Child Abuse
Child abuse is a broad term used to describe a spectrum of nonaccidental trauma inflicted upon children. Kempe et al. are generally credited with emphasizing the prevalence and importance of this entity when they coined the term battered child syndrome in 1962. This “syndrome” has subsequently been expanded to include an array of childhood abuses including physical abuse, sexual abuse, and neglect. Child abuse continues to be one of the most significant causes of childhood morbidity and mortality in the United States. In one 10-year study of medical records submitted to the National Pediatric Trauma Registry, child abuse accounted for 10.6% of all blunt trauma to patients under 5 years of age. Children who are abused tend to be younger, with the highest incidence seen in those under 3 years of age. High-risk groups include children with a history of prematurity, physical handicap, and behavioral problems. Factors that appear to be associated with an increased risk of abuse are summarized in Table 26-1 . Up to 75% of abuse may be missed in the acute care setting because of failure of recognition by medical professionals, and this may lead to lost opportunities to intervene.
| Child | Parent | Both |
|---|---|---|
| Prematurity | Partner violence within the family | Neighborhood factors |
| Mental retardation | History of past abuse or neglect | Crime |
| Disability | Substance abuse | Poor recreational activities |
| Congenital anomalies | Mental illness | Poverty |
| Clinging | Unemployment | Poor parent–child relationships |
| Excessive or inconsolable crying | Lack of external support | Substandard housing |
| Expectations inconsistent with normal child development | African-American child in single-parent household | Poor impulse control |
| Toilet training or toilet accidents (preschoolers) | Adolescent in age | Rely on children for emotional support |
Various abusive patterns may be evident in families where abuse is an issue. These include parents who were the victims of abuse themselves, parents with emotional disturbances, stressful crises within the family unit (i.e., loss of job or financial distress), and lack of a close support network for the family (see Table 26-1 ). Recognition of abuse is vital, because the trauma tends to be repeated (an abused child has up to a 50% chance of being abused again), and the risk of future injury or death is high. Instances in which there is a delay in reporting the injury, in which the degree and type of injury are at variance with the history offered, or in which the parents are evasive or vague as to the cause of injury are all suspicious and should lead to consideration for an abuse investigation. In evaluating the child with possible abuse, a detailed history is the most important component of the assessment. Vital details include the alleged mechanism of the injury, developmental history of the child, past medical history (especially of any disorders that may mimic abuse, such as coagulopathy or skin disorders), history of prior injuries, social history, and family history. A complete physical examination should be performed and should include high-quality photography of cutaneous lesions.
Radiographic findings in child physical abuse are often useful in the evaluation and are not discussed in great detail here. Findings that may increase suspicion for abuse include the classic metaphyseal lesion (also known as “corner fracture” or “bucket-handle fracture”), skull and femur fractures, and healing fractures, although each of these findings must be considered in the appropriate context of the medical history and physical examination findings.
Although abused children may exhibit multiple abnormalities on physical and radiographic examination, this section will focus primarily on the cutaneous stigmata.
Physical Abuse
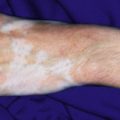
Nonaccidental injuries in children may take many forms, and often the skin reveals pathologic findings. Cutaneous trauma may be seen in the form of ecchymoses, burns, lacerations, bite marks, abrasions, underlying hematomas, pigmentary changes, and scars.
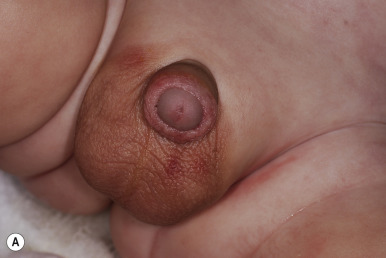
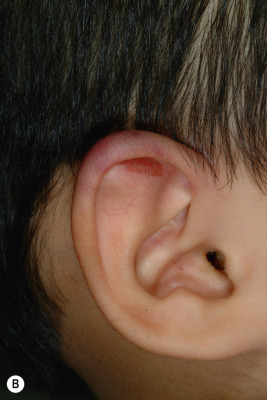
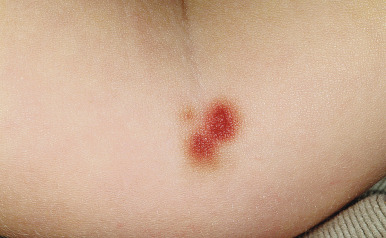
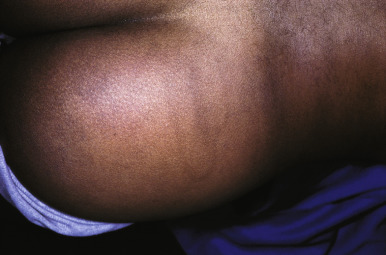
Ecchymoses (bruises) are the most common type of skin injury seen in children who have been abused. Lesions on the hands and face, adult human bites, and lesions on the cheeks, mouth, lips, lower back, buttocks, or inner thighs are particularly suspect. Ecchymoses in various different stages of healing are more suggestive of abuse. Ecchymoses on padded areas such as the buttocks, torso, face, and genitalia ( Fig. 26-1, A ) or uncommonly injured areas (earlobe, neck, lip, philtrum) are more concerning for possible abuse. In a study of discriminating bruising characteristics in children who have been abused, characteristics that were more predictive of abuse included bruising on the torso, ear ( Fig. 26-1, B ), or neck (in a child ≤4 years of age, termed the TEN region ) and bruising in any region in an infant younger than 4 months of age. Abuse-associated bruising should be differentiated from accidental bruising, which is more common in ambulatory children and occurs most commonly over bony prominences such as the forehead and shins. Any bruising in the noncruising infant under 9 months of age should raise significant suspicion for abuse. There are many potential mimics and non-abuse-related causes of ecchymoses, including Mongolian spots, hypersensitivity vasculitis (i.e., Henoch–Schönlein purpura or acute hemorrhagic edema of infancy), Ehlers–Danlos syndrome, vascular malformations, infantile hemangiomas, inks or dyes, and bleeding disorders.
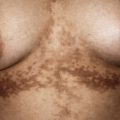
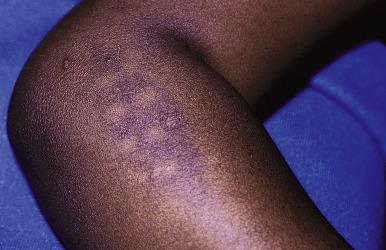
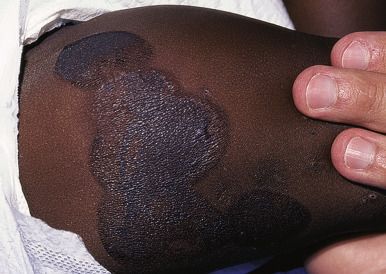
The configurations of lesions in battered children are morphologically similar to the items or methods used to inflict the trauma and may be useful in the abuse investigation. Multiple evenly spaced markings ( Fig. 26-2 ) or curvilinear loops and arcuate lesions ( Figs. 26-3 and 26-4 ) such as those that may be induced by lashing with a doubled-over belt or electric cord are typical of these trauma-induced lesions. They are usually ecchymotic, but they may also present as abrasions, lacerations, or hyperpigmentation.
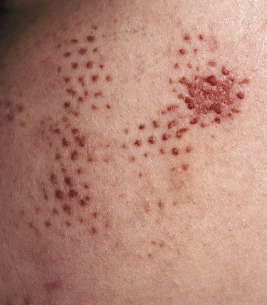
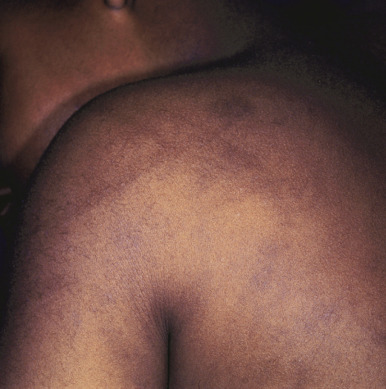
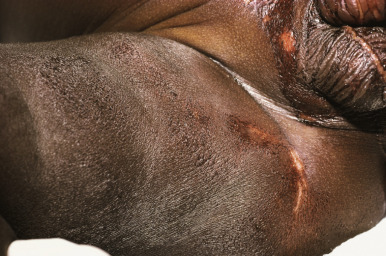
Belt-buckle imprints (ecchymotic or hyperpigmented) may result from intentional trauma with these items. Adjacent, small ecchymotic macules ( Fig. 26-5 ) are typical of pinch marks. Shackles on the wrists, ankles, or neck leave easily identifiable rings that are red if fresh and hyperpigmented if longstanding. Ligature marks on the neck or extremities and grab or slap marks (fingertip bruises; Fig. 26-6 ) on the shoulders, hands, or legs are particularly suspicious and highly suggestive of deliberate trauma. Slapping injuries result in linear bruising that outlines the blunt objects (fingers) because of the breakage of superficial skin capillaries. Çao gio (“coining”) and cupping, Asian customs believed to treat a variety of ailments, may be confused with ecchymotic lesions of abuse and must be appropriately recognized (see below in Cutaneous Mimickers of Abuse and Factitial Disorders section).
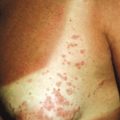
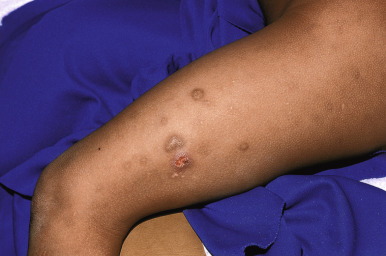
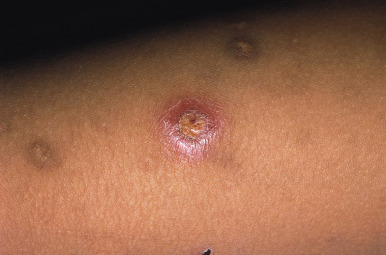
Burns are a very common type of injury seen in abused children and result from thermal injury to the skin and subcutaneous tissues. Burns can also be electrical, chemical, or radiant in nature. Thermal burns may be inflicted with cigarettes, matches, scalding liquid, or other heated objects ( Fig. 26-7 ) and are often mistaken for lesions of impetigo. Cigarette burns present as 8- to 10-mm, deep, round crusted ulcers that heal with scars and pigmentary changes ( Figs. 26-8 and 26-9 ). Although they may be accidental, multiple lesions with deeper involvement and significant scarring are highly indicative of abuse, because this pattern is usually suggestive of prolonged contact. The differential diagnosis of cigarette burns includes ecthyma, cellulitis, herpes, and bullous impetigo.

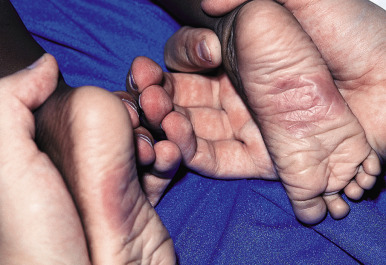
Branding injuries occur after prolonged contact with a heated object, and they may take on the shape of the object used to inflict them. Burns inflicted with a hot iron ( Figs. 26-10 and 26-11 ) reveal differing pigmentary changes between the heated metal surface and the steam vent openings. Figures 26-12 and 26-13 demonstrate burns inflicted by a heated metal spoon, with the shape of the spoon readily visible in the resultant skin markings. Dunking scald injuries are most commonly seen in infants and toddlers and present with a characteristic “stocking and glove” distribution on the extremities or with “doughnut-type sparing” that occurs when the child’s buttocks are held against the cooler tub or basin. These patients have erythema and blistering indicative of a second-degree burn. It should be remembered that children will not stay in contact with a hot surface or scalding hot water. They normally test the heat of the water and step into the bath with one foot at a time. Accordingly, symmetrical burns on the feet, the buttocks, or the hands require careful investigation and evaluation. Stun-gun injuries have been observed in the setting of physical abuse and present as evenly spaced (4 to 5 cm apart), erythematous to hypopigmented papules and macules, usually occurring in multiples.
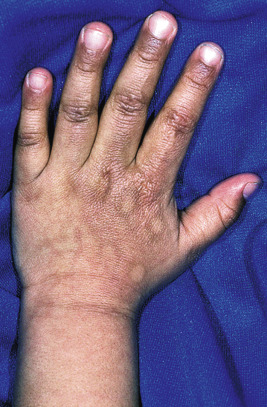
Bite marks are another pathognomonic sign of nonaccidental trauma. The human bite is differentiated easily from the dog bite by the contusing and crushing characteristics of the latter; dog bites rip and tear the flesh. It is important to distinguish adult from child bite marks, since the former is more likely to be seen in an abusive setting. Adult bites are characterized by a dental arch width greater than 4 cm 3 , whereas the markings of a child’s bite tend to be significantly narrower ( Fig. 26-14 ). The discovery of one bite mark necessitates a thorough examination of the child’s entire body for further evidence of bites or other findings of abuse. Traumatic alopecia may occur when the parent pulls the child’s hair, since the hair provides a readily accessible “handle” that can be used to grab or jerk at the child. The resultant alopecia is an irregularly bordered area that may reveal hemorrhage, hair breakage, and scalp tenderness.
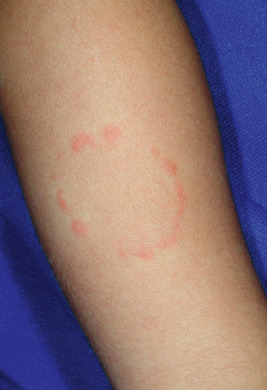
Oral injuries are another common feature in abused children. Findings may include tears of the labial or lingual frenulum caused by a blow to the mouth, forced feeding, or forced oral sex. Other manifestations include burns or lacerations of the gingivae, tongue, or palate from overly hot food or utensils. Teeth may also be involved, including fracture, displacement, or avulsion.
A difficult situation arises when the physician observes recent skin injuries in the child who does not seek treatment for trauma. In one large series, 76% of children between 9 months and 17 years of age seen in a clinic for a reason other than trauma were found to have at least one recent skin injury. Injuries were more prevalent in the summer (in regions with a temperate climate) and were most commonly observed on the shins and knees. The authors offered certain unusual characteristics that may suggest a greater risk of physical abuse (or bleeding disorder), and these include uncommon location, more than 15 injuries, bruises in a child younger than 9 months of age, numerous injuries elsewhere than the lower limbs, numerous injuries in cold seasons in a temperate climate, and injuries other than bruises, abrasions, or scratches. In another series of infants aged 6 to 12 months, bruises were noted to be generally limited to the face, head, or shins, and there was a direct correlation between the number of bruises and increases in mobility. In this group, the prevalence rate of bruises was 12%, and they were most often solitary.
Sexual Abuse
Sexual abuse has been defined in many ways, including “any exploitative sexual activity between a child and an adult”; “any sexual activity that a child cannot comprehend or give consent to, or that violates the law”; or “when a child is engaged in sexual activities that he/she cannot comprehend, for which he/she is developmentally unprepared and cannot give consent, and/or that violates the law or social taboos of society.” Some studies have suggested that 1% of children experience some form of sexual abuse each year. It is important to realize that boys may be the victims of sexual abuse as well as girls, although the former tend to be less likely to disclose abuse, and thus it is likely underreported, underrecognized, and undertreated. Adolescents are the perpetrators in up to 20% of reported cases of sexual abuse, and although women may be perpetrators, these allegations are significantly less likely than those involving males. Up to one fifth of adolescents who regularly use the Internet have been solicited by strangers for sex through the Internet. Childhood sexual abuse may lead to a variety of physical and mental symptoms and disorders, including depression, suicidal ideation, eating disorders, low self-esteem, and posttraumatic stress disorder.
The perpetrator of childhood sexual abuse is often well known, or related, to the victim. Activities involved in sexual abuse may include oral–genital, genital, or anal contact by or to the child, as well as nonphysical abuses such as voyeurism, exhibitionism, or involvement of the child in pornography. Sexual abuse should be differentiated from “sexual play” or age-appropriate exploratory behavior. The child who has been sexually abused may exhibit a variety of features including behavioral changes, school difficulties, regression, depression, eating disturbance, sexual acting-out, symptoms referable to the genitourinary or gastrointestinal tracts, pregnancy, various somatic complaints, or a sexually transmitted disease (STD).
Mucocutaneous findings suggestive of sexual abuse are listed in Table 26-2 . However, it should be noted that many children who have been sexually abused in the past may have a relatively normal physical examination. Many prepubescent patients seen in emergency departments for a sexual-abuse evaluation have not experienced recent abuse, in distinction to adolescents, who often come after the acute assault. A normal anogenital examination, therefore, does not preclude prior sexual abuse. The physical examination should be most focused on areas involved in sexual activity, including the mouth, breasts, genitals, perineum, buttocks, and anus. In females, a more thorough examination of the medial thighs, labia majora and minora, clitoris, urethra, hymen and hymenal opening, fossa navicularis, and posterior fourchette should be included. In males, the thighs, penis, and scrotum should be closely examined.
| Finding | Comment |
|---|---|
| Hymenal changes | Attenuated hymenal tissue, disruption of hymenal contour; acute laceration or ecchymosis |
| Anal area changes | Boys and girls; changes in anal tone, hematomas, abrasions, lacerations; scarring, skin tags; dilation |
| Fossa navicularis scarring | |
| Posterior fourchette scarring | |
| Inner thigh changes | Abrasions, ecchymosis (concerning but not diagnostic) |
| Labia minora changes | Scarring or tears (concerning but not diagnostic) |
| Other genital injuries | Circumferential injuries to penile shaft or glans penis |
| Oral injuries or diseases | Unexplained erythema or petechiae of the palate; oral or perioral gonorrhea or syphilis (pathognomonic for sexual abuse in the prepubertal child) |
Examinations for STDs should be performed when indicated. Factors to be considered include the possibility of oral, genital, or rectal contact and the child’s symptomatology. Table 26-3 summarizes the implications of various STDs and clinical findings for reporting childhood sexual abuse. Anogenital warts, which may be sexually transmitted in children, are often the result of benign, nonsexual transmission, especially in infants and young toddlers (see Chapter 15 ). Nonsexual modes of transmission include perinatal transmission, autoinoculation (child with common warts spreads them via skin-to-skin contact to his or her own anogenital region), heteroinoculation (caregiver with common warts spreads them via skin-to-skin contact to anogenital region of child), and possibly indirect spread from fomites. Importantly, molluscum contagiosum lesions involving the anogenital region in children are nearly always a result of benign transmission or autoinoculation and should not be considered as indicative of childhood sexual abuse. The details of the evaluation, treatment, and reporting of childhood sexual abuse are beyond the scope of this chapter but are well documented elsewhere. Importantly, however, when the diagnosis of childhood sexual abuse is being considered, review of the case with an expert in such evaluations (such as a child-abuse pediatrician) is advisable. Recent data suggest that five or more examinations per month may be required for ongoing competency in the interpretation of medical and laboratory findings in children in whom sexual abuse is suspected.
| STD or Finding | Implication for Abuse | Suggested Action |
|---|---|---|
| Gonorrhea * | Diagnostic | Report |
| Syphilis * | Diagnostic | Report |
| HIV infection * , † | Diagnostic | Report |
| Chlamydia * | Diagnostic | Report |
| Trichomoniasis | Highly suspicious | Report |
| Anogenital warts * , ‡ | Suspicious | Report |
| Genital herpes § | Suspicious | Report |
| Bacterial vaginosis | Inconclusive | Clinical follow-up care |
| Presence of sperm, semen, or acid phosphatase | Diagnostic | Report |
| Pregnancy | Diagnostic | Report |
* If not perinatally acquired.
† If not transfusion acquired.
‡ Not uncommonly transmitted via benign mode; see discussion in Chapter 15 .
Neglect
Neglect may be either physical, emotional, or both. The former results when a parent or caretaker fails to provide necessities of life such as food, appropriate supervision shelter, clothing, or medical care. General findings in the neglected child may include lack of immunizations, poor nutrition and growth, and developmental or behavioral problems. Potential cutaneous findings include poor hygiene, untreated injuries, infections, and infestations. Severe or extensive sunburns ( Fig. 26-15 ) may be a sign of parental neglect, although several conditions and medications may make children more sensitive to ultraviolet light. It is important to bear these in mind whenever the possibility of neglect or abuse is being considered.
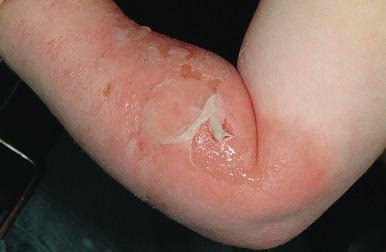
Physical neglect may also present as dental neglect, which is defined as the “willful failure of parent or guardian to seek and follow through with treatment necessary to ensure a level of oral health essential for adequate function and freedom from pain and infection.” Findings may include dental caries, periodontal disease ( Fig. 26-16 ), and other oral conditions. When left untreated, these conditions can lead to significant pain, infection, and loss of function.
Factitial Skin Disorders
Factitial skin disorders (also called self-inflicted skin lesions ) are a group of disorders characterized by self-inflicted lesions or artifacts on the skin. The individual cases vary in terms of the visible lesions and the underlying motive that causes the patient to act. These disorders may be associated with a variety of psychopathologic conditions, and comanagement with a psychologist or psychiatrist is often necessary. Factitial skin disorders fall under the rubric of psychodermatologic conditions or psychocutaneous disorders, although these two classifications also include dermatologic conditions with secondary psychiatric sequelae (i.e., alopecia areata or albinism) and dermatologic conditions that may be aggravated by psychologic factors (i.e., acne, atopic dermatitis, psoriasis). Diagnosis of factitial skin disorders is often delayed, and management is challenging, requiring the development of a therapeutic alliance between the physician and patient and treatment of any underlying psychiatric comorbid conditions. The diagnosis of factitial skin disorders largely remains a diagnosis of exclusion. Treatment often requires a multidisciplinary approach that may include the pediatrician, dermatologist, psychologist, and/or psychiatrist.
Factitious Dermatitis/Dermatitis Artefacta
Factitious dermatitis is one type of factitious disorder that is caused by a conscious or subconscious behavior driven in response to internal psychologic stressors and not associated with secondary gain. Dermatitis artefacta ( DA ) is often the terminology used to describe a disorder in which the skin is the purposeful target of self-inflicted injuries. In DA, the patient creates the lesions on the skin in order to satisfy a psychological need (of which he or she is often not consciously aware) and in the pursuit of secondary gain. There appears to be the need to satisfy an internal emotional necessity—the need to be cared for. The desired gain may be obvious or may not be readily evident. DA occurs predominantly among women, with a wide range in the quoted ratios of women to men, from 3 : 1 to 20 : 1. It may have its onset at any time, although it most commonly occurs in teenagers and young adults. When it occurs in children, DA may be related to various stressors including school examinations, bullying, and discord in the home. Several comorbid conditions may be present, including borderline personality disorder, disorders of impulse control, depression, anxiety, obsessive-compulsive disorder (OCD), and psychotic disorders. It may also result from a transient maladaptive response to a recent psychosocial stressor(s). A past and/or current history of sexual abuse is common. Patients with DA often have a close connection (either personally or through a close family member) with the healthcare field, and many have an “encyclopedic” grasp of medical knowledge and/or terminology. Some have suggested abandoning the terms factitial dermatitis and DA in favor of the terminology factitious disorders in dermatology .
DA has a variety of presentation patterns. Importantly, the cutaneous features are often only one facet of the entire picture, because these patients often have involvement of other organ systems and have visited numerous medical specialists for other bizarre or unexplained symptoms. The skin lesions themselves may consist of purpura, excoriations, abrasions, crusting, necrosis, blisters, ulcers, erythema, nodules, or scarring. When blisters are present (bullous DA), modes of injury often include thermal, electrical, or chemical injury. The lesions of DA usually lack features of recognizable dermatoses. Notable features often include linearity, geometric arrangements, and sharp demarcation from the surrounding normal skin. The face, upper trunk, and upper extremities are the sites most often involved, and there is notable sparing of areas outside of the patients’ reach (i.e., the middle back). There is often a prominence on one side, depending on the handedness of the patient. The lips may also be involved, presenting usually as persistent bleeding and crusting. The lesions are often fully formed and are all in a similar stage of development. This inability of the patient to give details of evolutionary change has been termed hollow history and is quite typical of DA.
Reported modes of injury include rubbing; scratching; picking; cutting; gouging; pinching; puncturing; biting; sucking; applying suction; applying heat, dye, or caustic substances; and injecting caustic materials or bodily secretions. The differential diagnosis may be broad and depends on the nature of the inflicted injury. A clue to the diagnosis of DA is indifference or lack of concern on the part of the patient, who will often deny pain or discomfort despite the impressive physical findings. Bullous DA caused by thermal injury may result after the “salt and ice challenge,” a trending dare contest in which participants sprinkle salt on the skin followed by compression with an ice cube.
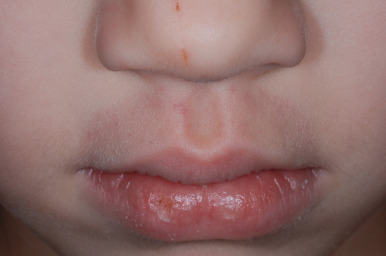
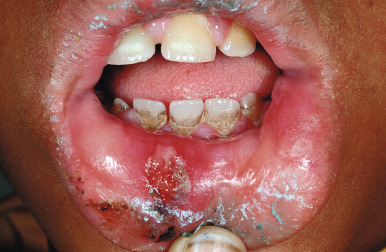
Factitious purpura, which is a form of mechanical purpura, may result in a detailed, lengthy investigation for other medical causes before the diagnosis is entertained. Patients may be entirely unaware that they are causing the skin lesions. A common form of factitious purpura is that caused by sucking air from a drinking glass placed over the chin and lower lip, resulting in a well-demarcated, circular area of purpura ( Fig. 26-17 ). Other forms may be caused by a variety of instruments or objects, with the purpuric lesions corresponding to the patterns of those objects. Figures 26-18 through 26-30 depict some various presentations of DA.