Introduction
Inhalation injury, or smoke inhalation injury, is defined as the damage that occurs to the lung and airways after inhalation of the products of combustion and the clinical manifestations of that damage.
Inhalation injury is particularly important for burn healthcare professionals for several reasons. First, inhalation injury is a fairly common finding in many burn patients. Second, the presence of an inhalation injury profoundly impacts the clinical course of burn patients from initial resuscitation, through burn excision and grafting, and into acute rehabilitation. Third, after age of the patient and extent of burn injury (percent of total body surface area [%TBSA]), inhalation is the third-most important determinant of mortality in patients with thermal injuries. , , 8 , 9 Inhalation injury is associated with hemodynamic instability, and volume requirements may be increased by as much as 50% when cutaneous burns are accompanied by inhalation injury. 10 , 11 , 61 , 62 Finally, even after recovery from acute inhalation injury, there may be long-term adverse effects, such as pulmonary fibrosis and/or bronchiectasis. 12
The incidence of inhalation injury among burn patients is highly variable depending on the population studied, the time and duration of study, and the geographic location of study. One of the lowest incidences of inhalation injury is 1.9% found in a study performed in Israel. At the other end of the spectrum, a study in the United States found incidents of 19.6% among patients with thermal injuries. Inhalation injury has been reported in 0.3% to 43% of patients with thermal injuries. A reasonable estimate is that approximately 10% of hospitalized burn patients overall and one-fourth to one-third of burn intensive care unit (ICU) patients will have inhalation injury. Inhalation injury also affects 5000 firefighters annually.
Inhalation injury can be classified by the general etiology of the injury and the location of the damage within the respiratory tract. Inhalation injury can be caused by the direct effects of increased temperature or by the effects of inhaled toxins both locally and systemically. Additionally, combustion almost always produces carbon monoxide, and in addition to heat and toxin damage, systemic injury by carbon monoxide poisoning must always be considered as a factor.
The oropharynx, hypopharynx, and particularly the larynx are effective heat exchangers and serve to protect respiratory structures below the level of larynx from direct damage by increased temperature. Therefore direct thermal injury is generally seen only in structures above the level of the larynx and rarely seen below this level. Exceptions to this include inhalation of steam and aspiration of hot liquids. ,
In contrast, damage to the respiratory tree below the level of the larynx is almost always because of the direct and indirect effects of inhaled toxins present in smoke and products of combustion. Inhaled toxins are generally present in smoke as a mixture of gases, fumes, and mists. Fumes are particles dispersed within gases. Mists are aerosolized liquid chemicals. The chemical identity and composition of the particular toxins in smoke depend on the material being burned. Typically, there are hundreds or even thousands of such chemicals. The most dangerous of these are acids, bases, aldehydes, esters, and other reactive species.
The severity of airway and lung damage, and the clinical manifestations after inhalation injury, is dependent on a number of factors, including the type of material being burned, the toxins produced, the concentration of toxins within the smoke, and duration and degree of exposure. Regardless of the precise etiologic agents, the pathogenesis of smoke in relation to injury tends to follow a common pathway characterized by mucosal and epithelial injury and loss, loss of ciliated cells, influx of fluid and inflammatory cells, obstructive debris within the airways and alveoli, impairment of gas exchange, ventilation and perfusion mismatch, and subsequent pulmonary dysfunction. Inhalation injury also often progresses to acute respiratory distress syndrome (ARDS) and/or frequently to pneumonia.
There is no definitive tool for diagnosis of inhalation injury. Inhalation injury can be suspected by a history of closed-space injury with exposure to concentrated smoke or aspiration of hot, toxic chemicals. It can also be suspected based on physical findings, such as carbon staining in the mouth and throat and the production of carbonaceous sputum. Laboratory values can be suggestive, such as an elevated carboxyhemoglobin (COHb) level or accompanying hypoxemia and/or hypercarbia. Diagnosis typically rests on fiberoptic bronchoscopy performed soon after presentation. Computerized tomography (CT) may also have utility. These are explored in greater detail later.
Finally, because there is no definitive diagnostic modality for inhalation injury, there also are no well-defined treatment protocols that obviously improve outcome. Treatment has focused on appropriate intubation, lung-protective ventilatory management, aggressive pulmonary hygiene with a focus on preventing pulmonary complications (e.g., pneumonia, ARDS), and aggressive treatment of carbon monoxide poisoning.
Advancements in the clinical and operative management of the cutaneous wounds of patients with thermal injuries have occurred over the past several decades. These include new options for topical wound management, dermal substitutes, epithelial autografts, and keratinocyte spray. In contrast, there have been few improvements in the diagnosis and management of inhalation injury over that same time period. Inhalation injury is inherently more difficult to study and understand than cutaneous injury because much of the airways and lungs are not directly accessible for evaluation. Thus the pathophysiologic mechanisms responsible for inhalation injury are incompletely understood. Likewise, no specific therapies have been identified.
Because of its significant clinical ramifications, reliable diagnosis and effective treatment of inhalation injury must be a priority for burn healthcare professionals. Indeed, at both of the American Burn Association State of the Science meetings (2006 and 2016), one of the top priorities was diagnosis and care of inhalation injury.
Diagnosis
One of the most challenging aspects of the clinical management of inhalation injury is the diagnosis and severity classification of the process. Although there is no widespread agreement or consensus on absolute diagnostic criteria for diagnosis of inhalation injury, it is usually possible to determine the presence or absence of the process. However, determining the severity of the initial injury and attempting to predict the degree of subsequent clinical manifestations prove difficult. 107 The degree of respiratory compromise ultimately manifested by the patient is not always proportional to the apparent intensity or severity of the initial injury. 13 Additionally, the systemic effects of the burn injury itself contribute to the severity of the respiratory disease; indeed, in some cases, this effect may actually be greater than that of the respiratory injury itself. 14 A scenario frequently seen is the development of respiratory insufficiency in pediatric patients with relatively large hot liquid scald burns and lack of associated inhalation injury. In these cases, the respiratory compromise can be fully attributed to the systemic effects of the burn injury. 15
The clinical utility of diagnostic maneuvers has also been called into question because there are not specific care modalities based on the severity of inhalation injury. Treatment, as described later, is almost wholly supportive and based on patient clinical response to intervention(s). Simply stated, because the diagnosis and grading of inhalation injury does not impact care significantly, why do it? There are several important reasons to pursue accurate diagnosis and grading of inhalation injuries. The first is triage and transport. If patients with severe inhalation injuries can be correctly identified early, then they can be transported to the appropriate facility and/or unit. This could be especially important in military and combat settings. Second, as we attempt to find effective treatments for inhalation injury, it will be important to stratify them based on severity so we know whether the intervention is efficacious. Third, at both of the American Burn Association State of the Science meetings (2006 and 2016) and at the Inhalation Injury Consensus Conference (2009), a top priority was diagnosis and grading of inhalation injury.
Diagnostic modalities used in the diagnosis and severity classification of inhalation injury include the history of the injury, physical examination of the patient, laboratory determinations, radiologic techniques, and bronchoscopy, among other methods. It is important when considering the diagnosis and management of inhalation injury that it is not confused with the necessity for endotracheal intubation of a burn patient. Inhalation injury is typically one indication for endotracheal intubation. However, there are other indications for intubation of a burn patient outside of inhalation injury, including inability to protect the airway from associated traumatic injury or intoxication, loss or potential loss of the airway because of upper-airway swelling from thermal injury, hypoxemia, hypercarbia, acidosis, and the need for significant analgesia and/or sedation as a result of the burn injury. 18
Injury history pertinent to the diagnosis of inhalation injury includes mechanism of injury, exposure to the products of combustion and/or chemicals, duration of exposure, and intensity of exposure. One of the most important clues to development of inhalation injury includes a closed-space exposure to the products of combustion, such as a house fire, vehicle fire, or any other enclosed space where smoke can accumulate and concentrate and subsequently be inhaled by the patient. This is particularly important in flame injuries. The human larynx is a particularly good heat-exchange device, and it is distinctly unusual for hot ambient temperatures to be transmitted below the level of the larynx. Thus an isolated flame injury without smoke exposure is unlikely to cause a true inhalation injury. On the other hand, if the products of the flame accumulate and concentrate in a closed space and the patient inhales them, then a smoke inhalation injury is likely. There are hundreds if not thousands of chemicals within smoke, depending on the character of the substances being consumed other than fire. These reactive chemicals include acids, bases, esters, alcohols, reactive oxygen metabolites, and many other potential toxins. Indeed, smoke inhalation injury is best thought of as a chemical injury to the airways and lung parenchyma.
A history of aspiration and inhalation of hot liquids is also an important factor to consider. This can be seen with exposure to steam injuries, which can transmit hot temperatures to the larger airways and lung. It can also be seen with exposure to hotter flaming liquids, such as aspiration of burning or exploding gasoline or other hydrocarbons. This may be seen in patients working on internal combustion engines with conventional carburetors when the combusting gasoline is forcefully projected into the person’s face. Occupational and residential exposure to caustic fumes and/or liquids can also result in a chemical inhalation injury.
It is also important to remember that a large thermal injury even in the absence of an associated inhalation injury can result in systemic effects, including the manifestation of respiratory injury. This seems to be particularly true in pediatric burn patients.
Physical examination of the burn patient can reveal signs and symptoms that are suggestive of a smoking-related injury. However, none of these physical findings are conclusively diagnostic of inhalation injury. The presence of upper-body thermal injuries—particularly burns to the face, singed eyebrows, or burned nasal hair—suggests exposure to high temperatures. However, while these thermal injuries may be devastating and may result in upper-airway swelling, thus sustaining emergency airway management, their presence alone is not diagnostic of inhalation injury. Associated soot deposits on the face and in the mouth, and in the oral nasopharynx, are suggestive of exposure to smoke in the products of combustion. The presence of true carbonaceous sputum evidenced by the coughing up of carbon-stained sputum in a nonintubated patient or the suctioning of carbon-stained sputum in an intubated patient, demonstrates that the patient has indeed inhaled the products of combustion and thus is at risk for an inhalation injury.
Additional important physical findings include hoarseness, stridor, wheezing, inability to handle oral secretions or drooling, and dysphasia. These often accompany inhalation injury but can also be seen in its absence. Therefore the presence of these findings suggests more thorough investigation into the possibility of an inhalation injury, but they are not diagnostic. Likewise, the absence of any obvious physical findings does not preclude the presence of inhalation injury.
Although inhalation injury patients may appear in no or minimal respiratory distress at the time of presentation, progression of the disease process can occur with eventual loss of airway. This may require emergent intervention. Loss of airway may also occur in burn patients without inhalation injury in the same manner. Indeed, pediatric intraoral scald burns have been compared with severe epiglottitis with regard to airway manifestations. 17
Routine laboratory determinations are generally not particularly useful in the diagnosis of inhalation injury, but with two exceptions. An elevated cyanide level is strongly suggestive of an inhalation injury or a caustic exposure. However, cyanide is not produced by all fires, and cyanide-level determinations often require 24 hours or longer and therefore are not particularly useful in the acute diagnosis of inhalation injury. In contrast, the single-most important laboratory value that one can determine is the COHb level, preferably obtained as close in temporal proximity to the time of injury or exposure as possible. COHb is usually given as a percentage of hemoglobin that is bound to carbon monoxide. Normal COHb levels are zero, although baseline levels can be elevated in patients who smoke tobacco and/or in patients who reside in industrial geographic regions.
Various studies on determination of biochemical markers and inflammatory mediator levels have yielded some interesting results and provided areas for future study. However, none of these studies has provided definitive tools to diagnose or exclude inhalation injury.
Radiologic diagnostic tools include chest radiograph and CT. Chest radiographs are generally considered an insensitive and unreliable diagnostic tool for the diagnosis of ventilation injury. Typically, the initial chest radiograph is normal. 16 Most well-conducted studies support this view. However, some studies have demonstrated positive findings on initial chest radiographs in a significant proportion of patients. Chest radiograph is an important diagnostic tool to determine baseline and/or preexisting chest or pulmonary abnormalities. It is important to realize that although early chest radiography is not an inaccurate diagnostic modality, a normal chest x-ray does not exclude the diagnosis of inhalation injury. 16 , 19
CT may have some utility as an early diagnostic tool in determining the presence and possibly the severity of inhalation injury. CT can more accurately portray anatomic and pathologic abnormalities associated with inhalation injury. These include atelectasis, infiltrates, consolidation, fluid collections, and other changes. Yamamura et al. studied CT-determined bronchial wall thickness (BWT) in patients with smoke inhalation. 35 BWT was predictive of ventilator days, ICU length of stay, and the development of pneumonia. Oh et al. found a radiologist’s lung CT scan score added to the prognostic value of bronchoscopy in predicting a composite outcome of death, acute lung injury/ARDS, and pneumonia in patients with smoke inhalation. Kim and Kim demonstrated that abnormal findings on CT scan were associated with longer hospital stays, time to admission to ICU, intubation requirement, and development of pneumonia.
Radionuclide studies, such as xenon-133 scans, have limited utility in the diagnosis of inhalation injury. Intravenously administered xenon-133 is excreted by the lungs and eliminated by exhalation. Delayed clearance of and/or inhomogeneous lung distribution of the radionuclide are indicators of inhalation injury. Interpretation of radionuclide scans is complicated by preexisting lung disease, and they are rarely performed currently in critically ill patients with thermal injuries. 33 , 34
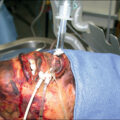
In most burn centers currently, flexible bronchoscopy ( Fig. 16.1 ) is the gold standard for diagnosing the presence or absence of inhalation injury. 20–22 Diagnostic bronchoscopy is typically performed at the time of admission or soon thereafter, and almost always within 24 hours of injury or exposure if possible. The indication for bronchoscopy can be based on the history, physical examination, and laboratory findings (see earlier). Bronchoscopy can confirm the presence of smoke exposure by finding soot and carbon staining below the level of the larynx in the trachea and in the mainstem, segmental, and subsegmental bronchi. 24 Bronchoscopy can also confirm the presence of other pathologic findings that may indicate airway injury, such as increased secretions, edema, and tracheobronchial mucosal injury, such as erythema, erosions, or ulcerations. 23 Bronchoscopy is particularly useful to identify smoke inhalation because of carbon staining. However, it may be less reliable in identifying airway and lung injury caused by other toxins or caustic injury because of the lack of staining and the possibility that the pathology of the airway and the mucosa has not manifested at the time of bronchoscopy.
Bronchoscopic view of the trachea from a patient with smoke inhalation injury.
Note generalized inflammation and erythema. Edema is manifested as indistinct tracheal rings and blunting of the carina. There are patchy areas of denuded mucosa, and a fibrinous exudate is forming at the carina.
The major limitation with flexible bronchoscopy as a diagnostic tool is the lack of an evidence-based scoring system that correlates bronchoscopic findings with clinical outcomes, such as the degree of lung injury and respiratory insufficiency. The most frequently used and referenced bronchoscopic scoring system is described by Endorf and Gamelli. 27 A retrospective review of this scoring paradigm in several independent studies by Spano et al. demonstrated that greater pathologic changes on bronchoscopy were generally associated with poorer clinical patient outcomes. 26 However, this correlation did not reach statistical significance, and the authors stated that bronchoscopy did not provide reliably predictive diagnostic information. A large retrospective study utilizing the American Burn Association’s Burn Repository database found that bronchoscopy was useful in the diagnosis of inhalation injury in burn patients.
Multiple bronchoscopic finding–based scoring systems have been developed to grade the severity of inhalation injury. The most widely recognized score is that developed by Endorf and Gemelli based on abbreviated injury score (AIS) criteria, and typically referred to as the AIS. 27 This score ranked bronchoscopic criteria from grade 0 (no injury) through grade 4 (massive injury) based on carbonaceous deposits, mucosal injury, and bronchial obstruction. Their initial study concluded that mortality was correlated with increasing grade of severity of bronchoscopic findings; however, the study did not correlate severity grade with fluid requirements. The data suggested that Pa o 2 /Fi o 2 ratios were a more accurate predictor of fluid requirements than bronchoscopic grade. Additional studies utilizing this grading system demonstrated equivocal results in predicting microbiologic and clinical outcomes. 28 , 29
An additional bronchoscopic scoring system, the Bronchoscopic Mucosal Score, was described by Hassan et al. 25 This system ranks findings from grade 0 (normal mucosal appearance) to grade 3 (necrotic mucosa) and assesses only mucosal characteristics without considering other bronchoscopic or patient factors. This retrospective study demonstrated that the scoring system was predictive of mortality. However, the authors stated that the Pa o 2 /Fi o 2 ratio was more predictive of mortality.
An early study by Brown et al. attempted to construct a composite predictive score using bronchoscopic findings along with Pa o 2 /Fi o 2 ratio, peak inspiratory pressure (PIP), and chest radiograph. Early mortality was associated with decreased Pa o 2 /Fi o 2 ratio, while later mortality was associated with increased PIP and abnormal chest radiograph. Bronchoscopic findings were not particularly useful in this paradigm.
In a similar study, Lin et al. developed a composite score from the AIS bronchoscopic score, combined with patient demographic and clinical data to predict the development of pneumonia in patients with inhalation injury. Higher bronchoscopic grade was associated with development of pneumonia in this population.
Overall, bronchoscopic scoring systems have been at best moderately and at worst poorly predictive of clinical outcomes in burn patients with inhalation injury. Currently, it appears that the best we can do is dichotomous grading separating mild inhalation injury from severe inhalation injury. Clearly, more rigorous study is needed.
It has also been suggested that the best diagnostic tool for determining the presence and severity of inhalation injury may simply be the patient’s response to treatment. For instance, the need for endotracheal intubation and mechanical ventilation may be an indicator of a moderate to severe inhalation injury. Confounding factors include other causes for intubation and ventilation (e.g., upper-airway swelling, intoxication). Along the same lines, patient response to oxygen administration may indicate inhalation injury. Decreased Pa o 2 /Fi o 2 ratios suggest parenchymal injury and may be a surrogate for inhalation injury. Finally, there is a fair amount of data in the burn literature that inhalation injury causes a corresponding increase in resuscitation fluid requirements. An increase in fluid administration could also be an indicator of inhalation injury. However, there are numerous other causes for increased fluid requirements (e.g., a degree of full-thickness injury, associated traumatic injury, medical comorbidities). Cancio et al. have suggested that the increased fluid requirements attributed to inhalation injury may actually be caused by mechanical ventilation and that the need for ventilation was a more important indicator of inhalation injury than increased fluid administration. 30 Others have suggested similar mechanisms. 31 , 32
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree