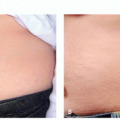
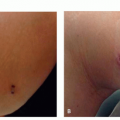
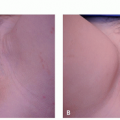
Constitutional: a well-demarcated brown band over the lower eyelid approximating the orbital rim, which may also involve the upper eyelid.
Postinflammatory: irregular brown or gray patches often with lichenification on the upper, lower, or both eyelids. There may be a personal or family history of atopy.
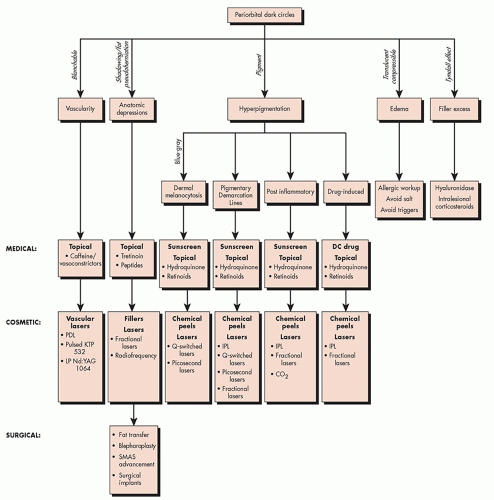
Vascular: erythema or bluish discoloration involving the lower eyelids that is more prominent with stretching of the skin. This is often due to translucent overlying skin.
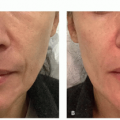
Shadow effect: dark shadow formation from fat pad prominence or presence of a deep tear trough.
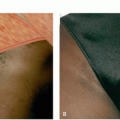
Pigmented: brown color
Vascular: blue/pink/purple color
Structural: skin color
Ocular rosacea
Nevus of Ota (see later discussion)
Nevus of Hori (see later discussion)
Blue nevus
Melasma
progressive infraorbital anatomic depressions worsen over time owing to osteoporosis, loss of subcutaneous fat, and loss of collagen and elastin in the overlying skin and orbital rim ligaments, combined with cheek laxity, exacerbating hollowness to the orbital rim and infraorbital sulcus.
TABLE 4.4.1 Classification of Periorbital Pigmentation | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree