21 Microtia
Summary
The auricle is located away from the facial triangle (eye–nose–eye). Therefore, the auricle is not the primary attention of people when they look at someone. The goal of ear reconstruction is to restore/create a natural-looking auricle. The surgeon’s focus will be to create the natural helical curve, eliminate unnatural curve, correct excessive protrusion, and restore the missing anatomical parts of the auricle.
Basic knowledge of normal anatomy, proportion, and dimension of the auricle helps prevent mistakes in ear reconstruction. Thin, supple, well-vascularized skin is a must to achieve clear definition of the auricle. It is imperative to create the balance between the amount of skin flap envelope and the cartilage framework to achieve the definition of the auricle.
To be able to create a new auricle from zero, it requires full knowledge and complete skill set of plastic surgery: meticulous skin flap dissection, delicate skin suture techniques, harvesting rib cartilage without perichondrium, elevating temporoparietal fascia flap, and skin harvesting/grafting. Mastering ear framework carving/fabrication techniques requires dedicated, intensive training before starting clinical cases.
Further, it is critical to recognize that what makes a reconstructed auricle beautiful is creating the natural curve of the auricle, especially helix–lobule curve, and concha outline.
21.1 Clinical Characteristics
Microtia varies from complete absence of auricular tissue (anotia) to a small ear with an ear canal. Nagata classifies microtia into three types: lobule type, small concha type, and concha type. Microtia is nearly twice as frequent in males as in females, and the right-to-left-to-bilateral ratio is roughly 6:3:1. Approximately one-third to one-half of the patients exhibit characteristics of craniofacial microsomia. Brent found that 15% of his 1,000 patients had paresis of the facial nerve. Dellon has shown that the palatal muscles are rarely spared in this syndrome.
21.2 Timing of Surgery
Brent begins ear construction at the age of 6, when the normal ear has grown to within 6 to 7 mm of its full vertical height. Nagata begins auricular construction at the age of 10, and chest circumference has grown over 60 cm at this age, at the xiphoid level. These two different timings could be explained by the difference in the amount of cartilage required.
21.3 Epidemiology and Genetics of Microtia
Microtia (= small ear) is a congenital condition with unknown cause. Prevalence of microtia varies significantly among ethnic groups (0.83–17.4 per 10,000 births), and is higher in Asian countries for unknown reason. About 80 to 90% of microtia is unilateral, and 10 to 20% is bilateral. There are more than 18 different microtia-associated syndromes with single-gene or chromosomal aberrations; however, there is no causal genetic mutation confirmed to date. Relatively common syndromes associated with microtia are hemifacial microsomia and Treacher Collins syndrome. Isolated microtia rarely runs in families. Treacher Collins Syndrome, inherited in an autosomal-dominant fashion, often presents with bilateral microtia.
21.4 Middle Ear Problem
Ideally, treatments of microtia involve reconstruction of the external ear and the restoration of normal hearing. Hearing impairment in microtia is related to abnormal auditory canal, tympanic membrane, and middle ear. The problem is conduction. Regarding middle ear surgery for hearing restoration, most surgeons presently feel that potential gains from middle ear surgery in unilateral microtia are outweighed by the potential risks and complications for the surgery and that this surgery should be reserved for bilateral cases. The bone-anchored hearing aid (BAHA; Cochlear, Mölnlycke, Sweden; and Ponto, Oticon, Kongeballen, Denmark) has been used since 1977 and does not require a functioning middle ear or patent canal. In microtia patients, BAHA was initially used for bilateral conducting hearing loss. Only 1 BAHA is usually placed because a single aid will stimulate both cochleae simultaneously. Although traditional teaching has been that hearing on a single side is sufficient for speech development and education, evidence indicates audiologic and subjective benefits when treating unilateral conductive hearing loss with a BAHA. Indications are evolving, and reconstructive surgeons and otologists should work together to achieve long-term success in hearing restoration and auricular construction.
21.5 History of Autogenous Ear Reconstruction
Sushuruta (6 BC) was probably the first surgeon to perform auricular construction, repairing the ear lobe with cheek flap. Tagliacozzi described repair of ear deformities with retroauricular flaps. Early surgical attention focused mainly on traumatic deformities. However, by the end of the 19th century, surgeons began to address congenital defects, in particular prominent ears (Ely, 1881). The concept of microtia repair began in 1920 when Gillies buried carved costal cartilage under mastoid skin and elevated it with cervical flap. Gillies (1937) also used maternal ear cartilage for more than 30 microtic ears; these were found to have progressive resorption. Peer (1948) diced autogenous rib cartilage and placed it in a Vitallium ear mold beneath the abdomen. After 5 months, he retrieved the banked mold, opened it, and harvested the ear framework for microtia repair. Steffensen (1955) attempted to use preserved cartilage and found it progressively resorbed.
Tanzer is the father of modern auricular construction. Tanzer’s excellent results (1959) determined the dominance of autogenous construction with rib cartilage in reconstructive surgery. In the United States, Brent succeeded Tanzer in the early 1970s, and Brent’s artistry has influenced reconstructive surgeons even today. Nagata’s method (two-stage method) gradually gained popularity, and currently is the most popular choice. To this day, autogenous cartilage remains the most reliable material that produces results with the least complications.
21.6 Alloplastic Implants
Although silicone breast implant survives even today, silicon ear framework is seldom used. Silicon framework, introduced by Cronin in 1966, like any other types of synthetic materials, extrudes, causes infection, and loses definition in the long term. Porous polyethylene (PPE) framework, a newer synthetic material, was first introduced by Reinisch in 1991. The disadvantage of the Medpor framework includes use of temporoparietal fascial flap, long-term risk of implant exposure or loss, and compromise of any future autogenous options.
21.7 Prosthesis
Controversies remain regarding appropriate treatment selection for patients with major ear deformities. This is especially true for severe trauma cases, such as extensive third-degree facial burns. Osseointegrated auricular prosthetic reconstruction is complementary to other approaches and provides a reasonable alternative for poor autogenous options and/or failed autogenous reconstruction. The disadvantages of a prosthesis include intermittent soft-tissue problems, long-term maintenance, requirement of a new prosthetic every 2 to 5 years, ongoing cost, inability for future autogenous options, and the need for a compliant patient.
21.8 Total Auricular Construction in Microtia: Author’s Methods
21.8.1 Patient Assessment
About 20 to 60% of children with microtia have associated anomalies or an identifiable syndrome; therefore, individuals with microtia should be examined for other dysmorphic features. Microtia is a common feature of craniofacial microsomia, mandibular dysostoses (e.g., Treacher Collins and Nager syndromes), and Townes–Brocks syndrome. These conditions should be considered among the differential diagnoses when evaluating an individual with microtia.
Facial Symmetry
Asymmetry of the face will make it complicated to locate the ear position. The location of vestige skin is sometimes misleading, and it influences the decision-making of surgeons. Even for expert surgeons, it is tempting to make the auricle based on the current location of the vestige skin, so the surgeons could apply their typical techniques.
Skin Envelope
Assessing the available, soft elastic skin is critical, since it will determine the volume, dimension, and size of the three-dimensional (3D) structure of the ear framework needed. Unbalance between skin envelope and framework may make definition of the auricle poor. Scar interferes the normal stretching of the supple skin envelope and may prevent good definition of the auricle. Scar along the course of the STA (superficial temporal artery) could be a sign of a severed STA, the pedicle of temporoparietal flap, which is an important salvage tool for auricular reconstruction. This is especially important for microtia patients with craniofacial deformities, such as Treacher Collins syndrome. These patients may have bicoronal scarring due to previous skeletal reconstruction.
Vestige Skin
Since microtia has inherent skin envelope deficiency, how surgeons utilize vestige skin strongly influences the definition of the new auricle. Surgeons need to evaluate the location, shape, and volume of the vestige. These factors will influence the design of skin incision, and surgical strategy. If the vestige skin is located inside or near the auricular rectangle, the vestige skin is ready to be utilized for auricular construction. If the vestige is located far away from auricular rectangle, staged transposition of vestige skin may be necessary prior to the framework placement procedure.
Hairline
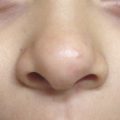
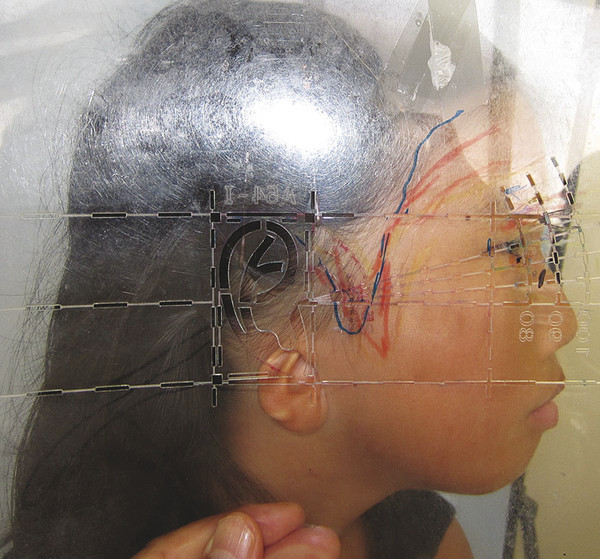
Surgeons need to recognize the presence of low hairline at the time of initial evaluation to formulate their surgical strategy (Fig. 21‑1). The extent of a low hairline influences the choice of surgical procedures. If the hairline exceeds beyond the upper one-third of the auricular framework, either preoperative laser hair removal or intraoperative, fascia flap coverage of the framework, after hair-bearing skin removal, may be necessary. If the extent of a low hairline is mild, hairs down to the scapha fossa can be removed during the second-stage procedure (ear elevation).
21.8.2 Trapezium Space behind Sideburns
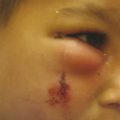
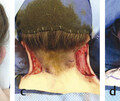
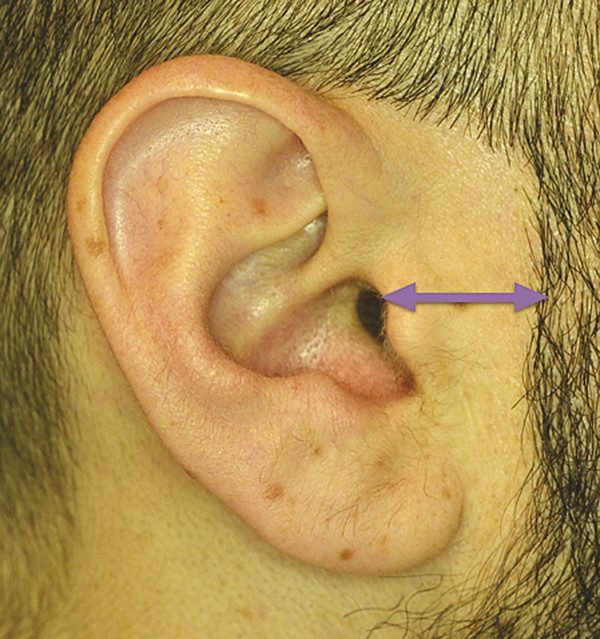
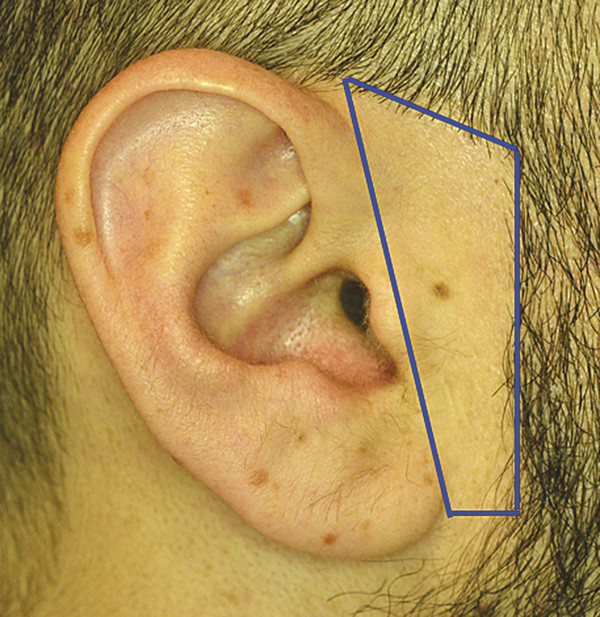
The sideburn is often missing in microtia patients, especially in hemifacial microsomia. If the patient has a normal sideburn, it is an anatomical landmark useful for locating the proper ear position. Anthropometrical study shows that the auricle is normally located approximately 20 mm behind the sideburn (Fig. 21‑2). There is a trapezium-shaped non–hair-bearing space between the sideburns and auricle normally (Fig. 21‑3). Avoid placing the ear framework in this trapezium to prevent anterior inclination of the auricle.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree