16 Non-surgical facial rejuvenation with neuromodulators and dermal fillers
INTRODUCTION
Nonsurgical facial rejuvenation procedures are highly sought as more patients demand less-invasive, yet effective, procedures to mitigate signs of facial aging with minimal downtime. Nonsurgical procedures accounted for 82% of cosmetic procedures performed in the United States in 2011, with 4,030,318 botulinum toxin type A injections followed by 1,662,480 hyaluronic acid (HA) filler injections. 1
The first injectable filler approved by the Food and Drug Administration (FDA) was bovine collagen (Zyderm®/Zyplast®, Inamed Aesthetics, Santa Barbara, CA), 2 made available in 1981. Although this was a great leap forward from the preceding era of liquid silicone injections, bovine collagen could potentially cause severe allergic reactions, which required pre-treatment skin testing. Today, collagen use has been largely replaced with HA fillers, which have the benefit of causing far fewer allergic reactions (0.6–0.8%) 3 as they are olysaccharides and not proteins. HA fillers also allow correction of mistakes using hyaluronidase. 4 There is some evidence that HA fillers can stimulate de novo synthesis of dermal collagen. 5 Several HA fillers are FDA approved: Restylane® (Medicis, Scottsdale, AZ); Perlane® (Medicis); Juvederm® (Allergan, Irvine, CA); Captique® (Allergan); and Hylaform® (Allergan). Several other non-HA fillers have gained FDA approval. These fillers include calcium hydroxylapatite (Radiesse,® Bioform Medical, San Mateo, CA); poly-L-lactic acid (Sculptra®, Sanofi-Aventis, Bridgewater, NJ); and polymethylmethacrylate or ArteFill® (Suneva Medical, San Diego, CA).
With the explosive increase in filler-type choices in the last decade, with and without premixed lidocaine, 6 the aesthetic surgeon must be well versed in the chemical and physiologic differences of each and the difference in injection depths of the fillers.
THE AGING FACE
The youthful face has smooth contours, few wrinkles at rest as well as animation, and appropriate soft tissue fullness. With age, the skin accumulates solar damage and shows uneven pigmentation and loss in dermal thickness and elasticity. Rhytids ultimately form due to a combination of these skin changes, gravitational descent of soft tissues, and repeated muscular contractions (Figure 16.1). Transverse forehead lines appear with repeated brow lifting by the frontalis muscle, worsened in patients with eyelid ptosis, which leads to forehead muscle compensation. 7 Vertical lines form in the glabella with repeated contraction of the corrugator supercilii, and crow’s-feet (lateral orbital rhytids) appear lateral to the eyes from the concentric movement of the orbicularis oculi. Further caudally, malar fat pads descend with gravity, starting a constellation of changes, including the appearance of deepened nasolabial folds as well as jowling and resultant prejowl sulcus formation. Perioral rhytids form due to a multitude of concomitant factors. Loss of lip volume combined with continued orbicularis oris motion lead to a stellate-type pattern of vertical rhytids around the mouth.

In addition to the visible changes in the skin, there is marked thinning of subcutaneous tissues. The face has anatomically defined compartments of fatty tissues 8 that may not all descend or thin simultaneously. With this knowledge, there has been a paradigm shift in treating the aging face. No longer are individual wrinkles treated to achieve a smooth and line-free face, but the combination use of neuromodulators and fillers tackles both the soft tissue volume loss and lines caused by muscle contraction. 9 Table 16.1 indicates equipment needed for treatment.
INDICATIONS FOR INJECTABLE FILLERS
Pronounced nasolabial fold
Marionette lines
Perioral lines
Lip augmentation
Jowl lines
Glabellar lines
Tear trough deformity
Facial lipoatrophy
INDICATIONS FOR BOTULINUM TOXIN INJECTION FOR FACIAL REJUVENATION
Glabellar lines (FDA approved for Botox® Cosmetic [Allergan]; Dysport® [Medicis, Scottsdale, AZ]; and Xeomin® [Merz Pharma, Frankfurt, Germany] at time of writing; off-label use for other indications)
Horizontal forehead lines
Crow’s-feet
Platysmal bands
Depressor anguli oris (DAO)
PRE-PROCEDURAL DETAILS
Patient evaluation and facial analysis
As with surgical rejuvenation, the patient’s goals must be realistic and congruent with our treatment plan. To achieve a successful outcome, the patient must understand the limitations of non-surgical facial rejuvenation. Fillers can augment soft tissue volume, but the skin envelope excess cannot always be addressed with non-surgical procedures alone. Patients with unrealistic expectations must be screened out prior to treatment, and we are obligated to point out what is not correctable without surgical intervention.
Assessment begins with a focused history and physical examination. Age is an important factor in the evaluation, as increased age may lead to decreased immunogenicity and less inflammatory risk; however, thinner skin can be less forgiving to an uneven injection of filler. 10 A careful medication history is obtained, and avoidance of nonsteroidal anti-inflammatory drugs (NSAIDs), blood thinners such as warfarin, and herbals such as gingko biloba for 36 hours and ginger for 2–3 weeks 11 prior to injection is highly encouraged. Patients all undergo a standardized set of photographs prior to any injection.
For charting purposes, it may be helpful to use a classification of facial wrinkles. The Lemperle scale (Table 16.2) of wrinkle severity is a validated scale 12 from grades 0 to 5, with 0 being no perceptible lines to 5 being a deep wrinkle with a redundant overhanging soft tissue fold. 13 Pre- and post-treatment photographs are strongly encouraged for self-critique and improvement of technique.
0 | No wrinkle |
1 | Just perceptible wrinkle |
2 | Shallow wrinkles |
3 | Moderately deep wrinkle |
4 | Deep wrinkle, well-defined edges |
5 | Very deep wrinkle, redundant fold |
In evaluating the patient, the face is scrutinized in an organized and systematic manner. A well-proportioned face has three zones of nearly equal height: the upper third from the hairline to glabella, the middle third from the brow to the base of the nose, and the lower third from the base of the nose to the chin point (Figure 16.2).
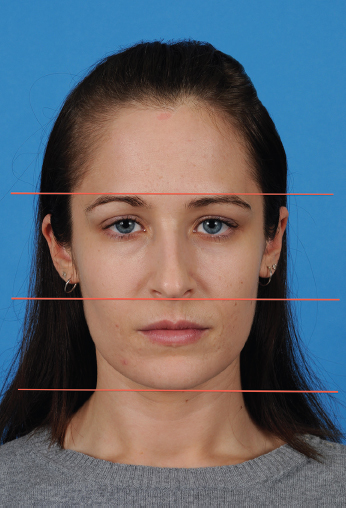
The top third of the face begins at the hairline and extends inferiorly to above the brow. Abnormalities such as a high-positioned hairline are noted. Transverse forehead lines are assessed with the patient in repose as well as with active brow elevation. Vertical glabellar lines may be marked prior to injection. To optimize results, the visible outline of the corrugator supercilii when frowning is noted. Laterally, temporal soft tissue loss is assessed.
The middle third of the face extends from the brow to the base of the nose. Here, the focus is the periorbital area. Periocular rhytids (crow’s-feet) are noted laterally. Transverse lines immediately cephelad to the nasion are a result of an overactive procerus muscle. Tear trough deformities are notoriously difficult to treat as these may be due to infraorbital fat herniation, and are likely not muscular in etiology. Furthermore, the infraorbital region has thin, unforgiving skin and is prone to bruising and surface irregularities from filler injection if injected superficially.
For the lower third of the face, the nasolabial fold and its infraoral continuation, the prejowl sulcus (marionette lines), are pointed out to the patient. These lines form with the descent of subcutaneous tissues in the setting of thinning skin. Loss of projection and fullness of the lips, vertical lines on the upper lip, and soft tissue loss on the lateral edges of the mental crease are noted.
Choice of product
The choice of fillers available on the market can be overwhelming. Due to aggressive marketing of each product in beauty magazines, on television, and online, patients may arrive with a choice of filler in mind. As the surgeon, it is paramount to be well versed in the differences of each product. It is beyond the scope of this chapter to discuss the benefits of each product, but a brief description of the general categories is discussed here.
Hyaluronic acid (HA) is a naturally occurring glycosaminoglycan ubiquitous in mammalian extracellular matrix and is especially abundant in loose connective tissue. 14 It can bind 1000 times its volume in water, making it a relatively ideal soft tissue filler. 15 In its natural form, the half-life is 24 hours. 16 Commercially available HA fillers have stabilized cross-linking, allowing for an increased life span when compared to the natural product.
HA products differ in chemistry by particle size, HA concentration, and degree of cross-linking. Restylane was the first FDA-approved HA filler; it has an HA concentration of 20 mg/mL, gel particle size of 400 µm, and 1% cross-linking. 17 Juvederm, FDA approved in 2006, originally had an HA concentration of 24 mg/mL and a higher percentage of cross-linking but is now available in a line of products with variable concentrations of HA, ranging from 18 to 30 mg/mL. Products with a smaller particle size are more forgiving and allow for smoother injection. Products with a larger particle size, such as Perlane and Juvederm Ultra, are marketed for a deeper dermis and subdermis injection plane for moderate to severe wrinkles.
Non-HA fillers can provide a much longer-lasting effect but may potentially have longer-lasting side effects in the hands of an inexperienced clinician. Radiesse is a mineral scaffold of 30% calcium hydroxylapatite spheres, ranging from 25–45 µm, approved for wrinkles as well as HIV facial lipoatrophy. 18 The scaffold allows for tissue ingrowth, and the spheres are eventually encapsulated by collagen fibers, leading to longer-lasting results than HA fillers. One study demonstrated an increased incidence of nodules when injected in the lip and recommended against its use there. 19 Another study showed a lip nodule formation rate of 5.9% of 349 lip injections with Radiesse. However, it was noted that the incidence declined to less than 2% for the last 100 injections, implying the complication rate is dependent on clinician experience. 20
Poly-L-lactic acid is a biodegradable polymer, available in microspheres as Sculptra (Sanofi-Aventis). It also stimulates collagen deposition gradually through a mild inflammatory response, and clinical response is seen over time. Meticulous injection with a fanning technique in the subdermal plane is required to optimize results. 21 It can be used for HIV lipodystrophy and is injected in the subcutaneous plane. In our experience, patients often need multiple injections spaced 2 months apart, with visible results expected in 4–6 months.
Botulinum toxin type A is a neurotoxin secreted by Clostridium botulinum. All type A toxins have the same mechanism of action: they cleave the protein SNAP-25, thus aborting the exocytosis of presynaptic vesicles containing acetylcholine. Because the toxin works at the presynaptic neuromuscular end plate, the toxin is injected into the muscle itself. At the time of publication, there are currently three brands of FDA-approved botulinum toxin type A available. Botox Cosmetic (onabotulinumtoxinA), Dysport (abobotulinumtoxinA), and Xeomin (incobotulinumtoxinA). Although all three are FDA approved for cosmetic use for glabellar rhytides, other facial injections for cosmetic use are currently off-label.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree