Abstract
Gynecomastia is an anomaly involving the enlargement of the male breast due to an increase in glandular, stroma, and/or fat tissue. Physiologic and pathologic etiologies of this condition are reviewed, with special emphasis given to the possibility of breast cancer. Surgical options discussed in detail include traditional suction-assisted lipectomy, ultrasound-assisted liposuction, the pull-through technique, direct periareolar excision, circumareolar resection, vertical resection, inverted T resection, and subcutaneous mastectomy with free nipple graft. The authors conclude their chapter with guidelines on postoperative care and outcomes.
39 Gynecomastia
39.1 Goals and Objectives
Understand the etiologies for both physiologic and pathologic gynecomastia.
Appreciate the presentation of gynecomastia and key findings in the history and physical examination that warrant additional testing.
Understand the various treatments for gynecomastia and when each is indicated.
Be able to discuss postoperative care, including complications.
39.2 Patient Presentation
39.2.1 Introduction
Gynecomastia remains an important problem encountered by plastic surgeons. It is the most common hyperplastic breast anomaly in children, affecting up to two-thirds of adolescent males during puberty. 1 True gynecomastia is the benign enlargement of the male breast resulting from an increase in glandular (ductal not lobular tissue), stroma, and/or fat. Pseudogynecomastia describes an isolated increase in fat. Patients may present with unilateral or bilateral breast tenderness and pain, a palpable lump, concern for malignancy, and dissatisfaction with their appearance. Gynecomastia is not just a cosmetic problem as patients often experience extreme psychosocial and self-esteem issues. 2 These patients suffer teasing from peers, have difficulty entering into relationships, and may avoid showers, swimming pools, or any sports activity that may result in exposing their chest. In these patients, consideration for psychotherapy as an adjuvant to surgical treatment should be given. 2 , 3
39.2.2 Etiology
The most common cause of gynecomastia is idiopathic (25%). Other causes can be broken down into physiologic and pathologic. 4 , 5 Physiologic gynecomastia has three categories: (1) neonatal, (2) adolescent, and (3) elderly. The cause is an increase in the estrogen to testosterone ratio, or defects in testosterone receptors. Obesity may contribute to the onset of gynecomastia due to increased estrogen secretion from fat cells. At birth, gynecomastia can be seen as higher levels of circulating maternal estrogens are present. This type of gynecomastia is transient and resolves as estrogen levels decline. Adolescence is the most common time period patients experience physiologic gynecomastia and can be seen in up to two-thirds of adolescent males during puberty. While gynecomastia may resolve with time and/or weight loss, surgery is an option when gynecomastia is persistent. Gynecomastia has a third peak in the elderly patients older than 65 years, believed to be from a decline in testosterone. 4 , 5
A list of pathologic causes are shown in Table 39‑1 and can be further divided into (1) systemic diseases, such as liver failure, renal failure, and malnutrition; (2) diseases/tumors of endocrine glands such as thyroid, pituitary, adrenal, and testes; and (3) drugs and medications. 4 , 5
39.3 Breast Cancer and Gynecomastia
The incidence of breast cancer in patients with gynecomastia is similar to that of the general male population. Males make up approximately 1% of all breast cancer, with an occurance of about 1 in every 1,000 males. 5 , 6 This means treatment with liposuction, in which no specimens are sent to pathology, can be safely performed without significant concern for occult malignancy. 7 Patients with Klinefelter syndrome, however, have a 20- to 30-fold higher risk of developing breast cancer than the general male population. While this must be considered for preoperative planning and surgical treatment, it is unclear if every male with Klinefelter syndrome should undergo screening mammography prior to breast surgery, as males still have a lower risk of breast cancer than the general female population. 6 In these patients, a discussion about male breast cancer should be initiated, and screening mammography should be performed on a case-by-case basis.
39.3.1 Histology
There are two main histologic types of gynecomastia: florid and fibrous. Florid gynecomastia is seen within the first few months of onset. It is characterized by an increase predominantly in ductal tissue. Fibrous gynecomastia is usually seen greater than 1 year after onset. Histology demonstrates an increase in fibrous stroma with minimal ducts. There is an intermediate subtype which occurs in the transition period from several months to 1 year of onset. 8
39.3.2 Classification
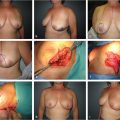
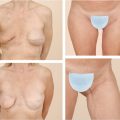
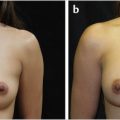
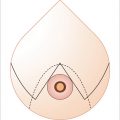
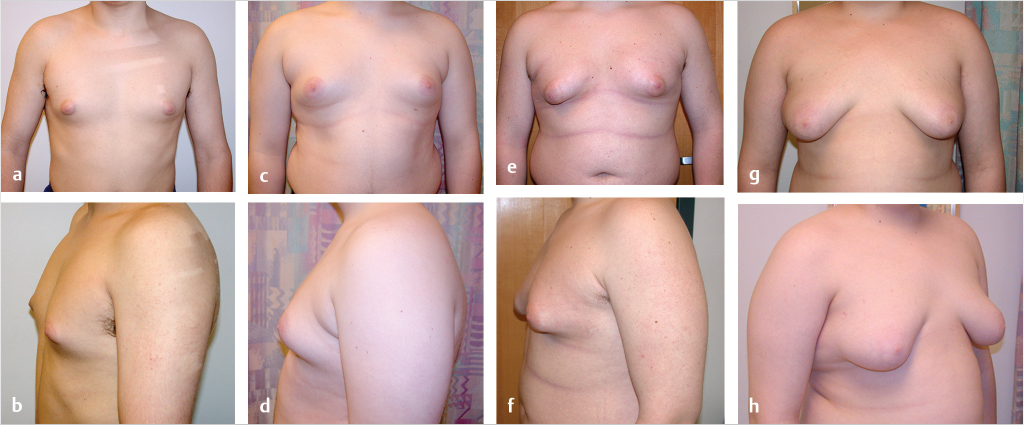
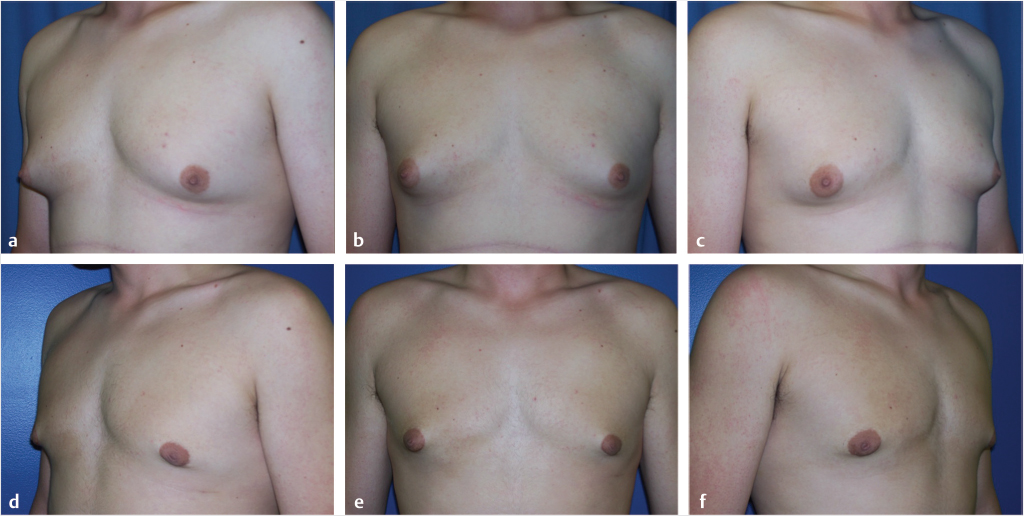
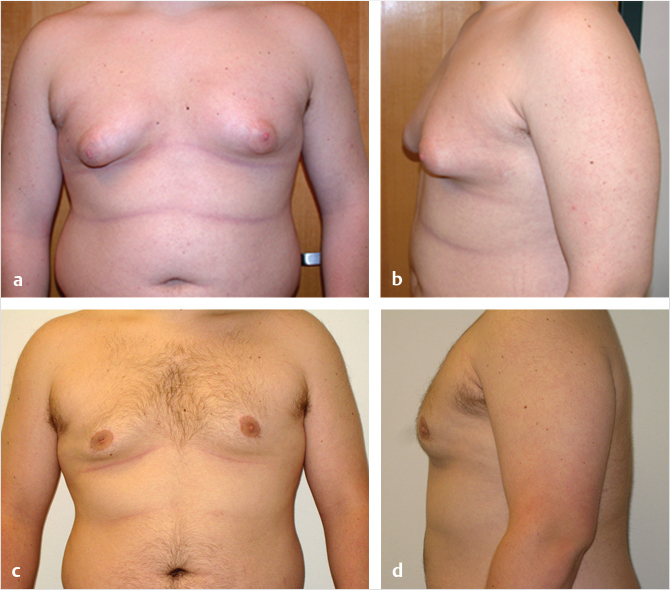
Gynecomastia may range from minimal enlargement of breast tissue to severe overgrowth with excess skin and/or ptosis (Fig. 39‑1). Classification systems take into account volume of breast tissue enlargement and whether or not there is excess skin and/or ptosis. Patients have different severities on presentation, varying from a retroareolar mass with no skin excess (Fig. 39‑1a,b), to extensive breast tissue and excess skin with no ptosis (Fig. 39‑1c,d), to significant breast tissue with skin excess and ptosis (Fig. 39‑1g,h). Although over the last several decades many classification systems have been developed for gynecomastia, there is no universally used system.
39.4 Preparation for Surgery
The history and physical examination is essential in evaluating patients who present with gynecomastia. Questioning should include symptoms, age of presentation, duration, whether the size of the breasts is stable, a careful review of systems and drug/medication use. Patients undergoing surgery must have proper assessment of risk factors that may influence safety and potential complications.
Key physical examination findings include a “pinch test” to help determine consistency of breast tissue (glandular, fibrous, solid, or fatty). The classic presentation for glandular gynecomastia is a mobile well-circumscribed retroareolar mass with a rubbery consistency. Excess skin and/or ptosis will affect treatment decisions. It is important to note that gynecomastia can be unilateral in 14 to 51% of patients, so unilateral breast enlargement alone is not cause for alarm. 9 , 10 , 11 Special attention should be given to abnormalities that raise concern for cancer such as spontaneous nipple discharge, irregular skin changes, and nodules with varying consistencies. Physical examination of the thyroid and testes should also be performed to evaluate for pathologic causes.
Laboratory testing and imaging studies are not necessary in every case. Healthy adults and pubertal adolescents having a history consistent with physiologic gynecomastia and a normal physical examination do not require further testing. If abnormalities are found on history or physical examination, or there is concern for pathologic gynecomastia, further testing is indicated. Prepubertal gynecomastia requires additional workup including testicular ultrasound. Patients with feminizing characteristics (small testis, lack of male hair distribution) also require hormone testing. Feminizing characteristics associated with a Marfanoid body habitus are associated with Klinefelter syndrome. Karyotype and hormonal testing are indicated. Testicular or thyroid masses require hormone testing and ultrasound. 4 , 5 Massive weight loss patients may require additional testing to assess nutrition and blood count. 12
39.5 Treatment
Surgery remains the gold standard treatment of gynecomastia. Indications include to improve symptoms, cosmesis, and patient well-being. Intervention should be considered no sooner than 12 months after the onset. Any abnormalities, underlying conditions, and causative drugs/medications should be addressed and treated prior to surgery. Treatment of the underlying cause and discontinuation of causative medications can cause regression of gynecomastia. Despite different approaches, objectives generally remain the same: to correct the appearance of a feminine chest, eradicate the inframammary fold, remove redundant breast tissue and/or skin, and to achieve symmetry and minimize scaring.
Surgical approaches to gynecomastia include the following techniques: traditional suction-assisted lipectomy (SAL), ultrasound-assisted liposuction (UAL), the pull-through technique, direct periareolar excision, circumareolar resection, vertical resection, inverted T resection, and subcutaneous mastectomy with a free nipple graft. Treatment is based on the degree of excess skin and/or ptosis, and the predominant tissue present in the breast. Mild cases of gynecomastia with no excess skin and/or ptosis can be initially treated by liposuction or excision without skin resection. Fatty tissue can be treated with liposuction, while glandular, fibrous, or solid tissue generally does not respond to liposuction and requires surgical excision. More severe cases of gynecomastia with excess skin and/or ptosis may require a skin resection procedure at the initial surgery. 13 , 14 , 15 , 16 , 17
39.6 Operative Technique
39.6.1 Liposuction
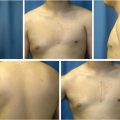
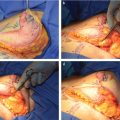
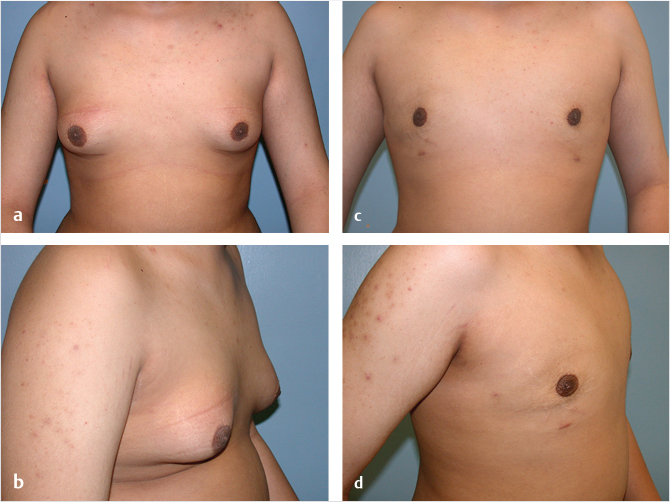
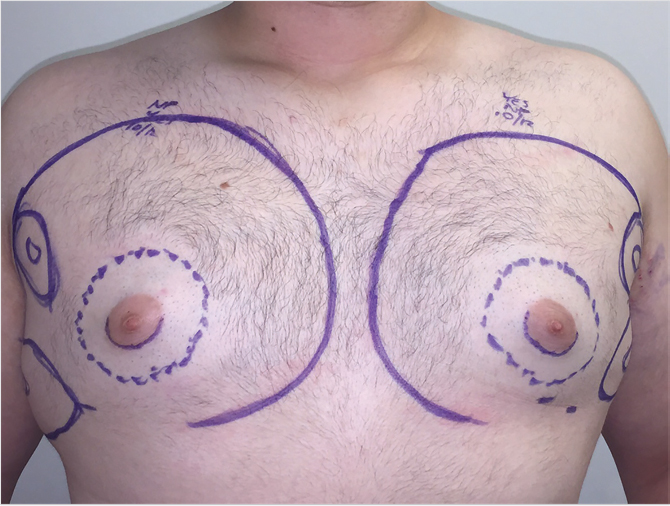
Patients with an isolated excess of fatty tissue can usually be treated with liposuction alone. Liposuction is important in achieving a smooth chest wall contour, disrupting the inframammary fold and removing fatty tissue with minimal scarring. The patient is marked in the upright position, highlighting areas of tissue excess and breast landmarks including the inframammary fold. Under general anesthesia, the patient is placed in supine position with arms abducted. Preoperative antibiotics should cover skin flora. Tumescent solution is used with the super wet technique, 1:1 ratio of infiltrate:aspirate. A standard tumescent solution contains 1 L of lactated Ringer solution + 25 to 50 mL of 1% lidocaine + 1 amp of 1:1,000 epinephrine (end concentration of epinephrine is 1:1,000,000) +/– 12.5 mL of 8.4% bicarb. Commonly two incisions are utilized, an incision in the lateral aspect of the inframammary fold and a periareolar incision at the inferior aspect of the areola. Tumescent infiltration is performed in all areas of tissue excess, through both incisions, using a feathering crosshatch pattern. The surgeon’s nondominant hand should be used to guide the cannula through the subdermal layer. A prominent inframammary fold in males is abnormal and creates the appearance of feminine breasts. While not every surgeon disrupts this fold, some surgeons feel it allows for a smooth transition between the breast and abdomen and improves postoperative skin retraction. 5 Finally, evacuation is performed with a standard 3-mm cannula for final contouring. The ideal endpoint is a smooth flat chest without palpable or visible excess tissue (Fig. 39‑2).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree