Abstract
This chapter examines the role of thigh lift and reduction in remediating medial thigh deformities, which are often caused by massive weight loss. The authors lay out the indications for thigh rejuvenation and then provide an in-depth description of how patients should be prepared for surgery, followed by the actual surgical procedure. Postoperative care guidelines are included, and a frank assessment of outcomes and possible complications concludes the chapter.
47 Thigh Lift and Reduction
47.1 Goals and Objectives
To educate the reader on the keys to evaluating a patient presenting with medial thigh deformity.
To describe where thigh lift and reduction fits into the sequence of body contouring.
To review current concepts in the surgical management of thigh contour deformities, including when to utilize liposuction as well as when to use the vertical, horizontal, or combined approach to excisional lift.
To outline common techniques for excisional thigh lift, including fascial anchoring and degree of excision.
To review current evidence on outcomes, complications, and patient satisfaction after thigh-contouring procedures.
47.2 Patient Presentation
The medial thigh is a common area of concern for patients when seeking plastic surgical consultation for body contouring, particularly after massive weight loss (MWL). Historically, the number of patients undergoing thigh lift has been low secondary to the scar burden and risk for complications. However, the technique has gained popularity in patients who have undergone MWL, either secondary to lifestyle modification or bariatric surgery. According to the procedural statistical report of the American Society of Aesthetic Plastic Surgery (ASAPS), over 17,000 thigh lift and reduction procedures were performed in the United States in 2014, marking a 500% increase from 1997. 1 These patients are often willing to trade the resulting scar burden for improved contour in this area.
The vast majority of MWL patients presenting with medial thigh deformity have concurrent excess truncal tissue. This should be addressed first with either an abdominoplasty procedure or lower body lift. Oftentimes, truncal contouring alone can correct mild upper third thigh laxity. However, if the medial thigh deformity persists, many advise waiting at least 3 months after abdominal contouring and it is necessary to address this in a separate procedure. 2
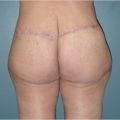
When evaluating a patient for thigh rejuvenation, it is useful to divide the medial thigh into thirds to accurately determine the location of excess tissue. By doing so, patients can be divided into four distinct groups: (1) patients who have upper third excess, (2) patients who have upper and middle third excess, (3) patients who have excess tissue throughout the entire medial thigh, (4) patients who have excess which extends past the knee (Fig. 47‑1). The distinction among these groups defines both the technique for skin excision, horizontal or vertical, and the extent of resection.
It is important to remember that the majority of MWL body-contouring patients may be undergoing multiple body-contouring procedures in one or more stages; so, it is important to consider the timing and sequencing of the medial thigh lift. In general, the abdominoplasty/lower body lift is completed prior to medial thigh lifting, typically separated by a healing period of 3 or more months. Addressing the trunk first includes tightening and anchoring the lateral thigh, making the medial thigh procedure more effective. During the surgical planning, the thigh should also be examined to determine whether there is excess skin and subcutaneous tissue, or simply excess skin involved. In patients in whom excess subcutaneous tissue is present, direct tissue excision can be combined with liposuction at a single stage. More commonly, liposuction is performed at an earlier phase (e.g., combined with the lower body lift) in a pre-resection decompressive strategy.
47.2.1 Preparation for Surgery
A thorough history and physical exam during the initial consultation are key to creating the best treatment plan for the patient. Patients who have undergone MWL should have a stable weight for at least 3 months prior to surgery. The body mass index (BMI) of the patient at the time of surgery is important both to the risk of complications and to the quality of the result which is to be expected. Patients with a BMI above 30 to 32 are usually not offered medial thigh plasty until they are able to reduce their BMI to this more favorable range. Pertinent comorbidities should be documented and optimized prior to surgical intervention, and note should be taken of any history of previous lower extremity surgery. As most patients present for body contouring after MWL, investigation into method of weight reduction should be undertaken, as many nutritional deficiencies that may impair wound healing are often present in this population. Smoking cessation is required for at least 1 month prior to intervention. Appropriate preoperative imaging and labs should be obtained based on patient age and risk factors.
Patient expectations should be clearly defined prior to any intervention. It is particularly important to ensure that patients understand the extent of achievable contouring and the possibilities of residual tissue laxity or excess. Patients should be counseled on the risks of surgical intervention, including poor scarring, wound dehiscence, seroma, hematoma, lower extremity swelling and lymphocele formation, infection, and recurrent deformity.
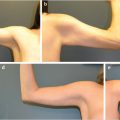
The first medial thigh lift was described by Lewis in 1957. 3 , 4 His initial technique involved excising tissue in both a horizontal and vertical vector. Lockwood later described performing a vertical vector excision through a horizontal scar pattern, and also advocated anchoring the medial thigh tissue to Colles’ fascia to improve results. 5 Despite the incorporation of these principles, horizontal medial thigh lifting is a procedure that is frequently compromised by scar descent (so that it is visible outside of undergarments or bathing suits) or traction on labial tissues, leading to symptoms of dryness (Fig. 47‑2).
For these reasons, patients with laxity limited to the upper third of the thigh may be candidates for horizontal excision. However, the majority of patients presenting for body contouring have laxity that extends beyond the upper third of the thigh. This must be addressed with a vertical excision pattern. The fundamental aspect of this approach to medial thigh lift is to use the vertical tissue resection to reorient the vertical tension vector in a horizontal fashion. This horizontal pull in the anterior and posterior planes allows for successful skin and thigh circumference reduction.
The patient is marked in the preoperative holding area prior to induction of anesthesia. The anterior extent of excision is planned using a variant of the lift and drop technique, with the proximal dog-ear taken out anteriorly along the groin. The final scar is designed to run along the medial aspect of the leg in an area of minimal visibility. The patient is placed in the supine position, antibiotics are administered, and general anesthesia is induced. The legs are abducted and may be supported in this position by stirrups, spreader bars, or bolsters. Pneumatic compression devices are placed prior to induction.
The anterior skin marking site is incised sharply, and dissection is carried out through the superficial fascia. At this plane, the tissue is mobilized from anterior to posterior. It is critical to maintain this level of dissection, which helps preserve the saphenous vein as well as the surrounding deep lymphatics. As the dissection is carried more proximally in the groin region near the femoral triangle, it is important to preserve all fat in this area and merely undermine skin, in an effort to avoid the underlying lymphatics. The posterior saphenous branch is consistently encountered coursing at an oblique angle into the elevated flap, and is ligated.
During the dissection from anterior to posterior, the elevated tissue is periodically advanced to determine the limits of dissection, with the goal being to minimize elevation of nonresected tissue and thus minimize surgical dead space. This measurement ultimately determines the extent of skin resection. In order to help conceal the scar proximally over the groin, we have followed the example of Kenkel and Eaves and added a “bottleneck” proximally, removing slightly more proximal anterior skin to better position the final scar. 6
Once the final extent of tissue excision is determined, hemostasis is achieved. In most cases, the tissue may be closed without a drain in place. However, drains may be considered for patients with an elevated BMI or those undergoing concomitant liposuction. Our approach to the excision and closure is a “close-as-we-go” philosophy. Closing the tissue in conjunction with the excision allows the closure tension to be continuously assessed for consistency. In the unlikely scenario that resection in a segment makes closure difficult, a portion of the incised flap can be repositioned back in the wound to assist in closing the wound. The superficial fascia is typically closed in interrupted fashion with a heavy polydioxanone suture (0 or 1). The skin is closed in one or two running layers of 3–0 or 4–0 monofilament absorbable suture. Topical skin adhesives may be utilized to dress the wound. Compression garments may be used immediately postoperatively based on surgeon’s and patient’s preference.
47.2.2 Postoperative Care
In properly selected patients, medial thigh plasty is safely performed in the ambulatory setting, and may also result in less postoperative complications. 7 Patients are encouraged to ambulate early postoperatively and gradually increase activities as comfort allows. Antibiotics are not routinely prescribed postoperatively. The wounds are examined for any evidence of infection or dehiscence, and minor wound complications are treated with daily wet-to-dry dressings until healing by secondary intention occurs. Compression garments may be utilized on a case-by-case basis depending on the use of concomitant liposuction, the presence and extent of swelling, as well as patient’s preference. Postoperative deep vein thrombosis chemoprophylaxis is recommended by some authors, but there is no currently consensus over use, timing, or duration.
47.3 Outcomes and Complications
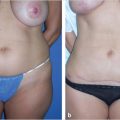
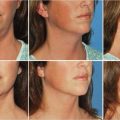
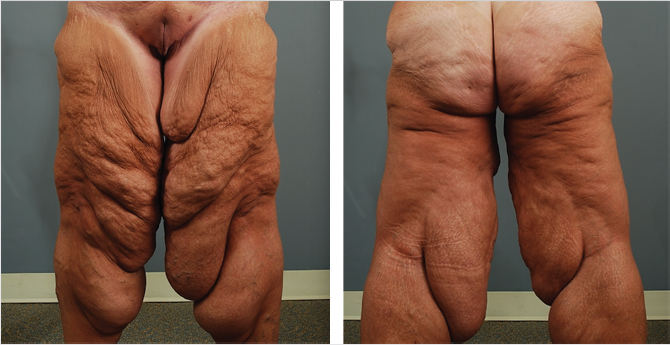
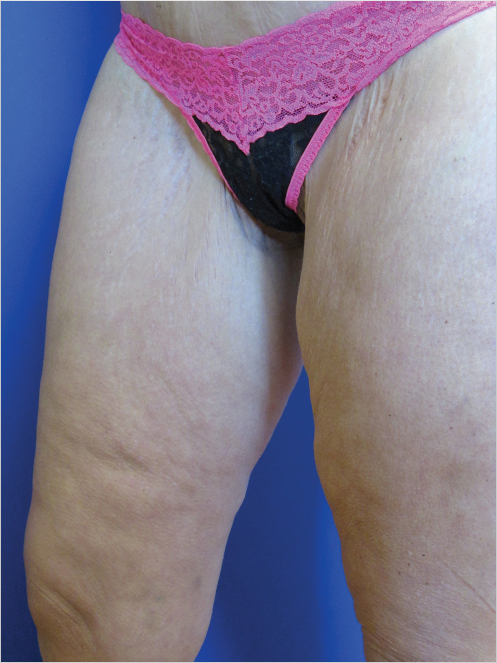
Medial thigh lift is an effective method of treating thigh excess, especially in patients who have undergone MWL (Fig. 47‑3; Fig. 47‑4). In patients seeking body contouring after MWL, quality-of-life (QOL) assessment is an important endpoint to evaluate the effectiveness of therapy. Some small case series have shown that following medial thigh plasty, patients report increased overall satisfaction rates and are willing to trade the scar burden for improved functional status and aesthetic appearance. 8 Overall patients have shown significantly improved mean QOL scores postoperatively when compared to preoperative evaluation. 9 , 10 Furthermore, these scores did not change over time, revealing that the improvements in quality are sustained. Currently, two new patient-reported outcome instruments are being developed, the Body-QoL and the BODY-Q, which will serve to measure satisfaction after body-contouring procedures specifically. 11 , 12 Once utilized, these tools will further elucidate the postoperative QOL changes in this patient population.
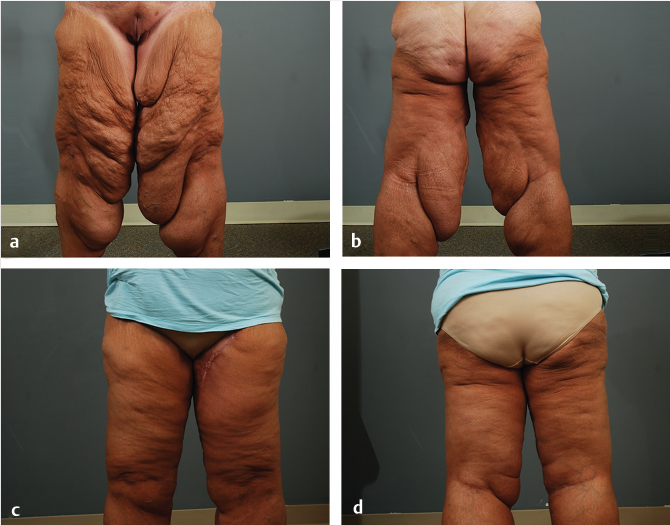
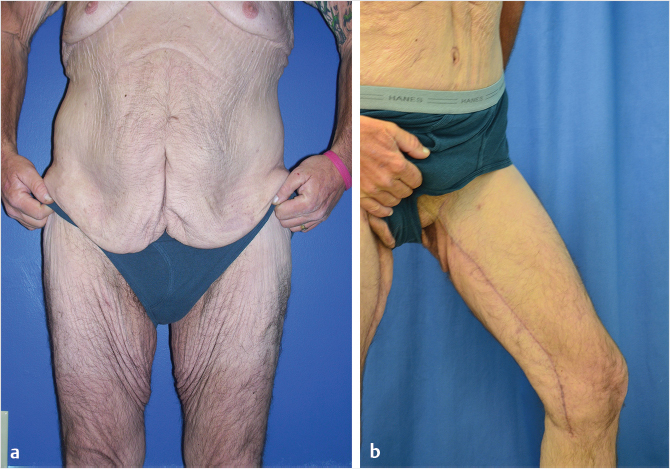
While the positive impact on patients from medial thigh lifting is significant, reported overall complication rates following medial thigh lift range from 40 to 68%. 9 , 13 , 14 In a review by Gusenoff et al, the authors concluded that sex, BMI, smoking, diabetes, hypothyroidism, and concomitant liposuction at the time of thigh plasty were not associated with increased complications postoperatively. 9 The commonly cited risk factors include anemia, older age, elevated BMI prior to weight loss, elevated BMI at the time of surgery, and hypertension. 9 , 14 Additionally, a larger resection length and additional procedures at the time of thigh plasty have also been associated with increased risk of complications. 9 , 15 The most common complication is the development of limited open wounds, especially proximally. These can typically be managed conservatively until healing by secondary intention occurs. Other common complications following body-contouring surgery include seroma, hematoma, soft-tissue infection, lower extremity edema, scar widening, pulmonary embolism, and labial distortion. A review by Shermak et al of MWL patients following body-contouring surgery cited a seroma rate of 18% with lower body-contouring procedures. Additionally, the authors concluded that in patients with a BMI greater than 30, the major risk factor for seroma formation was the weight of skin removed. 16
Development of lower extremity edema can occur after medial thigh plasty. While relatively uncommon, lower extremity edema has been reported to develop in 9 to 29% of cases. 9 , 13 , 17 , 18 Utilizing a superficial dissection superiorly and preserving the saphenous vein are important to reduce this risk. 9 , 19 Additionally, using a full length vertical incision may be associated with increased risk of lower extremity edema. 9 , 18 Many of these cases resolve with conservative management after 3 months, and almost all patients have improvement by 1 year. 9 There are various strategies in regard to compression garments postoperatively. Some authors recommend immediate compression, others recommend delayed compression, and some recommend no compression at all. Currently, there is not enough information known to make an evidence-based recommendation on compression strategies to prevent lower extremity edema.
There have been no large prospective studies examining thrombotic complications exclusively in the medial thigh lift population. However, the Caprini risk-assessment score has been validated for use in the plastic surgical population, and can be a useful tool to determine if a patient is at high risk for postoperative thrombosis. The overall rate of deep vein thromboses in body-contouring patients ranges from 0.05 to 3%, and risk factors identified include BMI greater than 35, older age, and inpatient admission. 20 , 21 However, since a relatively small percentage of these patients had isolated medial thigh plasty, the true incidence of venous thromboembolism or any benefit associated with pharmacologic prophylaxis following thigh lift still remains uncertain.
The medial thigh lift is a safe and effective procedure to address excess thigh tissue. The procedure is most commonly performed in the MWL population, and has been shown to significantly improve QOL postoperatively.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree