Anterior Cruciate Ligament Reconstruction With Open Physis and Closed Physis
Mininder S. Kocher
Physeal-Sparing Combined Intra-articular and Extra-articular Technique With IT Band
Operative Indications
Anterior cruciate ligament (ACL) reconstruction is indicated in full-thickness intrasubstance ruptures regardless of physeal status
It is preferable to perform ACL reconstruction in patients with open physes rather than waiting for skeletal maturity as this approach has been associated with an unacceptably high rate of meniscal and chondral injury
ACL reconstruction is also indicated in patients that have failed conservative treatment of ACL injuries due to either recurrent instability or the presence of other intra-articular injury such as meniscal tears or cartilage injuries
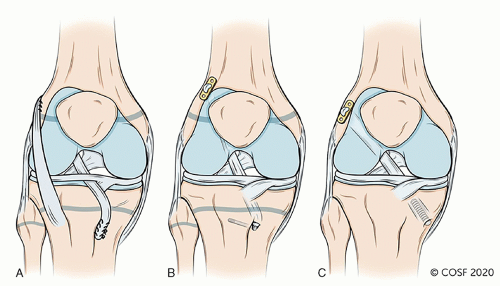
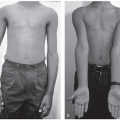
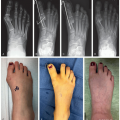
The combined extra-articular and intra-articular ACL reconstruction described below is indicated in patients at Tanner stage 1 or 2 and those with skeletal bone age ≤11 in females or ≤12 in males (Figure 31.1)
Transphyseal, all-epiphyseal, or hybrid reconstruction techniques are acceptable in older patients
Equipment
Knee arthroscopy equipment
Small joint equipment may be required for especially small patients
Cobb elevator
Meniscotomes (right, left, and end cutting)
Full-length curved clamp
Rat-tailed rasp
Periosteal elevator
Examination Under Anesthesia
Flexion and extension range of motion
Lachman examination
Pivot shift maneuver
Varus/valgus stress, posterior drawer, and dial test to rule out other injuries
Positioning
Position the patient supine on the operating room table with all bony prominences well padded
A nonsterile tourniquet is placed as high as possible on the thigh to allow enough room to harvest a 15-cm iliotibial band (ITB) graft
An arthroscopic leg holder or lateral post can be used to allow access to the medial compartment based on surgeon preference
Technique
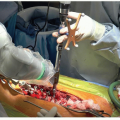
ITB Graft Harvest
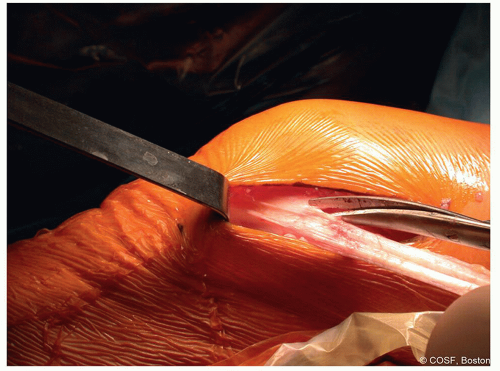
Make a 6-cm incision obliquely from the lateral joint line to the anterior border of ITB (Figure 31.2)
Use a Cobb elevator to separate the ITB from the superficial soft tissues
Incise the ITB in line with its fibers a few millimeters posterior to the anterior border of the ITB
Repeat this process just anterior to the posterior border of the ITB
Extend both ITB incisions proximally for 15 cm with the use of meniscotomes
Ensure the splits stay parallel to the fibers of the ITB so the graft is not prematurely transected
Use a curved, end-cutting, meniscotome to release the graft as proximally as possible
A cutting tendon stripper can be used if the graft is small enough to fit in the device
A counter incision can also be made proximally to release the graft under direct visualization
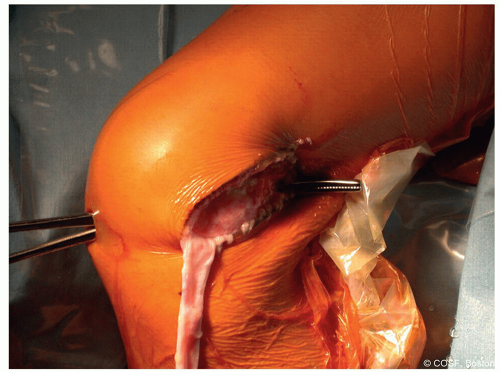
Distally, use scissors to continue the anterior and posterior incisions in the ITB to Gerdy tubercle (Figure 31.3)
Tubularize and whip stitch the proximal free end of the graft with heavy nonabsorbable suture
Place the graft under skin to prevent desiccation while performing the intra-articular portion of the procedure
Diagnostic Knee Arthroscopy
Standard anterolateral and anteromedial portals are created
The anteromedial portal, which will facilitate graft passage, can be created slightly distal and medial to the typical position to provide a better trajectory for passing the clamp around the “over-the-top” position
A complete diagnostic arthroscopy should be completed
Any intra-articular injuries such as meniscal or cartilage injuries should be addressed at this point
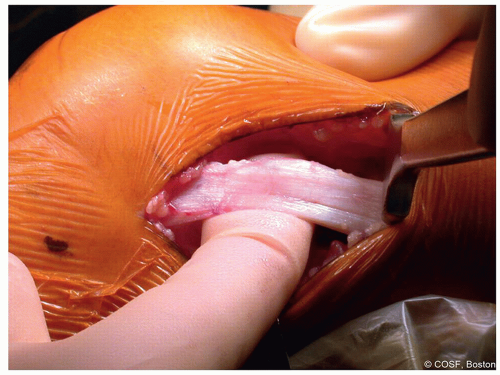 Figure 31-2 ▪ The iliotibial band is harvested through an oblique lateral knee incision. (Courtesy of Children’s Orthopaedic Surgery Foundation.) |
Femoral Graft Passage
Insert the tips of a full-length clamp through the anteromedial portal
The tips of the clamp are passed posterior and cranial to the ACL footprint around the lateral femoral condyle in the “over-the-top” position (Figure 31.4)
A portion of the soft tissues at the ACL femoral footprint should be preserved to act as a sling to prevent inferior subluxation of the graft
The tips of the clamp should be identified through the lateral open incision within the anterior and posterior borders of the ITB (Figure 31.5)
The clamp is then used to withdraw the ITB graft into the knee joint (Figure 31.6)
Tibial Bed Preparation
A 3 to 4 cm incision is made over the proximal tibia medial to the tibial tubercle and distal to the proximal tibial physis
Carry the dissection down to the periosteal layer and incise the periosteum in line with the incision
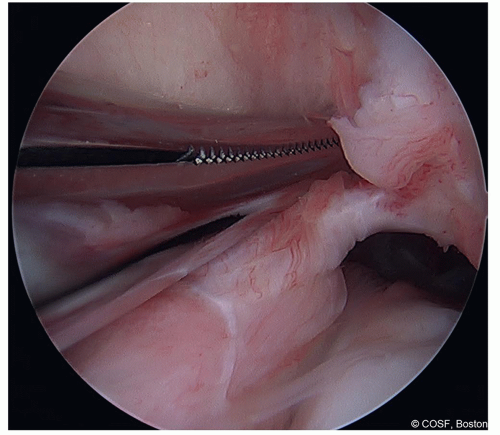
Figure 31-4 ▪ The tips of a full-length clamp are passed around the lateral femoral condyle in the “over-the-top” position. (Courtesy of Children’s Orthopaedic Surgery Foundation.)
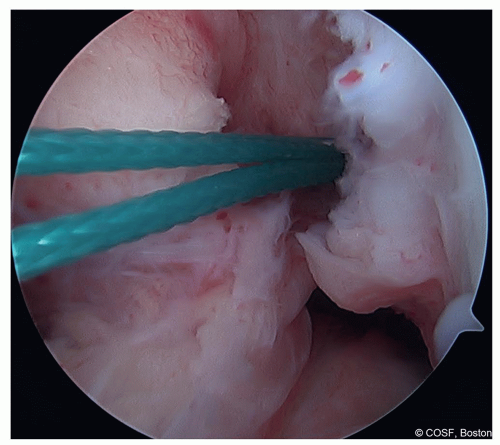
Figure 31-6 ▪ The sutures of the graft are brought into the knee joint through the over-the-top position. (Courtesy of Children’s Orthopaedic Surgery Foundation.)
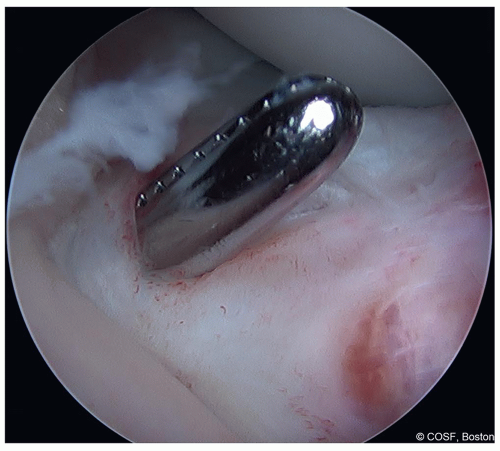
Figure 31-7 ▪ From the tibial incision, the clamp is passed into the knee joint under the intermeniscal ligament. (Courtesy of Children’s Orthopaedic Surgery Foundation.)
Use a periosteal elevator to create flaps medial and lateral to the periosteal incision
Take care laterally not to violate the tibial tubercle apophysis
A burr or rasp can be used to decorticate the proximal tibial bed to facilitate tendon to bone healing
Tibial Graft Passage
Insert a curved clamp through the tibial incision into the knee joint under intermeniscal ligament (Figure 31.7)
From the tibial incision, the proper trajectory is typically aimed at the anteromedial arthroscopic portal
After confirmation that the clamp is intra-articular and under the intermeniscal ligament, spread the tips of clamp to create a path for the graft
Remove the clamp and replace in the same trajectory with a rat-tailed rasp (Figure 31.8)
Again, ensure the rasp is under the intermeniscal ligament
Use the rasp to create a groove in the epiphysis, which will allow the graft to sit further posterior, more closely approximating the tibial ACL footprint
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree