BACKGROUND
Cutaneous squamous cell carcinoma (SCC) is extremely common and fortunately highly curable. As these lesions have a propensity for development and growth in visible regions of the skin, cosmetic outcomes are often very important. Critically important too is that a small subset of these cancers is locally and systemically aggressive and can become life-threatening. Therefore, optimal management for this diagnosis is of utmost concern.
This chapter reviews the state of the art in diagnosis and management of invasive cutaneous SCC with special emphasis given to those lesions at high risk for local treatment failure and also for poor cosmetic outcomes.
Nonmelanoma skin cancer is diagnosed in several million people annually, most commonly basal cell cancer followed by SCC.
1 The incidence and prevalence of SCC continues to rise due in large part to excessive unprotected sun exposure.
2 The intentional use of UV tanning booths further contributes to a younger population diagnosed with this malignancy. The success of immunosuppression for organ transplantation and other disease has contributed to a rise in aggressive forms of squamous cell disease.
3Classically cutaneous SCC is a disease of older individuals, with peak incidence in the sixth and seventh decade. Most lesions develop in sunlight-exposed skin, namely, the head, neck, and back of hands. Lighter color of skin (Fitzpatrick types I/II), outdoor work schedules, geographic location associated with intense sunlight, and older age increase risk of lesion development. Individuals in their 20s are more commonly being diagnosed in Australia, Florida, and
Southern California, so high levels of suspicion are always needed even in a young age group. In particular those with albinism and xeroderma pigmentosum are at extremely high risk for SCC development, even as young as 10 years of age.
4
PRESENTATION
Although SCC is most commonly a disease of the Caucasian elderly with a history of excess sun exposure, it can afflict the young, those with pigmented skin, and particularly those with genetic and immunosuppressive states.
5 Therefore, a high level of clinical suspicion is required.
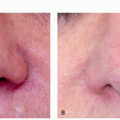
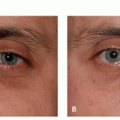
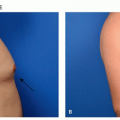
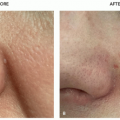
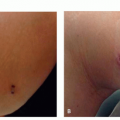
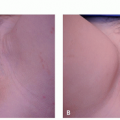
Patients typically present with a reddish growth with a rough surface.