Abstract
This chapter deals with the relevant considerations involved in breast implants. Specific data to be gathered during the presurgical exam are detailed, and implant shells (smooth, textured), implant fillers (silicone, saline), implant shape, and implant size are discussed. Relevant surgical procedures involving access incision, pocket location, and surgical techniques are thoroughly covered, and the chapter concludes with seasoned advice on postoperative care and potential outcomes and complications.
32 Breast Augmentation
32.1 Goals and Objectives
Understand the proper evaluation of prospective breast augmentation patients.
Clearly define the benefits and drawbacks for the different types of breast implants and various surgical approaches to breast augmentation.
Appropriately educate patients on the potential complications of breast augmentation.
Know the evidence-based perioperative care to maximize patient safety and quality outcomes.
32.2 Patient Presentation
Patients seeking breast augmentation can vary in diagnosis from simple hypomastia to breast asymmetry or ptosis, to the more complex tuberous breast deformity.
As with all surgical procedures, a general medical history is obtained in order to identify any contraindications to surgery. Specific focused history for breast augmentation patients should include the following:
Any previous breast pathology or breast cancer: Our group requires a documented normal mammogram and/or breast examination within 1 year prior to surgery. Any abnormalities encountered on examination or mammography must be thoroughly evaluated by a breast surgeon prior to breast augmentation.
Pregnancy history: Breasts often undergo substantial changes in both size and shape during pregnancy and breastfeeding. Our group recommends a waiting period of at least 3 months to allow for stabilization of breast size after completion of breastfeeding.
Changes in weight: Fluctuations in weight can significantly affect breast size and shape as approximately 50% of the breast is composed of fat. It is advisable to delay surgery until the patient’s weight has been stable prior to breast augmentation.
Patient’s age: Our group does not perform breast augmentation in patients younger than 18 years. If the patient is younger than 22 years, we do not use silicone implants without a signed waiver acknowledging Food and Drug Administration (FDA) off-label usage.
Physical exam should include a general observation of the patient, including height, weight, body frame, and the presence of any structural asymmetries or deformities. It is imperative to point out any and all asymmetries, as minor differences often go unnoticed by a patient preoperatively, yet can become a significant source of distress after the operation. This is likely due to an increase in the patient’s attention to her augmented breasts postoperatively. In the authors’ opinion, it is far easier to allay patient concerns about an asymmetry that was discussed and documented preoperatively.
Required measurements include nipple-to-sternal notch distance, nipple-to-inframammary fold (IMF) distance, and the breast base–width (taken just above the nipple). The measurement of breast height and intermammary distance are also recommended. Additional helpful findings on physical exam include a pinch test of the upper pole to assess the amount of soft-tissue coverage and an assessment of skin envelope quality (e.g., stretch marks may indicate an inelastic envelope). These measurements are verbalized as they are being taken to reinforce any asymmetries to the patient.
The lie of the breast on the chest wall (i.e., lateralization of nipple and breast) versus normal positioning should also be documented. It should be discussed with the patient that the postoperative intermammary distance is determined by the preoperative state. Simply stated, with a properly sized implant, the patient with a normal intermammary distance will be normal and patients with a wide intermammary distance will be wide postoperatively. It is imperative that the patient understands that the breast footprint cannot be changed. Essentially, breast augmentation fills out the existing breast behind the existing nipple position.
32.3 Preparation for Surgery
There is no single approach in breast implant surgery that is ideal for every patient. Surgical decision-making should be customized to the needs and expectations of the patient. However, in general, preparation and planning for surgery can be broken down into three major decisions: implant selection, access incision, and pocket location.
32.4 Implant Selection
32.4.1 Implant Shell
Essentially, two types of implant shell are currently available: smooth and textured. While the texturing process varies by manufacturer, these devices were developed to mimic the surface of polyurethane covered implants, which had very low capsular contracture rate, but were removed from the market due to breakdown to a carcinogenic compound. Level I studies have not supported the lower capsular contracture rates utilizing the current textured implants. 1 , 2 , 3 , 4 , 5 , 6 , 7 , 8 , 9 , 10 , 11 , 12 , 13 , 14 Moreover, there are as many level I studies showing no difference as there are that show a benefit, which likely indicates that surface texture does not have a major role in capsular contracture, especially in the subpectoral pocket plane. The available literature is less conclusive for subglandular pocket plane, and there seems to be a possible benefit of less capsular contracture with implant texturing in this position. 4 , 9 , 10 , 15 However, recent reports have shown an increased incidence of late seroma development associated with implant texturing. 16
32.4.2 Implant Filler Material
The type of implant filler is limited to two choices: silicone and saline.
Silicone is beneficial in that it offers the most natural feel. After a period of unavailability due to health concerns, the FDA again approved silicone implants for general aesthetic augmentation in 2006. However, it should be noted that when silicone implants are used for breast augmentation, their use is limited by the FDA to patients older than 22 years. 17 As new generations of implants have been introduced, the silicone gels have become progressively more cohesive through crosslinking of the silicone polymer. Currently, all modern silicone implants contain cohesive gels of varying viscosity. Form stable implants maintain their shape without collapsing under their normal weight or being deformed by the surrounding soft-tissue envelope. These implants are often referred to as highly cohesive gels. There is some evidence that form stability has some long-term advantages in minimizing implant-related complications, such as leak and capsular contracture. 18 , 19 , 20 However, for a given volume, form-stable implants require incisions 0.5 to 1.0 cm larger than round non–form-stable implants. For all modern silicone filled implants, the FDA recommends that patients receive MRI screening for silent rupture 3 years after the initial placement and every 2 years thereafter. 21
Although the feel of saline implants is less natural than that of the silicone gels, leaks are easier to detect and are safely absorbed by the body. Additional disadvantages include an increase in visible implant wrinkling. From a procedural standpoint, these implants require access incisions that are smaller and potentially more easily concealed, since they are inserted in a deflated state. In addition, there is room for intraoperative adjustment of the final implant size based on the manufacturer recommended fill range making these implants particularly advantageous in patients with significant asymmetries.
32.4.3 Implant Shape
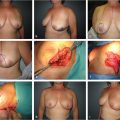
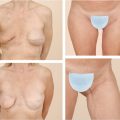
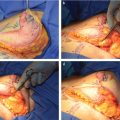
Both silicone and saline implants are now available in a large variety of shapes (Fig. 32‑1, Fig. 32‑2, Fig. 32‑3, Fig. 32‑4). Most round implants come in different projections for a given volume (low-profile, moderate-profile, moderate-plus-profile, high-profile, and ultra-high-profile). Shaped/anatomic implants come with even more variability because of an asymmetric shape in which width, height, and projection can all be varied. In general, these implants have a tapered upper pole and fuller lower pole, which is intended to give a more natural breast shape. However, utilization of shaped implants requires more precision as orientation must be both appropriate and symmetric. Over-dissection of the implant pocket can lead to malposition and rotation, which is highly problematic when utilizing a shaped device. Studies have shown that patient satisfaction is similar in using either a round or shaped device. 19 Further, plastic surgeons saw no difference in regard to overall breast beauty by implant shape and scored round implants higher in regard to naturalness and upper pole appearance (Fig. 32‑5, Fig. 32‑6, Fig. 32‑7). 22




32.4.4 Implant Size
The primary driving force for many patients regarding size selection remains achieving a desired cup size. However, choosing volume in this manner often leads to reoperation, as the volume selection has not matched the tissue characteristics or the footplate of the breast. Alternatively, and more appropriately, the guiding principles popularized by Tebbetts should be to optimally fill the breast while respecting its natural boundaries. 23 , 24 Classically, the most important dimension is the width of the breast and therefore the width of the implant itself. The other dimensions and skin envelope may further guide the selection process. Ultimately, we routinely utilize the breast width to select a range of implants available to the patient, and allow the patient to choose the final volume with assistance from the surgeon regarding the type and shape of implant that will best achieve the patient’s goals.
32.5 Access Incision
32.5.1 Inframammary
This approach provides the most direct access to all possible pockets and avoids having to enter the breast parenchyma. The scar is generally well concealed if appropriately planned. This is also the most versatile incision for future revisions. There are data to suggest a decreased capsular contracture rate with this incision when compared to the periareolar incision. 25 , 26
32.5.2 Periareolar
This approach typically results in a well-concealed scar within the interface of the nipple-areola complex (NAC) and the breast skin. However, a hypertrophic scar in this location is very unsightly and can be difficult to correct. A nipple diameter of at least 3.5 cm is required for adequate access. The contamination theory suggests a higher rate of capsular contracture through this approach due to bacteria present within the breast ductules. 27 , 28
32.5.3 Transaxillary
This approach completely avoids the potential for placing a scar on the breast. However, it is the least versatile of the recommended approaches and is furthest from the pocket. In general, only saline implants in the subpectoral pocket are recommended with this approach. Silicone gel implants and the subglandular plane may also be used but this is technically more challenging. With this approach, the utilization of an endoscope results in greatly enhanced visualization. 29
32.5.4 Transumbilical
This approach is restricted to inflatable saline devices and because of the blind nature of this dissection and imprecise pocket creation, it is not recommended by the authors in any situation.
32.6 Pocket Location
32.6.1 Subglandular
This pocket provides both good projection and shape, and minimizes distortion of the implant in muscular or active patients. This pocket may also provide a small degree of lift in breasts with mild ptosis and volume deflation. Utilization of this pocket requires at least 2 cm of upper pole soft tissue coverage as determined by pinch test. Drawbacks of this pocket include a potentially higher capsular contracture rate, more implant edge palpability, greater visible rippling or implant visibility, and an increased degree of mammography interference. 1 , 15
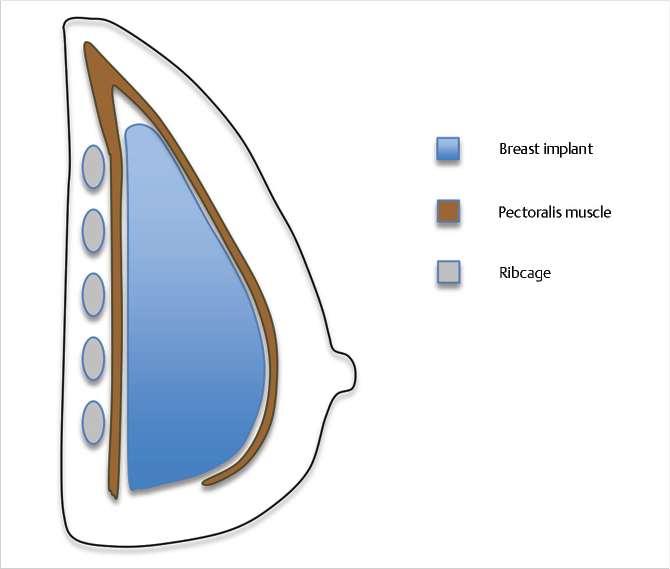
32.6.2 Subpectoral
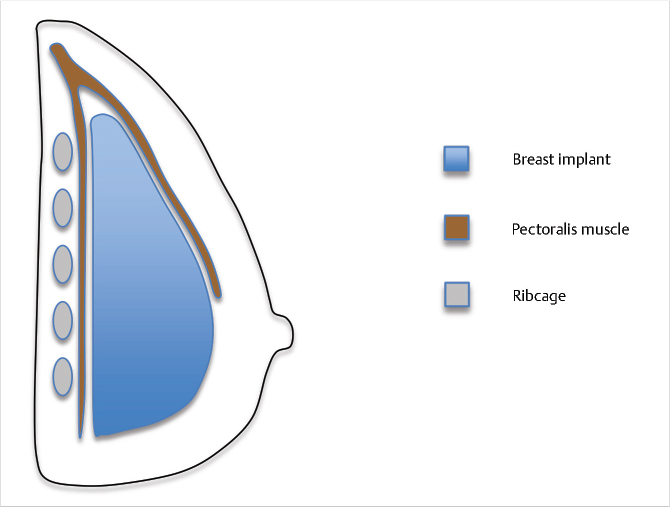
This pocket provides the thickest soft tissue coverage, lower capsular contracture rates, 1 , 15 and minimizes implant visibility and palpability. However, there is less upper pole projection when compared to the subglandular plane, and the upper pole projection is more challenging to control. Additional drawbacks of this pocket are related to the overlying pectoralis major, which may distort the implant with activity (animation deformity) and can also cause lateral displacement of the implant over time, resulting in a wider cleavage, or intermammary distance particularly when the patient lies down. A double bubble deformity where the breast tissue migrates inferiorly over the fixed implant is also more common when this pocket is utilized. Finally, muscle spasm should be anticipated and a pretreatment of such spasm should be considered.
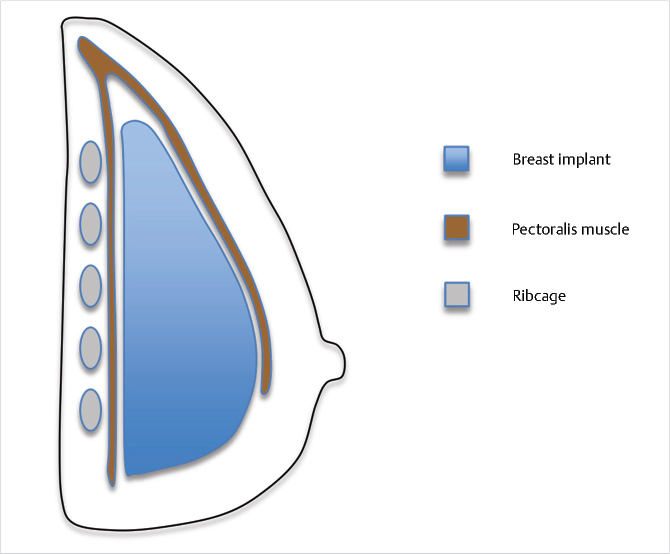
32.6.3 Biplanar (Dual Plane)
This approach allows for upper pole coverage by the pectoralis major with varying amounts of lower pole coverage by the breast parenchyma. Division of the origins of the pectoralis at the IMF allows for retraction of a portion of the pectoralis, with a resultant direct exposure of the implant surface to the breast parenchyma along the lower pole of the implant. This allows for the implant to rest at the IMF, thus expanding the lower pole and potentially improving breast ptosis.
Dual Plane I
This involves division of the pectoralis major origins along the IMF. No additional separation of the breast parenchyma and underlying pectoralis fascia is performed. The subpectoral space is then dissected for implant placement. This is the approach performed by our practice in most subpectoral breast augmentations (see surgical technique below).
Dual Plane II
In addition to the release of the pectoralis and creation of the subpectoral pocket as described in dual plane I, the breast parenchyma is released from the underlying pectoralis fascia to the level of the inferior border of the NAC. This is our group’s preferred approach in patients with mild ptosis that do not want a concurrent mastopexy.
Dual Plane III
This approach follows that of dual plane II but involves continued release of the breast parenchyma to the level of the superior border of the NAC. This maximizes the amount of parenchymal coverage of the implant while still providing additional soft-tissue muscle coverage of the upper pole (Fig. 32‑2).
32.6.4 Preoperative Patient Counseling
In addition to the normal risks of surgery (bleeding, infection, damage to nearby structures), additional considerations that should be routinely discussed include the potential for scarring, loss of nipple sensation, implant rippling, implant rupture, blocking of breast tissue on mammography, animation deformity (with submuscular pocket selection), capsular contracture or pocket malposition requiring further surgery and cost, and development of anaplastic large cell lymphoma (ALCL) at a rate of 1/200,000. 30 The current FDA recommendations for MRI surveillance should also be mentioned in patients undergoing breast augmentation with silicone gel implants and it should be noted that these costs are rarely covered by insurance. The published data regarding rupture and reoperation rates over a 10-year period of approximately 8 and 36%, respectively, is quoted. 31 No guarantees on results or cup size are implied or given.
32.7 Treatment
32.7.1 Surgical Technique: General
In all situations, the patient is initially given prophylactic antibiotics and appropriate deep venous thrombosis prophylaxis measures are taken. The patient is then prepped and draped in the usual sterile fashion with the upper extremities secured to arm boards at 90 degrees to the thorax. The planned incision is then marked and carried out in the manner selected as described below. Dissection of a precise pocket under direct visualization, while maintaining meticulous hemostasis, is aided with the utilization of a lighted retractor and/or endoscope depending on the desired approach. Early in one’s career, an exact implant sizer can be utilized to verify the pocket size and positioning. After the implant pocket has been appropriately created, the permanent implant and pocket are then irrigated with an antibiotic solution (50,000 units of bacitracin, 1 g cefazolin, and 80 mg gentamycin in 500 mL of normal saline). The pocket is again visualized to ensure hemostasis. All visible blood is copiously irrigated, after which the implants are inserted utilizing a no-touch technique. Although not utilized in our practice, a funnel device can aid in the placement of silicone implants. The patient is then brought into an upright sitting position to verify symmetry and implant position. When the surgeon is satisfied with the result, the patient is returned to the supine position and a meticulous layered closure is performed. We prefer to utilize chromic suture to close both the implant pocket and the deep dermis, in simple interrupted and buried interrupted fashion, respectively. The epidermis is then re-approximated with a subcuticular Monocryl suture. Surgical skin adhesive is applied. A 6-inch ACE wrap is then utilized to provide gentle but firm circumferential support. The details regarding incision and pocket location are detailed below.
32.7.2 Inframammary Approach
The incision is planned in the projected inframammary crease, with the majority of the incision placed lateral to a line projected down from the nipple. The incision length is usually 4.5 to 6 cm in length, depending upon the implant type and size. The incision is made and carried down until the prepectoral fascia is identified. If a subglandular pocket has been chosen, this is the plane of pocket dissection. If a subpectoral pocket has been chosen, dissection is then carried laterally to identify the lateral border of the pectoralis major. The plane beneath the pectoralis is then entered. The subpectoral pocket is then created from the lateral to medial direction. Only the inferior most attachments of the pectoralis to the ribs are divided using electrocautery. The methods of pocket creation, irrigation, implant placement, and closure as detailed above are followed.
32.7.3 Periareolar Approach
The incision is planned from the 3 o’clock to the 9 o’clock position on the inferior half of the areola at the junction of the areola and the breast skin. The dissection proceeds in a vertical direction directly through the breast tissue until the prepectoral fascia is encountered. Alternatively, some surgeons, although not our preference, create an inferiorly based breast skin flap, separating it from the parenchyma, providing access to the pectoral fascia along the inframammary fold. Again, if a subglandular pocket has been chosen, this is the plane of pocket dissection. If a subpectoral pocket has been chosen, the dissection proceeds in a more oblique fashion, and angled inferiorly until the prepectoral fascia is identified. Dissection is then carried laterally to identify the lateral border of the pectoralis major. The subpectoral pocket is then created from the lateral to medial direction. Only the inferior most origins of the pectoralis major to the ribs are divided using electrocautery. The sternal origins of the pectoralis major are not disrupted. The methods of pocket creation, irrigation, implant placement, and closure as detailed above are followed.
32.7.4 Transaxillary Approach
The incision is planned in the lower pole of the hair bearing skin of the axilla within the most anterior skin crease. This incision is then deepened bluntly to identify the lateral border of the pectoralis major. Blunt digital dissection is then utilized to develop a plane between the pectoralis major and pectoralis minor. The methods of pocket creation, irrigation, implant placement, and closure as detailed above are followed. With this approach, utilization of an endoscope can greatly enhance visualization and allow more precise dissection of the subpectoral and even the subglandular pockets.
32.7.5 Alterations in Technique for Tuberous Breast
In order to treat this challenging problem, we prefer to use the subglandular pocket as described above. Utilization of this pocket allows for release of the constricting bands between the pectoralis major and the breast parenchyma. Radial scoring of the breast parenchyma is performed with a resultant release of constricted tissue and a widening of the breast base. A periareolar mastopexy is then performed on both breasts to ensure symmetrical scarring. Finally, a saline filled implant is utilized for greater intraoperative adjustability and correction of asymmetry (Table 32‑1). (See Chapter 37 for greater details on the tuberous breast condition as well as surgical treatment.)
32.8 Postoperative Care
Dressings involve minimal use of tape to avoid skin irritation. Closed incisions are covered with surgical skin adhesive. A 6-inch ACE bandage is then wrapped circumferentially around the patient’s chest to provide some gentle compression in order to help position the implant, control edema, and decrease the risk of hematoma. This is left in place for 24 hours and then changed to a sports bra.
The patient is kept in the post anesthesia care unit until discharge qualifications are met. She is instructed to leave the dressings in place. Most patients are given oral narcotic pain medications and an empiric 7-day course of oral antibiotics to cover skin flora. 32
The patient follows up in clinic on postoperative day 1. Her dressings are removed and the patient is examined for the development of a hematoma. If her breasts are nontender, she is assisted into a sports bra. The patient is instructed to wear this bra and avoid breast manipulation for 2 weeks. The patient is told to return to light activity as tolerated, and back to full duty at 2 weeks.
She is seen again in clinic 2 weeks postoperatively. At this point, she is instructed on scar care. She is told to begin scar massage 3 weeks postoperatively with an over-the-counter scar cream, and to wear silicone sheeting as much as possible. Implant massage is not recommended by our group, although others advocate it, particularly in subpectoral or dual-plane implants. 26 Postoperative photographs are taken at 3 months and 1 year. With silicone implants, an MRI may be performed at 1 year to establish a baseline, and the FDA recommends a screening MRI to assess for silent implant rupture at 3 years followed by subsequent imaging studies every 2 years. 21
32.9 Outcomes and Complications
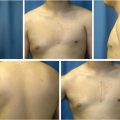
Patient satisfaction is generally excellent following breast augmentation, even if there is a need for further surgery (Fig. 32‑8, Fig. 32‑9). Patients have reported an improved body image, overall sense of well-being, and specifically improved satisfaction with breast appearance as well as psychosocial and sexual well-being. 33 , 34 , 35
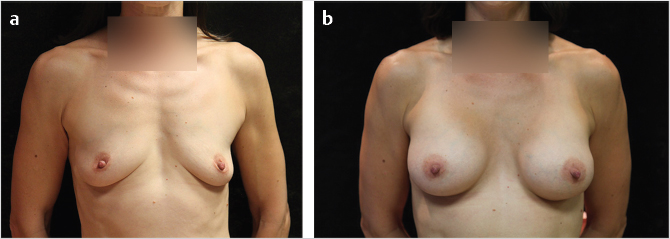
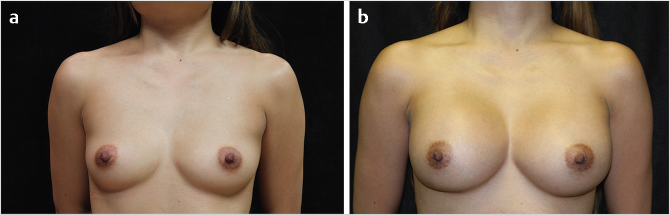
Acute complications are often self-limiting. Alterations in nipple sensitivity are common, but resolve over time in most patients. 36 , 37 , 38 If a patient presents with a wound infection, an ultrasound may be used to assess for a periprosthetic fluid collection. Simple wound infections with no or minimal periprosthetic fluid will generally respond to oral antibiotics if initiated early. If the infection is severe, does not resolve, or recurs, it should be treated with explantation. 39 , 40 Hematomas occur in about 1% of patients and must be evacuated if they are large or expanding. 41 , 42 Mondor’s disease is a superficial thrombophlebitis of the breast that may be treated with NSAIDs and warm compresses. 43 Wound breakdown leading to implant exposure must be treated with explantation. 39 , 40
The reoperation rate in our practice is similar to the published rate of 25%. 34 The most common indication for reoperation is capsular contracture, which generally occurs in the first year post operatively. 12 , 37 , 44 , 45 , 46 As discussed previously, the rate of occurrence is dependent upon implant type and pocket choice. 47 Additionally, bacterial contamination leading to biofilm production around the implant is thought to be a major driving force in the etiology of capsular contracture. 48 , 49 Factors that have been found to reduce the risk of capsular contracture are the use of an inframammary incision, textured implants, subpectoral placement, and antibiotic irrigation; conversely, hematoma, seroma, infection, smooth implants, and subglandular implant placement increase the risk of capsular contracture. 1 , 20 , 26 , 32 , 43 , 47 , 50
32.9.1 The Baker Classification and Grades of Capsular Contracture
Baker grade I and II capsular contractures generally require no intervention, whereas grade III or IV contracture should be treated operatively (Table 32‑2). 51
The gold standard for treatment of capsular contracture is total capsulectomy with implant removal. A position or “site” change is generally recommended, particularly if the original implant was placed subglandular. A subpectoral or dual plane pocket is preferred. 52 , 53 Due to the technical difficulties in performing a total capsulectomy, the authors have investigated other strategies such as anterior capsulectomies or leaving the capsule intact and creating a new supra- or subcapsular pocket; however, these techniques have not been proven to be as effective as total capsulectomy in preventing recurrence of capsular contracture. 9 , 54 Acellular dermal matrices are increasingly being used in the treatment of capsular contracture and are showing promise in preventing recurrence, although all studies are compared to historical cohorts. 55 , 56 , 57
Other significant complications are less commonly encountered. Visible implant rippling may be seen, particularly if the implant is too large. Dynamic distortion may occur during pectoralis muscle activation with a submuscular implant. Implant malposition may also occur and can be noted by lateral displacement, symmastia, or an inframammary fold that is too high or too low. If the malposition is minor, the implant may be massaged or compressed in the correct direction. However, these deformities may need to be corrected with pocket change, capsulorrhaphy, or biologic mesh placement. 58 , 59 , 60
Another possible complication is implant rupture. If it is a saline implant, the rupture will be noticeable due to resorption of the saline, and the implant should be explanted and replanted. In silicone implants, if the rupture is symptomatic or extracapsular, the implant should be removed. Significant benefits of removing an asymptomatic, intracapsular leaking silicone implant have not been proven. 61 , 62 However, if the patient requests removal in this situation, it is our practice to remove the implant.
In addition, there have been rare cases of ALCL reported in association with breast implants, with the vast majority associated with textured implants. 30 , 63 , 64 This typically presents as a late periprosthetic fluid accumulation. Any patient with a late appearing seroma should at least have fluid aspirated and sent for cytologic analysis. 65
Fortunately, complications of breast augmentation are well tolerated and patient satisfaction is high, making breast augmentation a rewarding procedure for both surgeon and patient.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree