Abstract
This chapter covers the pertinent considerations involved in this common surgical procedure for the localized or regional (abdomen, flanks, back, buttocks, lower extremity, upper extremity, neck, axilla, breasts) removal of fat. Case examples for the most common liposuction sites are included. It is a management tool for the purpose of body contouring, not for the management of obesity. The ideal candidate is described, as well as contraindications for surgery. The four primary treatment options (suction-assisted, power-assisted, ultrasound-assisted, laser-assisted) are discussed, and each technique employed in the operation is cited to guide the surgeon through the procedure. Seasoned advice on postoperative care and several paragraphs on potential outcomes conclude the study.
43 Liposuction
43.1 Goals and Objectives
Report the current incidence and trends of liposuction in North America and worldwide.
Effectively evaluate patients preoperatively for liposuction.
Formulate a surgical treatment plan to safely perform liposuction.
Understand the differences among the various types of anesthesia and wetting solutions involved in liposuction.
Institute appropriate perioperative care to maximize patient safety and surgical outcomes.
Diagnose postoperative complications (both early and late) and formulate appropriate treatment plans.
43.2 Patient Presentation
Suction-assisted lipectomy, or liposuction, involves the surgical aspiration of fat from the subcutaneous space. It involves removal of localized or regional deposits of adipose tissue for the purpose of body contouring, but is not a management of obesity. Liposuction is the most commonly performed aesthetic surgical procedure in the United States according to the American Society of Aesthetic Plastic Surgery (ASAPS) cosmetic national database (342,494 procedures performed in 2014). This represents a 94% increase since the database initiation in 1997. 1 According to the International Society of Aesthetic Plastic Surgery (ISAPS), liposuction ranks second behind eyelid surgeries in worldwide procedures performed in 2014 (1,372,901 procedures performed). 2 Liposuction is being performed increasingly in combination with other surgical procedures to enhance outcomes.
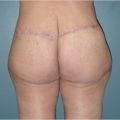
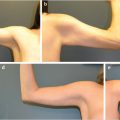
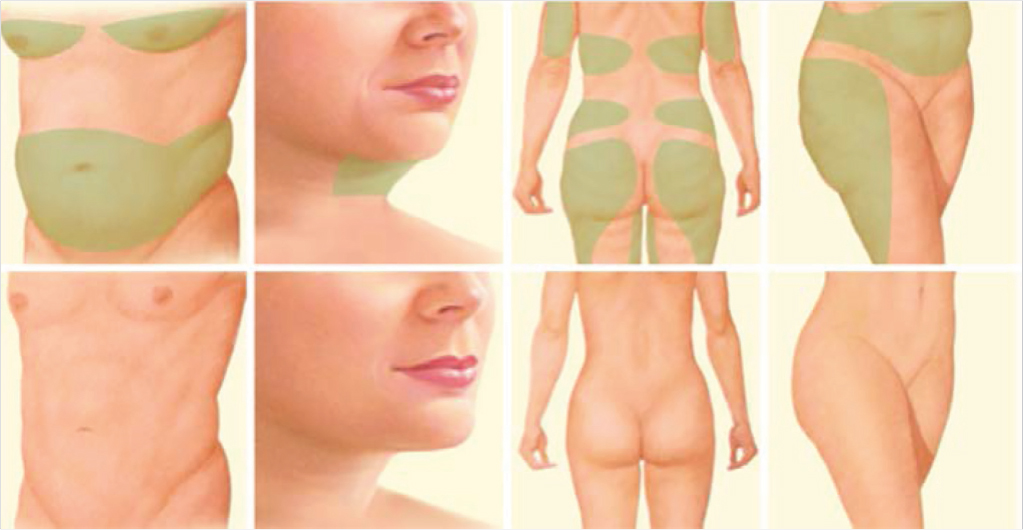
Patients who present for body-contouring procedures desire a reshaping of various regions of their body. Although the trunk has been classically known as the most popular site for liposuction, more and more patients are electing to remove excess adiposity from the upper and lower extremities, breasts/axilla, hips, and neck regions (Fig. 43‑1). Equally, patients must understand that liposuction is not a weight loss procedure, but aimed at the reduction of local accumulations of excess fat. 3 An ideal candidate for liposuction is a healthy individual, close to his or her ideal body weight, with realistic body-image expectations, and motivated to making long-term lifestyle changes. 4 Women typically desire to remove excess fat peripherally to obtain a gynecoid body figure, while men aim to reduce excess central fat distributions. 5
Patient evaluation should begin with a thorough medical and surgical history and a diligent physical exam. The medical history should include specific comorbid conditions, blood clotting disorders, and especially a full medication history (including vitamin supplements, herbal products, and any weight-loss medications). Medications that predispose to bleeding should be avoided. The surgical history should include any surgeries associated with the pertinent body areas in question as well as any major operations and any previous complications. Knowledge of previous weight loss and body-contouring procedures are particularly important. Prevention of venous thromboembolism is a particular concern of all body-contouring procedures, including liposuction. A higher rate of venous thromboembolism has been demonstrated in patients with a body mass index (BMI) greater than 30, patients taking hormone therapy, and those with a higher Caprini risk assessment. For patients receiving a general anesthetic, sequential compression devices (SCD) should be utilized when possible along with proper patient positioning (allowing maximal lower extremity venous drainage) and avoiding external pressure or constriction of the lower extremities. Preoperative chemoprophylaxis may be warranted depending on individual patient risk factors, guided by the venous thromboembolism task force recommendations by the American society of Plastic Surgeons (ASPS). 6 , 7
Obtaining a weight history is important in order to determine if a patient has a high risk of gaining weight following liposuction. 4 Candidates within 20% of an ideal body weight ultimately have the best long-term satisfaction. In general, patients with a BMI greater than 30 may benefit from lifestyle modifications before considering most body-contouring procedures. 8
During the physical examination, the patient should be completely disrobed. The patient’s height, weight, BMI, and circumferences of pertinent body regions should be documented. 6 The overall fat distribution should be assessed and gentle pinch testing should be used to assess the thickness of subcutaneous fat. The sites of interest should be examined in multiple positions: standing, sitting, and in the supine position. It is essential to evaluate the location and degree of adiposity as well as the laxity of the targeted areas. A comprehensive skin exam is also crucial to determining a good outcome from surgery. Skin and dermal quality can be assessed by observation and palpation. Thick dermis has more retractile strength, which is favorable for liposuction. Furthermore, elastic skin is favorable compared with flaccid skin for retraction outcome. A snap-test or pinch of skin test can be used to assess skin recoil. Individuals with cellulite, dimples, wrinkles, or very loose skin may have less than ideal results. Individuals with excess skin laxity may require skin resection (i.e., abdominoplasty, brachioplasty, thigh plasty, etc.) as liposuction without adequate skin recoil will result in loose and folded skin.
Lipodystrophy can be located in the following areas: abdomen, flanks, back, buttocks, lower extremity (thighs, knees, ankles, and calves), upper extremity, neck, axilla, and breasts. Men who present for abdominal liposuction should be examined diligently, as abdominal bulging can be attributed to intra-abdominal fat, which cannot be addressed with liposuction. The presence of an occult abdominal hernia must be evaluated and abdominal wall scars should be noted; an abdominal hernia can be most easily diagnosed in the supine position. Surface irregularities such as dimpling and cellulite (lipomatous deposits) should be noted and demonstrated to the patient, as these may remain and actually may become more perceptible postoperatively. Patients should understand that while liposuction can be used to contour areas, it does not address cellulite. In contrast, skin dimpling (typically caused by an underlying fascial attachment) may be improved with liposuction. 6 Furthermore, patients should be aware of possible persistent asymmetry, dimpling, and depressions following liposuction. Ideal patient characteristics for liposuction are listed in Table 43‑1 and relative contraindications are listed in Table 43‑2.
43.3 Preparation for Surgery
Healthy patients should have a complete blood count to evaluate preoperative hemoglobin and hematocrit for possible anemia or occult blood loss. Patients who have undergone significant weight loss operations (bariatric surgery) must be carefully assessed for nutritional status (serum albumin or prealbumin), anemia, and vitamin deficiencies contributing to anemia (vitamin B12 and iron). 9 The patient should consult with their primary care physician for discontinuation of herbal supplements (vitamin E, St John’s wort, etc.), weight-loss medications, nonsteroidal anti-inflammatory drugs, aspirin, hormone products (hormone replacement therapy [HRT], oral contraceptive pill [OCP], etc.), fish oil, and other supplements for at least 4 to 6 weeks before the procedure date to ensure normal wound healing and blood clotting and to lower the risk of thrombosis. Medications that interact with liver metabolism of lidocaine, one of the main components of tumescent solution, should also be stopped; these include selective serotonin reuptake inhibitors (SSRI), erythromycin, ketoconazole, and other agents.
Smoking increases the risk for postoperative complications because of tobacco’s primary effects on vasoconstriction and decreased wound healing capacity. The authors agree with the Centers for Disease Control and Prevention (CDC) recommendations of smoking cessation 30 days prior to surgery.
For higher risk individuals and patients in an inpatient setting, assessing coagulation profiles (PT/PTT), a comprehensive metabolic panel (CMP), HIV serology, and a hepatitis viral panel should be considered. An ECG and an echocardiogram should be obtained for individuals with pertinent cardiovascular history. Abnormalities should be cleared by the respective medical specialists prior to consideration of any elective surgery.
43.4 Treatment
Several options exist for liposuction procedures 10 :
Suction-assisted liposuction (SAL).
Power-assisted liposuction (PAL).
Ultrasound-assisted liposuction (UAL).
Laser-assisted liposuction (LAL).
Suction-assisted lipoplasty uses an external source of suction to facilitate fatty tissue removal. 6 In power-assisted lipoplasty, the system driving the cannula is an electrically or gas-driven power source; a motor moves the cannula tip in a forward and backward motion reducing physician fatigue. 6 This is effective for large-volume fat removal, fibrous areas, and revision procedures. Syringe aspiration of fat is effective for sensitive and smaller volume areas such as the neck. Ultrasound-assisted liposuction uses a cannula to deliver ultrasound subcutaneously to liquefy fat. 6 This facilitates removal of fat from fibrous areas such as the upper abdomen and back, especially during secondary or revision procedures. Thermal injury is a risk during this technique but can be avoided by keeping the cannula in constant motion and by using tumescent solution as this cools the heat generated in the process. Additionally, the ultrasound should be used in a time-limited manner, usually at about 1 minute per 100 mL of tumescent solution instilled. Laser-assisted liposuction is designed to achieve skin tightening from the thermal effect of laser on the dermis through selective photothermolysis of fat and water chromophores. 11 There are currently no randomized controlled studies reporting laser-assisted liposuction to have significant clinical advantages over “traditional” suction-assisted liposuction. 11
The indications for liposuction surgical treatment fall broadly under several categories:
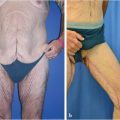
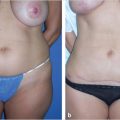
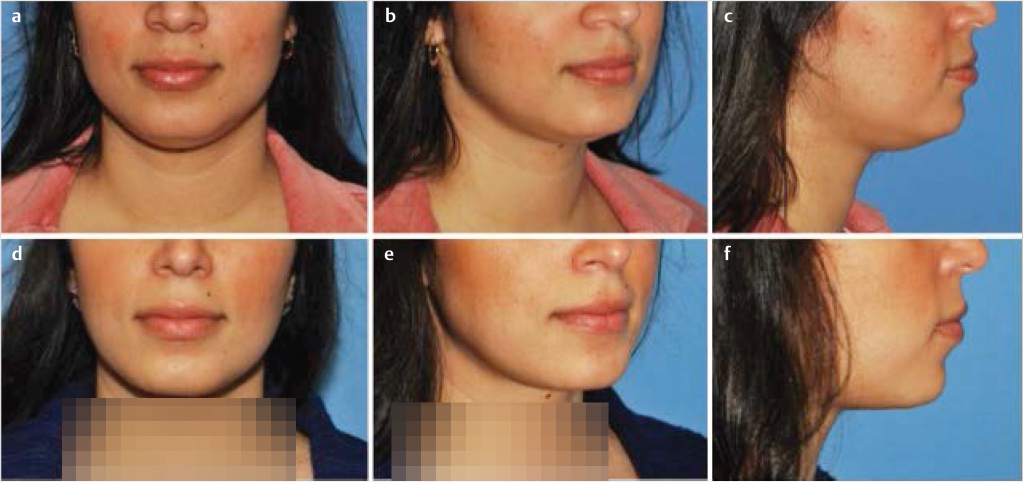
“Isolated procedure” cosmetic contouring (most common indication, Fig. 43‑2).
Adjuncts to other cosmetic surgical procedures (abdominoplasty, body lift, breast reduction, breast augmentation, weight loss skin removal surgeries to debulk adipose tissue content). 12
Liposuction can be used on abdomen and flanks in combination with full and mini-abdominoplasties after tissue dissection and resection.
Treatment for specific medical disorders.
Gynecomastia—often requires additional resection of glandular tissue.
Buffalo hump—reducing uncomfortable fat deposits on back.
Lipomatosis syndromes.
Other—lipodystrophy from HIV, etc.
43.5 Surgical Preparation
Preoperative markings are done in the standing position. Zones of facial adherence are noted and to be avoided. Multiple access incisions are used for cannula placement and may be placed in natural skin folds. This often provides easier access and greater safety, especially for transition areas such as the costal margin where injury to intrathoracic/abdominal structures are at greater risk. A thorough operative record is maintained during the procedure to document the volume of subcutaneous tumescent infiltration and the volume of aspiration at each body area of liposuction.
Assessment and reduction of perioperative morbidity is critical and, thus, it is important to note the American Society of Anesthesiologists (ASA) classification for the given patient. Class I and II ASA patients who are healthy or have mild/stable illness, respectively, can be managed as outpatient procedures if the estimated liposuction aspirations are less than 5,000 mL (Table 43‑3). Mortality and morbidity rate increases with more invasive liposuction procedures and an inpatient setting may be considered for ASA class III patients, procedures with an estimated liposuction aspiration more than 5,000 mL, estimated blood loss more than 500 mL, or duration of surgery more than 2 hours. 6 , 13 , 14 , 15 , 16 , 17
Various types of anesthesia are appropriate for liposuction depending on overall patient health and estimated volume of fat to be aspirated. In smaller volume liposuction aspiration cases, anesthetic infiltrate solutions alone may be sufficient to provide adequate pain control during the procedure. This is sometimes combined with a field block performed prior to tumescent infiltration. Several factors allow for increased lidocaine administration over traditional limits. The risk of systemic toxicity from the lidocaine and epinephrine solution is dramatically decreased due to numerous factors including the slow absorption of the infiltrate from fat, the vasoconstriction effect of epinephrine, and because a significant amount of the solution is aspirated. Lidocaine doses up to 35 mg/kg have been generally considered safe to use for solutions containing epinephrine injected into subcutaneous fat; however, doses as high as 55 mg/kg have been described. 6 , 18 , 19 , 20 In patients with low protein states or medical conditions leading to accumulation of lidocaine metabolic byproducts, the maximum lidocaine doses should be reconsidered. It is important to recognize and be cognizant of the signs of lidocaine toxicity, which can vary from lightheadedness, tinnitus and a metallic taste in the mouth to tremors, convulsions, respiratory depression, and even cardiac arrest. 6 Doses of epinephrine should not exceed 0.07 mg/kg, although higher doses have been used safely. 6 Staging the infiltration of multiple anatomical sites can equally reduce the risk of excess epinephrine. Although it is highly unlikely that liposuction would be done in patients who have hyperthyroidism, severe hypertension, cardiac disease, peripheral vascular disease, or a pheochromocytoma, epinephrine should be avoided when such conditions exist. 6 Intravenous sedation can be used in limited smaller volume liposuction cases to maintain patient comfort. General anesthesia is typically required for larger volume liposuction procedures.
Anxiolysis if needed can be maintained with preoperative oral diazepam or lorazepam; less effective are opioids and narcotics. Antihistamines like hydroxyzine can also be used to add sedation and to reduce nausea and pruritus. Finally, as discussed previously, preoperative chemoprophylaxis (either low-molecular-weight heparin or unfractionated heparin) can be used for venous thromboembolism prophylaxis for high-risk patients along with standard lower extremity compression devices.
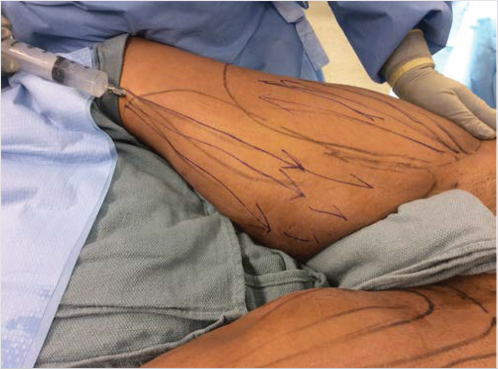
Multiple techniques of liposuction fluid administration exist and have evolved over time. The dry technique involves liposuction without subcutaneous solution infiltration. This has been abandoned because of substantial swelling, discoloration, and blood loss, with suction aspirates containing 20 to 45% blood. 8 In the wet technique, 200 to 300 mL of infiltrate is injected per body area before insertion of the liposuction cannula; this reduces blood loss up to 4 to 30% of the aspirate. 8 In the superwet technique, 1 mL of solution is injected for each 1 mL total aspirate to be removed; this reduces blood loss to less than 1% of the aspirate volume. In the tumescent technique, 3 to 4 mL of infiltrate is infused for each planned 1 mL of aspirate; blood loss in this technique is also estimated to be less than 1% of the aspirate volume. 8 After wetting solution injection in the tumescent technique, the skin should feel firm and indurated indicating complete infusion (Fig. 43‑3). Large-volume liposuction, defined as a total aspirate of 5,000 mL or greater, can be safe for selected patients and with appropriate intraoperative fluid balance. Overnight observation is recommended after large-volume liposuction. 21 Liposuction fluid resuscitation guidelines are outlined in Table 43‑4.
Small-volume aspirations (<5 L) | Large-volume aspirations (>5 L) |
Maintenance fluida Subcutaneous infiltrateb | Maintenance fluida Subcutaneous infiltrateb 0.25 mL of intravenous crystalloid per mL of aspirate >5 L |
aAmount of fluid to be replaced from preoperative, nothing by mouth status. b70% is presumed to become intravascular. | |
43.5.1 Operative Technique
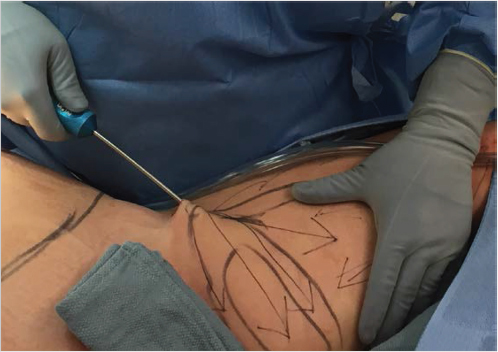
Following infiltration of tumescent solution, 10 to 20 minutes is allotted to allow for the full effect of vasoconstriction prior to liposuction. The same access points used for tumescence are typically used for liposuction. During liposuction, a blunt-ended hollow cannula is used to tunnel under the skin and aspirate fatty tissue. The diameter of the tip typically ranges from 2 to 5 mm and is driven backward and forward manually in SAL or with a motor in PAL. The cannula is first inserted vertically into the incision site, and then readjusted to the orthogonal plane (the coronal plane for abdominal liposuction). The key to safe and adequate aspiration with the cannula is tunneling in an appropriate plane, just deep to the superficial fascia. The operating surgeon should at all moments know the exact location of the cannula to ensure safe technique. This is facilitated by the nondominant hand that can be used to push down and apply gentle pressure to the skin above the deep plane to guide the cannula. Care must be taken not to compress the tissue when lifting skin and subcutaneous tissue with the cannula; skin pinching to assess for asymmetry and lumps is appropriate. Linear and rhythmic strokes should be made in fan-like distribution that circumferentially removes the fat consistently and evenly in the marked out area. Tunneling should be done in the mid-fat and deep-fat planes to ensure even adipose removal (Fig. 43‑4). Major lymphatic, nerve, and blood vessels should be avoided; tunneling parallel to the longitudinal axis of the body (e.g., avoiding epifascial lymph vessels in lower extremity) has been shown to reduce the risk of vessel damage. 22 , 23
Liposuctioned fat is emulsified and oily, and can be preserved for autologous fat transfer. 24 Incisions can be closed with 5–0 nylon sutures (or fast absorbing suture) or can be left open for drainage if greater than 2,000 mL of lipoaspirate was removed in total.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree