![]() Visit Elsevier eBooks+ (
eBooks.Health.Elsevier.com
) for complete set of videos.
Visit Elsevier eBooks+ (
eBooks.Health.Elsevier.com
) for complete set of videos.
Introduction
The multitude of respiratory complications caused by smoke inhalation, flame burns, and their treatment epitomize the clinical challenges that confront health care workers. Smoke inhalation injury and its sequelae impose demands on the practitioners who play a central role in its clinical management. These demands may range from intubation and resuscitation of victims in the emergency room to assistance with diagnostic bronchoscopies, performance of pulmonary function studies, monitoring of arterial blood gases, airway maintenance, chest physiotherapy, and mechanical ventilator management. Additional demands are placed on the practitioners in the rehabilitation phase in determining disability or limitations diagnosed by pulmonary function studies or cardiopulmonary stress testing. It is imperative that a well-organized, protocol-driven approach to respiratory care of the burn patient be used so that improvements can be made and the morbidity and mortality associated with inhalation injury can be reduced ( Box 17.1 ). This chapter provides an overview of the common hands-on approaches to the treatment of inhalation injury, with emphasis on mucociliary clearance techniques, pharmacologic adjuncts, mechanical ventilation, infection control, and the late complications associated with inhalation injury.
Box 17.1
Inhalation Injury Treatment Protocol
-
■
Titrate humidified oxygen to maintain SaO 2 >90%
-
■
Cough, deep breath exercises every 2 h
-
■
Turn patient side to side every 2 h
-
■
Chest physiotherapy every 4 h
-
■
Aerosolize 3 cc of 20% N-acetylcysteine every 4 h with a bronchodilator
-
■
Alternate aerosolizing 5000 units of heparin with 3 cc of normal saline every 4 h
-
■
Nasotracheal suctioning as needed
-
■
Early ambulation on postoperative day 5
-
■
Sputum cultures for intubated patients every M-W-F
-
■
Pulmonary function studies before discharge and at outpatient visits
-
■
Patient/family education regarding inhalation injury
-
■
The protocol is continued for 7 days.
Bronchial hygiene therapy
Airway clearance techniques are an essential component of respiratory management of patients with smoke inhalation. Bronchial hygiene therapy is a term used to describe several of the modalities intended to accomplish this goal. Therapeutic coughing, chest physiotherapy, bronchial drainage and positioning, percussion and vibration, early ambulation, airway suctioning, and therapeutic bronchoscopy have been effective in the removal of retained secretions.
Therapeutic coughing
Therapeutic coughing functions to promote airway clearance of excess mucus and fibrin casts in the tracheal bronchial tree. Impairing the cough mechanism may result in retained secretions, bronchial obstruction, atelectasis, and/or pneumonia. A cough can either be a reflex or a voluntary action. The mechanisms of a cough include:
-
1.
A deep inspiration
-
2.
The closure of the glottis
-
3.
Contraction of the muscles in the chest wall, abdomen, and pelvic floor
-
4.
Opening of the glottis
-
5.
A rapid, expulsive exhalation phase.
During a cough, alveolar, pleural, and subglottic pressures may rise as much as 200 cm H 2 O. A failure of the cough mechanism may be caused by an impairment of any step in the sequence described. When this occurs, it is necessary to perform techniques that are used to improve the cough.
Series of three coughs
The patient is asked to start a small breath and small cough, followed by a bigger breath and harder cough, and finally a very deep breath and hard cough. This technique is particularly effective for postoperative patients who tend to splint from pain.
Tracheal tickle
The respiratory therapist places their index and middle fingers flat in the patient’s sternal notch and gently massages inward in a circular fashion over the trachea. This is most effective with obtunded patients or with patients recovering from anesthesia.
Cough stimulation
Patients with artificial airways cannot cough normally because a tube is placed either between their vocal cords (endotracheal tube) or below their cords (tracheostomy). Adequate pressure cannot be built up without the cords in close proximity. A cough may be stimulated by inflating the cuff on the tube, giving a large and rapid inspiration with the manual resuscitation bag, holding the breath for 1 to 2 s, and rapidly allowing the bag to release and exhalation to ensue. This technique is normally performed by two persons, and it is made more effective with one therapist performing vibration and chest compressions from the time of the inspiratory hold all during exhalation. Cough and deep breathing exercises are encouraged every 2 h to aid in removing retained secretions.
Chest physiotherapy
The definition of chest physiotherapy has progressed to gravity-assisted bronchial drainage with chest percussion and vibrations. Studies have shown that the combination of techniques is effective in secretion removal.
Bronchial drainage/positioning
Bronchial drainage/positioning is a therapeutic modality that uses gravity-assisted positioning designed to improve pulmonary hygiene in patients with inhalation injury or retained secretions. Studies have shown that a patient’s arterial oxygenation may fall during bronchial drainage/positioning. Therefore it is common practice in intensive care units to turn patients side to side every 2 h to aid in mobilizing secretions ( Fig. 17.1 ).
Patient positioning for secretion mobilization.
Percussion
Percussion aids in the removal of secretions from the tracheal bronchial tree. It is performed by cupping the hand to allow a cushion of air to enter between the therapist’s hand and the patient. If this is done properly, a popping sound will be heard when the patient is percussed. There should be a towel between the patient and the therapist’s hand to prevent irritation of the skin. Percussion is applied over the surface landmarks of the bronchial segments that are being drained. The hands rhythmically and alternately strike the chest wall. Incisions, skin grafts, and bony prominences should be avoided during percussion ( Fig. 17.2 ).
Chest physiotherapy techniques.
Vibration/shaking
Vibration/shaking is a movement used to move loose secretions to larger airways so that they can be coughed up or removed by suctioning. Vibration involves the rapid shaking of the chest wall during exhalation. The percussor vibrates the thoracic cage by placing both hands over the percussed areas and vibrating into the patient, isometrically contracting or tensing the muscles of their arms and shoulders. Mechanical vibrations have been reported to be clinically effective. Gentle mechanical vibration may be indicated for patients who cannot tolerate manual percussion ( Fig. 17.3 ). Chest physiotherapy techniques should be used every 2 to 4 h for patients with retained secretions.
Gentle mechanical chest vibrations.
Early ambulation
Early ambulation is another effective means of preventing respiratory complications. Patients routinely should be helped out of bed on postoperative days 3 to 5, and they should be encouraged to ambulate and sit in a chair. With the appropriate use of analgesics, even patients on continuous mechanical ventilation can be assisted out of bed and into a chair ( Fig. 17.4 ). The rocking chair ( Fig. 17.5 ) has several beneficial effects:
-
■
The patient can breathe with regions of the lungs that are normally hyperventilated.
-
■
Muscular strength and tone are preserved.
-
■
Contractions are prevented, and exercise tolerance is maintained.
Early ambulation.
Patient up out of bed, secretions being mobilized by rocking, and chest physiotherapy techniques.
Airway suctioning
Airway suctioning is another method of clearing an airway. Normal bronchial hygiene is usually accomplished by the mucociliary escalator process. When these processes are not effective in maintaining a clear airway, tracheobronchial suctioning is recommended. Nasotracheal suctioning is intended to remove accumulated secretions and other foreign material from the trachea that cannot be removed by the patient’s spontaneous cough or by less invasive procedures. Nasotracheal suctioning refers to the insertion of a suction catheter through the nasal passages and pharynx into the trachea to aspirate secretions or foreign material.
The first step in this process is to hyperoxygenate the patient with 100% oxygen. The patient should be positioned in the Fowler position, and the catheter slowly advanced through the nares to a point just above the larynx. The operator then listens for air sounds at the proximal end of the catheter. When airflow is felt to be strongest and respiratory sounds loudest, the tip of the catheter is immediately above the epiglottis. On inspiration, the catheter is advanced into the trachea. After the vocal cords have been passed, a few deep breaths are allowed, and the patient is reoxygenated. Suction begins while the catheter is slowly withdrawn from the trachea. The patient should not be suctioned for more than 15 s without being reoxygenated.
Suctioning is not without potential hazards. , Complications include irritation of the nasotracheal mucosa with bleeding, abrupt drops in Pao 2 , vagal stimulation, and bradycardia. Preoxygenating and limiting suction time have been shown to decrease or eliminate the fall in Pao 2 . Sputum cultures should be performed for microbiologic identification when they are clinically indicated.
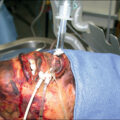
Therapeutic bronchoscopy
When all other techniques fail to remove secretions, the use of the fiberoptic bronchoscope may be beneficial. In addition to its diagnostic functions, bronchoscopy retains important therapeutic applications. The fiberoptic bronchoscope is small in diameter, flexible, and has a steerable tip that can be maneuvered into the fourth- or fifth-order bronchi for examination or specimen removal. Copious secretions encountered in patients with inhalation injury may require repeated bronchoscopic procedures when more conservative methods are unsuccessful.
Pharmacologic adjuncts
Bronchodilators can be helpful in select cases. Inhalation injury to the lower airways results in a chemical tracheobronchitis, which can produce wheezing and bronchospasms. Most drugs used in the management of bronchospasms are believed to control bronchial muscle tone. Aerosolized sympathomimetics are effective in two ways: they cause bronchial muscle relaxation, and they stimulate mucociliary clearance. A newer compound of note is metaproterenol, which is available as a cartridge inhaler, as an aerosolized liquid, as a tabular oral medication, or as a syrup. The recommended oral dose is 10 to 20 mg every 6 to 8 h, or one to two puffs every 3 to 4 h as an inhaled bronchodilator with a duration of action of 1 to 5 h.
Albuterol can also be aerosolized or be administered orally or parenterally. Albuterol is available in a metered cartridge inhaler, and its standard dose is one to two puffs three to four times daily. Aerosolized albuterol has a duration of action of approximately 4 to 6 h.
Racemic epinephrine is used as an aerosolized topical vasoconstrictor, bronchodilator, and secretion bond breaker. The vasoconstrictive action of racemic epinephrine is useful in reducing mucosal and submucosal edema within the walls of the pulmonary airways. A secondary bronchodilator action serves to reduce potential spasms of the smooth muscles of the terminal bronchioles. Water, employed as a diluent for racemic epinephrine, serves to lower both adhesive and cohesive forces of the retained endobronchial secretions, thus serving as a bond-breaking vehicle. Racemic epinephrine has also been used for the treatment of postextubation stridor. Its mode of action is thought to be related to the vasoconstrictive activity, with the resultant decrease in mucosal edema. Aerosolized treatments may be given every 2 h as long as the heart rate is not increased.
Hypertonic saline offers a theoretically more effective form of mucokinetic therapy. The deposition of hypertonic droplets on the respiratory mucosa causes the osmotic attraction of fluids from the mucosal blood vessels and tissues into the airway. Thus a “bronchorrhea” is induced. The watery solution helps dilute the respiratory tract secretions and increase their bulk, thereby augmenting expectoration. Furthermore, there is evidence that hypertonic saline has a direct effect on the mucoprotein DNA complexes, and by reducing the cohesive intramolecular forces, the salt helps reduce the viscous properties of the mucoid fluid. Excessive use of hypertonic saline is not recommended because burn patients cannot tolerate the sodium load and may develop edema.
Oxandrolone is a synthetic testosterone analog that has been shown to significantly reduce hypermetabolism and significantly increase height percentile, bone mineral content, lean body mass, and strength in pediatric burn patients. A 2012 report showed that pediatric patients treated with oxandrolone for 1 year had significantly higher maximum voluntary ventilation compared with untreated patients. Also, during maximal exercise, the subjects treated with oxandrolone had a significantly higher maximal minute ventilation ( V ˙ ). The administration of oxandrolone may be used as an agent in the future to improve lung function in burn patients.
Aerosolized acetylcysteine is a powerful mucolytic agent in use in respiratory care. Acetylcysteine contains a thiol group; the free sulfhydryl radical of this group is a strong reducing agent that ruptures the disulfide bonds that give stability to the mucoprotein network. Agents that break down these disulfide bonds produce the most effective mucolysis. Of note, acetylcysteine is an irritant to the respiratory tract. It can cause mucosal changes, and it may induce bronchospasms. For this reason, patients are evaluated for signs of bronchospasms, and a bronchodilator may be added if necessary. Acetylcysteine has proved to be effective in combination with aerosolized heparin for the treatment of inhalation injury in animal studies.
Last, heparin-acetylcysteine combinations have been used as scavengers for the free oxygen radicals produced when alveolar macrophages are activated either directly by chemicals in smoke or by one or more of the compounds in the arachidonic oxidative cascade. Animal studies have shown an increased ratio of partial pressure of oxygen in arterial blood/ fraction of inspired oxygen (PaO 2 :FiO 2 ), decreased peak inspiratory pressures, and a decreased amount of fibrin cast formation with heparin-acetylcysteine combination therapy. In a retrospective review, Desai et al. have shown that the use of heparin and N-acetylcysteine is effective in pediatric patients with inhalation injury. Results indicated a significant decrease in reintubation rates and the incidence of atelectasis, and showed improved mortality for patients treated with the combination therapy. Therefore a standard treatment for patients with inhalation injury may include 5000 to 10,000 units of heparin and 3 mL normal saline nebulized every 4 h, alternating with 3 to 5 mL of 20% acetylcysteine for 7 days. This ensures that the patient receives an aerosolized treatment every 2 h. Baseline and daily clotting analyses are recommended for the entire length of the aerosolized treatments.
Mechanical ventilation
Over the past 30 years, and particularly over the past decade, there has been an increase in new ventilation techniques that present alternatives for the treatment of patients with smoke inhalation. Unfortunately, although the number of options available to the clinician has appeared to increase, randomized and placebo-controlled clinical trials defining the specific role for each mode of ventilation and comparing them with other modes of ventilation have not been forthcoming. The recommendations from the American College of Chest Physicians Consensus Conference on Mechanical Ventilation serve as general guidelines. The conference concluded:
-
■
The clinician should choose a ventilator mode that has been shown to be capable of supporting oxygenation and ventilation and that the clinician has experience in using.
-
■
An acceptable oxygen saturation should be targeted.
-
■
Based primarily on animal data, a plateau pressure of greater than 35 cm H 2 O is cause for concern. However, with clinical conditions that are associated with a decreased chest wall compliance, plateau pressures greater than 35 cm H 2 O may be acceptable.
-
■
To accomplish the goal of limiting plateau pressures, Pco 2 values should be permitted to rise (permissive hypercapnia) unless other contraindications exist that demand a more normal Pco 2 or pH.
-
■
Positive end-expiratory pressure (PEEP) is useful in supporting oxygenation. An appropriate level of PEEP may be helpful in preventing lung damage. The level of PEEP required should be established by empirical trials and reevaluated on a regular basis.
-
■
Large tidal volumes (10–12 mL/kg) with PEEP may be needed to improve oxygenation if the use of protective ventilation strategies becomes ineffective. Peak flow rates should be adjusted as needed to satisfy patient inspiratory needs. Care must be taken to avoid the consequences of using high ventilator pressures if large tidal volumes are required.
Animal studies showed a reduction in ventilator-induced injury with a reduction in plateau pressures to 35 cm H 2 O by increasing PEEP and decreasing tidal volume. A number of clinical trials have been conducted to support this treatment strategy. A metaanalysis of these trials was conducted by the Cochrane Anesthesia Review Group in 2007. It showed a reduction in mortality and duration of mechanical ventilation with the use of plateau pressure at less than 30 cm H 2 O and tidal volume at less than 7 mL/kg body weight. In light of this evidence, the tidal volumes used when initiating mechanical ventilation should be 6 to 8 mL/kg of predicted body weight. If the patient becomes obstructed with fibrin cast and presents with an acute increase in Paco 2 and decrease in Pao 2 , the clinician should first provide aggressive pulmonary toilet and then consider changing over to volume ventilation with higher tidal volumes. If ventilation continues to worsen, tidal volumes of 10 to 12 mL/kg may be needed to provide adequate mechanical ventilation.
Modes of ventilation
Volume control mode
In the volume control mode of ventilation, the ventilator automatically delivers a set number of breaths at a rate selected by the operator. The ventilator will deliver a set tidal volume for each breath, guaranteeing a minimum level of minute ventilation in the sedated or paralyzed patient. The tidal volume, inspiratory flow rate, flow waveform, sensitivity, and control rate are set. This mode of ventilation is often used in patients with acute respiratory distress syndrome (ARDS) to directly set the tidal volume delivered to the patient with each breath.
Disadvantages of volume control are as follows:
-
■
Excessive patient work occurs in case of inadequate peak flow or sensitivity settings, especially if the ventilator drive of the patient is increased.
-
■
It is often poorly tolerated in awake, nonsedated subjects, and it can require sedation to ensure synchrony of patient and ventilator.
-
■
It can cause respiratory alkalosis.
-
■
It may worsen air trapping with patients with chronic obstructed pulmonary disease (COPD).
Synchronized intermittent mandatory ventilation
Synchronized intermittent mandatory ventilation (SIMV) combines a preset number of ventilator-delivered mandatory breaths of the preset tidal volume with the facility for intermittent patient-generated spontaneous breaths. , The advantages are as follows:
-
■
The patient can perform a variable amount of respiratory work, and the security of a preset mandatory level of ventilation is maintained.
-
■
SIMV allows for variation in the level of partial ventilation support from near total ventilation support to spontaneous breathing.
-
■
It can be used as a weaning tool.
Disadvantages include:
-
■
Hyperventilation with respiratory alkalosis could occur.
-
■
Excessive work of breathing because of a poorly responsive demand valve, suboptimal ventilation circuits, or inappropriate flow delivery could occur.
-
■
In each case, extra work is imposed on the patient during spontaneous breaths.
Pressure control mode
In pressure-controlled ventilation, all breaths are time- or patient-triggered, pressure-limited, and time-cycled breaths. The length of inspiration, pressure level, and back-up rate are set by the operator. The tidal volume is based on the compliance and resistance of the patient’s lungs, the ventilator system, and the preset pressure.
Pressure support ventilation
Pressure support ventilation (PSV) is a pressure-targeted, flow-cycled mode of ventilation in which each breath must be triggered by the patient. It is used both as a mode of ventilation during stable ventilation support periods and as a weaning method. It is primarily designed to assist spontaneous breathing; thus, the patient must have an intact respiratory drive.
Advantages include:
-
■
It is generally considered a comfortable mode of ventilation for most patients.
-
■
It can be used to overcome airway resistance caused by the endotracheal tube.
-
■
Pressure support may be useful in patients who are difficult to wean.
Disadvantages include:
-
■
The tidal volume is not controlled, and it is dependent on respiratory mechanics, cycling frequency, and synchrony between the patient and ventilator.
-
■
Pressure support may be poorly tolerated in some patients with high airway resistances because of the preset high initial flow rates.
Alternate modes of ventilation
Over the past three decades, a new concept of ventilation has emerged in the treatment of ARDS patients. In severe cases of ARDS, only a small part of the lung parenchyma remains accessible to gas delivered by mechanical ventilation. , As a consequence, tidal volumes of greater than 10 mL/kg may overexpand and injure the remaining normally aerated lung parenchyma. High airway pressures may result in overdistension and local hyperventilation of more compliant parts of the lung. Overdistension of lungs in animals has been shown to produce diffuse alveolar damage. This is the primary reason that alternative modes of ventilation, which are all based on a reduction of end-inspiratory airway pressures and/or tidal volumes delivered to the patient, have been developed and are used by many clinicians caring for patients with severe forms of acute or chronic respiratory failure. The following four alternative modes of ventilation will be discussed: high-frequency ventilation, high-frequency percussive ventilation, airway pressure release ventilation, and volumetric diffusive ventilation.
High-frequency ventilation
High-frequency ventilation (HFV) is the administration of small tidal volumes of 1 to 3 mL/kg at high frequencies of 100 to 3000 cycles/min. This mode of ventilation is based on a marked reduction in tidal volumes and airway pressures, and it has the greatest potential for reducing pulmonary barotraumas. There are different types of high-frequency ventilation techniques. The two most common are high-frequency jet ventilation (HFJV) and high-frequency percussive ventilation (HFPV).
HFJV is the only high-frequency mode routinely used to ventilate patients with ARDS, and it is primarily used in Europe. This type of ventilation uses a brief jet of gas at a high frequency. Comparative data concerning the advantages of HFJV over conventional ventilation are limited. There is no agreement, however, that HFJV is better than conventional mechanical ventilation in ARDS.
HFPV has shown some promise in the ventilation of patients with inhalation injury. HFPV refers to ventilation using the Volume Diffusive Respiration (VDR) ventilator, and it oscillates between inspiratory and expiratory airway pressures. Clinical studies indicate that this mode of ventilation may aid in reducing pulmonary barotrauma. , In a retrospective study, Cortiella et al. have shown a decreased incidence of pneumonia and peak inspiratory pressure and an improved P/F ratio in children ventilated with the use of HFPV compared with controls. In the first prospective randomized study of HFPV, Mlcak et al. have shown a significant decrease in the peak inspiratory pressures needed to ventilate pediatric patients with inhalation injury. No significant differences were found for incidence of pneumonia, P/F ratios, or mortality.
Based on clinical experience, the following guidelines are suggested for initial setup of HFPV in children ( Table 17.1 ). The pulsatile flow rate should be set at 20 cm H 2 O, the pulse frequency (high rate) should be set between 500 and 600 Hertz (Hz), and the low respiratory rate should be set between 15 and 20. Oscillatory PEEP levels should be initially set at approximately 3 cm H 2 O, and demand PEEP should be set at 2 cm H 2 O. Ventilator settings are adjusted based on the patient’s clinical condition and blood gas values. To improve oxygenation, the ventilator can be switched to a more diffusive mode (increased pulse frequency); to eliminate carbon dioxide, the ventilator can be switched to a more convective mode (decreased pulse frequency). With HFPV, subtidal volumes are delivered in a progressive stepwise fashion until a preset oscillatory equilibrium is reached and exhalation is passive.
Table 17.1
High-Frequency Percussive Ventilation Set-Up Guidelines
| Variable | Settings |
|---|---|
| Pulsatile Flow Rate | 20 cm H 2 O |
| Pulse Frequency (high rate, Hz) | 500–600 |
| Low Respiratory Rate | 15–20 |
| I:E Ratio | 1:1 or 2:1 |
| Oscillatory PEEP | 3 cm H 2 O |
| Demand PEEP | 2 cm H 2 O |
I:E , inspiratory-expiratory ratio; PEEP, positive end-expiratory pressure.
Clinicians must be familiar with each technique used and its possible limitations. There must be adequate humidification of the respiratory gases, or severe necrotizing tracheobronchitis can occur. Special delivery devices for providing adequate humidification during HFV are required. It is not clear when and how HFV should be used after inhalation injury. As the methodology for HFPV evolves, it is anticipated that HFPV will play a larger role in the care of select mechanical ventilation–dependent populations.
Airway pressure release ventilation
Airway pressure release ventilation (APRV) is a pressure-regulated mode of ventilation support that allows for time-cycled decreases in pressure to facilitate CO 2 elimination. This mode allows spontaneous breathing while limiting airway pressures; therefore, it may limit the amount of sedatives or neuromuscular blocking agents needed. APRV is a protective ventilator strategy that uses inverse ratio ventilation at two levels of PEEP. Several limited studies have suggested that APRV may be beneficial for the treatment of burn patients who develop ARDS. Evidence-based recommendations to use this mode of ventilation await outcome studies.
Volumetric diffusive ventilation
The VDR is a pneumatically powered, pressure-limited ventilator that stacks oscillatory breaths to a selected peak airway pressure by means of a sliding venturi called a Phasitron . After inspiration, exhalation is passive and ends at a selected level of oscillatory continuous positive airway pressure (CPAP). Studies comparing VDR to high-volume strategies have shown VDR improves gas exchange, decreases peak pressures, and lowers mortality. However, there is a need to compare VDR to the low tidal volume ventilation practiced more recently. Usage of the VDR requires special training; the other disadvantages are the inability to monitor tidal and minute volumes and the requirement of humidified air and nebulized saline to prevent airway desiccation.
Ventilator settings
A large multicentered study by the Acute Respiratory Distress Syndrome Network evaluated the use of volume ventilation with low versus high tidal volume for ARDS. This study documented a decreased incidence of mortality in patients with ARDS who were ventilated with small tidal volumes. Based on this study in 2000, it has become clinically accepted practice to use low tidal volumes when initially setting up mechanical ventilation ( Table 17.2 ).
Table 17.2
Targeted Mechanical Ventilation Guidelines in Children
| Variable | Settings |
|---|---|
| Tidal Volumes | 6–8 mL/kg |
| Respiratory Rate | 12–45 breaths/min |
| Plateau Pressures | <30 cm H 2 O |
| I:E Ratio | 1:1–1:3 |
| Flow Rate | 40–100 L/min |
| PEEP | 7.5 cm H 2 O |
I:E , inspiratory-expiratory ratio; PEEP , positive end-expiratory pressure.
Tidal volumes
In volume-cycled ventilation, a machine-delivered tidal volume is set to be consistent with adequate gas exchange and patient comfort. The tidal volume selected for burn patients normally varies between 6 and 8 mL/kg of predicted body weight. Numerous factors, such as lung/thorax compliance, system resistance, compressible volume loss, oxygenation, ventilation, and barotrauma, are considered when volumes are selected. Sousse et al. showed in 2015 that the use of higher tidal volumes in pediatric burn patients with inhalation injury may decrease the incidence of ARDS and atelectasis as well as the number of days on a ventilator when compared with lower tidal volumes. Of critical importance is the avoidance of overdistension. This can generally be accomplished by ensuring that peak airway and alveolar pressures do not exceed a maximum target. Many would agree that a peak alveolar pressure greater than 35 cm H 2 O in adults raises concern regarding the development of barotrauma, and ventilator-induced lung injury increases. , Expired tidal volumes should be measured for accuracy at the connection between the patient’s wye and the artificial airway.
The range of tidal volumes will vary depending on the disease process, with some diseases requiring maximum tidal volumes and others needing less. Severe interstitial diseases such as pneumonia and ARDS may require a tidal volume of greater than 8 mL/kg to adequately inflate the lungs and improve gas exchange if protective ventilation strategies become inadequate, particularly in pediatric burn patients.
Respiratory rate
Setting of the mandatory respiratory rate is dependent on mode of ventilation selected, delivered tidal volume, dead space-to-tidal volume ratio, metabolic rate, targeted Paco 2 levels, and level of spontaneous ventilation. With adults, the set mandatory rate normally varies between 4 and 20 breaths/min, with most clinically stable patients requiring mandatory rates in the 8 to 12 range. It is important to have targeted arterial blood gas values set to aid the clinical team in proper management ( Table 17.3 ). Along with Paco 2 , pH, and patient comfort, the primary variable controlling the selection of the respiratory rate is the development of air trapping and auto PEEP.
Table 17.3
Arterial Blood Gas Goals
| Variable | Goal |
|---|---|
| pH | 7.25–7.45 |
| PaO 2 | 55–80 mm Hg or SaO 2 of 88%–95% |
| PaCO 2 | 35–55 mm Hg (permissive hypercapnia can be used as long as pH >7.25) |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree