Abstract
This chapter surveys the types of mastopexy and augmentation-mastopexy procedures. Ptosis refers to the descent of the breast due to various factors (aging, weight loss, pregnancies, etc.) and mastopexy refers to the treatments meant to correct ptosis. Patients are evaluated according to Regnault’s classification of ptosis and surgical treatment is determined. The authors provide detailed information in the text and table format regarding the desired outcome for each degree (minor, moderate, major) of ptosis. The advantages and disadvantages of mastopexy techniques (crescent, concentric circumareolar, vertical, etc.) are thoroughly discussed. Augmentation-mastopexy augmentation techniques are also covered. The chapter concludes with guidelines for postoperative care and a listing of anticipated outcomes and possible complications.
31 Mastopexy
31.1 Goals and Objectives
Understand the proper evaluation of patients with breast ptosis.
Clearly define the indications for the various types of mastopexy and augmentation–mastopexy procedures.
Appreciate the technical aspects of skin and parenchymal management in mastopexy and augmentation–mastopexy procedures.
Know the advantages and disadvantages of each technique and their complications.
Understand the postoperative management of mastopexy and augmentation–mastopexy.
31.2 Patient Presentation
The breast is an important organ to a woman, and it remains the central focus of femininity and the source of attraction. It has been depicted throughout centuries as the source of sensuality and perfection. Nature shapes the breasts in each individual, but the shape often changes due to aging, lifestyle, injury, or congenital deformity. In Greek, ptosis means “falling” and describes the descent of breast parenchyma, which is managed by mastopexy. In Greek, mastos means “breast,” pexy means “fixation,” and it involves a series of principles and techniques to correct breast ptosis. It is essential for the plastic surgeon to know the hallmarks of the youthful breast, and identify those techniques that are most likely to restore the breast to its optimal aesthetic form in a given patient. This chapter presents a comprehensive review of the evolution and principles of the management of the ptotic breast by means of mastopexy or augmentation–mastopexy.
According to the American Society of Plastic Surgeons (ASPS) statistics report, more than 92,000 mastopexies were performed in 2014 (75% increase from 2000), and was ranked the seventh most common aesthetic surgical procedure in the United States. 1 A similar trend is reflected in the American Society for Aesthetic Plastic Surgeons (ASAPS) national statistical data, which indicate that mastopexy was ranked the sixth most common aesthetic surgical procedure. The majority of patients were between the ages of 35 and 50 years, and returned to work within 1 to 2 weeks postoperatively. 2
Geographical variation of the published mastopexy techniques exists. It appears that North American surgeons use the inverted T incision and inferior pedicle more frequently, use fascial sutures less often, and usually do not incorporate “auto” augmentation in their procedures. Conversely, Latin American and European surgeons prefer the vertical incision and superior pedicles, and use fascial sutures and “auto” augmentation more often. 3
31.2.1 Etiology
Ptosis results when breast parenchymal volume is relatively deficient within the larger skin envelope. Factors found to have a statistically significant correlation with ptosis include advanced age, history of significant weight loss, high body mass index (BMI), large bra cup size, greater number of pregnancies, and smoking history. 4
With age, the breast assumes a lower position on the chest wall becoming ptotic and losing the youthful breast contour. Factors that may play a role include glandular hormonal regression, atrophy, gravity, and loss of skin elasticity. This leads to stretching and lengthening of skin and glandular attachments. As glandular tissue settles, the upper pole of the breast loses its fullness and appears deflated. 4 Breast ptosis is a very common in post-bariatric patients who have undergone massive weight loss. Studies have shown that weight loss is an issue if greater than 50 lb is lost. 4 High BMI and large bra cup size (breast weight > 400 g) have been shown to be predisposing factors, most likely because of the increased pull caused by gravity on heavier breasts. 4 Although pregnancy per se was not found to predispose to breast ptosis, an increase in the number of pregnancies does. The reason is uncertain, but weight gain during pregnancy was not found to be associated with ptosis. 4 Smoking has been shown in experimental and clinical studies to impair the production of collagen and increase the production of tropoelastin and matrix metalloproteinases. These cause an abnormal deposition of elastotic material and degradation of collagen, elastic fibers, and proteoglycans, leading to dermal connective tissue degenerative changes, wrinkling, and loss of skin elasticity and tone. 5 Breast-feeding is widely held accountable for breast ptosis and has been shown to be a reason for early termination of breast-feeding. 6 This is a significant misconception, as there is no evidence to support this hypothesis. 4 Another misconception is the role of regular upper body exercise to reduce the risk of ptosis. No evidence exists to support this argument. 4 Other factors mentioned in the literature as predisposing factors for ptosis include congenital deformities such as tubular breasts, thin skin, excessive breast size, and postoperative changes.
31.2.2 Classification of Ptosis
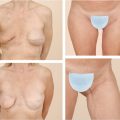
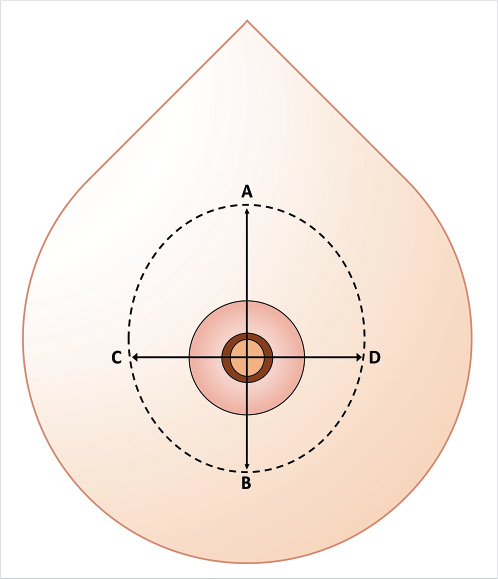
The youthful breast is positioned between the third and sixth intercostal spaces, with the inframammary fold located at the level of the fourth to fifth intercostal space, with a full rounded lower pole contour, a lateral outward convexity that covers the rib cage as it sweeps toward the axilla becoming concave, and a nipple–areola complex (NAC) positioned directly at the point of maximal projection. Several classifications have been introduced to define the degree of ptosis; however, Regnault’s classification remains the most widely employed. 7 The degree of ptosis is based on the position of the nipple in relation to the inframammary fold and the gland. Breast ptosis is classified as pseudoptosis, glandular or “partial” ptosis, and three degrees of true ptosis (Fig. 31‑1; Table 31‑1). 7
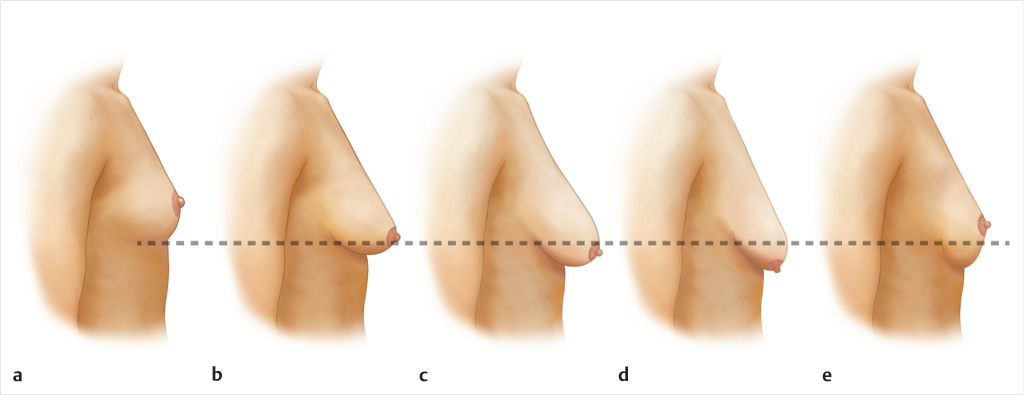
The terms “pseudoptosis” and “glandular ptosis” to this day are often used incorrectly interchangeably. “Pseudoptosis” describes a breast that is hypoplastic, with a loose skin envelope and the nipple lying above the inframammary fold; this combination of factors results in an appearance similar to the one of minor ptosis, and can be resolved by increasing breast volume (e.g., inserting an implant). “Glandular ptosis” was referred by Regnault as “partial ptosis,” and also presents with the nipple above the inframammary fold, but the gland and skin brassiere follow the influence of gravity; this results in the lower portion of the skin brassiere to be elongated, while the upper portion to remain the same length. 7
31.2.3 Patient Evaluation
A thorough history and physical examination is the basis for a successful surgical strategy. Evaluation of the patient’s preoperative medical status must include conditions that can affect the shape and size of the breast (such as breast disease, significant weight gain followed by weight loss, previous breast surgery or biopsies); family history of breast cancer; details of recent mammograms; reproductive history including number of pregnancies, breast-feeding history, and plans for future children.
Examination requires a careful and systematic evaluation of each breast, and includes a detailed visual analysis and thorough palpation. The visual inspection is performed to evaluate the shape, symmetry, contours, skin quality, scars, breast volume, along with the NAC shape, position relative to the inframammary fold, and amount of breast overhanging the inframammary fold. Careful notes are made regarding symmetry of contour, NAC position, presence of striae, and overall skin quality. Additionally, the presence, size, and location of contour deformities are recorded and pointed out to the patient preoperatively. Surface measurements from key breast anatomic points noted above are recorded in the patient’s chart. This includes a bio-dimensional analysis of topographic landmarks including supra-sternal notch to nipple distance, breast base width, nipple to inframammary fold distance at rest and on stretch and pinch thickness of the upper and lower poles of the breast.
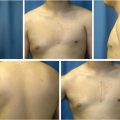
Tactile examination includes careful palpation of the skin and breast parenchyma, looking for masses, tenderness, areas of thickening, scar adherence, glandular mobility, along with parenchymal and skin elasticity. The parenchyma is also assessed for volume, position, distribution, and elasticity. Pinching the lower pole or lateral inferior pole of the breast mound can simulate the superior transposition of the parenchyma. The ability to simulate a favorable upper pole shape change this way suggests that the patient is a good candidate for vertical mastopexy (Fig. 31‑2). On the other hand, the lack of breast shape change with this maneuver suggests that the patient is more likely to benefit from a mastopexy with a combination of vertical and horizontal skin excision, or a mastopexy, which includes the placement of an implant.
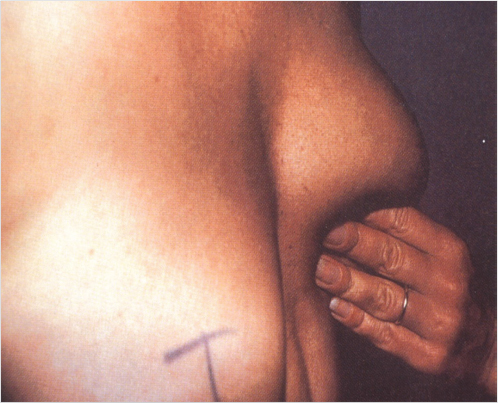
Each patient presents with preconceived ideas of an ideal breast appearance. Sometimes they already have a shape in mind and may attempt to explain or show it by adjusting the contour of their breast with their hands. For this reason, it is vitally important for the plastic surgeon to understand the patient’s primary concerns and goals. The patient’s expectations must be realistic and she must understand that the surgery will result in permanent scars on the breasts. Once the breasts have been accurately assessed and classified, an honest discussion is undertaken with the patient regarding the various elements of her deformity, the recommended treatment, limitations and complications of operative intervention, and appropriate expectations regarding outcome.
31.3 Preparation for Surgery
Preoperative radiological or laboratory evaluation in preparation for surgery is similar to other major elective procedures and would be dependent on the patient’s age and comorbidities. Patients who are of menstruating age must have a urine HCG. Blood work is not routine but directed by significant medical conditions.
Preoperative mammogram is routinely ordered by the senior author (KCS) in patients aged 40 years and over, and in patients aged 30 years with a family history of breast cancer or previous breast tissue diagnosis. The mammogram is used as a baseline study for future mammograms.
Anteroposterior, lateral, and oblique photographs are taken in the upright position in a uniform way, using the same background color, lighting conditions, and patient position. If certain areas of the breasts are of particular interest, other views are taken including photographs from above, below, or in the supine position.
31.4 Treatment
Mastopexy entails breast reshaping and varying degrees of nipple elevation in the context of using the most appropriate incisions. Many algorithms have been introduced to guide surgeons on the best approach according to the degree of ptosis. 7 , 8 , 9 , 10 However, no ideal technique has been identified and the shortest scar procedure may not necessarily be the most appropriate in all patients. Each patient requires an individually tailored surgical plan as the surgeon needs to consider the incision pattern, need for tissue rearrangement, parenchymal fixation, or implant placement as dictated by his/her analysis described above. There are three basic incision patterns, with several variations, and the most commonly used techniques are described below.
The degree of ptosis is one of the factors to guide the choice of the surgical approach to be used. Additionally, the patient’s preference, aesthetic breast evaluation, careful parenchymal and skin elasticity assessment, and the surgeon’s experience and level of comfort all influence the surgical choice. The trend is toward using minimal incision patterns but ultimate selection of incisional technique is best guided by the Regnault classification. Table 31‑2 provides a guideline to the surgical approach of ptotic breasts.
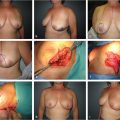
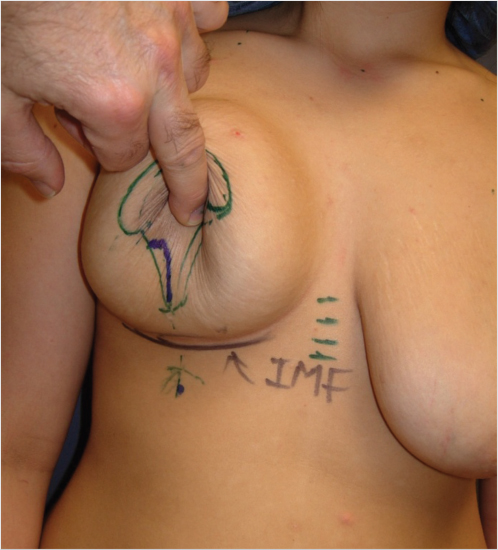
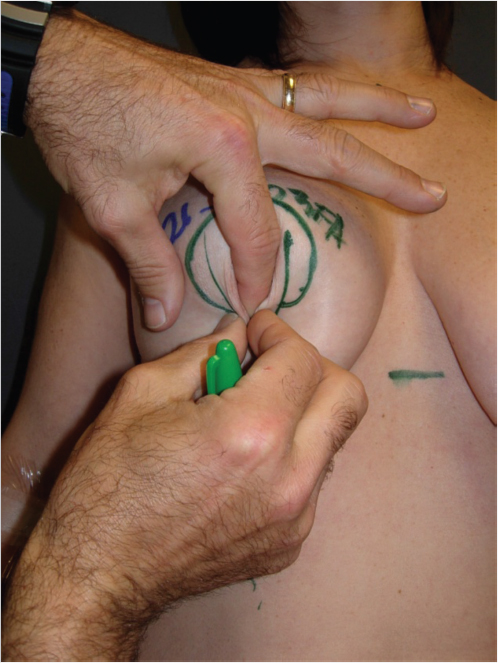
Important technical maneuvers for all mastopexy procedures done without an implant begin with skin marking. This is done with the patient in the standing position. Most importantly these include establishing new nipple position, which will correspond to the newly created maximal projecting portion of the breast as created by movement of breast tissue to the upper pole. As such the new position for the nipple will most often be above the inframammary fold, especially if an implant will be used concomitantly. This may be anywhere from 1 to 4 cm above the inframammary fold in the upright position (Fig. 31‑3). In addition, determining the approximate skin resection area (in the periareolar, vertical, and horizontal orientations if necessary) can often be fairly accurately estimated preoperatively by gentle digital manipulation of the tissues (Fig. 31‑4).
The plan and operative technique must include
Flexibility—Preoperative planning is important but it is presumptive and not definitive; the surgeon must develop the ability to intraoperatively alter incision design and nipple position using tailor-tacking.
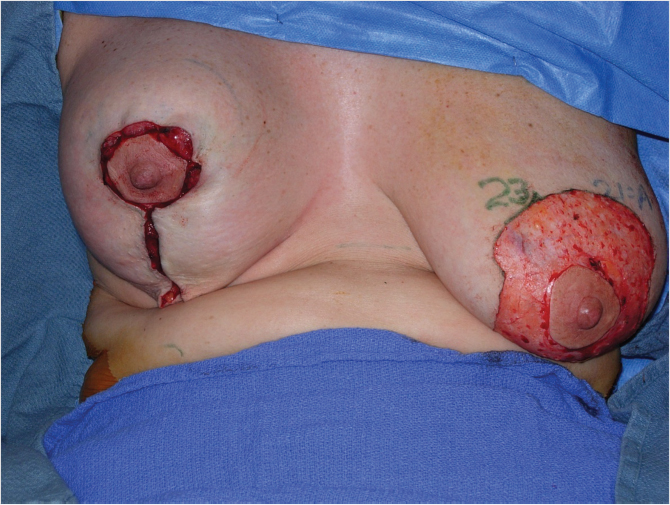
Tailor-tacking—skin sutures or skin stapling to simulate changes in breast shape which occur with skin tightening or plication (Fig. 31‑5).
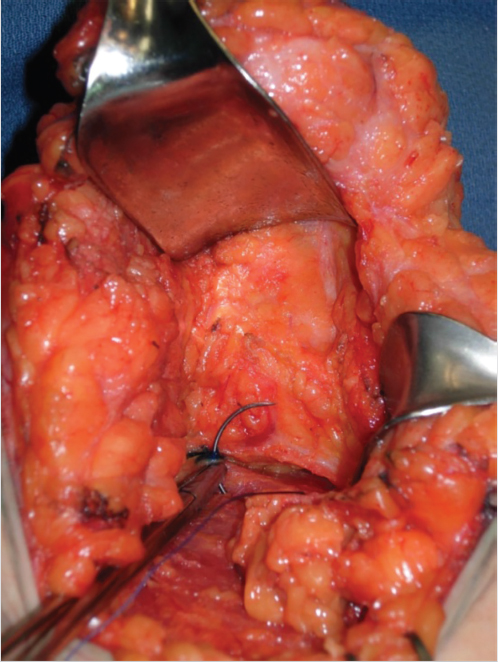
Parenchymal suturing—performed in almost every case. This includes pedicle fixation by “pexy sutures” to pectoralis major muscle fascia, suturing de-epithelialized dermal wings, and lower breast pillar sutures in case of vertical mastopexy (Fig. 31‑6).
The insertion of an implant has various effects on the shape of the breast and NAC including increase in upper pole fullness and breast projection, widening of areola, and change in upper pole contour from linear (preoperatively) to slightly outwardly convex (postoperatively). 11 However, it must be kept in mind that the breast mound is only minimally elevated (less than 1 cm), the lower pole expands and may stretch slightly, and although the actual NAC position is not changed, the changes produced by the implant produces an illusion that it is elevated. 11 Therefore, augmentation alone should be reserved for selected patients where the main complaint is a deflated breast with inadequate volume and minimal inferior displacement of the NAC. Spear advocates augmentation alone if less than 2 cm of breast overhangs the fold, the nipple is appropriately positioned on the anterior surface of the breast, non-pigmented skin is visible between the lower areola and the inferior border of the breast, and the nipple to inframammary fold distance is less than 9 cm. 12 In some of these patients, a periareolar excision of skin (periareolar mastopexy) can elevate the NAC 1 to 2 cm and may enhance the result.
A combined augmentation and mastopexy approach to treat deflated and ptotic breasts can either be performed as a one-stage or two-stage procedure. The one-stage procedure was first described in the 1960s by Gonzalez-Ulloa. 13 Since then multiple plastic surgeons have shared their outcomes and opinions on a one-stage procedure, leading to a controversial debate on its reliability and relative safety. 14 , 15 , 16 , 17 , 18 One-stage procedures are challenging because augmentation and mastopexy work against each other, producing diametrically opposed effects on the breast tissue and skin envelope, at times potentially altering the blood supply to the NAC and skin flaps, and always placing greater tension on the closure. Mastopexy repositions the nipple, reshapes the breast with some element of tension in the line of closure with a reduction of the redundant skin envelope. On the other hand, augmentation expands the breast, increases the size of the skin envelope, and increases the tension of wound closure. Furthermore, augmentation introduces potential implant-related complications such as capsular contracture, potential lower pole stretch, and possible inferior or lateral implant malposition. These possible untoward sequelae must be explained to the patient preoperatively.
Patient selection is key for a successful one-stage augmentation–mastopexy and the decision is based on the patient’s preoperative breast evaluation, tissue condition, and suitability to the procedure along with the surgeon’s experience and level of comfort with this plan. Favorable characteristics include first and second degree ptosis; using a small implant (less than 300 mL); nipple elevation less than 4 cm; light toned skin with good elasticity; and absence of peri-operative risks (e.g., obesity, smoking history, and massive weight loss). The main indication of a one-stage augmentation–mastopexy includes ptosis combined with significant volume deficiency. Depending on the degree of ptosis, a periareolar, vertical, or inverted T technique can be used. The choice of implant size is an important part of planning regardless of the chosen technique, and depends on the preoperative characteristics of the breast. The larger the implant, the less aggressive the skin excision is. Deflated pendulous breasts require an implant whose diameter matches the base diameter of the breast, and often ptotic breast tissue in the lower pole must be excised in the so called plus/minus mastopexy. Constricted or tuberous breasts almost always require implants with a diameter that exceeds the original breast base width. For this reason, mastopexy must be very conservative in these patients. No evidence exists on the specific association of complication rates and the implant type or pocket used in one-stage augmentation–mastopexy. However, most studies indicate a higher use of silicone implants (up to 75% of cases) placed in a dual submuscular plane (up to 96% of cases). 14 , 15 , 16
The senior author and most experienced surgeons believe that the smallest implant that will provide volume meeting the patient’s expectations should be used. It is generally felt by most authors that insertion of the implant is done prior to mastopexy because increased volume within the breast conferred by the implant results in less ptosis and correspondingly less skin that needs to be excised. 19
However, some patients may present a very high risk for a one-stage augmentation–mastopexy, especially in patients displaying the following unfavorable characteristics: extreme third-degree ptosis; heavy breasts with more than 4 cm of tissue overhanging the inframammary fold; required implant volume greater than 400 mL; nipple elevation greater than 6 cm; poor skin quality or pronounced striae; patients with BMI greater than 35; massive weight loss; extreme asymmetry; medially displaced NACs; and perioperative risks such as smoking history. 20 It is the senior author’s (KCS) opinion that patients considered for a for a two-stage augmentation–mastopexy first undergo a mastopexy and subsequently have an implant placed, if still desired, 4 to 6 months later. Other than the safety benefit, a two-stage augmentation–mastopexy allows the patient to evaluate the appearance of her breasts after mastopexy. If satisfied with the result, the patient may opt to forgo breast augmentation.
Important technical pearls in augmentation–mastopexy:
Using the smallest implant that will satisfy patient expectations.
Placing the implant first usually through an incision that will be incorporated in the mastopexy plan.
Planning for conservative skin resection and on-table adjustment with tailor-tacking with the patient sitting at 90 degrees.
Nipple elevation and final nipple position guided by presumptive preoperative planning and tailor-tacking to be repositioned 2–5 cm (most commonly 3–4 cm) above the inframammary fold, since the implant adds significant fullness to the upper pole of the breast.
31.4.1 Techniques in Mastopexy
A variety of mastopexy techniques have been described. This section provides an overview of the three basic incision patterns (periareolar, vertical, and inverted T) and the techniques used to manage the underlying breast parenchyma.
Periareolar Mastopexy
Crescent Mastopexy
Indications
Rarely indicated and it is mainly used to address upper areola level asymmetry.
Technique
Crescent mastopexy was originally described by Puckett as an eccentric circumareolar skin excision without NAC mobilization nor purse-string suture. 21 A crescent-shaped incision is made around the upper half of the areola, down to the reticular dermis. A wedge of de-epithelialized skin is excised to mobilize the NAC up to 2 cm but most commonly much less. The incision can be as extensive as needed (it can almost resemble a circumareolar shape) depending on the degree of breast ptosis, and the NAC’s diameter and circumference. The orientation of the incision can help reshape or reposition the NAC as needed including superior lifting, medial or lateral shifting, inferior repositioning, reduction, or a combination of the above.
Advantages and Disadvantages
The main advantage includes the very short scar that can be camouflaged by the border of the areola. The main disadvantage of this technique is that the force applied to the areola along the vertical axis, can result in an oval-shaped or elongated areola, which frequently results in a suboptimal aesthetic result.
Concentric Circumareolar Mastopexy
Indications
First- and early second-degree ptosis, large areolar diameter, and tuberous breasts.
Technique
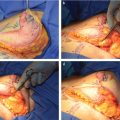
Benelli introduced the “round block” technique in 1990. 22 The technique begins by marking an outer ring that defines the outer border of the de-epithelialization area. This ring joins the superior and inferior borders of the new NAC, and varies depending on the amount of excess skin. The new areolar circumference (approximately 4 cm in diameter depending on breast size) is then drawn using an areolar sizer, which defines the inner border of the de-epithelialization area (Fig. 31‑7). The redundant skin found between these two markings is excised to reposition the NAC. The skin is then undermined to expose the parenchyma, which is then incised leaving the NAC on a superior pedicle. Depending on the degree of ptosis, the management of the parenchyma differs. For mild degree of ptosis the base of the breast is simply plicated and invaginated. Whereas for more severe ptosis, medial and lateral parenchymal flaps are created and overlapped to provide breast width narrowing, and breast shape lifting and coning. The periareolar incision is then closed in a purse-string fashion with non-absorbable sutures, which allows a reduction in scar tension as described by Benelli. 22 An excellent variation of this technique is described by Goes, which includes the use of a prosthetic mesh layer to support the breast parenchyma. 23 or the use of implants to minimize the skin resection required. 9 , 17 It is important that the surgeon not excise too much skin as the quality of the aesthetic result depends on breast parenchymal re-shaping with subsequent skin redraping.
Advantages and Disadvantages
The circumareolar mastopexy is more versatile than the crescentic approach and generally provides better aesthetic outcomes. The circumareolar scar can be camouflaged at the border of the areola. The main disadvantages include flattening of the anterior contour of the breast mound and recurrence of ptosis. 8 , 10 , 22 , 24 Benelli notes that this circumareolar technique is not suitable for all breasts and that shape correction must be sacrificed in favor of a reduced scar. 22 It must be emphasized that the learning curve with this procedure is steep.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree