute AD, more chronic changes are found such as parakeratosis, acanthosis, and diminution of spongiosis. In chronic AD, lichenification is seen with epidermal acanthosis that is usually more irregular than psoriasiform acanthosis. There may be hypergranulosis when the affected area is more lichenified.3
Subtypes
Early-onset (pediatric) AD
Late-onset (postpubertal) AD
Associated Conditions
About 70% of patients with AD have a personal or family history of atopic disease.5 As noted earlier, the epidermal barrier dysfunction allows for epicutaneous sensitization. Thus, patients with AD often develop other atopic conditions simultaneously or in succession, which is known as the “atopic march.” AD presents first in infants and young children, followed by food allergies, then asthma in older children, and finally pollen allergy in adolescents.1 Other associated conditions include pityriasis alba, keratosis pilaris, and ichthyosis vulgaris.6
Quality of Life
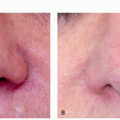
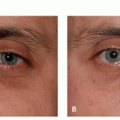
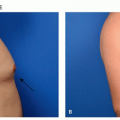
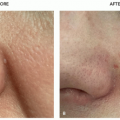
AD is not a cosmetic or aesthetic condition but has a profound impact on appearance and well-being. Pruritus in AD can range from occasional and paroxysmal to continuous and extreme, affecting a patient’s ability to sleep and perform activities of routine daily living and work.7 Intense pruritus and subsequent frequent visible scratching may amplify observer fears for the possibility of contagion, leading to feelings of isolation. Eczematous lesions can occur in highly visible locations such as the face or hands, the presence of which can be unsightly and embarrassing. Lichenified, excoriated plaques of AD can leave scars and hyperpigmentation or hypopigmentation even after treatment. Resulting self-consciousness can lead to feelings of depression, diminished self-worth, and social anxiety.7 Children and adults with AD report significantly higher levels of anxiety, depression, and sleep disturbance.8,9 Eczematous lesions can also pose occupational hazards as they may limit the use of affected areas and place patients at higher risk of acquiring transmissible disease and contact allergies via open lesions.
Differential Diagnosis
Allergic contact dermatitis
Asteatotic dermatitis
Eczematous drug eruption
Nummular dermatitis
Seborrheic dermatitis
Psoriasis
Scabies
Dermatophytosis
Cutaneous T-cell lymphoma
Dermatitis secondary to immune deficiency syndromes
Chronic actinic dermatitis
PATHOGENESIS
Immune overactivity in AD lesions is evidenced by increased prevalence of TH2 cells, which produce inflammatory cytokines, including interleukin (IL)-4, IL-13, and IL-31.10 These and other cytokines increase IgE production, activate additional TH2 cells, cause pruritus, and impair proper epidermal keratinocyte differentiation, thus promoting inflammation and contributing to barrier dysfunction.11
Epithelial barrier dysfunction allows for increased penetration of allergens and antigens, which leads to increased TH2 activation and amplifies the inflammatory cascade. The barrier dysfunction also leads to increased transepidermal water loss, causing xerosis and increased susceptibility to viral and bacterial infections, including Staphylococcus aureus, herpes simplex virus, and molluscum contagiosum.12
There is still ongoing debate on whether the inappropriate immune activation with production of inflammatory cytokines, IgE, and pruritus-derived scratching engenders damage in the epidermal barrier or whether inherent barrier dysfunction allowing for increased
penetration by allergens triggers the inappropriate inflammation.13
penetration by allergens triggers the inappropriate inflammation.13
There is also a significant genetic component in the pathogenesis, as evidenced by a higher concordance rate for AD among monozygotic twins (80%) compared with dizygotic twins (20%).14 Additionally, mutations in the filaggrin gene (FLG), which lead to loss-of-function variants, have been found in high proportions in both European and Asian populations with AD. The FLG encodes a protein that is vital for epidermal barrier function. These mutations are associated not only with an increased risk of developing AD (odds ration >4, compared with noncarriers) but also with an earlier onset of disease and more severe, persistent phenotype.15
TREATMENT
The purpose of treatment of AD is to eliminate pruritus and to restore patient’s skin to normal appearance and function. In selecting a topical treatment regimen, it is important to consider not only efficacy and safety of the treatment method but also the aesthetic acceptability of different vehicles to the patient. Different delivery systems (creams, ointments, etc) will have differences in ease of application and speed of absorption, presence of residues, and interference with daily life, all of which can greatly impact patient compliance and effective utilization of the treatment.16 Algorithm 14.2.1 describes the treatment of patients with a diagnosis of AD.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree