18 Lower eyelid blepharoplasty
INDICATIONS
Lower eyelid blepharoplasty can be utilized to surgically manage patients with any of the following indications:
Excess infraorbital fat
Pseudoherniation of fat
Redundant skin and muscle
Lower eyelid malposition
There are currently a number of techniques and surgical approaches to correct imperfections of the periorbital region, particularly with regard to the lower eyelid. These include the following:
Transconjunctival approach: Indicated for patients with pseudoherniation of fat and minimal or no excess skin
Subciliary approach with skin-muscle flap: Indicated for patients with pseudoherniation of fat, excess skin, and redundant orbicularis oculi
Subciliary approach with skin-only flap: Indicated for patients with both pseudoherniation of fat and excess skin only, with preservation of the orbicularis oculi
INTRODUCTION
One of the first areas in the face to demonstrate significant signs of aging is the periorbital region. Surgical procedures to restore a youthful appearance to the lower lid region date back over 2000 years, with various techniques used to reduce redundant tissue and excess skin. To be considered a candidate for surgery, a patient must undergo a preoperative evaluation consisting of a thorough review of all ocular and medical problems, particularly with regard to the following:
Prior periorbital surgery
Visual deficits
Glaucoma
Dry eye symptoms
Medical history (e.g., comorbidities such as hypertension, diabetes, or thyroid disease which can prevent adequate wound healing)
Medications (e.g., anticoagulation, vitamin E, ginkgo biloba)
Smoking
Knowledge of the medical history and ophthalmic conditions is crucial as the procedure could potentially exacerbate or worsen such conditions. A preoperative ophthalmology evaluation can help identify some of these conditions. Table 18.1 indicates special equipment needed for this procedure.
0.5% topical ophthalmic tetracaine hydrochloride 1% lidocaine with 1:100,000 epinephrine 30-gauge needle Lubricating ophthalmic ointment Corneal shield Mosquito hemostat Needle-tip electrocautery 5-0 nylon suture 6-0 fast-absorbing gut suture Desmarres retractor Small blunt-tip dissection scissor Cotton-tip applicators |
TRANSCONJUNCTIVAL APPROACH TO LOWER BLEPHAROPLASTY (FIGURES 18.1 AND 18.2)
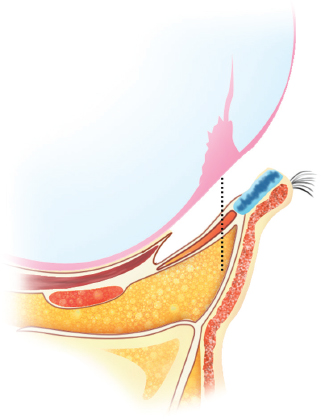
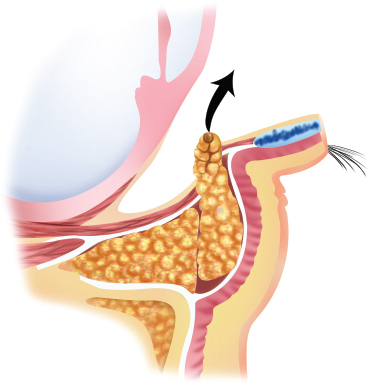
Preoperative markings
A marking pen is used to make surgical markings 4 mm inferior to the lower border of the tarsal plate to preserve the orbital septum.
The medial extent of the markings should be in line with the inferior punctum.
The lateral extent of the markings should be 4–5 mm medial to the lateral canthus.
Intraoperative details
Two drops of 0.5% tetracaine hydrochloride are instilled into each inferior fornix.
Corneal eye shields are placed bilaterally.
The lower lid conjunctiva is injected with 1 cc 1% lidocaine with 1:100,000 epinephrine using a 30-gauge needle.
A needle-tip electrocautery is used to make a transconjunctival incision as previously marked, keeping the orbital septum intact.
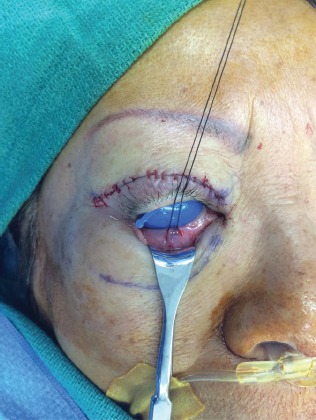
A 5-0 nylon suture is placed through the conjunctiva closest to the fornix to retract the posterior llamella over the cornea with a mosquito hemostat held on to the patient’s head wrap to hold the suture under tension (Frost retention suture) (Figure 18.3).
Simultaneous eversion of the lower eyelid using a Desmarres retractor and gentle pressure on the globe will produce a bulge of orbital fat which helps guide the dissection.
Blunt dissection with the assistance of a cotton-tip applicator is performed until the medial, central, and lateral fat pads are identified.
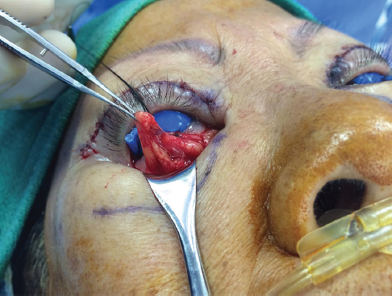
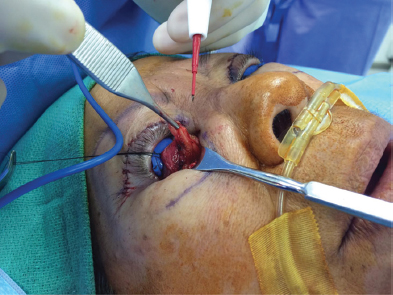
A fine forceps is used to carefully tease out the excess fat with care to remove only the excess herniated fat to prevent a hollowed-out appearance (Figure 18.4).
A mosquito hemostat is used to clamp the fat pad at its stalk. The fat pad is then transected with a needle-tip electrocautery (Figure 18.5).
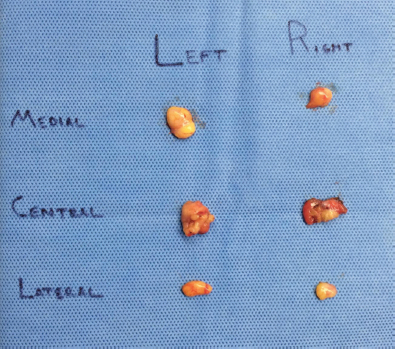
After resection of fat, the surgical field is examined until meticulous hemostasis is achieved, and a comparison of left and right lower eyelids is performed for symmetry.
The volume of fat removed from each fat compartment can then be compared between sides (Figure 18.6).
Finally, fat repositioning may be performed to fill in more inferior orbital hollowing by redraping the fat over the arcus marginalis and to fill nasojugal deficiencies after releasing the orbitomalar ligament.
Additional facial fat grafting to the nasojugal grove or tear trough can also be performed as an adjunctive procedure.
The conjunctival incision can then be reapproximated with or without suture closure.
Adjunctive procedures to treat excess skin can now be performed, including chemical peel, laser resurfacing, or skin-pinch excision.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree