Introduction and epidemiology
It has been more than 3 decades since Herndon and colleagues’ first manuscript on inhalation injury was published. It was initially reported in 1985 that inhalation injury was a major determinant of mortality in severe burn patients. The standard of care has evolved over time, but inhalation injury remains a major problem. Although sepsis is reportedly the most frequent cause of death among burned children, roughly two-thirds of burn patients who have died at the Shriners Hospitals for Children suffer from inhalation injuries. Based on data from 506,628 admissions to burn units from 1988 to 2008, burn patients with inhalation injury are more likely to die than those without inhalation injury ( P <0.001). Furthermore, when 791 burn patients from 44 hospitals were retrospectively reviewed in 2014, the mortality rate of patients with inhalation injury was 17.9% compared with 0.7% in patients without inhalation injury ( P <0.05).
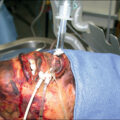
Smoke inhalation causes 5000 to 10,000 deaths annually in the United States and more than 23,000 injuries, including approximately 5000 firefighter injuries. In fact, the United States has the 10th-highest fire death rate per million people among industrialized countries. Approximately 15% of burned individuals with over 80% total body surface area (TBSA) burned who are admitted to burn centers in the United States have a concomitant smoke inhalation injury. Greater percentages of fire victims who have sustained smoke inhalation are seen in several other countries. The lung is a critical organ, and progressive respiratory failure associated with pulmonary edema is a pivotal determinant of mortality. Although not as lethal, smoke inhalation alone is a serious problem. According to World Health Organization estimates, more than 4 million people die from household air pollution from cooking with solid fuels ( Fig. 15.1 ).
An example of direct exposure to smoke as result of open fire using various materials as a fuel.
The inhalation of toxic materials has been of interest for a number of years, particularly because of the use of toxic gases in civilian mass casualty events. In the 1940s, two very large fires focused attention on smoke inhalation in fire accidents. The first was a fire at the Cocoanut Grove nightclub in Boston, Massachusetts, where a large number of people were trapped in a burning building and consequently sustained severe inhalation injury. , The second disaster occurred in 1947, in Texas City, Texas. A ship loaded with ammonium nitrate fertilizer exploded in the harbor and set off a chain of explosions and fires among 50 refineries and chemical plants, resulting in more than 2000 hospital admissions. Many of the victims were burned and simultaneously inhaled smoke, while many others suffered from smoke inhalation alone. Disasters like those in Boston and Texas City led to the establishment of centers for the care of burn victims and research into the pathophysiology of burn injury.
In many ways, the September 11, 2001, disaster at the Pentagon was similar to these two earlier disasters because the burn and inhalation injuries involved combustion of petroleum products. Among the 790 injured survivors of the terrorist attack on the World Trade Center in New York on September 11, 49% suffered inhalation injury. The situation was the same as in the Pentagon attack in that inhalation injury was seen in some patients who were not burned.
Inhalation injury can be classified as follows: (1) upper airway injury, (2) lower airway injury, (3) pulmonary parenchyma injury, and (4) systemic toxicity. The extent of inhalation damage depends on the fire environment: the ignition source, temperature, and the concentration and solubility of the toxic gases generated. For instance, hot air and smoke chemical compounds usually cause upper airway injury. Water-soluble materials, such as acrolein and other aldehydes, damage the proximal airways and set off reactions that inflame in the bronchi and parenchyma, whereas agents with lower water solubility, such as chlorine, phosgene, nitrogen oxide, and nitrogen dioxide (N 2 O 3 or even N 2 O 4 ), are more likely to cause insidious injury.
Pathophysiology
Injury to the oropharynx
Many of the pathophysiologic changes occurring after inhalation injury are related to edema formation in the oropharynx, bronchial areas, and parenchyma. This edema results from an increased transvascular fluid flux from vascular beds in these respective tissues. Before discussing the changes that occur in these structures after inhalation injury, a review of the forces responsible for the variables of the Starling-Landis equation should be reviewed , :
This equation describes the physical forces and physiologic mechanisms that govern fluid transfer between vascular and extravascular compartments. J v , the transvascular fluid flux, is equal to lymph flow during equilibrium states. As transvascular fluid flux increases, interstitial volume also increases (edema formation) until a new equilibrium with lymph flow occurs. K f is the filtration coefficient, an index of the total number of pores that are filtering. The number of pores could increase if a larger area of the microcirculation were perfused or if there were more pores per given area of the microcirculation. These pores are the same size as water and electrolytes, as opposed to the larger pores associated with permeability to protein. P c and P if are the hydrostatic pressures in the microcirculation and interstitial space, respectively. The reflection coefficient, σ, is an index of microvascular permeability to protein. If σ is 1, the membrane is impermeable to protein; when σ is 0, the membrane is completely permeable to protein. COP p and COP if are the oncotic or colloid osmotic pressures in the plasma and interstitial spaces, respectively.
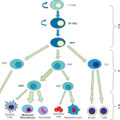
The major pathophysiology seen in the oropharynx after inhalation injury is induced by microvascular changes similar to those seen with thermal injury in other areas of the body. Heat denatures protein that, in turn, activates complement. Complement activation causes the release of histamine. , Histamine then causes the formation of xanthine oxidase, an enzyme involved in the breakdown of purines to uric acid. During this conversion, reactive oxygen species (ROS) are released. , ROS combine with nitric oxide, constitutively formed in the endothelium, to form reactive nitrogen species (RNS). The latter produce edema in the burned area by increasing the microvascular pressure and permeability to protein. , Eicosanoids and proinflammatory cytokines are also released. These, along with oxygen free radicals and interleukin 8 (IL-8), attract polymorphonuclear cells to the area. These neutrophils then amplify the release of oxygen radicals, proteases, and other materials into burned areas ( Fig. 15.2 ).
Mechanism for edema formation in the oropharynx.
The massive edema occurring in the soft tissue of the oropharynx after burns involves most variables in the Starling equation. There is a large increase in microvascular hydrostatic pressure, a decrease in interstitial hydrostatic pressure, a fall in the reflection coefficient, and an increase in interstitial oncotic pressure. , The usual treatment for burn resuscitation calls for the administration of large amounts of crystalloid solutions, which has the effect of reducing the plasma oncotic pressure. , This reduction not only affects the oncotic pressure gradient in the microcirculation but also has been reported to increase the filtration coefficient. , The result of this almost complete breakdown in control of the microvascular function and the insult of fluid administration is massive edema. This is probably nowhere more apparent than in soft tissues of the face and oropharynx. The danger to the patient is extreme. The edema may obstruct the airway, making it not only laborious or impossible to breath but also difficult for the anesthesiologist to intubate the patient ( Fig. 15.3 A). To avoid this problem, many units prophylactically perform tracheostomies on patients who have evidence of thermal injury to the upper airway on admission. However tracheostomy itself may present problems. The tube may further damage injured areas, especially the larynx. It may be time to reconsider some of these practices. Perhaps some consideration should be given to fluid resuscitation with colloids, which can prevent some of this soft-tissue edema and reduce the volume of fluids required for resuscitation. ,
Facial and airway injury after burn and smoke inhalation. (A) A facial burn is often associated with thermal injury to the upper airway. (B) Hyperemia of airway epithelium. (C) Formation of airway obstructive cast.
(A, From Cancio LC. Airway management and smoke inhalation injury in the burn patient. Clin Plast Surg . 2009;36[4]:555-567.)
Injury to the tracheobronchial area
With rare exceptions, such as inhalation of steam, the injury to the airway is usually from chemicals in smoke. The heat capacity of air is low, and the bronchial circulation is very efficient in warming or cooling airway gases so that most gasses are at body temperature as they pass the glottis. Flames must almost be in direct contact with the airway to induce thermal injury. The chemicals in smoke depend on the materials that are being burned; however, for the most part, the host response is similar. In most instances, biologic materials, such as cotton fabric, wood, grass, or products of these (e.g., cattle feces, which is commonly used as fuel in developing countries), are the fuel for the fire. Burning of these materials produces ROS and RNS, organic acids, and aldehydes that, upon inhalation, cause damage to the respiratory epithelium. The inhaled chemicals interact with the airway to induce an initial inflammatory response. In sheep that have inhaled cooled cotton smoke, there is damage to the tracheobronchial , and alveolar epithelium. Injury and loss of these cells lead to an intense inflammatory response.
Many of the studies on bronchial circulation after smoke inhalation injury have been performed in sheep because these animals have a single bronchial artery and a single lymphatic draining the lung, thus allowing measurement of pulmonary transvascular fluid flux. In these animals, a 10-fold increase in bronchial blood flow occurs within 20 minutes of smoke inhalation. These same animals demonstrate a sixfold increase in pulmonary transvascular fluid flux and a fall in Pa o 2 /Fi o 2 to 200 or less, but these changes are delayed, occurring around 24 hours after injury. The increase in bronchial blood flow not only leads to the airway-wall edema formation, which largely contributes to the airway lumen narrowing, but it also significantly increases the pulmonary transvascular fluid flux and parenchymal edema formation. , Similar findings have been reported in patients with smoke inhalation alone or a combination of large cutaneous thermal injury and smoke inhalation.
Hyperemia of the airway is such a consistent finding in smoke inhalation that it is used to diagnose the injury. Other variables that are used include injury in an enclosed space, singed nasal hair, and soot in sputum. However these latter injuries may be present but the subject may still not develop the signs of pulmonary edema characteristic of inhalation injury. Airway inflammation plays a major role in the overall response to inhalation injury (see Fig. 15.3 B and C).
As noted, there is a large sustained increase in blood flow in the airway after smoke inhalation. These changes in blood flow are associated with increased bronchial microvascular permeability to protein and small particles and pressure. Simultaneous with changes in bronchial microvasculature function, there is a loss or shedding of the bronchial columnar epithelium. , , These changes result in a perfuse transudate with a protein content similar to an ultrafiltrate of the plasma. There are also copious secretions from the goblet cells of the lining and mucosal epithelium. Early in the response, these secretions form a foam material in the airway that many have mistaken for severe pulmonary edema in patients. After several hours the transudate/exudate, exfoliated epithelium, secreted mucus, and inflammatory cells form obstructive materials in the airways. The degree of obstruction at this early stage statistically correlates with decreasing pulmonary function. With increasing time after injury, these obstructive materials formed in the upper airway may appear in the lower airway and alveoli. , This obstructive material is problematic from several standpoints. In some rare instances of severe airway injury, these materials can induce total obstruction and are life threatening ( Fig. 15.4 ). Occlusion of some bronchi or bronchioles in the setting of high nitric-oxide production can lead to a loss of hypoxic pulmonary vasoconstriction and thus increased shunt fraction. Loss of hypoxic pulmonary vasoconstriction has been reported with inhalation injury. If single bronchi are occluded while the patient is on a volume-limited ventilator, there may be overstretch, and barotrauma to the alveoli of the nonoccluded portion of the lung can occur. Nebulized anticoagulants have been used to combat the upper airway obstruction that can occur with severe inhalation injury. These are beneficial in reducing cast formation and improving pulmonary performance, , although their use in the clinical environment has not yet been reported. Airway mucosal edema and luminal obstruction after an inhalation injury occur alongside airway smooth muscle hyperreactivity. Adrenergic , and antimuscarinic bronchodilator therapies have been shown to be beneficial in reducing ventilatory peak pressure and improving pulmonary function. The initial hyperreactive response of the airways to injury and inflammation is followed by a more long-term pathogenesis of inhalation injury that includes bronchopneumonia. Pneumonia is the leading complication in the critical care of burn victims, with the incidence of pneumonia in a burn patient with inhalation injury being two- to fourfold greater than that seen in burn patients without inhalation injury. , Conceptually, the high incidence of pneumonia in burn patients with inhalation injury is associated with the loss of airway epithelium and the essential properties of these cells in innate defense. Studies that have focused on the repair of the epithelium after burn injury are limited. In an ovine model with a selected area of smoke injury to the tracheal epithelium, the epithelial repair process was completed at 18 days. Further study by this team of investigators revealed that nebulization of cefazolin and growth factors could improve the rate of airway healing. Because of the effects of pneumonia and inhalation injury on burn patient morbidity and mortality, further studies on the dynamics of airway damage and airway epithelial repair after toxic exposure are needed to improve critical burn care.
Airway obstructive cast. (A) Macroscopic views of an airway obstructive cast in sheep 48 hours after burn and smoke inhalation injury. (B) Macroscopic views of an airway cast taken from a patient with burn and smoke inhalation injury by bronchoscope. (C) Microscopic views of bronchi totally blocked by obstructive cast in sheep. (D) Mucus totally obstructing a bronchiole in a patient after burn and smoke inhalation injury. The tissue had been immunostained for mucin 5B, an upper airway-specific mucin subtype.
(B, From Nakae H, Tanaka H, Inaba H. Failure to clear casts and secretions following inhalation injury can be dangerous: Report of a case. Burns. 2001;27[2]:189-191; C, from Cox RA, Burke AS, Oliveras G, et al. Acute bronchial obstruction in sheep: Histopathology and gland cytokine expression. Exp Lung Res . 2005;31[9–10]:819-837; D, from Cox RA, Mlcak RP, Chinkes DL, et al. Upper airway mucus deposition in lung tissue of burn trauma victims. Shock. 2008;29[3]:356-361.)
The airway is richly innervated with vasomotor and sensory nerve endings. These fibers are known to release neuropeptides that can engender inflammatory responses. Neuropeptides in the upper airway are also involved in mucous secretion, thus their release and interaction with the mucosal gland epithelium can increase the early obstructive pathology that occurs with inhalation injury. , Neuroinflammation is responsible for pathophysiologic changes associated with a number of clinical conditions, including tissue injury induced by chemicals. , Lange and colleagues reported that antagonists to substance P and calcitonin gene-related peptide had a marked effect on this response when administered to sheep and mice that were injured with both burn and smoke inhalation. , In an ovine model, the combination of burn and smoke inhalation injury caused a 10-fold increase in pulmonary transvascular fluid flux and a reduction of Pa o 2 /Fi o 2 to 200 or less. These changes were reversed by neuropeptide receptor-blocking agents. Released neuropeptides can activate nitric oxide synthase (NOS), have chemokine activity, and change microvascular permeability. The resultant activities lead to the formation of ROS and RNS. Some of the latter are very potent oxidants that can damage DNA. Damage to DNA triggers activation of a DNA repair enzyme, poly(ADP-ribose) polymerase (PARP). This enzyme depletes the cell of high-energy phosphates and causes the activation of nuclear factor κB (NF-κB). , NF-κB activation induces upregulation of inducible NOS (iNOS) and IL-8, thus accelerating production of ROS and RNS. Nitric oxide and 3-nitrotyrosine (an index of RNS), and iNOS mRNA and protein, have been reported to be in the airway after smoke inhalation. , Compounds that catalyze the breakdown of peroxynitrite reduce the response to smoke inhalation. Poly(ADP-ribose) (PAR), the product of the constitutive enzyme PARP, is detectable in airway tissues after smoke inhalation. PARP inhibition prevents PAR formation, NF-κB upregulation, and 3-nitrotyrosine formation. Similarly, Lange and colleagues have reported that compounds that inhibit peroxynitrite by catalyzing its rapid breakdown likewise prevent the formation of these materials. It is interesting to note that mice missing the PARP genes or given a PARP inhibitor will not show the typical inflammatory changes usually observed with asthma. Thus, in many ways, inhalation of smoke may be similar to other forms of airway injury. The fact that the response to inhalation injury is driven by neuroinflammation suggests that the response to smoke from wood or cotton is similar.
Injury to the lung parenchyma
As noted earlier, burn and smoke inhalation induce delayed lung parenchymal changes as reflected by reduced Pa o 2 /Fi o 2, decreased compliance, and increased edema formation. The delay is dependent on the severity of the airway injury. , Lung injury is associated with an increased pulmonary transvascular fluid flux. The degree of transvascular fluid is proportional to the duration of smoke exposure and is not caused by carbon monoxide in the inhalant gas. However, the degree of arterial carbon monoxide is related to severity of inhalation injury. The factors responsible for fluid leak are codified in the Starling-Landis equation. , The variables of this equation relate fluid movement to pressure and permeability variations. With inhalation of smoke, there is a reduction in the reflection coefficient (permeability to protein), an increase in the filtration coefficient (permeability to small particles), and an increase in pulmonary microvascular pressure. , Animals exposed to smoke inhalation injury were also noted to have reduced Pa o 2 /Fi o 2 . These variables are more severely affected when the inhalation is combined with burn injury and show a good relationship to histologic injury scores and changes in transvascular fluid flux. In addition, there is a loss of hypoxic pulmonary vasoconstriction in the injured animals that may help to explain the loss of oxygenation.
As in the oropharynx, injury to the lung parenchyma is associated with PARP activation and 3-nitrotyrosine, and it is markedly reduced by the administration of iNOS or PARP inhibitors.
The venous outflow of the bronchial circulation drains into the pulmonary microcirculation at the precapillary level. Given that initial damage to the airway appeared to drive the pathophysiology of the parenchyma, investigators hypothesized that bronchial blood might deliver cytotoxic materials or cells to the pulmonary microcirculation. To test this hypothesis, several investigators have tied off the bronchial artery of sheep and then exposed the animals to smoke. , , Lung parenchymal changes are reduced by this approach, affirming the hypothesis. It has also been shown that increased bronchial blood flow after smoke inhalation injury carries inflammatory mediators to the parenchyma, augmenting the injury process. Recent ovine studies demonstrate that nebulized epinephrine (nonspecific adrenergic agonist) has similar effects after smoke inhalation injury: reduced airway blood flow, attenuated pulmonary edema, and reduction in proinflammatory mediators to levels seen in sheep with ablated bronchial circulation. , The latter observation is of particular clinical importance because the ligation/ablation of bronchial artery is not feasible in clinical practice. Another clinical importance of the nebulized epinephrine is that it can cause a bronchodilation via its β 2 -adrenergic effects. Fukuda et al. demonstrated that efficacy of nebulized epinephrine is superior to those of nebulized albuterol.
What could be the linkage among the airway, the bronchial venous drainage, and parenchymal injury to the lung? Neutrophils activated in the bronchial circulation flow out into the bronchial venous drainage. Activated polymorphonuclear cells (PMNs), especially neutrophils, are stiff. The diameter of neutrophils that have been fixed is approximately 7 μm. Because these cells have been dehydrated in alcohol as part of the fixation process, unfixed cells are much larger, on the order of 12 μm. The pulmonary capillary is small, with an average diameter of 6 μm. Normally, large neutrophils can traverse the pulmonary capillary by changing shape. However, after injury, many of the neutrophils in the bronchial areas have their F-actin activated. As a result, these cells are stiff and cannot deform. These stiff cells are carried to the pulmonary microvasculature where they are captured by the narrow pulmonary capillaries. The activated neutrophils release ROS and proteases that damage the parenchyma. The following evidence supports this concept of neutrophil cytotoxicity. Oxidative processes are well established after inhalation injury, with lipid peroxidation and release of proteolytic enzymes after injury. Moreover, administration of protease inhibitors or ROS scavengers will reduce the response to smoke inhalation , when activated PMNs lose L-selectin on their surfaces. This L-selectin shedding is prevented by treatment with an L-selectin antibody, which prevents changes in transvascular fluid flux and other aspects of parenchymal damage. Final proof of this hypothesis is provided by studies of how the response to inhalation injury is affected by depleting animals of neutrophils. In these studies of sheep depleted of their leukocytes, a large portion of the response to smoke inhalation was blocked.
Coagulopathy has increasingly been described as a critical complication of burn and smoke inhalation injury. After burn injury, there is a hypercoagulable state associated with severe deficiency of the potent endogenous anticoagulant antithrombin. In preclinical studies, supplementation with recombinant human antithrombin has been shown to attenuate pulmonary edema, downregulate proinflammatory mediators, and improve pulmonary gas exchange. , In pilot clinical studies, antithrombin deficiency after cutaneous burn was correlated with TBSA, presence of smoke inhalation, length of intensive care unit and hospital stay, morbidity severity, and mortality. Recent unpublished observations showed that of six sheep exposed to smoke inhalation, all developed some degree of pulmonary vascular emboli (clot) observable by computed tomography scan. The pathophysiology of acute lung injury secondary to burn and smoke inhalation injury is summarized in Fig. 15.5 .
Pathophysiology of burn and smoke inhalation induced acute lung injury. iNOS , Inducible nitric oxide synthase; PARP , poly(ADP-ribose) polymerase.
(From Fishman A, ed. Pulmonary Diseases and Disorders . ed 5. China: McGraw-Hill Companies; 2015:1428-1440.)
In addition to exhibiting a depletion of antioxidants as discussed earlier, burn patients are depleted of arginine. When arginine levels are low, NOS produces superoxide rather than nitric oxide. After smoke inhalation, arginase activity is also elevated. This enzyme also depletes arginine by converting it to ornithine. Administration of arginine may assist in reducing the oxidation that occurs with inhalation injury. However, the necessity of administering arginine as arginine hydrochloride (because of solubility) limits the amount that may be given intravenously without producing acidosis.
Long-term effects of inhalation injury
When earlier editions of this book were published, mortality from inhalation injury was high, and the acute inflammatory aspects of the injury were considered a major vector of mortality. Now 85% of our patients survive inhalation injury. This also translates to burn patients as a whole. Capek et al. showed a significant decrease in observed mortality data compared with historical predictions ( p <0.0001) and a 2% reduction per year in mortality over the past 30 years. Thus the future of burns will focus on protocols that improve quality of life and long-term outcomes, including protocols for the management of inhalation injury, nutrition, resuscitation, and early excision and grafting.
When patients are examined years after burn injury, they demonstrate symptoms of restrictive lung disease and reduced diffusion capacity, both of which are signs of lung fibrosis. At autopsy, both patients and animals reportedly show hyaline membrane and deposition of collagen in their lungs, changes similar to those seen in other forms of acute lung injury. , As stated earlier, two enzymes compete for arginine: NOS and arginase. NOS forms nitric oxide and RNS. Arginase forms ornithine, which is converted into polyamines and proline, leading to the formation of collagen. When NOS is active, it forms N(omega)-hydroxy-nor- l -arginine (NOHA). NOHA is broken down into nitric oxide and citrulline. NOHA is a potent inhibitor of arginase. , Thus, as long as NOS activity is elevated, arginase is inhibited. It has recently been reported that the endogenous NOS inhibitor asymmetric dimethylarginine (ADMA) begins to rise in the lung of sheep after combined burn and smoke inhalation injury. As ADMA increases, nitric oxide production falls and tissue levels of collagen increase. The increase in collagen results in hyaline membrane formation and thickening of the alveolar septum that interferes with the diffusion of oxygen into the lung. ADMA is formed in the lung on a regular basis but it is rapidly catabolized by dimethylarginine dimethylaminohydrolase (DDAH). , DDAH is inactivated by oxidation. After burn and inhalation injury, lung levels of DDAH fall as markers of oxidation rise, and, as these events occur, levels of ADMA, arginase, and collagen increase. We have previously determined that oxidation is such a serious problem that survival is dependent of the degree of oxidation. In addition, it was recently reported that levels of γ- and α-tocopherol are markedly depleted in children with thermal injuries. In sheep depleted of α- and γ-tocopherols after burn and smoke exposure, the administration of tocopherol, especially γ-tocopherol, either orally or through nebulization into the airways (more effective), restored not only lung levels of tocopherol but also normal oxidation status and pulmonary function during the acute phase of injury. Preliminary experiments using the long-term model reported by Sousse et al. indicate that the nebulization of γ-tocopherol also reduces collagen deposition; blocks elevation in arginase, proline, and ADMA levels; and restores DDAH levels.
Recent preclinical ovine studies indicate that smoke inhalation causes structural damage in the brain as seen by neuronal and astrocyte death and microhemorrhage (unpublished data). It has previously been reported that smoke-induced oxidative DNA damage in the brain is extensive, and compromised fidelity of DNA repair may underlie neurotoxicity and contribute to delayed death of hippocampal neurons. Furthermore, acute smoke exposure significantly compromises the respiratory capacity of hippocampal mitochondria. These results suggest that fire victims, especially those with smoke inhalation injury, should carefully be monitored for possible nonpulmonary organ damage, including central nervous system (CNS) dysfunction.
Finally, there have been several publications addressing the presence of inhalation injury in burns and its role in long-term outcomes. In 2019, Stockly et al. analyzed 1871 burned individuals (208 [11%] with inhalation injury, 1663 [89%] without inhalation injury; median age 40 years, 68.8% male) and found that individuals with inhalation injury were less likely to be employed at 2 years postburn compared with individuals without inhalation injury (odds ratio = 0.63, P = 0.028). In 2020, Bourgi et al. studied quality of life and their predictors in 130 burned adults, and the group found that inhalation injury was associated with total Burn-Specific Health Scale–Brief. Thus long-term outcomes in burn patients with concomitant inhalation injury warrant further resource allocation and treatment paradigms. As an example, oxandrolone, which is a testosterone analog, has been shown to alleviate pulmonary complications in burn patients 6 months postinjury; its daily administration improved lung function (maximum voluntary ventilation and maximum expired ventilation, P <0.02).
The fire environment and toxic smoke compounds
Smoke toxicity is an increasing concern because modern industrial products are changing from woods and natural materials toward lighter construction materials, synthetics, and petrochemical-based materials. These materials ignite and burn two to three times hotter and faster than conventional material and, when heated, emit a gas or smoke that is more toxic than natural biologic materials. Consequently, firefighters have less time to gain control of a fire, and victims are more likely to be incapacitated by breathing toxic gases and to sustain smoke inhalation because they have less time to escape from the burning area. Inhalation injury is caused by steam or toxic inhalants, such as fumes, gases, and mists. Fumes consist of small particles with various adherent irritants or cytotoxic chemicals that are dispersed in air. Mists consist of aerosolized irritant or cytotoxic liquids. Smoke consists of a combination of fumes, gases, mists, and hot air. Heat, toxic gases, and low oxygen levels are the most common causes of death in fires. A large variety of toxic gases and chemicals can be generated depending on the fire environment ( Table 15.1 ).
Table 15.1
Origin of Selected Toxic Compounds
From Prien T, Traber DL. Toxic smoke compounds and inhalation injury: a review. Burns Incl Therm Inj. 1988;14:451-460.
| Gases and Chemicals | Material | Source |
|---|---|---|
| Carbon monoxide |
|
|
| Cyanide |
|
|
| Hydrogen chloride |
|
|
| Phosgene | Polyvinyl chloride | Upholstery, wire/pipe coating, wall, floor, furniture coverings |
| Ammonia |
|
|
| Sulfur dioxide | Rubber | Tires |
| Hydrogen sulfide | Wool, silk | Clothing, fabric, blankets, furniture |
| Acrolein |
|
|
| Formaldehyde | Melamine resins | Household and kitchen goods |
| Isocyanates | Polyurethane | Insulation, upholstery material |
| Acrylonitriles | Polyurethane | Insulation, upholstery material |
Many of these compounds may act together to increase death, especially carbon monoxide and hydrogen cyanide. , A synergism between these compounds has been found to increase tissue hypoxia and acidosis and may decrease cerebral oxygen consumption and metabolism. , Hydrogen sulfide would also be predicted to synergize with carbon monoxide because both cyanide and hydrogen sulfide are inhibitors of mitochondrial cytochrome oxidase. Victims may be incapacitated by the blinding and irritating effects of smoke and by the decreasing oxygen concentration that occurs with combustion and results in progressive hypoxia.
Toxic gases such as carbon monoxide and cyanide rarely damage the airway but instead affect gas exchange and produce more systemic effects. Thus it is important to obtain information on the source of the fire and the combustion products generated when treating a fire victim (see Table 15.1 ). It is also important to know the duration of exposure and the extent to which the fire victim was in an enclosed area because this relates to the dose of toxic materials received.
Carbon monoxide
Carbon monoxide is an odorless, colorless gas that is produced by incomplete combustion of many fuels, especially cellulolytic (cellulose) products such as wood, paper, and cotton. Carbon monoxide toxicity remains one of the most frequent immediate causes of death after smoke-induced inhalation injury. The predominant toxic effect of carbon monoxide is attributed to its binding to hemoglobin (Hb) to form carboxyhemoglobin (COHb). The affinity of carbon monoxide for Hb is approximately 200 to 250 times higher than that of oxygen. Inhalation of a 0.1% carbon monoxide mixture may result in generation of a COHb level as high as 50% of the total Hb. The competitive binding of carbon monoxide to Hb reduces delivery of oxygen to tissues, leading to severe hypoxia, especially in the most vulnerable organs, such as the brain and heart, where oxygen extraction is considerably higher than that in most other organs. The oxygen-Hb dissociation curve loses its sigmoid shape and is shifted to the left, thus further impairing tissue oxygen availability. , In addition, the ability of carbon monoxide to bind to intracellular cytochromes and to other metalloproteins contributes to its toxicity. This competitive inhibition with cytochrome oxidase enzyme systems (most notably cytochromes A and P450) results in an inability of cellular systems to use oxygen. , Shimazu and his colleagues have shown that extravascular binding of carbon monoxide to cytochromes and other structures accounts for 10% to 15% of total body carbon monoxide stores. This intracellular binding of carbon monixide explains its two-compartment elimination from the circulation. Miro and colleagues reported that carbon monoxide inhibits cytochrome C oxidase activity in lymphocytes. The electron chain dysfunction induced by carbon monoxide may cause electron leakage, leading to superoxide production and mitochondrial oxidative stress.
Although smoke inhalation commonly affects the respiratory system, CNS disturbances can also develop. CNS signs can be classified as being related to either acute or delayed toxicity. The veterinary literature contains a few reports on the neurologic consequences of smoke inhalation. In dogs, smoke inhalation produces lesions that are consistent with acute carbon monoxide toxicity. Lesions are confined to the caudate nucleus, globus pallidus, and the substantia nigra bilaterally, as well as the cerebellum, cerebral cortex, and dorsal thalamus. A case report by Kent and colleagues describes the clinicopathologic sequelae in acute carbon monoxide toxicity.
Symptoms and diagnosis of carbon monoxide poisoning
Symptoms of carbon monoxide poisoning predominantly manifest in organs and systems with high oxygen utilization. The severity of clinical manifestations varies depending on carbon monoxide concentration. For instance, CNS symptoms such as headache, confusion, and collapse may occur when the blood COHb level is 40% to 50%. Symptoms such as unconsciousness, intermittent convulsions, and respiratory failure may occur if the COHb level exceeds 60%, eventually leading to death if exposure continues. The cardiovascular manifestations may result in tachycardia, increase in cardiac output, dysrhythmias, myocardial ischemia, and hypotension depending on severity of poisoning. The correlation between clinical manifestation and severity of carbon monoxide poisoning is summarized in Table 15.2 .
Table 15.2
Symptoms and Signs at Varying Concentrations of Carboxyhemoglobin (COHb)
From Einhorn IN. Physiological and toxicological aspects of smoke produced during the combustion of polymeric materials. Environ Health Perspect . 1975;11:163-189; Schulte JH. Effects of mild carbon monoxide intoxication. Arch Environ Health. 1963;7:524-530.
| COHb % | Symptoms |
|---|---|
| 0–10 | None |
| 10–20 | Tightness over forehead, slight headache, dilation of cutaneous blood vessels |
| 20–30 | Headache and throbbing in the temples |
| 30–40 | Severe headache, weakness, dizziness, dimness of vision, nausea, vomiting, collapse |
| 40–50 | As above; greater possibility of collapse, syncope, increased pulse and respiratory rate |
| 50–60 | Syncope, increased pulse and respiratory rate, coma, intermittent convulsions, Cheyne-Stokes respirations |
| 60–70 | Coma, intermittent convulsions, depressed cardiac and respiratory function, possible death |
| 70–80 | Weak pulse, slow respirations, death within hours |
| 80–90 | Death in <1 hour |
| 90–100 | Death within minutes |
Diagnosis should be based on direct measurement of COHb levels in arterial or venous blood by co-oximetry, taking into account that venous blood underestimates the arterial COHb content. Diagnosis may be facilitated by use of onsite portable breath analyzers. The inability to differentiate oxyhemoglobin from COHb limits the use of a pulse oximeter. The use of blood gas analyzers that estimate sulfur dioxide based on measurement of dissolved partial pressure of oxygen should also be avoided. Measuring acid-base balance, plasma lactate levels, and bicarbonate is helpful in managing carbon monoxide poisoning with accompanying lactic or metabolic acidosis. It is important to note that high oxygen concentrations are usually administered to the victim in transit to the hospital, and some delay from cessation of exposure to measurement of carbon monoxide may limit evaluation of the true extent of exposure. A nomogram has been developed that can relate the COHb levels of a patient to the values that may have been present at the time of smoke inhalation, and this can be used to estimate the true degree of inhalation injury.
Hydrogen cyanide
Hydrogen cyanide, the gaseous form of cyanide, is generated by the combustion of nitrogen- and carbon-containing substances, such as wool, silk, cotton, and paper, as well as synthetic substances, such as plastic and other polymers. Combustion of these materials may produce the rapid and lethal incapacitation of a victim at the fire source. Hydrogen cyanide is a colorless gas with the odor of bitter almonds; however, it is difficult to detect at the site of the fire. Hydrogen cyanide is cytotoxic mainly owing to its reversible inhibition of cytochrome C oxidase, the thermal oxidase of the respiratory chain, through interaction with the ferric ion of cytochrome A 3 . This suppresses cellular oxygenation and causes tissue anoxia. Hydrogen cyanide also adversely affects a number of other enzyme systems; it is also toxic by virtue of its combination with essential metal ions, formation of cyanohydrins with carbonyl compounds, and sequestration of sulfur as a thiocyanate.
The importance of hydrogen cyanide in smoke inhalation injuries is reflected by a study of residential fires in Paris, France, showing that mean blood hydrogen cyanide concentrations in both fire victims who survived (21.6 mol/L) and those who died (116.4 mol/L) were significantly higher than those in control subjects (5 mol/L) and that levels in fire victims who died were significantly higher than those in survivors. A study of 144 fire victims in Dallas County, Texas, showed results consistent with the Paris study. Elevated hydrogen cyanide concentrations are directly related to the probability of death, suggesting that its poisoning rather than carbon monoxide poisoning may be the predominant cause of death in some fire victims. Hydrogen cyanide also played a greater role in mortality after an aircraft fire at Manchester International Airport in the United Kingdom in 1985. These patients were not severely burned. The large majority (87%) of the 54 individuals who died had potentially lethal levels of hydrogen cyanide in their blood, whereas only 21% of these fire victims had COHb levels exceeding 50%. This strongly suggests that, under certain conditions, hydrogen cyanide can be a more important determinant of morbidity and mortality after smoke inhalation than carbon monoxide, which is usually regarded as the primary toxic threat. Smoke is also an often overlooked source of hydrogen cyanide exposure in terrorist bombings. After the first World Trade Center bombing in 1993, traces of hydrogen cyanide were found in the vans where the explosion originated. The US Centers for Disease Control and Prevention and the Department of Homeland Security consider hydrogen cyanide among the most likely agents of chemical terrorism. It possesses all attributes of an ideal terrorist weapon: it is plentiful, readily available, and easily obtainable because of its widespread use in industry and laboratories. In addition, the use of hydrogen cyanide does not require any special knowledge. It is capable of causing mass incapacitation and casualties, and it can cause mass confusion, panic, and social disruption.
Symptoms and diagnosis of cyanide poisoning
Diagnosis at the fire scene may be difficult. Poisoning may results in CNS, respiratory, and cardiovascular dysfunction caused by inhibition of oxidative phosphorylation, depending on the concentration of hydrogen cyanide inhalation ( Table 15.3 ).
Table 15.3
Symptoms of Cyanide Toxicity
| Symptoms in Low or Moderate Inhaled Cyanide Concentrations | Symptoms in Moderate or High Inhaled Cyanide Concentrations |
|---|---|
|
|
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree