Abstract
“Rhinoplasty” covers the spectrum of issues related to the aesthetic and functional components of nose plastic surgery. Factors that influence overall outcome—including patient goals, proper patient selection, psychological fit, etc.—are discussed, as well as up-to-date approaches and techniques used (e.g., software imaging systems). Salient considerations during the presurgical physical examination are listed (e.g., physical deformities and/or abnormalities). Preoperative preparation is stressed, and preoperative considerations are reviewed. A systematic method of facial analysis—involving the frontal, lateral, and basal views—is presented in table format and in the text. Surgical techniques, including the critical area of incisions, are identified, discussed, and compared. Guidelines for postoperative care, complications, airway obstructions, deformities, and outcomes/patient satisfaction conclude the discussion.
20 Rhinoplasty
20.1 Goals and Objectives
After reading this article, the participant should be able to
Discuss essential aesthetic, functional, and other components of the preoperative assessment of patients seeking rhinoplasty.
Identify factors that can influence overall outcome so that successful patient selection is performed in those seeking nasal surgery.
Understand the common approaches and techniques used in rhinoplasty as well as their advantages and disadvantages.
Understand common rhinoplasty complications and be able to identify the principles and methods used in the management and corrective treatment of these sequelae.
20.2 Patient Presentation
Patients seeking rhinoplasty may present in a variety of ways. Regardless of the variability in which patients seek consultation, the initial preoperative assessment is similar. The following methodological approach allows the surgeon to critically understand why the patients are dissatisfied and what their levels of expectation are for surgery. This allows the surgeon to evaluate whether expectations can be met while also allowing the physician to accurately assess and comprehend the patient’s psychological fit for the intended procedure. The goals for surgery should be clearly stated by the patient and easily understood by the surgeon. The single most important determinant of procedural success in rhinoplasty is proper patient selection. It ensures that consistent, reproducible outcomes are achieved while maximizing patient satisfaction. 1
Standardized two-dimensional photographs, including the frontal, oblique, lateral, and basal views, must be obtained in every consultation as they are an important component of the medical record, are instrumental in preoperative planning, and aid in the critical evaluation of the postoperative results. 2 , 3 , 4 Additionally, with the evolution and implementation of software imaging systems commonly employed among practicing rhinoplasty surgeons, this can be helpful for some patients to improve communication between surgeons and their patients. 2 , 5 Most recently, advancements in computer imaging, specifically 3D modeling, can assist in unifying the intended postoperative goals of the surgeon with the intended vision of the patient. 6 , 7
Careful assessment of the psychiatric state of each patient should be performed, as it is instrumental in proper patient selection. This includes evaluating the emotional stability and motivating factors in patients seeking surgery. In a report by Picavet et al, moderate to severe body dysmorphic syndromes were reported in 33% of the overall rhinoplasty population, while this number increased to 43% in patients seeking aesthetic rhinoplasty (level of evidence: risk, III). 8 A significant correlation was found between the prevalence of body dysmorphic disorder in patients who sought aesthetic consultation, in patients who had undergone previous rhinoplasty procedures, or in patients who had an existing psychiatric history.
Obtaining a thorough nasal history is an important component of the patient evaluation. In patients who present with aberrant nasal physiology, identifying the laterality, duration, and time of onset of such symptoms should be noted. Careful inquiry into any mitigating factors that contribute to worsening or alleviation of these symptoms, the presence of headaches, visual disturbances, other otologic symptoms, and/or seasonal allergies should be recorded. Other aspects of the nasal history, including any history of trauma, previous surgery, medication use (with particular attention to vasoactive nasal sprays), and/or use of tobacco, alcohol, or drugs should be documented.
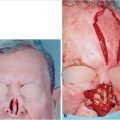
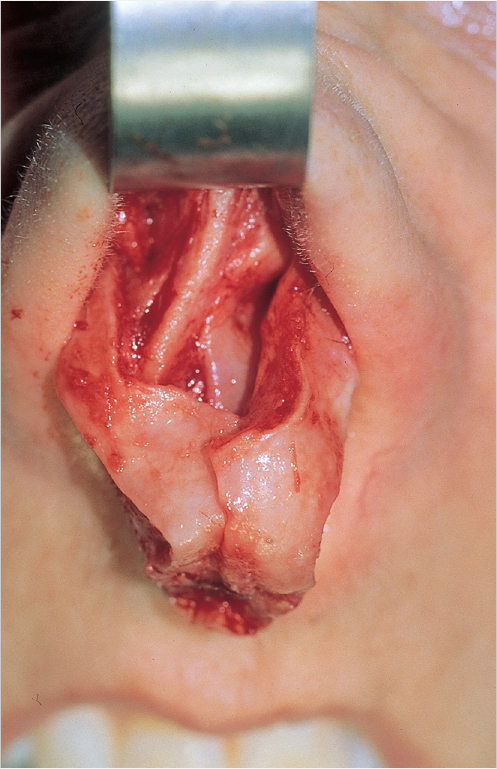
Physical examination of the patient plays a critical role during the consultation, with particular attention to the nasal anatomy (Fig. 20‑1). Careful identification is made of any physical deformities and/or abnormalities of the external and internal nasal valves, the nasal septum, and inferior turbinates. Completion of the physical assessment can be performed with the aid of a headlight, speculum, and vasoconstriction, if needed. The presence of uncharacteristic masses found on intranasal exam or those with obstruction of unidentifiable source dictates further workup by rhinomanometry or sinus computed tomography. 9 , 10 , 11 External inspection should note the presence of inspiratory collapse of the external nasal valve(s) or subjective improvement in inspiratory breathing upon application of the Cottle maneuver (where the examiner places gentle lateral traction on the cheek to simulate improved suspected airway obstruction), either of which should raise the suspicion for nasal airway obstruction. 12
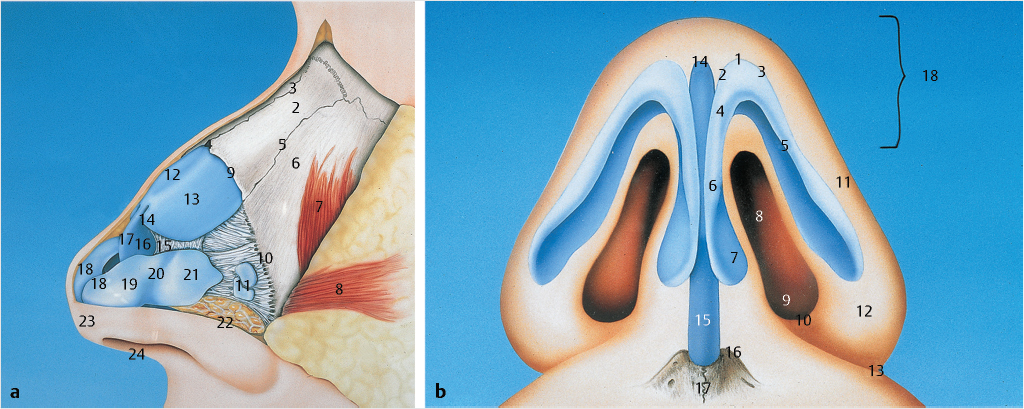
Successful treatment of rhinoplasty patients demands a keen understanding of nasal physiology. Approximately 50% of overall airway resistance stems from the nasal airway which builds up negative pressure during inspiration, causing the nostrils to enlarge, the upper lateral cartilages (ULCs) to move medially toward the septum, the internal nasal valve to narrow, and the tip to plunge. A variety of factors, however, can influence this process and result in various degrees of obstruction with two broad categories including those secondary to an anatomic etiology or those that result from a physiologic response. Patients who complain of constant obstructions are more likely to suffer from a fixed anatomical etiology and are often unilateral while those who have bilateral obstruction, which varies in severity, often suffer from mucosal disease.
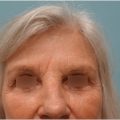
Seasonal obstruction relates to obstruction from pollen, dust, mold, or other allergens and should raise suspicion for allergic rhinitis in patients with such history. Physical examination may be notable for “allergic shiners” which appear as dark circles under the eye. Often, these patients have a history of past or ongoing medication use, which must be documented prior to surgical correction. In patients who do not present with clear findings, trial medication management for nasal airway obstruction can help clarify the clinical presentation.
Rhinitis medicamentosus refers to the rebound engorgement and vasodilation of nasal mucosa secondary to the excessive use of topical nasal decongestants including Afrin (Bayer, Pittsburg, PA) or Neo-Synephrine (Hospira Inc, Lake Forest, IL). When diagnosed, treatment consists of patient education, stopping the offending agent, use of combination of oral antihistamines and decongestants, topical nasal steroid sprays, and potentially, a steroid taper. Asthmatics often have a crease in the skin just cephalic to the dome area secondary to long-standing forces that elevate the tip upward.
20.3 Preparation for Surgery
Nasal surgery is considered a clean contaminated field due to intranasal colonization by commonly identified organisms including Staphylococcus epidermidis, Staphylococcus aureus, and Staphylococcus viridans. Commonly, first- or second-generation cephalosporins are used for perioperative antibiotic prophylaxis which should be given 30 minutes prior to surgical incision. 13 , 14 , 15 However, the available literature includes several studies that have demonstrated no difference in infection rates with the use of postoperative prophylactic antibiotics.
Currently, there is no high-level, evidence-based research which finds benefit in preoperative screening and treatment of those colonized with methicillin-sensitive S. aureus. In one review by Nicholas et al, only a history of methicillin-resistant S. aureus (MRSA) was found to significantly correlate with colonization at the time they presented for outpatient rhinoplasty procedures. 16 Other presumed risk factors including occupational health workers, recent hospitalization, and recent antibiotic use were not found to be lone significant risk factors. Difficulty treating MRSA infections following septorhinoplasty does seem to warrant careful identification of patients at risk for MRSA colonization with swab and culture, while identification of at-risk patients who present with suspected surgical site infection is prudent so that empiric treatment may be initiated.
Paramount to successful rhinoplasty is a thorough preoperative preparation, which helps to provide consistent, reproducible results that minimize undue sequelae. Comprehensive analysis includes review of nasal history, anatomic examination of both internal and external nasal structures, identification of the patient’s deformities and their expectations for the surgical outcome are critical factors. Most importantly, the treating surgeon must perform a thorough nasal analysis to establish a prudent surgical plan of correction. Skin type, thickness, and quality are noted, as thicker, more sebaceous skin tends to camouflage changes to the osseocartilaginous framework necessitating greater and more aggressive modification of the osseocartilaginous framework. Thin skin, on the other hand, may allow for identification of even slight change and reveal the presence of minor irregularities that would have otherwise been obscured. The nose is examined within the context of the entire face, including the chin and neck, helping to ensure that facial harmony and balance are achieved while preexisting asymmetries are identified and communicated to the patient.
A systematic method of facial analysis must then be performed. A variety of orderly approaches exist which allow for through analysis which include using the frontal, lateral, and basal views to determine key findings (Box 20.1).
Box 20.1 Systematic Nasal Analysis
Frontal View
Facial proportions
Skin type/quality—Fitzpatrick type, thin or thick, sebaceous
Symmetry and nasal deviation—midline, C-, reverse-C-, S- or S-shaped deviation
Bony vault—narrow or wide, asymmetrical, short or long nasal bones
Midvault—narrow or wide, collapse, inverted-V deformity
Dorsal aesthetic lines—straight, symmetrical or asymmetrical, well or ill defined, narrow or wide
Nasal tip—ideal/bulbous/boxy/pinched, supratip, tip-defining points, infratip lobule
Alar rims—gull shaped, facets, notching, retraction
Alar base—width
Upper lip—long or short, dynamic depressor septi nasi muscles, upper lip crease
Lateral View
Nasofrontal angle—acute or obtuse, high or low radix
Nasal length—long or short
Dorsum—smooth, hump, scooped out
Supratip—break, fullness, pollybeak
Tip projection—over- or underprojected
Tip rotation—over- or underrotated
Alar-columellar relationship—hanging or retracted alae, hanging or retracted columella
Periapical hypoplasia—maxillary or soft tissue deficiency
Lip-chin relationship—normal, deficient
Basal View
Nasal projection—over- or underprojected, columellar-lobular ratio
Caudal septal deviation
Nostril—symmetrical or asymmetrical, long or short
Columella—septal tilt, flaring of medial crura
Alar base—width
Alar flaring
From Rohrich R, Adams W, Ahmad J et al., ed. Dallas Rhinoplasty. Nasal Surgery by the Masters, 3rd Edition. Thieme; 2014.
20.3.1 Frontal View
Facial proportions—three horizontal lines, tangent to the level of the hairline, brow, nasal base and chin (menton)—are used to divide the face into thirds. The lower third is further subdivided into thirds by placing a horizontal line at the level of the oral commissures (stomion). Concern for a craniofacial anomaly, such as vertical maxillary excess or maxillary hypoplasia, should be raised when deviation is identified.
Symmetry and nasal deviation are examined by using an imaginary vertical line from the midglabellar to the menton to determine if the nose is straight or crooked. Deviation from the midline is suggestive of either bone and/or cartilaginous origin. Cartilaginous deviation is indicative of underlying deviation of the septum that can be classified as midline, C-, reverse C-, S or S-shaped.
Analysis of the dorsal aesthetic lines should be performed. These curvilinear lines should appear as two slightly curved lines which originate at the supraorbital ridges, converge at the level of the medial canthus, and then diverge slightly as they extend to the tip defining points. They should be characterized based on their symmetry, width, and degree of definition.
The cartilaginous and bony vault evaluation should include the length of the nasal bones, their shape, and width. Ideally, the bone base should be approximately 75 to 80% of the alar base width and, when excessive, may warrant performing osteotomies, although over-narrowing should be avoided, especially in males as this may have a feminizing effect. The mid-vault should be assessed for the presence of an inverted-V deformity (where an inverted V-shape depression is palpated between the ends of the nasal bones and the start of the upper lateral cartilage), contour irregularities, and possible nasal wall collapse.
The width of the alar base is observed and should be equivalent to the intercanthal distance. When in excess, the degree of nasal flaring should then be ascertained such that greater than 1 to 2 mL difference between the maximum alar width and the alar base is maintained, suggesting the etiology is alar flaring, often corrected by alar base resection. If less than 1 to 2 mm difference is found, the underlying cause is intrinsic to a primarily excessively wide alar base. The alar rims are examined for the presence of retraction, notching, symmetry, and overall shape. The outline of the rims and columella should maintain a slight inferolateral flare resembling a gull in flight. Angles more steep in quality suggest increased infratip lobular height.
The nasal tip is analyzed by drawing two opposing triangles that connect the two tip-defining points, the supratip point and the columellar-lobular angle point. By connecting these four points with lines drawn within this diamond, the two triangles that are formed should appear equilateral. Further analysis of the tip should characterize the tip as bulbous or boxy and identify the possibility of alar malposition.
20.3.2 Lateral View
The lip–chin relationship is analyzed by drawing a one-half the ideal nasal length tangent to the vermillion of the upper lip. In the resting position, the lower lip should lie approximately 2 mm posterior to the upper lip. The ideal chin position in men should have the chin at the level of the lower lip, while in females, the chin should be slightly posterior. Deviation from this should raise the suspicion that orthodontics, a chin implant, or orthognathic surgery might be necessary (Fig. 20‑2).
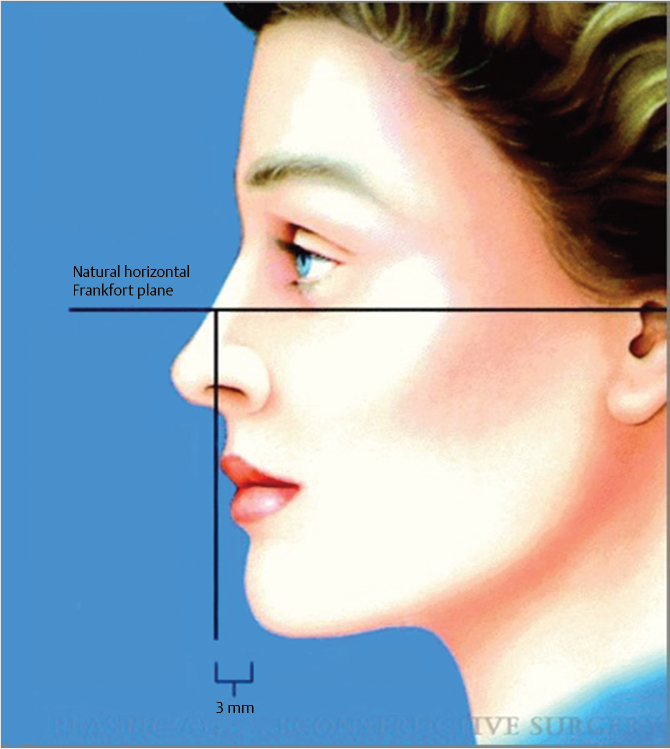
On profile view, analysis of the nose should include the dorsum and tip. The radix should be ideally placed at a level between the upper lash line and the supratarsal fold. The slope of the dorsum, identified by drawing a line from the radix to the tip should be straight in males while a slight concavity approximately 2 mm inferior to this line with a supratip break is considered ideal. Excessive quadrangle cartilage with inferior descent of the nasal tip cartilages is defined as a tension nose.
Tip projection is defined as the distance from the alar cheek junction to the nasal tip and should equal width of the alar base as well as two-thirds of the distance from radix to the tip. An additional method of analysis involves drawing a vertical line tangent through the most projecting portion of the upper lip vermillion. Fifty to 60% of the tip should lie anterior to this line (Fig. 20‑3).

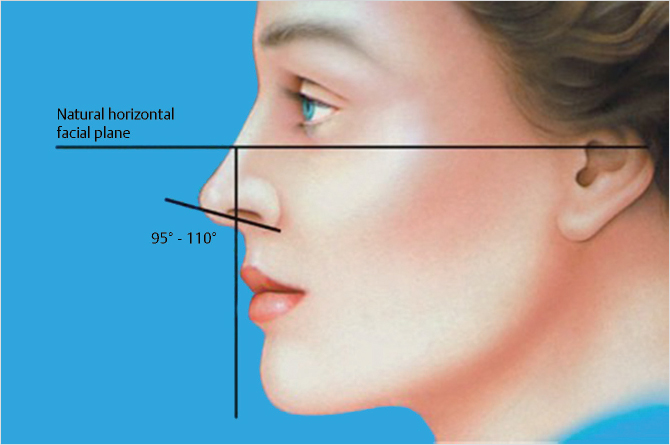
The degree of tip rotation is assessed by calculating the nasolabial angle. This is the angle formed between a line connecting the anterior and posterior portions of the nostril and plumb line dropped perpendicular to the natural horizontal facial plane. Men should have angles between 90 and 95 degrees, and women between 95 and 100 degrees (Fig. 20‑4). Commonly confused with tip rotation is the columellar–labial angle which is the angle formed by the junction of the columella with the upper lip. Ideally 30 to 45 degrees, fullness in this region usually relates to excessive caudal septum.
20.3.3 Basal View
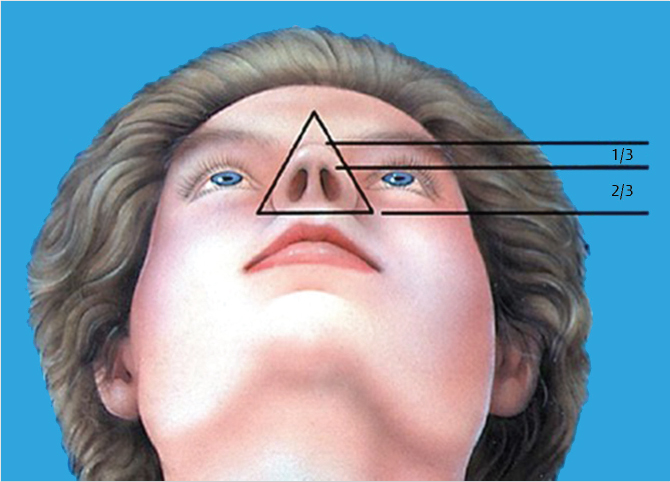
Examination of the nose from the basal view should demonstrate two equilateral triangles each formed by the alar rims and nasal tip with a 1:2 relationship of the nasal tip to the columella. The orientation of the nostril should have a slight medial direction of the long axis and an overall teardrop geometry (Fig. 20‑5).
20.4 Treatment
Surgery may be performed under either local anesthesia with IV sedation or general anesthesia with the use of either laryngeal mask or endotracheal intubation. Upon induction, the patient is prepped for surgery by first trimming the nasal hairs and swabbing the nostrils with Betadine. For an open rhinoplasty, the planned columellar incision is then marked with an indelible marker if using the open approach. Next, the soft-tissue envelope of the nose, the septum, and nasal mucosa are infiltrated with 1% lidocaine with 1:100,000 epinephrine. Additional infiltrate is injected into the inferior turbinates if their manipulation is anticipated. Cotton pledgets soaked in either 4% cocaine or oxymetazoline are then inserted into each nare to help shrink the nasal mucosa, facilitate exposure, and minimize blood loss.
The debate of whether an open versus closed (endonasal) approach to rhinoplasty has been long-standing with firm supporters of each method arguing the merits of why one is better than the other. Regardless of the generic advantages and disadvantages of each method, rhinoplasty should ideally be performed by a surgeon who tailors the operation to the specific anatomic deformities of each patient; thus, one should be familiar with both approaches.
Many surgeons feel that the exposure provided by the open approach allows for more precise identification of the diagnosis or etiology for the nasal obstruction or aesthetic deformity. Moreover, manipulation of these structures and the consequence produced by their dynamic interplay is best appreciated. Although the open approach can be used for all rhinoplasties, three particular circumstances may lend themselves to the open approach, including revisional surgery, posttraumatic deformities in which complete release of the intrinsic and extrinsic deforming forces is necessary, when complex tip modification is necessary. 1 , 2 , 3
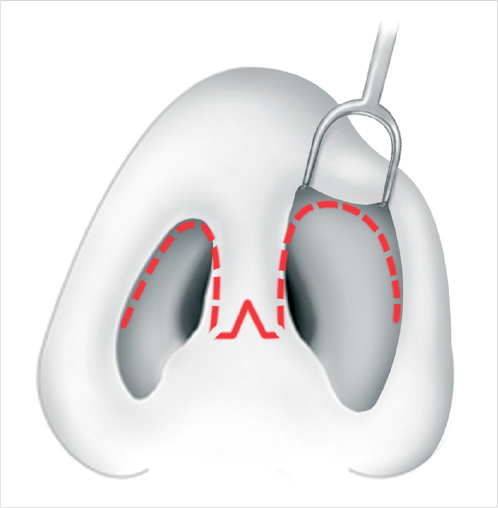
Several types of transcolumellar incisions exist and include the stair-step and inverted-V (Fig. 20‑6). The ideal incision should minimize scar contracture, provide for optimal scar camouflage, and ease closure by the provision of anatomic landmarks. Infracartilaginous extensions of the incision are then made bilaterally and connected to the columellar incisions with careful and meticulous identification of the caudal borders of the lower lateral cartilages (LLCs) so that iatrogenic injury to these structures and particularly the domes is prevented.
The closed approach lends itself to patients with isolated deformities of the nasal dorsum and/or tip which require minimal tip modification. A combination of incisions is often used to access the regions of concern. They include both alar and septal incisions.
20.5 Alar Incisions Used During Closed Rhinoplasty
Intercartilaginous: incisional placement between the upper and lower lateral cartilages.
Transcartilaginous: incision placed at the level of the lower lateral cartilages with the LLCs delivered via a cartilage-splitting approach.
Marginal: incision made at the alar rim and in conjunction with an intercartilaginous incision that allows for delivery of the LLC.
20.6 Surgical Incisions for Both Open and Closed Rhinoplasty
Complete (transfixion) incision: the membranous and caudal cartilaginous junction is incised in its entirety, exposing the nasal spine and the depressor septi muscle.
Limited partial transfixion: allows for preservation of the attachments of the caudal septum to the medial crural footplates but decreases access to the nasal tip.
Partial transfixion: starts caudal to the anterior septal angle and ends just short of the medial crural attachments to the septum.
Hemitransfixion: placed unilaterally at the junction of the caudal septum and columella.
High septal transfixion: preserves the junction of the caudal septum to the medial crura and membranous septum.
Regardless of the method of approach, the skin envelope is then sharply skeletonized immediately superficial to the perichondrial surfaces of the cartilages in a cephalad direction until the bony pyramid is reached. At this point, a subperiosteal dissection is carried out in limited fashion over the portion of the bony dorsum that needs modification while minimizing disruption to the periosteal attachments which maintain nasal bone position and attachment to the ULCs. The periosteum of the nasal bones is elevated with a Joseph periosteal elevator, and with the same instrument the depressor septi nasi are swept off the maxilla in order to reduce nasal tip plunging.
20.6.1 Nasal Dorsum
Hump reduction can be performed in either a composite or component fashion. Several techniques have been described with osteotome and rasp being the most common method of reducing the dorsal hump (Fig. 20‑7). In the composite method where the upper lateral cartilages and nasal bones are reduced together, the risk of separating the nasal bones from the ULCs, resulting in an inverted-V deformity, is possible and necessitates restoration of the ULC position to maintain the internal nasal valve.
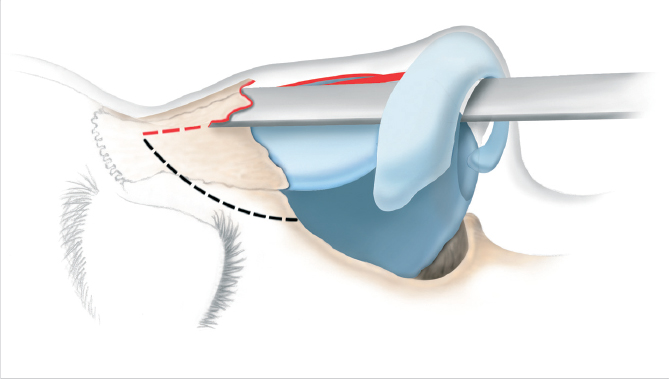
In the component method of reduction, the ULCs are separated from the septum by creating bilateral superior sub-mucoperichondrial tunnels which allows for sharp division of these transverse processes while not violating the nasal mucosa. Alternatively, the upper lateral cartilages can be separated from the septum with a no. 11 blade. Upon separation into three distinct components (the septum and the ULCs on each side), the cartilaginous dorsum can then be sharply lowered under direct visualization. The ULCs are reduced if indicated. This type of separation of the ULCs from the septum is necessary when spreader cartilage grafts are placed for treatment of airway obstruction (Fig. 20‑8).
Incremental dorsal bony reduction is then performed with either a power burr or a guarded 8-mm osteotome when large (>5 mm) or with a sharp, down-biting diamond rasp if smaller. Verification using three-point palpation and a saline moistened dominant index fingertip is performed repeatedly throughout this process to assess for dorsal irregularities or contour depressions of both the left and right dorsal aesthetic lines and the septum centrally.
Dorsal augmentation can be carried out using a variety of techniques with the use of autologous cartilage being most common. Dorsal onlay grafts can be fashioned by performing partial-thickness cuts into various shaped grafts. Care must be taken to minimize graft visibility as skin thickness and graft placement increase this potential risk. More commonly used in Asia, synthetic implants include silicone (expanded polytetrafluoroethylene Gore-Tex) and high-density polyethylene (Medpor; Porex Surgical, Newman, GA).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree