Angiofibromas
Christopher G. Bunick
Amanda Zubek
Macrene Alexiades
BACKGROUND
Angiofibromas are benign papules that typically present on the face of children or adults. When multiple, they may be associated with an underlying medical or genetic condition. Angiofibromas are extremely common in the general population. When they are solitary or few on the nose they are also referred to as benign fibrous papule of the nose. When present on the corona of the glans penis, they are referred to as pearly penile papules.
PRESENTATION
Patients present with a complaint of bumps or red to flesh-colored growths typically on the face. They are slow growing and may remain stable in size for many years.
DIAGNOSIS
Clinical Diagnosis
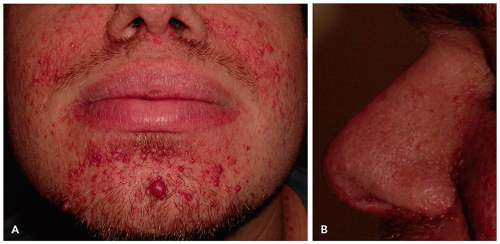
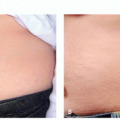
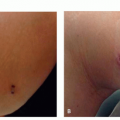
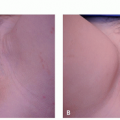
Angiofibromas present as small (˜0.1-0.4 cm), round to dome-shaped, skin-colored to pink-red papules usually located on the face (Figure 11.1.1A). They involve the nose and medial cheeks most commonly (Figure 11.1.1B).1 The clinical approach to angiofibromas starts with understanding whether the patient has a “solitary angiofibroma” or “multiple angiofibromas.” Solitary angiofibromas are benign and usually unassociated with systemic disease; they are commonly referred to as “fibrous papules” or “benign fibrous papules of the nose.” They can mimic benign nevi of the face and be difficult to distinguish from basal cell carcinoma. Multiple angiofibromas, however, are a clinical sign of possible systemic disease.2 The classic triad of systemic diseases that involve multiple facial angiofibromas are tuberous sclerosis (TSC), multiple endocrine neoplasia 1 (MEN1), and Birt-Hogg-Dube syndrome (BHDS). Figure 11.1.1 shows patients with tuberous sclerosis with multiple angiofibromas on the face.
Histopathology
Histologic examination of angiofibroma demonstrates ectatic superficial vessels in a fibrotic stroma consisting of increased fibroblasts with periadnexal and perivascular lamellar collagen fibers.3
Subtypes
Sporadic
Fibrous papule
Pearly penile papule
Genetic
Multiple angiofibromas (TSC, MEN1, BHDS)
Periungual fibroma (TSC)
Differential Diagnosis
Basal cell carcinoma
Intradermal nevus
Trichofolliculoma
Desmoplastic trichoepithelioma
Hemangioma
Rosacea
Condyloma acuminatum (when on the genitalia)
Periungual verruca
Periungual fibrokeratoma
PATHOGENESIS
Studies of both solitary and multiple angiofibromas indicate that the mTOR signaling pathway plays a pathogenic role in the formation of the cutaneous lesions. In the case of tuberous sclerosis, TSC1 (hamartin) and TSC2 (tuberin) act as tumor suppressors of mTOR; but when TSC1 or TSC2 are mutated, mTOR activity is no longer checked and a progrowth environment ensues, leading to hamartomatous tumors. Recent analysis of solitary angiofibromas demonstrated high levels of phosphorylated mTOR expression in dermal stromal cells and epidermal keratinocytes, similar to that from TSC-associated angiofibromas.4
TREATMENT
Because angiofibromas are benign, some patients will find clinical observation and reassurance are the best treatment for them. For those who have symptomatic or cosmetically unacceptable lesions, there are a number of therapies available to consider, including surgical, topical, and laser-based therapies (Algorithm 11.1.1). Bedside surgical procedures that can be done in a matter of minutes are cryotherapy, shave excision, punch biopsy, or curettage. The last method can be coupled with electrodessication when needed. A more extensive treatment, especially when treating multiple lesions, is dermabrasion. Patients with either solitary or multiple angiofibromas could benefit from topical therapies. The topical therapy most directly targeting the pathogenic mechanism of angiofibromas is the use of an mTOR inhibitor (eg, rapamycin/sirolimus).5 There is report of successful treatment with topical podophyllin as well.6 Lasers can be used to destroy angiofibromas, with the carbon dioxide (CO2) laser producing excellent results.7 With any of these therapies, there are risks: scarring, infection, bleeding, and pigmentary changes.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree