![]() Visit Elsevier eBooks+
(
eBooks.Health.Elsevier.com
) for complete set of videos.
Visit Elsevier eBooks+
(
eBooks.Health.Elsevier.com
) for complete set of videos.
Introduction
In recent decades, improvements in survival and functional recovery from major burns continue through aggressive fluid resuscitation, early excision and grafting of burns, development of more effective antimicrobials, advances in nutritional support, and rehabilitation. , Whereas in 1950 the “lethal dose 50%” for burns in a 21-year-old patient was 40% total body surface area (TBSA), today it is over 90% TBSA. These advances have come with continuous improvements often by small advances.
Major burn injury results in pathophysiologic changes in virtually all organ systems. Box 12.1 lists and Figs. 12.1 and 12.2 illustrate some of the challenges presented by the acutely burned patient during the perioperative period. This chapter will concentrate on the care of acute burn patients. The acute phase of burn injury is defined as the period from injury until the wounds have been excised, grafted, and healed.
Box 12.1
Pathophysiologic Changes Associated with Acute Burns
-
Compromised airway
-
Pulmonary insufficiency
-
Altered mental status
-
Hypovolemia
-
Decreased colloid osmotic pressure
-
Decreased myocardial contractility
-
Dysrhythmia
-
Extensive edema
-
Impaired temperature regulation
-
Altered drug responses
-
Renal insufficiency
-
Immunosuppression
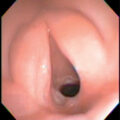
This image illustrates the many technical challenges regarding airway management, vascular access, application of monitors, temperature regulation, associated with the anesthetic management of patients with major burns.
Occasionally, patients requiring burn excision present with special needs, as with this 3-day-old patient.
Cardiovascular, hepatic, and renal physiologic systems are immature, and vascular access adequate to replace extensive blood loss can be technically difficult.
Modern burn care depends on coordination of a multidisciplinary team. Rational and effective anesthetic management of acute burn patients requires an understanding of this multidisciplinary approach so that perioperative care is compatible with the hospital course and overall treatment goals for the patient. Following extensive burns, the systemic effects of inflammatory mediators on metabolism and cardiopulmonary function reduce physiologic reserve, and the patient’s tolerance to the stress of surgery deteriorates with time. Assuming adequate resuscitation, extensive surgery is best tolerated soon after injury, when the patient is most fit. However, it must be recognized that the initial resuscitation of patients with extensive burns results in large fluid shifts and may be associated with hemodynamic instability and respiratory insufficiency. Reynolds et al. reported that more than half of deaths after burn injuries occur due to failed resuscitation. A careful preoperative evaluation includes judging the quality of the resuscitation.
Reviews of anesthetic management for burn surgery have been written during the past decade. , This chapter aims to describe evidence for guidelines for anesthesiologists involved in the initial resuscitation as well as perioperative anesthetic management of patients with major burns.
Initial care
Anesthesiologists’ involvement in the care of burn patients should not be limited to perioperative management, especially in hospitals lacking a burn unit. Burn patients are often transferred from the scene of the injury not to a burn center but to the emergency department of a local hospital. Since the clinical skills and experience of anesthesiologists match the urgent needs of patients with acute burns, they should participate in the initial care, resuscitation, and preparation for transfer to a burn center.
Preoperative evaluation
Major burns can be viewed as a dynamic wound evolving from the initial event to healing of skin and a slow resolution of systemic dysfunction. The dramatic changes that occur in all organ systems following burn injury directly affect anesthetic management. These changes provide multiple challenges to the anesthetist (see Box 12.1 ).
As a result, besides the standard preoperative exam there are unique features of burn pathophysiology and surgery that require additional or special attention because they are associated with increased technical challenge and risk. The severely burned patient presents with numerous preoperative concerns ( Box 12.2 ). The preoperative evaluation must be performed within the context of the hospital course and planned operative procedure, which will depend on the location, extent, and depth of burn wounds, time after injury, presence of infection, and existence of suitable donor sites for autografting.
Box 12.2
Major Preoperative Concerns in Acutely Burned Patients
-
Age of patient
-
Extent of burns (% total body surface area burned)
-
Burn depth (superficial or full thickness)
-
Distribution of burns
-
Mechanism of injury (flame, scald, chemical, electrical)
-
Airway patency
-
Elapsed time from injury
-
Adequacy of resuscitation
-
Associated injuries
-
Coexisting diseases
-
Surgical plan
Respiration
Airway issues and respiratory insufficiency are common in burn patients. During the hospital course, changes that distort anatomy may resolve as edema fluid is reabsorbed or may worsen as scar formation limits mobility. Facial burns may impede direct laryngoscopy, and mask ventilation may be difficult as mandibular mobility becomes limited by scars.
The level of respiratory support in the intensive care unit (ICU) may range from supplemental oxygen to intubation and mechanical ventilation. Acute lung injury can occur from inhalation injury, systemic inflammation from burns, sepsis, a difficult resuscitation, or ventilator-induced injury. With very high levels of positive end-expiratory pressure (PEEP) or peak inspiratory pressure, it should be determined if the anesthesia ventilator is adequate or if an ICU ventilator will be needed.
Circulation
During the first few days after a large burn injury, there is a biphasic change in cardiovascular function. Initially, with loss of fluid from the vascular space, hypovolemia develops quickly without aggressive replacement. This is associated with decreased cardiac output and increased systemic resistance. Over the next 2 to 3 days, if resuscitation is successful, this pattern is reversed. A hyperdynamic pattern develops with significantly elevated cardiac output and decreased systemic vascular resistance.
Accurate predictions of blood loss are crucial in planning preoperative management of burn patients. With extensive wound excision or debridement, large amounts of blood can be lost rapidly. Adequate preparation in terms of monitors, vascular access, and availability of blood products is essential. Desai et al. reported that surgical blood loss depends on the area to be excised (cm 2 ), time since injury, surgical plan (tangential vs. fascial excision) ( Fig. 12.3 ), and presence of infection.
(A) An important determinant of bleeding is surgical technique. Here the burn is excised tangentially with a Watson knife down to viable tissue, which is recognized by bleeding. (B) Bleeding during burn excision is less when the burn is excised down to the fascial layer, as in this image.
Metabolic changes associated with burn injury
Increased metabolic rate is the hallmark of the metabolic alterations that take place after thermal injury. This results in increased O 2 consumption along with an increased CO 2 production that demands a higher respiratory effort. Anesthetic care must accommodate these changes.
The hypermetabolic pattern also increases caloric needs, and reduced nutritional support can exacerbate catabolism and impair immune function and wound healing. With standard guidelines for general anesthesia, pre- and postoperative fasting can interrupt continuous feeding for 10 hours for each procedure. Varon et al. compared patients fed intraoperatively through postpyloric feeding tubes with patients fasted for surgery. There were no adverse events, and fed patients met nutritional goals sooner. Imeokparia et al. studied 31 burn patients. Patients with interrupted feeding fell 125% below their metabolic needs, whereas patients with continuous feeding surpassed metabolic needs. Larger studies are necessary to establish the safety of intraoperative feeding, but many practitioners consider this safe in the presence of a cuffed endotracheal tube.
Critical care of burn patients often involves parenteral nutritional support and may include insulin infusions. It is important to recognize these interventions during the preoperative evaluation of the burn patient in the ICU.
Renal function
Folkestad et al. conducted a review and meta-analysis of reports through December 2018. Acute kidney injury occurred in 38% of burn patients admitted to an ICU, and 12% of all patients received renal replacement therapy. The presence of renal failure complicates intraoperative management. It seriously reduces the margin of error for fluid replacement of blood loss. Electrolyte balance, especially potassium, should be watched closely, and extra caution with dosage and rate of administration of nephrotoxic drugs such as antibiotics is needed.
Pharmacology
Major burn injury exceeding 25% to 30% TBSA induces many pathophysiologic responses that affect pharmacokinetics and pharmacodynamics of drugs used in the perioperative period. During the acute phase, because of hypovolemia and profound vasoconstriction in gut and cutaneous areas, uptake by these routes may be impaired. During the hypermetabolic phase, there is enhanced clearance of drugs by the liver and kidneys because of enzyme induction and increased blood flow. This is a concern for maintaining therapeutic levels of some antibiotics, muscle relaxants, and opioids, which have blood flow–dependent elimination. Massive edema and loss of drugs through burn wounds increase the volume of distribution of other drugs. As a general rule, burn injuries require larger than normal doses of almost all intravenous (IV) medications, including antibiotics, neuromuscular blocking drugs (NMBDs), opioids, and benzodiazepines. The enhanced elimination kinetics play a contributory role in the increased dose requirements; the predominant cause for the higher dose requirements, however, is the pharmacodynamic changes related to cellular responses induced due to the injury and the drugs per se.
Clearance of drugs highly extracted by the liver, such as propofol and fentanyl, may be significantly increased due to increased hepatic blood flow. Upregulation of nicotinic receptors at the myoneural junction contributes to resistance to nondepolarizing relaxants but can cause an exaggerated hyperkalemic response to succinylcholine sufficient to cause cardiac arrest. As a result, succinylcholine should be avoided after 48 hours following major burns. The duration of this risk is unclear, but resistance to nondepolarizing relaxants has been observed more than 1 year after healing of burns. An increase of the dose of rocuronium for rapid sequence induction from 1.2 to 1.5 mg/kg has been recommended.
Thermoregulation
Maintenance of proper body temperature is an important factor in the care of severely burned patients. Skin is the major effector organ for thermoregulation and its destruction by burns makes patients vulnerable to hypothermia. This risk is greater in anesthetized burn patients because anesthetics ablate thermoregulatory mechanisms. Hypothermia exacerbates the hypermetabolic and catabolic effects of large burns and is poorly tolerated by burn patients.
Patient transport
The safe transport of a critically ill burn patient to and from the operating room requires careful planning and preparation. A methodical approach will help to ensure patient safety and the seamless maintenance of respiratory, hemodynamic, and general support. Hemodynamic status should be optimized prior to patient transport; pharmacologic support may be required. The American Society of Anesthesiologists standards mandate evaluation, treatment, monitoring, and equipment appropriate to the patient’s medical condition for any transport. Depending on the patient’s condition, simple observation may be appropriate. Patients requiring supplemental oxygen should be monitored by pulse oximetry. Hemodynamic monitoring is guided by the patient’s hemodynamic status. Sufficient battery power must be available for uninterrupted monitor and infusion pump function during transport.
Airway supplies should be readily available, including a full oxygen cylinder, a self-inflating Ambu bag with mask, and intubation equipment. The patient’s airway and ventilation, as well as overall condition, must be continually observed by the anesthesia care team. Drugs for resuscitation should accompany the patient on any transport. Because hypothermia is poorly tolerated by patients with an acute burn injury, it is imperative that patients be kept warm.
Intraoperative care
Airway management
If injuries do not preclude conventional airway management (i.e., mask fit, jaw lift and mouth opening), then standard induction and intubation procedures are appropriate. Hu et al. reported that gastric emptying was not delayed in patients with severe burns, so rapid sequence induction is not necessary; however, development of sepsis can slow gastric emptying.
Burns of the face and neck can distort anatomy, making direct laryngoscopy and mask ventilation difficult. Under these circumstances, fiberoptic intubation while maintaining spontaneous ventilation is a safe and reliable technique. Fiberoptic intubation can be performed in adults with sedation and topical anesthesia, but pediatric patients require deeper sedation. Ketamine is uniquely suited for fiberoptic intubation of either adults or children. It provides profound analgesia but does not depress respiratory drive or airway reflexes.
Securing an endotracheal tube in patients with facial burns is difficult. A nasal endotracheal tube can be secured with confidence using a septal bridal ( Fig. 12.4 ). Oral tubes can be secured with a red rubber catheter passed through the nose and brought out the mouth to form a loop around the hard palate. The endotracheal tube can be tied to the catheter with umbilical tape.
Endotracheal tube, nasogastric tube, and duodenal feeding tube are all secured in place after being tied to a septal bridal.
When fastened in this manner, the endotracheal tube is very secure, and tape or ties do not irritate burn wounds of the face or neck.
A laryngeal mask has also been used successfully during pediatric burn surgery. McCall et al. reported on 141 general anesthetics for burn excision in children. Nineteen (14.5%) of the procedures were complicated by events such as unseating and mild laryngospasm that required intervention. Two required intubation without sequelae, while all others resolved with therapy. Laryngeal mask airway may be preferred in patients with laryngeal injury because a translaryngeal endotracheal tube may exacerbate an injury.
Monitors
In addition to perioperative pathophysiology associated with major burns, monitoring must be adequate to assess rapid changes in blood pressure and tissue perfusion associated with rapid blood loss and inflammatory mediators released with manipulation of inflamed tissues. Continuous and vigilant measurement of body temperature is imperative. Transmission pulse oximetry may be difficult when sites are either burned or within the surgical field. Nasal clip probes and reflectance probes are now available.
When vasoactive infusions are needed or blood loss is expected to be extensive, the blood pressure may change more rapidly than appropriate for noninvasive measurements. In this case, an arterial catheter can provide continuous measures along with waveform that can give additional information. Beat-to-beat monitoring allows measurement of systolic pressure variation, which is sensitive to variation of stroke volume and has been used to predict response to fluid volume administration. The use of these dynamic measures of fluid responsiveness and their limitations has been reviewed by Monnet ; however, no single physiologic variable can be consistently relied on to correct all deficiencies of tissue perfusion. Wound manipulation can release inflammatory mediators and bacterial products that alter myocardial compliance and contractility as well as vascular tone. Volume replacement alone may not correct hemodynamic deficiencies. It is necessary to utilize all information available, including hemodynamic variables, urine output, blood gas, electrolytes, and other metabolic measures, to manage these complex clinical scenarios.
When hemorrhage is brisk, the decision to administer volume is not difficult. In other cases, during burn wound manipulation, hypotension and other evidence of poor perfusion can occur in the apparent absence of significant blood loss. Inappropriate fluid administration can cause hemodilution, increased cardiac filling pressure, and fluid overload. Measurement of central venous pressure (CVP) can indicate if there is room in the intravascular space for volume administration, and dynamic measures of fluid responsiveness can identify patients who are more likely to respond to fluid loading with an increase in cardiac output and tissue perfusion. Reliability of dynamic indices of fluid responsiveness requires several conditions, including regular heart rhythm, muscle relaxation and positive pressure ventilation, and limits of tidal volume and heart rate. Positive pressure ventilation increases fluid requirements.
No single physiologic variable can be relied on to correct all deficiencies in perfusion during burn wound debridement. During challenging cases with rapid bleeding, volume replacement alone may not correct hemodynamic deficiencies. It is necessary to monitor blood gases, electrolyte changes, and urine output, as well as arterial and central venous pressures. Inadequate tissue perfusion may manifest as metabolic acidosis despite apparently adequate arterial and central venous blood pressures.
Blood samples from a central vein are not truly mixed venous, but trends in central venous oxygen tension can help identify inadequate tissue perfusion or utilization. A central venous catheter (CVC) sutured into place also provides very secure IV access and is the preferred route for administration of vasoactive infusions. A pulmonary artery catheter is usually not required for burn surgery. In some cases, however, the ability to monitor ventricular function and oxygen supply/demand relationships more closely may be helpful in the presence of preexisting disease or when large doses of inotropes or high PEEP is required.
Urine output is the most useful perioperative monitor of renal function. Urine output of 0.5 to 1 mL/kg/hour is often recommended as an end point for fluid management in acute burn patients. Adequate urine output is one measure of both renal and global perfusion. When intraoperative transfusion is planned, examination of the urine may be the only reliable indicator of a transfusion reaction because signs and symptoms other than hematuria are masked by general anesthesia or hemodynamic changes associated with burn surgery. Myoglobinuria may also occur after burn injury; in this case, a Foley catheter is necessary to monitor response to therapy. Diuretic therapy for myoglobinuria or any other indication will negate the usefulness of urine output as an index of global perfusion.
Temperature control
As mentioned, maintenance of proper body temperature is an important factor in the care of severely burned patients. Actions such as maintaining higher ambient air temperature, covering extremities and head, applying warm blankets, utilizing radiant heaters and forced air warming devices, warming fluids and blood, and warming gases are usually effective in maintaining core temperature if applied aggressively. Hypothermia revealed in the preoperative evaluation may be due to inadequate resuscitation or metabolic instability. Either situation may predispose burn patients to intolerance of anesthetic drugs or the stress of surgery.
Vascular access
Care of patients with major burn injury requires secure vascular access for resuscitation, blood sampling, hemodynamic monitoring, and IV medication. In patients with large burns, a CVC can serve several purposes: A CVC sutured in place can be maintained longer than peripheral sites, and a multiport CVC can allow simultaneous infusion of incompatible drugs.
Catheter selection must take into consideration multiple clinical needs: blood sampling, monitoring, rapid infusion of fluid or blood products, and administration of medications. During wound excision, a large lumen may be required to administer volume rapidly. As mentioned earlier, although CVP has been found to correlate poorly with response to fluid, when hypotension or anemia occur, the CVP can indicate if there is sufficient room in the vascular space for a fluid challenge or to raise the hematocrit quickly and avoid overload. ICU management may require a different catheter (e.g., multilumen) than the large-bore single lumen appropriate during surgery.
In recent years, peripherally inserted central catheters (PICCs) have been used in burn centers. Although the PICC avoids some risks of CVC, such as pneumothorax, it carries its own unique set of risks. The incidence of catheter-related infection may be similar to CVCs. Despite the use of antithrombotic prophylaxis, upper-extremity deep-vein thrombosis that can lead to fatal embolic events is associated with PICC placement. Although a PICC may be adequate for ICU needs in terms of maintenance fluids and IV medications, it is inadequate for administering fluids and blood products rapidly enough to keep up with surgical blood loss.
Selection of anesthetic agents
Many anesthetics have been used effectively for induction and maintenance of anesthesia in burn patients. IV agents can be used for both induction and maintenance, and the specific agent used will depend primarily on the patient’s hemodynamic and pulmonary status as well as on the potential difficulty of securing the patient’s airway.
Propofol is an IV induction agent commonly used in burn patients. Dose requirements for propofol will vary over time after the initial burn injury. Initially, with hypovolemia and reduced cardiac output, a lower dose may be required, but as the hypermetabolic and hyperdynamic circulatory pattern develops, the volume of distribution (V d ) and clearance rate for propofol are increased enough to increase dose requirements. Care should be taken in the selection of propofol for induction of anesthesia in patients with face and neck burns. Propofol relaxes pharyngeal tissues, causing narrowing or closure of the pharyngeal airway. Normally, this can be remedied by mandibular advancement, but as healing and scar formation of the neck and face take place, mandibular mobility may be lost, making mask ventilation and direct laryngoscopy difficult or impossible.
Ketamine has many advantages for use in burn patients. Except in patients who are catecholamine depleted, ketamine generally preserves hemodynamic stability. In addition, ketamine preserves hypoxic and hypercapnic ventilator responses and reduces airway resistance. Ketamine increases sympathetic tone and supports circulation in contrast to all volatile anesthetics that uniformly result in vasodilation. More recently, Cancio et al. reported safe and successful maintenance of total IV anesthesia with ketamine for major burn surgery for more than 400 critically ill patients requiring high-frequency percussive ventilation, which precluded the use of inhaled agents.
There are reports of safe and effective use of ketamine without an endotracheal tube for patients undergoing burn excision and grafting. While the use of ketamine for major burn excision without a secure airway has not gained general acceptance, these reports are strong evidence of the ability of ketamine to support airway patency, respiration, and circulation during painful procedures such as wound care.
Ketamine provides excellent conditions for securing the airway by fiberoptic bronchoscopy. When using this technique, the addition of potent volatile agents should be avoided until the airway is secured because these anesthetics may cause airway obstruction due to relaxation of pharyngeal tissues.
Within certain limits, regional anesthesia techniques have also been used with success in burn surgery. Spinal or epidural anesthesia is relatively contraindicated for cases involving extensive bleeding because of impaired sympathetic nervous system function. Regional nerve blocks are more suited for smaller burns or extremities where the needle placement does not involve the burn. Donor sites for harvest of split-thickness skin grafts are especially painful, and regional blocks have been used successfully to provide postoperative analgesia. , Scalp blocks have been reported to reduce nausea associated with reconstructive scalp procedures.
Fluid management
Fluid administration should be guided not only by intraoperative events but also by previous hospital course and ICU treatment goals. If procedures are performed during the first 24 hours after injury, perioperative fluid management may involve the initial resuscitation, and fluid needs will exceed replacement of shed blood. Even after this period, insensible fluid requirements are increased by large open surfaces from excised wounds, hypermetabolic state, and elevated body temperature. Also, the initial resuscitation results in extensive edema. Excessive crystalloid during the intraoperative period can increase the risk of complications of overload, such as compartment syndromes. Later ICU therapy may include vigorous diuresis to reduce edema. In this case, it is not helpful when the patient receives several liters of fluid in the operating room. Intraoperative fluid management must also consider clysis fluids the surgeons may inject to facilitate donor skin harvest. Although it is important to avoid overhydration, vigorous diuresis in the ICU may result in a patient who presents to the operating room intravascularly hypovolemic despite generalized peripheral edema.
It is impossible to accurately estimate the amount of blood shed during the procedure. Shed blood is concealed beneath the patient, in drapes, in sponges, or may be washed down a drain on the operating table. As with the initial resuscitation, there is no one physiologic end point to titrate volume replacement. CVP is not a reliable predictor of response to volume, and hematocrit and changes in urine output lag behind rapid reductions in blood volume. Metabolic acidosis indicates a problem with oxygen delivery or utilization but does not identify the specific problem. All these variables should be interpreted together. The CVP can be useful in determining if a volume challenge will be tolerated by the patient. If the CVP is elevated, then volume administration may cause overload. Hemodynamic instability with hypotension, elevated CVP, and poor preload reserve (per dynamic indices, such as pulse pressure and stroke volume variation) is an indication for echocardiography. ,
In a comprehensive review, the international Fluid Optimization Group recommended the use of colloid solutions as an approach to limiting administered fluid volume, which may contribute to a better outcome. Complex procedures are best managed with a combination of balanced crystalloid and colloid solutions.
Blood transfusion
Extensive blood loss is common during excision and grafting of burns. Desai et al. reported that the amount of blood loss during burn excision is determined by the age of the burn, percentage of TBSA involved, and whether infection of the burns is present. In general, more blood loss was observed as the time from the initial injury increased and if the burns were infected. Burn-induced changes in coagulation, fibrinolysis, and inflammation can be significant; sepsis may exaggerate these changes, and guidance may be required for intraoperative blood component transfusion.
Controversy exists regarding transfusion triggers and targets. There is no general consensus on the administration of blood products during burn surgery. Triggers should be individualized based on the patient’s physiologic state and preexisting disease. Assessment of blood transfusion needs is best determined by evaluating the clinical status of the patient; specifically, that includes assessment of ongoing blood losses, current hemoglobin level, vital signs, and urine output. Metabolic evidence of inadequate oxygen delivery, such as acidemia, and decreasing mixed venous oxygen tension provide important information regarding oxygen balance. Overall, the American Society of Anesthesiologists guidelines indicate that blood transfusion is rarely required at a hemoglobin of 10 g/dL or above and is almost always indicated at a hemoglobin of less than 6 g/dL. A multicenter trial showed a profound reduction in blood loss when a comprehensive conservative strategy was employed during burn excision and grafting.
It should be recognized that the hypermetabolic condition associated with major burns results in a much higher oxygen consumption, indicating necessarily higher oxygen delivery. During excision of large burns, patients may require one or more blood volumes of transfused blood to replace losses. Massive blood transfusion can be associated with a variety of complications, and the use of blood products is associated with significant financial costs. A number of interventions to reduce blood loss have been employed, including extremity tourniquets, topical or subcutaneous vasoconstrictors, and topical thrombin. , Antifibrinolytic agents (tranexamic acid, aminocaproic acid) have been used extensively in burn excision surgeries and may reduce perioperative transfusion needs. ,
During brisk bleeding, it may become necessary to transfuse before laboratory confirmation of criteria. In this case, clinical judgment is based on estimates of ongoing blood loss, physiologic variables, and previous laboratory values.
Point-of-care viscoelastic testing allows for rapid assessment and treatment of coagulopathy and may reduce blood product transfusions. These systems include thromboelastography, rotational thromboelastometry, and more recently developed monitors utilizing sonorheometry. ,
Perioperative pain management
Amelioration of burn injury pain in the perioperative period continues to pose major challenges to caregivers. Both basal and procedure-related pain (due to dressing changes, excision and grafting, physical therapy, etc.) need amelioration. In addition, psychosocial factors and anticipatory anxiety can aggravate the pain. It is paramount that effective communication and explanations occur, which can mitigate opioid and anxiolytic requirements. Despite opioid administration for pain control in burn patients over 30 years, no report exists of opioid addition in children after burn injury, and a low addiction rate in adults. Because of tolerance, particularly in intubated patients, it is not unusual for children to receive 1 mg/kg/hour of IV morphine in addition to other drugs. Opioid requirements rapidly decrease once they are extubated and wounds are closed; they can be started on oral morphine or methadone.
Rodent studies indicate burn injury leads to a hyperalgesic state with both reduced effectiveness of morphine due to downregulation of spinal μ-opioid receptors and increases in N-methyl- d -aspartate (NMDA) receptors. The increases in NMDA receptors induced by burns provide the rationale for the widespread use of ketamine to treat pain in these children. Opioids per se can cause a hyperalgesic state earlier than normal in these burn patients. Opioid tolerance and opioid-induced hyperalgesia can be exaggerated with long-term coadministration of midazolam. Alternative drugs that can be coadministered to mitigate opioid tolerance include dexmedetomidine and gabapentin. Dexmedetomidine has been used successfully for sedation, although larger doses may be needed. , When dexmedetomidine was compared with midazolam as an adjunct to ketamine in sedation and analgesia for burn dressing changes, the authors determined that both were effective adjuncts but that the dexmedetomidine-ketamine group had better sedation with less hemodynamic instability.
Dressing changes sometimes present one of the greatest analgesic challenges. , These are very painful, cause a rapid increase above baseline pain, and are associated by the child with anticipation of impending pain. Strategies to manage this pain include additional opioids and benzodiazepines, ketamine, , intranasal fentanyl, remifentanil, immersive virtual reality, , and music therapy. Management of the child’s pain depends on physiologic and pharmacologic factors, as well as the psychological state of the child.
When poorly controlled, pain and anxiety have adverse psychological and physiologic effects. Posttraumatic stress disorder occurs in up to 30% of those with serious burns and may be related to both the accident and the treatment, particularly in the setting of inadequate control of pain and anxiety. Substantial escalation of drug doses, particularly in children with large injuries, is commonly required; doses should be titrated to the child’s needs. When the patient is being weaned toward extubation, background medications should be tapered to yield a sensorium consistent with airway protection; many can be safely extubated while the children are still receiving opioid and benzodiazepine infusions; following this, they are transitioned to oral medications, usually methadone. Finally, it is essential to emphasize that the most effective of all analgesics and anxiolytics is prompt, definitive wound closure.
Evidence indicates that burn injury, with its complications and hormonal responses, may affect the number of receptors in tissues. , , Therefore reports of aberrant responses to drugs acting on adrenergic and cholinergic receptors are not surprising. Cardiovascular responses to catecholamines may be attenuated because of a reduced affinity of β-adrenergic receptors for ligands and diminished second messenger responses, thus the need for greater than standard doses to achieve the desired clinical response. Thermal injuries greater than 30% TBSA cause an upregulation of acetylcholine receptors and consequent resistance to NMBDs. Other aberrant responses include altered sensitivity to succinylcholine and increased pulmonary vascular sensitivity to dopamine. , , , , Dexmedetomidine infusion may cause hypotension particularly in the hypovolemic state because of the known hypotensive effects of the α 2 A -adrenoceptor agonists; particular attention to limit the dose and to ensure euvolemia may minimize the hemodynamic consequences. A similar tolerance has been observed with opioids due to drug and injury-induced changes in neuronal and nonneuronal microglia cells. , The persistence of such pharmacodynamic changes make the clinical responses to opioids somewhat unpredictable and point out the need to titrate drugs according to patient responses. Therefore clinical effects should always be closely monitored. Anesthesiologists can play a key role in the treatment of thermal injury pain because of their better understanding of pharmacokinetics and pharmacodynamics.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree