24 Classification and Analysis of the Breast-Conserving Therapy Deformity
Ideally, BCT should result in a breast with a normal appearance, without any major asymmetry or deformity. Unfortunately this is not always the case and subsequent deformities are not uncommon. An estimated 20% to 40% of women who undergo BCT have a residual deformity or breast asymmetry. 1 – 3 Some of these patients are referred to a plastic surgeon for reconstruction to improve the appearance of the treated breast; such reconstruction may take place many years after the initial treatment is completed. 4 A growing number of plastic surgeons are faced with requests for the correction of complex sequelae of BCT; these surgeons also face the technical problems related to managing an irradiated breast.
In 1998 and 2004, we published a classification of cosmetic sequelae after conservative treatment based on two series of patients. 5 , 6 This classification was proposed as a guide to help surgeons identify cosmetic sequelae and to plan reconstruction.
Patients and Methods
BCT protocols can be schematically classified into two groups. The first group includes patients with small tumors (less than 3 to 4 cm), treated with BCS and postoperative radiotherapy, with or without adjuvant therapy (chemotherapy and endocrine therapy). 7 – 9 The second group comprises patients with larger tumors, treated with preoperative therapy (chemotherapy, endocrine therapy, or even radiotherapy, separately or in combination) to reduce the tumor volume and to allow BCS in patients responding to this treatment. 10 In all BCT patients, the combination of conservative surgery and radiotherapy can induce both skin and glandular sequelae. Various combinations of these sequelae are observed, and the possible asymmetry with the untreated breast always presents a complex problem for the plastic surgeon. We classify these cosmetic sequelae into the following three types to simplify the surgical approach. 5 , 6
Type 1 Cosmetic Sequelae
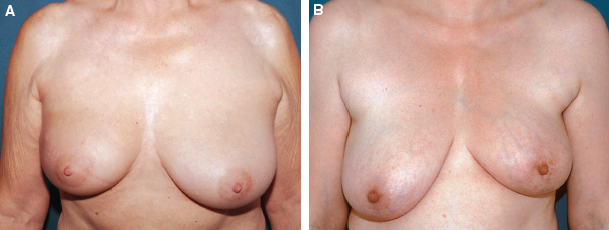
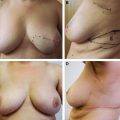
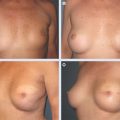
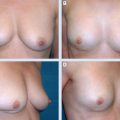
The overall shape of the treated breast is maintained, because there is no deformity. The major abnormality is an asymmetry in the shape and volume between the two breasts (A and B), which can be repaired by conserving the irradiated breast and symmetrizing the contralateral breast.
Type 2 Cosmetic Sequelae
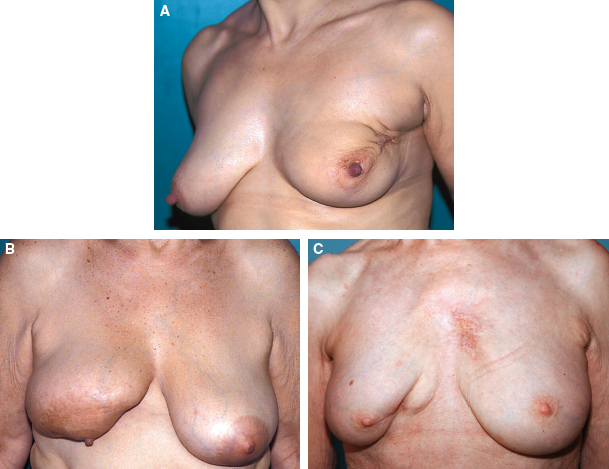
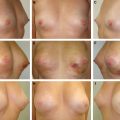
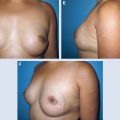
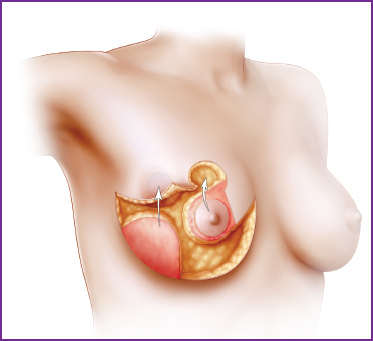
There is an obvious deformity of the treated breast associated with breast asymmetry, often resulting from the resection of an upper outer quadrant tumor (A), a lower quadrant tumor (B), or an inner quadrant tumor (C). A mastectomy is not required. For these patients, reconstruction is compatible with breast conservation.
Type 3 Cosmetic Sequelae
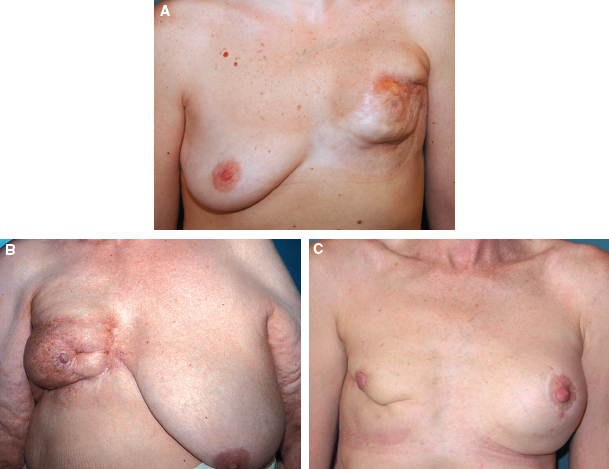
There is a massive retractile fibrosis of the entire breast (also called marble breast) (A and B) and/or a major postoperative deformity of the breast (C), making partial reconstruction impossible. The breast is so severely deformed that it cannot be conserved. A mastectomy with immediate reconstruction is the only possible option for restoring the normal breast shape and contour.
We have operated on more than 150 patients with cosmetic sequelae. A systematic prospective analysis of the first 85 consecutive patients was published in 2004. 6
After reconstruction, patients were followed during the immediate postoperative period and every 6 months thereafter. The median follow-up after reconstruction was 33 months (range 6 to 132 months). At each breast cancer follow-up visit, the cosmetic result of reconstruction was quantified and recorded. The cosmetic result after reconstruction for cosmetic sequelae was evaluated using the following scoring system: 1 (excellent), 2 (good), 3 (average), 4 (below average), and 5 (poor). These scores were described in our previous publications 5 , 6 , 11 and represent the mean of the individual scores given by a panel of three individuals—the surgeon, his or her nurse, and his or her assistant. Scores of 1, 2, and 3 were broadly categorized as good, and scores of 4 and 5 were categorized as poor.
Results and Analysis of the Initial 85 Cases
The mean patient age was 44 years (range 27 to 68 years). The interval between the initial BCT and reconstruction of cosmetic sequelae ranged from 10 to 318 months (26.5 years), with a median of 87 months (7.3 years).
UICC Classification
Patients were classified according to the 1998 UICC classification, 12 with the exception of seven patients (Tx, or those with an unknown tumor stage) who were initially treated by another team and subsequently referred to us for cosmetic sequelae with no detailed documentation of their cancer stage. The tumors for the 85 patients were given the following classifications: 13 T0, 25 T1, 35 T2, 5 T3, and 7 Tx.
Cosmetic Sequelae Classification
All sequelae were graded according to our classification, as shown in the tables. Forty-eight patients (56.5%) had type 1 sequelae, 33 (38.8%) had type 2 sequelae, and 4 (4.7%) had type 3 sequelae.
Tumor Site
Most tumors were in the upper outer quadrant (45 cases), 15 were in the upper inner quadrant, 13 in the lower outer quadrant, 7 in the lower inner quadrant, and 5 in the central region. Lower quadrant tumors more frequently involved type 2 sequelae (33% of the cases) than type 1 sequelae (16.6%).
Initial Local Therapy (BCT)
A lumpectomy and radiotherapy were proposed in 81 patients (95.3%). Three (3.5%) patients chose not to undergo postoperative irradiation. Four patients (4.7%) were treated with radiotherapy alone.
Reconstruction of Type 1 Cosmetic Sequelae
Forty-eight patients had type 1 cosmetic sequelae after BCT (see Tables 24-1 and 24-2).
| Type of Cosmetic Sequelae |
| ||
Type of Surgery | Type 1 (n = 48) | Type 2 (n = 33) | Type 3 (n = 4) | Total (%) (n = 85) |
Ipsilateral | 25 | 30 | 4 | 59 (68.2) |
Contralateral | 46 | 27 | 2 | 75 (88.2) |
nb: Most patients were treated with a combination of ipsilateral and contralateral procedures.
NB: Several procedures were performed in some patients to obtain an optimal result. Other procedures include excision of fat necrosis, liposuction, and scar revision.
NAC, Nipple-areola complex.
This patient had cancer in the upper inner quadrant of the left breast. Preoperatively, the breast had a normal shape but was asymmetrical with the contralateral breast (A). The asymmetry was treated with a contralateral mammaplasty (B). No procedures were performed on the irradiated breast.
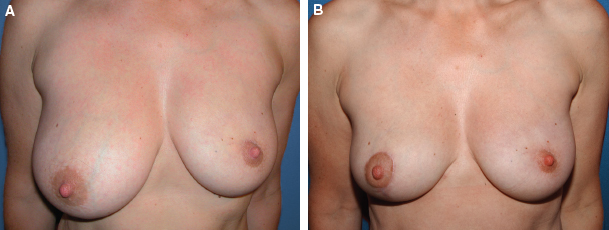
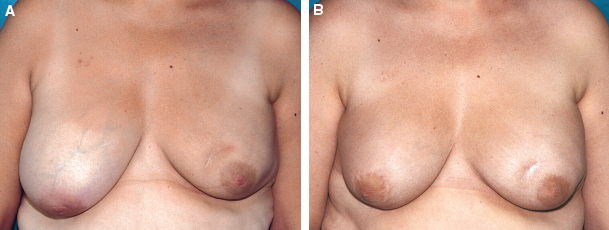
This patient had a tumor located at the junction of the upper quadrants of the left breast. The patient is shown preoperatively (A). A right breast reduction was performed (B).
Treatment of the Irradiated Breast
Twenty-five patients (52.1%) had ipsilateral surgery. Of these, only 6 had mammaplasty, because we try to avoid glandular undermining on an irradiated breast. 9 , 10 , 13 Six other patients had breast augmentation with a submuscular implant. The remaining 13 patients had minor procedures, such as NAC repositioning, minimal resection of a fibrous zone, scar revision, or localized liposuction.
Treatment of the Contralateral Breast
Contralateral symmetrization was performed in 46 of these 48 patients. Reduction mammaplasties were performed in 39 patients, breast augmentation in 5 patients, and other procedures in 2 patients; 23 patients (47.9%) were treated solely with a contralateral procedure.
Number of Operations
Thirteen patients (27.1%) had a second operation to further improve their cosmetic sequelae.
Reconstruction of Type 2 Cosmetic Sequelae
Thirty-three patients were treated for type 2 cosmetic sequelae (see Tables 24-1 and 24-2).
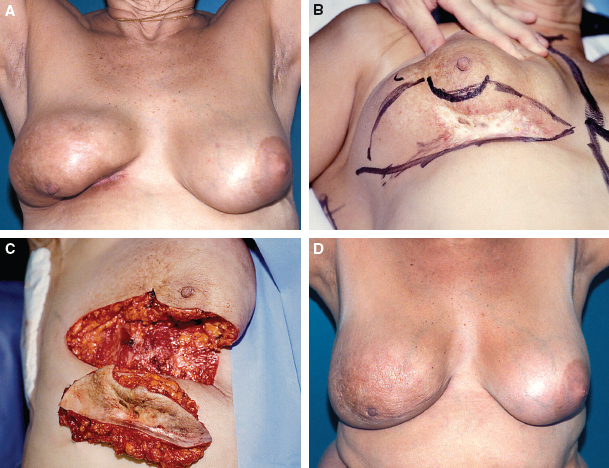
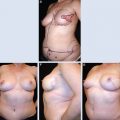
Preoperatively, this patient had breast retraction, pain, and skin ulceration (A). A partial reconstruction of the lower quadrants with a latissimus dorsi flap was performed (B and C). The surgical plan included resection away from the fibronecrotic zones. The patient is shown 3 years postoperatively (D).
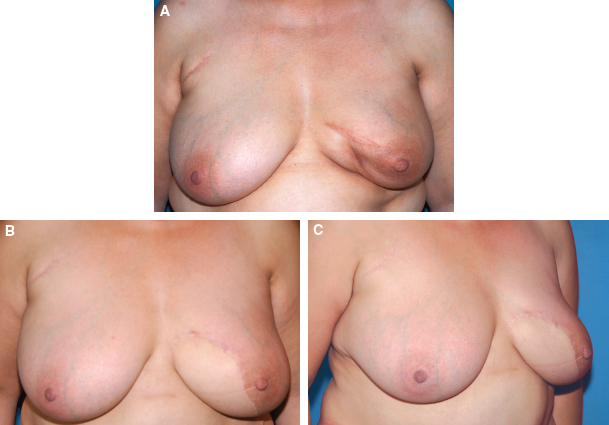
This patient had type 2 cosmetic sequelae affecting the lower inner quadrant. Preoperatively, she had a major retraction of the quadrant with skin adhesions to the chest wall (A). A partial breast reconstruction with a latissimus dorsi flap was performed. She is shown 2 years postoperatively (B and C).
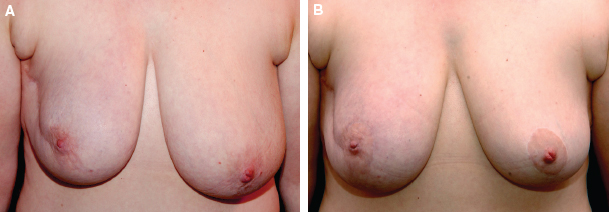
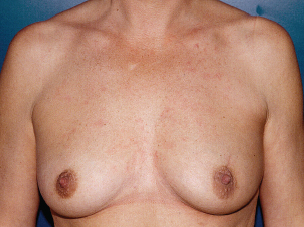
This patient had type 2 cosmetic sequelae affecting the upper outer quadrant. Preoperatively, the quadrant was retracted, causing volume asymmetry (A). Partial breast reconstruction with fat grafting was performed. The patient is shown 1 year postoperatively (B). In addition to fat grafting, scar revision and a contralateral breast reduction were performed.
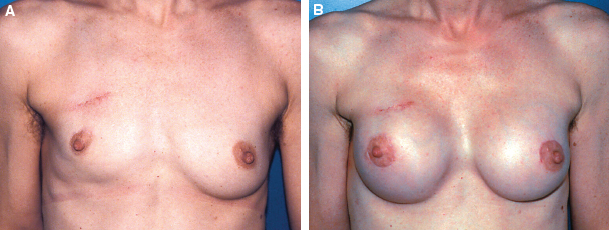
Preoperatively, this patient had major volume asymmetry, postradiotherapy fibrosis of the upper quadrants, and nipple-areola complex deviation (A). Partial breast reconstruction with a submuscular implant was performed, and both NACs were repositioned. She is shown 1 year postoperatively (B).
Because the predominant sequela in these patients was a major breast deformity, a corrective procedure on the irradiated breast was performed in almost all of these patients: 30 of 33 (91%). A partial breast reconstruction with a myocutaneous flap was performed in 15 patients, or 45.5% (latissimus dorsi in 14 cases and transverse rectus abdominis [TRAM] flap in 1 case). Another 15 patients were treated using an atypical mammaplasty, limiting undermining. This mammaplasty usually consisted of an en bloc resection of the distorted zone of the breast and overlying skin, with a direct glandular suture and recentralization of the NAC. Other procedures were performed, either alone or in combination with a flap or a mammaplasty: NAC repositioning in 13 cases (39.4%), implant augmentation in 6 cases (18.2%), and other techniques in 3 cases (18.2%).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree