Introduction
Acute renal dysfunction represents a critical complication of an acute thermal injury and is associated with a significant increase in morbidity and mortality. Currently, the incidence of acute renal failure (ARF) in burn patients varies between 0.5% and 30%, and the risk of mortality associated with renal failure in burn patients has been reported to be as high as 40% to 100%.
Prior to 1965, there were no reported survivors from ARF following a thermal injury. Although there has been marked progress in the management of renal dysfunction, the exact mechanisms to avoid permanent dysfunction and an exact way to attenuate injury remain undiscovered. Even renal replacement therapy (RRT), one of the core milestones of modern medical progress, has yet to show a significant improvement in the mortality rate of burn patients suffering from ARF.
This chapter will review the definition, etiology, pathophysiology, diagnosis, and treatment of ARF in association with thermal injury ( Fig. 25.1 ).
Autopsy specimen from a patient with acute tubular necrosis and renal failure. Note the edema and the alteration of medullar pyramids. Acute renal failure in burn patients carries a high mortality.
Definition
Until 2004, with no consensus regarding a definition for ARF, more than 30 different definitions were used within the literature to define failure. The RIFLE criteria, established in 2004, divided renal compromise into five discrete categories (risk, injury, failure, loss, end-stage renal disease) ( Table 25.1 , Fig. 25.2 ) and provided a means to quantify grades of acute kidney injury (AKI). , In 2007, the definition simplified the stratification of renal injury into three stages (I, II, and III), with the RIFLE’s failure, loss, and end-stage renal disease categories folded into grade III. In 2012, the Kidney Disease Improving Global Outcomes (KDIGO) Acute Kidney Injury Work Group published a consensus definition of renal injury that essentially merged the two previous frameworks, with slight adjustments.
Table 25.1
Comparison of Serum Creatinine Criteria in RIFLE, AKIN, and KDIGO Systems
From Brochard L, Abroug F, Brenner M, et al. An official ATS/ERS/ESICM/SCCM/SRLF statement: prevention and management of ARF in the ICU patient: an international consensus conference in intensive care medicine. Am J Respir Crit Care Med . 2010;181(10):1128-1155. Updated with current reference to published KDIGO guidelines.
| SERUM CREATININE CRITERIA FOR THE DEFINITION AND CLASSIFICATION OF ACUTE KIDNEY INJURY | ||||
| RIFLE Criteria—Acute Dialysis Quality Initiative (ADQI) | AKIN Criteria—Acute Kidney Injury Network | KDIGO Criteria—Kidney Disease Improving Global Outcomes | ||
| Risk |
|
|
|
Stage I |
| Injury |
|
|
|
Stage II |
| Failure |
|
|
|
Stage III |
Note: Urine output-based criteria are the same in all three systems.
Multifactorial etiology of sepsis-induced acute renal failure. cGMP , Cyclic guanosine monophosphate; iNOS , inducible nitric oxide synthase.
While the proliferation of consensus definitions may seem to undermine the basic goal of establishing a universal metric for research and clinical applications, the three systems have proved fairly interchangeable. Multiple studies applying the different scoring systems to the same patient populations have found that they ultimately yield similar results. , Specifically in burn populations, Chung et al. found that RIFLE and the Acute Kidney Injury Network identified similar subpopulations when applied to a large cohort of patients. Despite this complex history, over the past decade, the KDIGO definition of renal injury has emerged as the clear consensus standard definition for renal failure in contemporary burn care.
Etiology
Burn-associated AKIs can generally be divided into two categories: early and late. Early occurring AKI presenting within the first 48 hours of the burn injury typically results from uncontrolled burn shock through underresuscitation. Later occurring AKI presents often after operative intervention or more than 72 hours postburn, and typically stems from sepsis via infections or iatrogenic means such as medication toxicity or large volume loss.
Early acute kidney injury
Within the first 24 to 28 hours of a massive burn injury, AKI results from the pathologic response to thermal injury. Early burn-associated AKI is multifactorial; hypovolemia and inflammatory mediators cause extensive tissue destruction, there is release of denatured proteins, iatrogenic causes from management (i.e., nephrotoxic agents) manifest, and cardiac dysfunction all contribute to this renal insult. Literature suggests that AKI happens relatively quickly in the early postburn time frame occurring within the early burn time frame. In the setting of delayed resuscitation, hypovolemia is the most immediate threat to renal function. Perhaps more perplexing is that AKI can still develop in the thermally injured patient despite aggressive fluid resuscitation and a normal urine output. It is in these situations that both endogenous (i.e., denatured proteins) and exogenous (i.e., medications) factors as a response to burned tissue may play a role. Although not a typical presentation within the early time frame of 48 hours, sepsis from infection must also be considered. Please see the late kidney injury section where infection is discussed further.
Hypovolemia
In large surface area burns, decreased renal blood flow results from massive fluid shifts and losses. Local and systemic cytokine release leads to capillary leak, shifting fluids from the intravascular to interstitial space. Burn-induced compromise of the watertight dermal barriers results in rapid evaporative losses from the extravascular compartment, which facilitates further extravasation of the intravascular compartment in a vicious cycle. Given the sheer speed and volume fluid shift seen in burn shock, profound intravascular hypovolemia can result. Renal blood flow is restricted in a compensatory response to hypovolemia resulting in renal ischemia. The ischemic insult is known to produce oxygen free radicals that cause direct tubular damage as well as disruption of tight junctions, resulting in obstructing casts that further reduce effective glomerular filtration rate (GFR).
Hypovolemia can develop within the course of minutes in the absence of appropriate fluid replacement. As such, hypovolemia represents by far the most likely source of AKI in any burn patient showing signs of renal insult within 24 hours of the burn.
Overresuscitation and abdominal compartment syndrome
Unfortunately, overadministration of fluids can be just as harmful as underresuscitation. The mechanisms for which this occurs at the cellular level are becoming better understood and may be related to destruction of the endothelial glycocalyx layer. On a systemic level, studies have shown that AKI can develop in burn patients despite fluid resuscitation volumes in excess of that recommended by the Parkland formula and despite normal average urine output (0.5–1 mL/kg/hour). , Furthermore, the risks of overresuscitation have been well documented and include pneumonia, acute respiratory distress syndrome, compartment syndromes, and an overall increase in mortality. ,
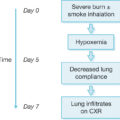
Despite the physician’s greatest effort to monitor end points of resuscitation, obligatory intercompartmental fluid shifts will occur during resuscitation. These intercompartmental fluid shifts can be particularly hazardous if they occur into fascial bound compartments, such as the peritoneal cavity. Numerous studies from trauma literature have described the adverse physiologic effects of increasing intraabdominal pressure (IAP) on visceral perfusion. , , Intraabdominal hypertension (IAH) is a known pathologic process that may occur during initial burn resuscitation as defined by IAPs greater than 12 mmHg. Abdominal compartment syndrome (ACS) is defined as an IAP of greater than 20 mmHg with at least one concomitant organ failure, such as renal, liver, and pulmonary dysfunction. The exact level of abdominal hypertension required to compromise visceral perfusion varies depending on a variety of patient factors and is difficult to predict but is related to impaired capillary flow from arterial to venous circulation. O’Mara et al. demonstrated that the volume and type of fluid resuscitation affect the development of ACS in the burn patient and suggested that fluid resuscitation with crystalloid of greater than 0.475 L/kg should alert the clinician to possible IAH/ACS and to monitor for decreased cardiac output, decreased lung compliance, or decreased renal perfusion. In a mixed population of critically ill patients, a multicenter prospective trial has demonstrated that the occurrence of IAH during the intensive care unit (ICU) stay was an independent outcome predictor.
Rhabdomyolysis
Rhabdomyolysis frequently presents within 24 hours of thermal injury and represents a well-documented risk for AKI and subsequent renal failure. Rhabdomyolysis can arise secondary to direct thermal damage or compartment syndrome and is commonly seen following a severe electrical injury. The release of myoglobin into the systemic circulation results in blockage of renal tubules, constriction of afferent arterioles, and the generation of oxygen free radicals. Myoglobinuria occurs when serum myoglobin exceeds 1500 to 3000 ng/mL. Myoglobinuria does not always result in renal injury, but certain risk factors have been identified. The risk of renal injury is directly related to the number of iron-containing molecules released, the state of hydration, and the degree of associated acidosis. Elevated creatinine at baseline and creatinine kinase levels greater than 5000 U/L have been associated with the development of AKI and the need for RRT, both in general trauma populations and in studies of burn patients. ,
Cardiac dysfunction
Patients suffering burns greater than 50% total body surface area (TBSA) are subject to decreased cardiac output, increased myocardial workload, and myocardial ischemia. Several authors have suggested theories to explain the decreased cardiac output associated with thermal injury: (1) increased sympathetic activity with impaired adrenal response, (2) hypovolemia resulting in myocardial ischemia, and (3) direct myocardial suppression.
Cardiac dysfunction results in reduced renal blood flow and hence contributes to AKI. Increased circulating catecholamines reduce blood flow to many organ systems, such as the kidney. In conjunction with this adrenergic response, hypovolemia ultimately decreases renal blood flow and thereby increases ischemia seen by the nephron and the heart. These are the more evident ways the renal-cardiovascular axis is affected by burn injury, but direct cardiac suppression also plays a role. Tumor necrosis factor α (TNF-α) is known to be released by myocytes stimulated by endotoxin or direct thermal injury. The effects of TNF-α on cardiac function include reversible biventricular dilatation, decreased ejection fraction, and decreased stimulation to catecholamines (see Fig. 25.2 ). , , This is typically a transient phenomenon, and, with adequate support, it usually resolves within 24 to 72 hours. Without appropriate support, frank heart failure can develop, bringing a myriad of complications with long-lasting or even permanent sequelae. Myocardial dysfunction after thermal injury is commonly overlooked by physicians due to the concentrated effort to correct the overwhelming state of hypovolemic shock and electrolyte abnormalities. In a patient presenting with burn shock (i.e., hypoperfusion) found to have a lower than expected cardiac response, serious consideration should be given to obtaining imaging further evidence of cardiac dysfunction. Transthoracic echocardiography, serology (troponins), and noninvasive measures of cardiac indices can be useful to this end and may help establish need for inotropic agents.
Absent of any clear finding of cardiac dysfunction, an effective burn surgeon must rapidly reestablish adequate renal blood flow by correcting the diminished preload state while keeping in mind the impact of burn injury on the entire cardiovascular system.
Late acute kidney injury
Despite successful resuscitative efforts, AKI can still develop, most commonly from sepsis. Because of the high risk for infection and the difficulty of diagnosing such infections in this patient population, underlying infection must be seriously considered in any patient found to have new or worsening renal failure more than 48 hours out from their initial injury.
Iatrogenic renal injury is also an important consideration in late burn-associated AKI, particularly given these patients’ frequent exposure to multiple antibiotics and diuretics.
Sepsis
Early aggressive resuscitation and excision have significantly influenced the course of ARF immediately associated with thermal injury. Acute renal dysfunction associated with the septic syndrome nonetheless continues to cause significant mortality. ,
Sepsis and septic shock are the most common causes of death in the ICU and are seen in up to 87% of cases of acute renal dysfunction in the burn ICU. , Several authors have found the degree of sepsis to be directly related to the incidence of acute renal dysfunction ( Table 25.2 ). , The pathophysiology of AKI associated with sepsis is multifactorial in nature but begins clinically with a generalized arterial vasodilatation secondary to a decreased systemic vascular resistance (see Fig. 25.2 ). Initially, bacteria or their products activate sepsis-associated cytokines locally at the site of direct invasion. The homeostatic balance between production and inactivation of these cytokine mediators is altered, allowing for systemic release, which causes direct damage to the endothelium, vasoparesis, and a procoagulant state. It has been theorized that acute renal insufficiency associated with sepsis is the result of each of these pathologic processes.
Table 25.2
Renal Failure Dysfunction and Sepsis
| Sepsis | Severe Sepsis | Septic Shock | |
|---|---|---|---|
| Acute renal dysfunction | 19% | 23% | 51% |
The vasoparesis seen in sepsis results in a profound state of hypotension and activates the neurohumoral axis. In an effort to maintain systemic arterial circulation, the sympathetic nervous system and the renin-angiotensin-aldosterone axis respond by increasing cardiac output and by direct renal arteriolar vasoconstriction. Furthermore, the systemic inflammatory response results in the release of additional vasoconstricting cytokines (i.e., TNF, endothelin) and locally secreted vasodilators (endothelial and inducible nitric oxide) to counterbalance these sepsis-associated vasoconstrictors. , Ultimately, this compensatory response comes at the cost of renal perfusion by further exaggerating the prerenal state.
Finally, as mentioned previously, sepsis induces a procoagulant state by affecting the expression of complement and the fibrinolytic cascade. This alteration in the homeostasis of coagulation may result in a state of disseminated intravascular coagulation with direct injury to the kidney by glomeruli microthrombi. The net result is a lack of perfusion to the kidneys during sepsis that will ultimately culminate in ischemic acute tubular necrosis ( Table 25.3 ).
Table 25.3
Comparison of Serum Creatinine Criteria in RIFLE, AKIN, and KDIGO Systems
From Khwaja A. KDIGO clinical practice guidelines for acute kidney injury. Nephron Clin Pract . 2012;120(4):c179-c184.
| KDIGO CRITERIA FOR RENAL INJURY | ||
| Stage | Serum Creatinine Criteria | UO Criteria |
| I |
|
<0.5 mL/kg/h for ≥6 h |
| II | Increase in serum creatinine to 2–2.9 times baseline | <0.5 mL/kg/h for >12 h |
| III |
|
<0.3 mL/kg/h ≥24 h or anuria ≥12 h |
UO, Urine output
Toxins
Antibiotics. Given the immunocompromised state associated with massive burn injuries, burn patients tend to accrue significant exposure to systemic antibiotics over the course of their care. Unfortunately, many of the systemic antimicrobial agents most commonly used in burn patients carry significant risk of nephrotoxicity.
Multidrug-resistant organisms have become more commonplace in hospitals worldwide. Among them, methicillin-resistant Staphylococcus aureus (MRSA), resistant Pseudomonas aeruginosa (PSA-R), and Stenotrophomonas spp. are particularly virulent organisms that are challenging to treat, and their medications can cause further renal damage. When utilizing agents such as vancomycin (MRSA), piperacillin/tazobactam (PSA-R), or trimethoprim/sulfamethoxazole ( Stenotrophomonas spp.), it is important to weigh the need of the medication against the renal deleterious effects. In addition, to prevent further resistance, antimicrobial stewardship is an important consideration.
In the case of vancomycin, there are measures one can take to minimize the risk of nephrotoxicity. Multiple studies have indicated that longer duration of therapy and higher serum concentration troughs are associated with increased risks of vancomycin-associated renal injury. , As concomitant aminoglycoside therapy has also been shown to significantly increase the chance of renal insult, these agents are best avoided when using vancomycin or any other nephrotoxic antibiotic as a component of combination antimicrobial therapy. Other antibiotics for resistant organisms do not have ways to monitor serum levels, so extra precaution should be taken when initiating these therapies. Antimicrobial therapy should be based on culture data, with the goal of deescalating therapy to the fewest necessary antimicrobials and safest complication profile (i.e., the least nephrotoxic).
Diagnosis
Using the consensus definitions discussed earlier, diagnosing AKI requires no more than measuring serum creatinine, estimated GFR, and/or urine output. It is also important to discern, if possible, the cause of the AKI as to prevent further injury and to allow for more informed treatment. Following are the common measures used to diagnose and monitor AKI in burn patients. In addition, there is ongoing effort to identify novel biomarkers, which might serve as a means to identify impending AKI earlier in the process.
Urine volume
Urine represents by far the simplest and most intuitive monitor of renal function. Urine volume is a specific but, unfortunately, not very sensitive test for renal failure. Most clinicians regard the presence of adequate urine output of little diagnostic value in the evaluation of renal dysfunction because severe renal injury may exist with any volume of urinary output. Urine output is not determined by the GFR alone but by the difference between GFR and tubular reabsorption. As such, AKI-associated tubular dysfunction can offset the decline in GFR, resulting in preserved urine output volume.
A urine output of less than 50 mL/day, anuria, or a complete cessation of GFR is a clinically significant finding. By far, the most common cause is a severe prerenal condition. Although it is true that other conditions (e.g., acute cortical necrosis, bilateral arterial occlusion, and rapidly progressive acute glomerulonephritis) may cause anuria, their incidence is exceedingly low in the acute burn care setting, and the diagnosis is usually readily apparent due to additional clinical signs. The Foley catheter should be checked if still correctly functioning when there is a marked decrease in urine output to ensure proper measurement of urine.
Although a return of urine output in the oliguric or anuric patient may offer encouragement, it does not necessarily indicate reversal of the inciting renal injury. Of particular concern, one must be careful to watch for a conversion of anuric or oliguric renal failure to polyuric renal failure. Failure to appreciate a polyuric renal failure and replace inappropriate fluid losses could result in a second prerenal insult, increasing the cumulative damage. Obtaining urine studies in cases of changes in urinary status can help avoid secondary renal insult.
Urinalysis
Creatinine clearance
Creatinine clearance is an inexpensive, consistent, time-tested technique for providing a rough estimate of GFR and renal function. Creatinine clearance measurement does involve the inconvenience of sustained urine collection, traditionally over a 24-hour period. However, this can be markedly simplified by foregoing the 24-hour convention for a more practical short-term (e.g., 6-hour or even 2-hour) collection, which has been shown to be just as accurate as the 24-hour assay and provides a more responsive measure of real-time function.
A significant disadvantage of creatinine clearance is that it becomes less accurate as GFR drops because renal tubules secrete a small amount of creatinine into the urine (in addition to that which is filtered). Normally, renal tubular secretion is so minor that it does not significantly impact the creatinine clearance calculations at normal GFRs, but it can create significant distortion as the real GFR drops. The impact of these variations in tubular creatinine secretion can be largely overcome by administering cimetidine, which inhibits tubular creatinine secretion, 1 hour before urine collection. ,
Fractional excretion of sodium
The primary goal of evaluating urinary electrolytes in a thermally injured individual is to differentiate between the prerenal and renal forms of AKI. It has been well established that a prerenal state in the presence of a functional nephron is associated with enhanced absorption of sodium or a low fractional excretion of sodium (FENa). The FENa is defined as:
with a value less than 1% associated with a prerenal condition and a value greater than 1% associated with organ dysfunction (i.e., “renal” renal failure). There are several conditions that affect renal absorption of sodium and thus have been shown to affect the calculated value ( Table 25.4 ).
Table 25.4
Factors That Affect Fractional Secretion of Sodium
| Condition | Effect on Fractional Sodium Excretion |
|---|---|
| Glycosuria | Increase |
| Diuretics | Increase |
| Mannitol | Increase |
| Dopamine | Increase |
| Myoglobinuria | Decrease |
| Radiocontrast media | Decrease |
Fractional excretion of urea (<0.35) has shown marginally improved sensitivity and specificity over sodium in distinguishing between prerenal and renal forms of ARF. Several additional indexes can be used to differentiate between the two forms of ARF ( Table 25.5 ).
Table 25.5
Differential Diagnosis of Acute Renal Failure
| Urinary Index | Prerenal | Renal |
|---|---|---|
| U osm (mOsmol/L) | >500 | <350 |
| U Na (mEq/L) | <20 | >40 |
| Specific gravity | 1.020 | 1.010 |
| U creat /P creat | >40 | <20 |
| Fractional excretion of sodium | <1 | >2 |
| Fractional excretion of urea | <35 | >50 |
Microscopy
Microscopic examination of urinary sediment is an easy and inexpensive initial evaluation of AKI that often lends insight into the underlying renal pathology. , The combination of normal urinary sediment, hyaline casts, and oliguric/anuric urinary output would suggest a prerenal condition. The presence of epithelial casts and abundant tubular epithelial cells is pathognomonic for acute tubular necrosis. Similarly, the identification of pigmented casts on microscopic evaluation signifies the diagnosis of myoglobinuria, likely secondary to rhabdomyolysis.
Serum biomarkers
Creatinine
For generations, creatinine has served as the most widely used marker of renal function. There is no question that creatinine levels correlate to renal function, and acute elevations of creatinine are clearly associated with an increased risk of renal failure and additional mortality. Indeed, serum creatinine levels (and changes therein) are central components to the three consensus AKI definition and staging systems proposed in the past 15 years.
Despite these advantages, serum creatinine levels cannot be counted on for accurate real-time assessment of renal function. Creatinine rises slowly in response to an acute drop in GFR, with a lag time of hours to days seen between the actual drop in GFR and the increase in serum creatinine levels. As serum creatinine levels reflect a balance between the rate of production and excretion of this endogenous protein, it takes time for serum creatinine levels to reach a new equilibrium when one side of this equation (excretion) changes ( Table 25.6 ). Therefore, even once the serum creatinine has begun to rise, it is typically hours to days before it reaches a new steady state. This makes it difficult to identify real-time changes in renal function and impossible to recognize the real-time stabilization or resolution of renal injuries.
Table 25.6
Factors Affecting Serum Creatinine
| Factors | Effect on Serum Creatinine |
|---|---|
| Liver insufficiency | Decreased production |
| Decreased muscle mass: | |
|
Decreased production |
|
Decreased production |
| Trauma | Increased production |
| Fever | Increased production |
| Immobilization | Increased production |
Neutrophil gelatinase-associated lipocalin
Neutrophil gelatinase-associated lipocalin (NGAL) is a polypeptide released by damaged nephron tubular cells in the setting of local inflammation. In multiple settings, NGAL has been shown to be identifiable in the serum and urine within 1 to 4 hours of ischemic renal insult and highly predictive of AKI. Multiple groups have found NGAL elevations earlier in a patient’s course to be predictive of subsequent AKI. Sen et al. and Jahajet al. demonstrated that elevations in whole-blood levels of NGAL occurred as early as 4 hours postburn . Furthermore, on multivariate analysis, NGAL levels identified a risk for subsequent AKI well before urine output rates or changes in serum creatinine; NGAL continues to show sensitivity as an early marker for AKI and may rival the usefulness of creatinine. ,
Others
Various investigators have identified additional novel early markers in burn patients. Serum uric acid levels, interleukin 18, and a novel protein (kidney injury molecule 1) have been found to predict AKI shortly after injury in isolated single-institution studies. ,
Treatment
The key to the treatment of AKI is prompt diagnosis coupled with a rapid reversal of the underlying pathophysiology while avoiding iatrogenic injury. Early in the course of acute burn care, the emphasis is on treating the underlying burn shock and minimizing the exposure to secondary injury from nephrotoxic injury products. Later, during acute care, the focus is on monitoring for the emergence of new signs of renal injury and eliminating or treating the underlying cause—typically infection or chemotherapeutic nephrotoxicity. In either context, the most effective approach is one that detects the presence (or imminence) of renal injury as early as possible, such that the underlying insult can be minimized or reversed as soon as possible.
Any injury that progresses to fulminant renal failure despite initial therapeutic maneuvers requires RRT. This section will address treatment and prevention of burn-associated renal injuries.
Renal protection in the early phase of acute burn care
Resuscitation
As stated previously, the vast majority of cases of AKI presenting within 24 hours of injury results from inadequate renal perfusion. , Several authors have demonstrated that the timing of initiation of resuscitative fluids is directly related to the incidence of renal dysfunction. Resuscitative efforts should therefore begin immediately to reestablish effective renal perfusion. Several resuscitative formulas have been established based on multivariate logistic regression analysis ( Table 25.7 ). Which formula to use is far less important than the flexibility and care with which they are applied. The clinician must recognize that these formulas are estimates to be used as starting points. The true amount is directly dependent on the patient’s own physiologic status and degree of injury, neither of which can be fully captured by a single formula.
Table 25.7
Burn Formulas for Estimating Initial Resuscitation
| Crystalloid | Colloid | |
|---|---|---|
| Colloid: | ||
|
NS 1 mL/kg/%burn | 1 mL/kg/%burn |
| Crystalloid: | ||
|
4 mL/kg/%burn | |
|
2 mL/kg/%burn | |
| Pediatric formulas: | ||
|
4 mL/kg/%burn + 1500 mL/m
2
|
|
|
||
|
TBSA | |
|
5000 mL/m
2
BSA + 2000 mL/m
2
|
|
|
||
|
TBSA | |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree