Summary
The effects of thermal injury on osseous metabolism are often clinically underrecognized in the greater care of the burned patient. After burn, several interconnected regulatory systems for mineral metabolism become disordered with pathologic changes to osseous homeostasis. This can result in highly variable and severe bone loss that must be addressed and managed to mitigate the potential for long-term morbidity. Pathologic formation of extracellular bone—a process called heterotopic ossification (HO)—can also occur and causes significant and intractable morbidity when localized to critical anatomic structures. These changes to bony metabolism represent the final outcome of a spectrum of interrelated traumatic and inflammatory insults resulting in aberrant healing and pathologic turnover of the native machinery for bone homeostasis. Severe burns, often concomitant with orthopedic and neurologic polytrauma, prime the patient for a series of clinical events progressing from local inflammation, swelling, and pain to the progressive development of cartilage and bone. Although many of these lesions may remain clinically irrelevant, more extensive HO lesions may be disfiguring, painful, and cause loss of function and ankylosis of affected joints. Mature, ossified HO is only treatable by surgical extirpation, and risk of recurrence is high. Proper prediction of those at risk, identification of early signs and symptoms, and prompt prophylactic management are critical in the prevention of HO morbidity after thermal injury. In this chapter we will discuss the clinical history, biology, and epidemiology of the mineral and osseous metabolic derangements in bone as they relate to the identification, management, and treatment of both osteopenia of native skeleton and the formation of extra skeletal bone and will explore current and proposed therapeutic options to assist in the management of HO-related morbidity.
Global and osseous metabolic changes
The effect of burn injury on bone
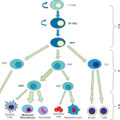
The effect of burn on bone is systemic and results in disorder to native mineralization and calcium homeostasis ( Fig. 20.1 ). Although it is possible that a burn may be deep enough to affect bone locally, the entire skeleton is affected by systemic factors resulting from burn: (1) the inflammatory response, (2) the stress response, and (3) immobilization, whether absolute or relative. The cumulative effect of these forces is to increase bone resorption and to decrease bone formation . This results in a net loss of bone. Using measurements of density in children, lumbar spine bone mineral content, composed of trabecular bone, decreases by 7% over the first 6 to 8 weeks postburn, whereas total body bone mineral content, composed of 80% cortical bone, decreases by about 3% over the first 6 months postburn.
Vitamin D and calcium metabolism. PTH, Parathyroid hormone.
There is a window in which active bone resorption and reduced formation take place together, beginning at day 1 postburn and ending at approximately day 21, after which the production of endogenous glucocorticoids by the stress response results in apoptosis of osteoblasts, osteoclasts, and osteocytes ( Fig. 20.2 ). , The resulting adynamic bone is a state that persists through most, if not all, of the first year after a severe burn ( Figs. 20.3 and 20.4 ). This window of opportunity to prevent bone loss, as well as its surprising effect on muscle mass, will be discussed later.
Mechanisms of bone loss after severe burn. IL, Interleukin; PTH, parathyroid hormone.
Goldner trichrome stain of an iliac crest bone biopsy of a healthy person. The blue-green area represents mineralized bone. The red area represents unmineralized osteoid. Spindle-shaped cells from the osteoid surface are osteoblasts.
Goldner trichrome stain of an iliac crest bone biopsy of a burned patient. The blue-green area represents mineralized bone. Compared with Fig. 20.3 , note that osteoblasts are absent from the osteoid surface.
Because of the apoptosis of bone cells at approximately 3 weeks post-burn and the persistence of that state throughout the first postburn year, the skeleton does not have the opportunity to recover lost bone till well after the first year postburn. It has been shown that cortical bone recovers first, usually by 24 months after the injury, whereas it is uncertain that trabecular bone, as measured by lumbar spine bone mineral density, recovers fully, even after 5 years postburn ( Fig. 20.5 ). The consequence of this delay in bone recovery is an annual extrapolated postburn fracture incidence in males of twice age-matched normal and in females of 50% more than in age-matched unburned normal. A study of children at Shriners Hospital in Cincinnati showed a 1-year postburn fracture rate of 15%.
Distribution of lumbar spine bone mineral density Z-scores of severely burned children compared with a standard distribution curve. Note that the distribution after burn is shifted to the negative side.
Accompanying loss of bone is the loss of skeletal muscle. Not as much work has been done on the loss of muscle, but what is currently known is that burn injury sets up a generalized catabolic response, and the known mechanism will be considered in more detail in that discussion. However, as we will soon see, the muscle response to burns cannot be completely detached from the skeletal response.
The prevention and treatment of bone loss: Growth hormone and oxandrolone
Studies with recombinant human growth hormone (rhGH) daily injections in children of 0.05 or 0.1 mg/kg/d for the first year postburn resulted in improvement in muscle strength by approximately 9 months postburn and in bone mass by approximately 12 months postburn. However, both the discomfort of daily injections and the expense of the treatment led to a search for a less painful and less expensive alternative. In addition, rhGH was not as effective in adults as it was in children, and a small study of rhGH among critically ill adults in an intensive care unit was reported to raise mortality.
The current standard of treatment is the nonaromatizable anabolic steroid oxandrolone, which, when given as an oral dose of 0.1 mg/kg/d in adults and 0.1 mg/kg twice daily in children for 12 months, has effects similar to rhGH and over a similar time scale. , As an oral dose, it avoids painful injections and is much less expensive for the patient. The mechanism presumed to be active at the time was a primary increase in muscle mass and strength that then increased skeletal loading, resulting in increased stimulation for formation of new bone as the bone marrow recovered and endogenous glucocorticoid production waned.
New horizons
In 1998, a new study began at Shriners’ Hospital in Galveston. Because of the early onset of bone resorption documented in a sheep model of burn injury, a trial of the bisphosphonate pamidronate, an antiresorptive agent usually used for the treatment of osteoporosis in adults but also used in children with osteogenesis imperfecta, was initiated in pediatric burn patients. , , This trial was a placebo-controlled, randomized, double-blind study in children with at least 40% total body surface area burns. The study was unblinded at the 6-month mark and patients were followed for another 18 months. The dose given was 1.5 mg/kg with a maximum dose of 90 mg. The intent was to give two doses, the first within the first 10 days of the burn and the second a week later. However, many of the patients received only the first dose.
The results of this study at 6 months were unequivocal. Patients who received even one dose of pamidronate continued to accrue bone normally, whereas those who received placebo lost 7% of lumbar spine (trabecular) bone mass at 6 weeks, remaining stable up to 6 months, and 3% of total body bone mass (80% cortical) at 6 months postburn. When these patients were followed up to 24 months postburn, the placebo-treated group still lagged significantly behind the pamidronate group at the end of the study, as was reflected in the differences between their age-adjusted lumbar spine bone density Z-scores. Unfortunately, fracture-incidence data was unable to be obtained at the 2-year follow-up, so it is unknown if this therapy has antifracture efficacy. , However, we could conclude that trabecular bone, the more metabolically active constituent of bone, is more adversely affected than cortical bone, and that bisphosphonates appear to be more active in protecting trabecular bone from all-cause resorption. This was not the end of the story, however.
What about skeletal muscle?
Because antiresorptive treatment was not known to confer protection from postburn fracture, and because its benefits over oxandrolone therapy in restoration of musculoskeletal mass and strength were unknown, the therapeutic use of bisphosphonates was neither recommended nor employed.
However, in 2013, a database of muscle protein kinetics using stable isotopes became available for pediatric burn patients at Shriners Children’s Texas in Galveston. Upon examining the database, we came across 17 of the 62 patients (27.4%) enrolled in the randomized clinical trial of pamidronate. We found that for patients who received pamidronate, the rate of muscle protein breakdown was half that of those who received the placebo, and the net protein balance in the pamidronate group was surprisingly positive, compared with the negative net protein balance seen in the placebo group. Moreover, at 9 months postburn, at the beginning of a resistance exercise-training period, baseline lower limb muscle strength, as measured by peak torque, was no different between pamidronate-treated patients and normal unburned, physically fit, age-matched children, whereas the trend of lower limb strength in placebo-treated patients was lower, almost to the point of significance ( P =.052). Thus as little as a single dose of pamidronate administered within the first 10 days of burn injury resulted in a prevention of muscle wasting.
To understand how this happened, Pin et al. used an in vitro study of murine C2C12 myoblasts incubated with serum from burn patients who received pamidronate or placebo or serum from normal unburned children. They found that cultures of myoblasts with serum from placebo-treated patients had reduced diameter of developing myotubes, suppressed anabolic pathway phosphorylation (activation), and upregulated catabolic pathway signaling. In cultures containing serum from patients treated with pamidronate, myotube diameter was partially rescued, the anabolic pathway showed increased phosphorylation (activation), and the catabolic pathway was suppressed. Furthermore, when the culture experiment was repeated with the addition of an antibody to transforming growth factor (TGF)-β1, myotube size in the cultures with serum from placebo-treated patients was rescued to the same magnitude diameter as in the cultures with serum from pamidronate-treated patients. In contrast, cultures with serum from pamidronate-treated patients did not significantly increase myotube diameter when TGF-β antibody was added. These experiments provided evidence that bone resorption after burns released TGF-β that had paracrine catabolic effects on muscle in burn-injured patients and that early administration of an antiresorptive agent, such as a bisphosphonate, could lead to sparing of skeletal muscle and trabecular bone after burn injury.
These findings should justify a large-scale randomized controlled study of the effects of antiresorptive agents on skeletal muscle sparing and on bone mass after severe burn injury, with the potential effect of shortening rehabilitation time and the period of reintegration of burn patients into their communities. Also of significance is that there were no demonstrable adverse effects, most notably hypocalcemia, attributable to the use of bisphosphonates in pediatric burn patients. Thus the safety of administration and the efficacy of preventing catabolic bone and muscle loss should provide an additional tool for the management of acute severe burn injury.
Calcium
Related to the effects of burn injury on bone and muscle is the effect of burns on calcium metabolism. At the outset, it is important to point out that calcium is affected differently by a burn injury depending on whether the patient is a child or an adult.
Children with severe burn injury are hypocalcemic, hypoparathyroid, and hypercalciuric, whereas adults are normocalcemic or mildly hypercalcemic and euparathyroid or mildly hyperparathyroid.
To understand this difference, it is necessary to understand the working of the parathyroid calcium-sensing receptor (CaSR). The parathyroid CaSR is a transmembrane G-protein–coupled receptor residing on the membrane of the parathyroid chief cells. It is one of the many CaSRs in the body and its behavior is one of the best understood. From the work of Nielsen et al. and others, the parathyroid CaSR, whose function it is to “sense” extracellular calcium and magnesium concentrations, among others, can provide feedback to the chief cell nucleus when it is upregulated. In this case, the CaSR will signal the nucleus to reduce secretion of parathyroid hormone (PTH). This signaling lowers the amount of circulating calcium necessary to suppress PTH secretion and creates a condition of hypocalcemic hypoparathyroidism with urinary calcium wasting. This is precisely what we see in burned children. However, as mentioned earlier, this is not found in adults. The pediatric condition is also what we found when studying a sheep model of burn injury.
Note that analyzing total serum calcium acutely is not accurate in determining true calcium status of a patient. This is because acutely, with the extrusion of plasma binding proteins from the circulation, the calcium-binding protein albumin is lost from the circulation, giving a reading of circulating calcium that is low and potentially misleading. It is much more reliable to assess blood ionized calcium concentration if such technology is available.
It is also important to know that when bone is resorbed due to proinflammatory cytokines, the calcium released from the bone enters the circulation, where it has proinflammatory effects. These include stimulating the release of chemokines from peripheral blood mononuclear cells and activating the NLRP3 inflammasome of the innate immune system, stimulating monocytes and macrophages to produce interleukin (IL)-1. , These effects can potentially intensify or prolong an inflammatory response. Thus pediatric patients can upregulate the CaSR in response to proinflammatory cytokines and excrete excess amounts of calcium in the urine, whereas adult burn patients cannot. The difference in calcium handling may partly explain why adult burn patients suffer greater morbidity and mortality than pediatric burn patients. Table 20.1 indicates suggested treatment for hypocalcemia and hypophosphatemia after a burn injury.
Table 20.1
Treatment of Calcium and Phosphate Imbalance
| Disturbance | Decision Point | Recommended Treatment |
|---|---|---|
| Hypocalcemia | Symptomatic |
|
| Asymptomatic | Oral calcium carbonate or intravenous calcium gluconate | |
| Hypophosphatemia | Symptomatic | Infants or children: 5–10 mg/kg infused over 6 hours followed by 15–45 mg/kg given by infusion over 24 hours |
| Asymptomatic | Oral administration of 20–25 mg/kg of elemental phosphorus in four divided doses each day |
Vitamin D
There have been multiple reports in the literature over the past decade describing acute vitamin D deficiency after burn injury. These reports are flawed because acutely plasma constitutive binding proteins leak out of the vasculature causing binding protein deficiencies. The most well described is albumin loss, as discussed earlier. However, that also applies to vitamin D binding protein as reported by our group in 1993. The low vitamin D binding protein levels make it impossible to determine the significance of serum 25-hydroxyvitamin D measurements inasmuch as those performed by currently available assays for total 25-hydroxyvitamin D. The only way to determine acute vitamin D deficiency after a burn injury would be to measure free 25-hydroxyvitamin D. This assay is mostly used for research purposes and is both labor-intensive and expensive. Therefore, for practical purposes, acute vitamin D status is unclear. To complicate matters, the period to return to normal levels of serum vitamin D binding protein concentration has not been determined. The earliest observed return of serum albumin concentration to normal levels is 6 months after a burn. That does not imply that 6 months postburn is the time that vitamin D binding protein returns to normal. However, it is highly unlikely that the serum concentration of vitamin D binding protein returns to normal before a key protein such as albumin.
Serum concentration of 25-hydroxyvitamin D has been reported to be low for long periods of time, up to 7 years postburn. At first, the mechanism for this was unclear. However, the initial review of the manuscript first reporting chronically low serum concentration of 25-hydroxyvitamin D raised the issue of how we controlled for sun exposure, and we had not done so. Therefore our group assumed that the group of patients we reported had been exposed to ultraviolet B (UV-B) rays from the sun, and if that were the case, the skin of burn victims must be unable to process UV-B light to convert the 7-dehydrocholesterol precursor to vitamin D 3 . We tested this hypothesis by irradiating skin biopsies from burn scar, normal-appearing skin adjacent to burn scar, and normal unburned skin and found that both burn scar and normal-appearing adjacent skin converted UV-B light to vitamin D 3 at about 25% of the normal quantity. This finding indicates that normal-appearing skin adjacent to a burn scar is also biochemically damaged. Moreover, the quantity of the 7-dehydrocholesterol precursor in both burn scar and adjacent normal-appearing skin is deficient, indicating that the normal-appearing skin adjacent to a burn scar lacks vitamin D 3 precursor and possibly has damage to the cell membranes as a resulting from precursor deficiency.
These findings explain the mechanism of chronic vitamin D deficiency after burn injury but raise several important questions, all of which have been unaddressed.
-
1.
When is the earliest time that serum 25-hydroxyvitamin D levels can be accurately determined?
-
2.
How can the adequacy of vitamin D maintenance be evaluated without normal serum concentration of vitamin D binding protein? The answers to both questions depend on finding out when serum concentration of vitamin D binding protein returns to normal.
-
3.
What is an appropriate maintenance dose of vitamin D? Are vitamin D 2 (ergocalciferol, a plant sterol) and vitamin D 3 (cholecalciferol, the biologic form of vitamin D 3 synthesized in our skin) equally effective in maintaining normal levels of serum 25-hydroxyvitamin D in patients postburn?
-
4.
Pursuant to the answers to questions 1 and 2, when should this maintenance dose of vitamin D be started?
-
5.
Is vitamin D from food sources equally effective in maintaining normal levels of serum 25-hydroxyvitamin D as oral vitamin D supplements?
-
6.
What is the effect of chronic vitamin D deficiency on bone density, muscle function, and immunity?
Summary
Burn injury causes inflammatory bone resorption, as well as bone resorption secondary to immobilization or insufficient mobilization. At present it is not possible to sort out the separate effects of inflammation and immobilization on bone resorption. We know that the bone resorption releases TGF-β1 from the bone matrix. TGF-β1 from the bone has paracrine catabolic effects on muscle protein breakdown while suppressing muscle protein synthesis contributing to the catabolic muscle protein wasting. Experimental evidence and evidence from a small clinical trial show that the use of antiresorptive agents acutely after burn may prevent some bone resorption and preserve both bone and muscle mass.
We have also shown that inflammatory cytokines postburn can stimulate bone resorption and upregulate the parathyroid CaSR in a sheep model of burns and in pediatric burn patients. This upregulation prevents the excess calcium appearing in the circulation after bone resorption from remaining in the circulation, causing hypercalciuria and a resulting low circulating level of blood ionized calcium. Calcium has been shown to stimulate the inflammatory response by stimulating peripheral blood mononuclear cells to produce chemokines and by stimulating the NLRP3 inflammasome to stimulate monocytes and macrophages of the innate immune system to produce more IL-1. Thus the dumping of excess calcium in the urine via the upregulation of the parathyroid CaSR may serve to reduce the systemic inflammatory response in children. This responsiveness to proinflammatory cytokines disappears in adults, so the upregulation of the CaSR in children may at least partly explain the decrease in postburn morbidity and mortality in children compared with adults.
Finally, we cannot currently evaluate the acute status of vitamin D in burn patients because the currently used assay is based on measurement of total 25-hydroxyvitamin D, including that part bound to vitamin D binding protein. Vitamin D binding protein is acutely low after burn injury, and the time it takes to return to normal levels is unknown at present. We do know that chronically burned skin and adjacent normal-appearing skin is unable to synthesize vitamin D 3 from UV-B sunlight exposure and that this mechanism likely contributes to chronic vitamin D deficiency after a burn. Therefore we need studies to determine when vitamin D binding protein levels return to normal in serum, the proper form and dose of vitamin D supplementation, when this supplementation should be initiated, and the effects of chronic vitamin D insufficiency/deficiency on bone, muscle, and immune function of postburn patients.
Osseous pathology after burn
Introduction
HO is most simply described as a pathologic form of tissue healing. Injury invites inflammation, and the consequences of this cascade stimulates a range of tissues, most predominantly those of mesenchymal origin resulting in a series of events characterized by mesenchymal proliferation, and the pathologic redemonstration of developmental processes including endochondral and intramembranous ossification. Propagation of HO after burns requires several critical elements: (1) thermal injury; (2) inflammation or related systemic stress response; (3) a population of mesenchymal cells available to react to this signal; and (4) a systemic environment supportive of osseous differentiation and proliferation. , As described earlier, after burn, the necessary injury and environment are abundant. Mobilization of bone stores of calcium increases the available circulating levels to promote the pro-osseous environment required. Further, given the ubiquity of the mesenchymal lineage in connective tissues, this can occur in essentially any anatomic site with an equivalently diverse range of presentations. In thermal injuries alone, HO has been described in sites as variable as the hand, forearm, elbow, shoulders, knees, hips, and temporomandibular joints. Given this variability, it is paramount that the provider be vigilant, particularly after high-risk injuries, for those common signs and symptoms indicative of early HO.
History
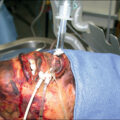
Ectopic or heterotopic bone formation is common to a range of pathologic conditions variably named and described by cause and anatomic location. Whereas heritable conditions of ectopic bone formation such as myositis ossificans progressive were described as early as 1692 by Dr. Patin in pediatric patients, recognition of HO forming after trauma is a relatively recent phenomenon. , One of the earliest descriptions of posttraumatic HO can be found in the work of Drs. DéJerine and Ceillier in 1918 under the name paraosteoarthropathy . At the time it was described as a consequence of neurologic injury, specifically of traumatic paraplegia after spinal cord injury (SCI), and was primarily presented as a condition of the hip and lower extremities. In the ensuing decades, awareness of the disease grew slowly; scattered case reports of periarticular and intramuscular sites after thermal and musculoskeletal injuries were published. In this period, HO of the elbow was first recognized as a consequence of severe burns ( Fig. 20.6 ). In the intervening years as the number of cases has grown, the relationship between orthopedic and neurologic injury and surgery have expanded and the modern paradigm of an inflammation-driven pathologic condition affecting any of the myriad connective tissues investing every anatomic structure in the human body has gained greater support.
Radiograph demonstrating ectopic bone formation around the elbow after thermal injury.
Incidence and epidemiology
Across the various etiologies of HO, male gender and younger age are consistent risk factors. Although not specifically a “genetic cause” of HO, certain osteogenic and inflammatory conditions including Paget disease, ankylosing spondylitis, and hypertrophic osteoarthritis have been associated with HO. As alluded to earlier in this chapter, both genetic and nongenetic HO are often triggered by an inciting injury. Whereas even relatively minor trauma has the potential to progress to ectopic bone formation, there are several well-described “high-risk” insults that more frequently initiate HO formation.
Burns and trauma
Although HO may form after chemical or electrical burns, in this section we will focus primarily on thermal injury as an inciting event. , In thermal burns, the extent, magnitude, and site of injury are key to the risk of HO. Whereas retrospective numbers are significantly lower, prospective analyses have identified up to 22% to 23% of patients with third-degree injuries and 2.4% of patients with second-degree injuries progressing to radiographic evidence of ectopic bone. , Burn injuries affecting greater than 20% of the body and those resulting in full-thickness injury near a joint confer additional risk. When accounting for the severely burned patient or in complex burn polytrauma, rates may rise to 60%. , Key risk factors for burn-associated HO are orthopedic and major trauma—particularly blast, polytrauma, and amputation, as well as major orthopedic surgeries particularly in the area of large-joint arthroplasties. Blast and amputation injuries, seen most commonly in military populations, reach prevalence of up to 65% when accounting for all severities of ossification.
Orthopedic surgery
Rates of HO formation after orthopedic injuries are highly variable in the literature and generally higher for cases of polytrauma versus single-bone fractures, however, in prospective analyses of orthopedic monotraumatic injuries, femoral fractures (52%), acetabular fractures (40%), and forearm fractures (20%) present with the highest rates of ectopic bone. Surgical delay, use of bone grafts, bone substitutes, and/or cements appear to confer additional risk in the repair of orthopedic injury. , Postarthroplasty HO varies both in extent and severity by location. Outside of trauma, approximately 40% of patients after total hip arthroplasty will develop some degree of ossification, although severe periarticular HO is less frequent, between 2% and 7%. In general, the extent of the surgery matches the risk of HO, with minimally invasive approaches carrying a lower risk and revisional procedures or those with longer ischemia time being greater risk factors.
Neurogenic injury
Neurogenic injuries, particularly those affecting the central nervous system, such as traumatic brain injuries (TBIs) and SCIs, particularly those resulting in paraplegia and quadraplegia with resultant immobility, carry additional severe risk. , , Up to 10% to 53% of patients presenting with TBI or SCI progress to develop HO. Risk factors in this population include high thoracic spinal injuries and injuries with more severe comorbid presentations including spasticity, need for tracheostomy, prolonged ventilator requirement, decubitus ulcers, or concurrent infection (e.g., pneumonia, urinary tract infection).
Nontraumatic causes
Other common, albeit less strongly associated, risk factors include chronic, inflammatory, and autoimmune conditions such as chronic pressure ulcers, abdominal and/or systemic sepsis, dermatomyositis, or systemic sclerosis.
Clinical presentation/natural history
At earliest preosseous presentation, HO is characterized by localized edema, effusion, warmth, and pain often occurring in the first 3 to 12 weeks and as late as 3 to 6 months after injury. Diagnosis at this point may be challenging and overlap with other posttraumatic causes including infection, hematoma, and/or vascular conditions. In many cases, this may be followed by a rapid increase in size of the affected area concerning for oncologic etiology, which may require further consideration. As HO begins to process from its inflammatory/proliferative phases toward osteochondral maturation, the lesion may begin to localize and take on osseous characteristics. Typically, HO differs from reactive periosteal lesions in that it starts within the soft tissue proper, however this can be challenging to identify clinically. As the lesion continues to grow and mature ulceration, symptoms of ankylosis such as lost or restricted range of motion, nerve compression, and entrapment of surrounding structures may occur. Anatomic site and comorbidities vary with cause. Juxtaarticular regions are at high risk for restricted range of motion. Given the predilection for postburn HO to present at the elbow ulnar nerve compression is a well-described risk of HO in the burned patient.
Imaging findings
Given the nonspecific findings described earlier, radiography and advanced imaging modalities are critical to the timely and accurate diagnosis of HO ( Fig. 20.7 ). This is of particular importance in the burned patient, where contracture and adhesion, lost range of motion, chronic pain, swelling, and tissue friability/ulceration can overlap with postburn scarring and soft tissue loss. As extirpation remains the only effective treatment option once HO matures, management is focused on prevention and prophylaxis. Therefore diagnostic strategies focus a multimodal strategy targeted to anatomic site, inciting event, and presumed disease stage/extent.
Diagnostic modalities for heterotopic ossification.
Conventional radiography
In most cases the initial imaging modality pursued is XR. Although effective in identification of early-ossifying or mature HO, radiographs are highly dependent on disease progression. Thus during early/inflammatory, mesenchymal, or cartilaginous phases, radiographs will not detect evidence of ossification. Early ossifying lesions may demonstrate an irregular area of radiopacity, however, as the anlagen matures it commonly takes on an ordered, “zonal” pattern of peripheral ossification before ossifying fully in its later stages. The general shape of the lesion is highly dependent on the anatomy in which it is found. As mentioned previously, HO classically initiates within soft tissue without immediate physical connection to underlying bone or periosteum. As HO grows and matures, however, this distinction may be lost or blurred. Within the soft tissue proper HO may track along anatomic structures—ligaments, tendons, muscles, and so on—however, care should be given to the presence of indistinct calcifications or irregularly, poorly demarcated ossific lesions as XR is not sufficiently specific to differentiate irregular opacities of HO from oncologic or dystrophic causes of calcification. As a general rule abnormal features on XR require more sensitive imaging modalities as follow-up.
Bone scan
Nuclear bone scans are sensitive versus XR for early developing HO and are a common second modality. A triple phase bone scan with technetium-99m–methylene diphosphonate (MDP-99mTC) can demonstrate increased uptake in areas of soft tissue swelling 1 to 2 weeks before radiographic evidence of calcification/ossification. Care should be taken in the burned patient or in areas of traumatized soft tissue, as extensive or persistent inflammation can result in increased uptake leading to false positives.
Computed tomography
Whereas conventional computed tomography (CT) may provide an additional level of sensitivity and specificity over XR, a noncontrasted CT image shares many of the limitations with CR. As with XR, HO stage determines the expected findings, and early in disease progression the inflamed site may present itself only as a low-density mass. Serial imaging may provide earlier identification of zonal maturation versus XR. Major benefits of CT imaging include visualization of those anatomic structures incorporated by and adjacent to the HO anlagen. This can be used to enhance preoperative planning. Enhanced CT imaging (micro- and/or nano-CT) are higher-resolution techniques that may drastically improve sensitivity; the availability of these techniques in the clinical setting remains limited.
Positron emission tomography and single-photon emission CT
Similar to the nuclear medicine bone scan, advanced CT imaging using radiolabeled uptake markers may help differentiate between early HO and other lesions. During bone growth and turnover, radiolabeled fluoride-F18 is taken up and bound to hydroxyapatite amplifying the signal and allowing for earlier detection of ossification. Alternatively, radiolabeled glucose (FDG) may be used to highlight areas of increased metabolic demand, such as inflamed and/or rapidly proliferating sites that may correspond to early HO. , Single-photon emission CT imaging augmented with MDP-99mTC may be further used to localize areas of osteoblastic activity enhancing the sensitivity toward both HO formation and recurrence in previously resected lesions. ,
Magnetic resonance imaging
As with each of the listed techniques, magnetic resonance imaging (MRI) is most sensitive to the identification of mature HO and is limited by the heterogenous composition of the early preosseous anlagen. Ectopic bone under MRI is typically well circumscribed. Under contrast, the lesion is typically highly vascular with circumferential edema of surrounding tissues. , , As above, these imaging characteristics may overlap with oncologic lesions, and diagnosis may benefit from a multimodal approach to imaging. In mature HO, the characteristics of zonal ossification and rim enhancement in a contrasted MRI help to differentiate from sarcoma or similar oncologic pretender. The combination of MRI and CT imaging may further enhance both sensitivity and specificity of diagnosis, particularly in the early, heterogenous stages of HO development.
Ultrasound
Although it is not currently widely used in the diagnosis of HO, ultrasound (US) is well suited to the early detection of soft tissue abnormalities before obtaining radiographic evidence of ossification. , Because of the operator dependency of ultrasonography and challenges differentiating between the later stages of ossification, US is most commonly used in high-risk settings such as post-SCI or after hip arthroplasty where pretest suspicion is high. ,
Spectroscopy
Similar to US, transcutaneous spectroscopic techniques (Raman spectroscopy, near-infrared [NIR] imaging, reflectance) are noninvasive means to detect early preosseous changes in tissue. Spectroscopic techniques detect highly subtle changes in collagen mineralization (Raman), vascularity/inflammation (Reflectance), or water content (NIR) to mark which tissues are at risk of later ossification.
Pathologic findings
Immediately after trauma, HO is histologically indistinct from its tissue of origin. As the early lesion develops, the site becomes progressively hypercellular with the presence of spindle cells, inflammatory and multinucleated giant cells, and extravasated erythrocytes. At this time there is typically no evidence of osseous matrix. HO lesions that occur through endochondral ossification at this point may begin to demonstrate evidence of cartilaginous lesions progressing from immature to hypertrophic cartilage. After this progression, ossification may progress in zonal fashion as ossification centers begin to form within or around areas of hypertrophic cartilage. As ossification continues, immature woven bone will mature to develop into well-circumscribed lamellar structures. During intramembranous formation of HO, woven bone may arise immediately after the early inflammatory and proliferative stages without evidence of intervening cartilaginous tissue. In all cases, as HO lesions fully mature they take on the appearance of native bone with a central marrow cavity, sinusoids, and a progressive lamellar and compact/cortical bone tissue.
Care must be taken in the diagnosis of HO after trauma, however, given the overlapping similarities between soft tissue ossification and osteosarcoma. The hypercellular early inflammatory/proliferative stage of HO overlaps with presentations of “nodular fasciitis” and should be characterized by normal mitotic figures often with a progressively well-circumscribed lesion. In more developed lesions, HO may be differentiated from osteosarcoma by the progressive maturation of peripherally mature bone with internal immature osseous trabeculae and osteoblastic rimming. Key to differentiation is that HO should be absent of typical mitochondria or nuclear figures that would be more consistent with the presentation of sarcoma.
Biomarkers and lab studies
Currently there are no diagnostic biomarkers in blood/serum, saliva, or urine that are clinically used to detect HO after thermal injury; however, several promising small molecules and proteins have been identified in both clinical and preclinical models. Nonspecific markers of skeletal trauma, such as alkaline phosphatase, may remain elevated throughout the development of HO and persistent elevation after high-risk injury should raise suspicion for possible ossification. Inflammatory markers including C-reactive protein and erythrocyte sedimentation rate may also remain elevated during the early development of HO; however, they may normalize as bone matures. In the case of skeletal muscle involvement, creatine kinase elevations have been described as correlating to extent of muscular injury. Less commonly, elevated IL-3 and matrix metalloproteinase 9 have been described; however, both are commonly elevated in major trauma and complex burns, and consequently HO-specific elevations are challenging to identify. ,
Classification systems
Classification and grading of HO is a mix of clinical, radiographic, and histopathologic findings with various systems used at different sites. Given the prevalence of HO after total hip arthroplasty, several grading systems have been developed to classify HO based on radiographic findings ( Table 20.2 ). The most common of these are the Brooker and Modified Brooker Scales. The original Brooker scale used a system of 4 classes of ascending severity based on the HO distance from and/or involvement/ankylosis of the hip joint. A simplified classification, the Della Valle classification, breaks this down A common modification is the inclusion of class 0 or absence of HO. In the elbow, the Hastings and Graham classification assesses both radiographic and clinical findings on an ascending scale from 1 to 3. Histopathologic scales have been similarly described that classify HO on the bases of ossification grade and presence of pathologic comorbidities such as necrosis and/or osteomyelitis.
Table 20.2
Clinical and Radiographic Classification of Heterotopic Ossification
|
CLINICAL/RADIOGRAPHIC SCALES
|
PATHOLOGIC SCALES
|
||
| Brooker Classification (Hip) | Ohlmeler Classification (Histopathologic) | ||
| Class 1: | Non-contiguous islands of bone within the soft tissues | ||
| Class 2: | Bone spurs from the pelvis or proximal femur; space between opposing bones is ≥1 cm | Ossification Score: | |
| Class 3: | Bone spurs from the pelvis or proximal femur; space between opposing bone is <1 cm | Grade 1: | Low formation, low destruction, low infiltration |
| Class 4: | Ankylosis of the hip | Grade 2: | Moderate formation, moderate destruction, moderate infiltration |
| Grade 3: | High formation, high destruction, high infiltration | ||
| Modified Brooker Classification (Della Valle) | |||
| Grade A: | HO is either absent or present as soft-tissue island <1 cm in length | Bone Formation: | |
| Grade B: | Greater than or equal to 1 island of bone | Low: | Bone formation <1/3 of evaluated area |
| >1 cm in length | Moderate: | Bone formation 1/3–2/3 of evaluated area | |
| >1 cm of distance between opposing bones | High: | Bone formation >2/3 of evaluated area | |
| Grade C: | Bone spurs with <1 cm between opposing bones or ankylosis | ||
| Bone Destruction: | |||
| Hastings and Graham Classification (Elbow) | Low: | <5 osteoclasts and osteoblasts per HPF | |
| Class I: | Radiographic evidence of HO without ROM limitations | Moderate: | 5–10 osteoclasts and osteoblasts per HPF |
| Class II: | Radiographic evidence of HO with partial ROM limitation | High: | >10 osteoclasts and osteoblasts per HPF |
| IIA: Limited flexion/extension | |||
| IIB: Limited pronation/supination | Inflammatory Infiltration: | ||
| IIC: Both Class IIA and IIB limitations | Low: | <5 leukocytes per HPF | |
| Class III: | Radiographic evidence of HO with ankylosis | Moderate: | 5–10 leukocytes per HPF |
| IIIA: Ankylosis in flexion/extension | High: | >10 leukocytes per HPF | |
| IIIB: Ankylosis pronation/supination | |||
| IIIC: Both class IIIA and IIIB limitations | |||
| Mavrogenis Classification (Neurogenic) | |||
| Type 1: | HO at anterior hip or proximal femur | ||
| Type 2: | HO at posterior hip or proximal femur | ||
| Type 3: | HO at anterior and medial hip or proximal femur | ||
| Type 4: | HO circumferential around hip | ||
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree