14 Management of Acute Complications of Aesthetic Breast Surgery Part II—Malpositions and Rippling
Summary
Implant malposition, inframammary fold asymmetry/deformity, and implant rippling remain an important driving factor in patient dissatisfaction after breast augmentation. Knowledge of how to approach both the patient and operative management is of the utmost importance. With adequate preoperative planning and careful management of patient expectations, these complications may be addressed with satisfactory results. In this chapter, we detail the underlying etiology and describe various operative approaches for managing this group of complications.
14.1 Introduction
14.1.1 Definitions
Implant and Inframammary Fold Malposition
Implant malposition, in which a breast implant is incorrectly positioned, is the second most common complication arising after breast augmentation, second to capsular contracture (discussed in Chapters 13 and 15).
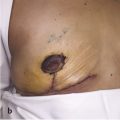
Implant malposition may manifest in different ways, and in some cases, the displacement may occur in more than one direction. Medial malposition may cause confluence of the breasts in the midline, known as symmastia. The term symmastia was coined by Spence et al in 1984, combining the Greek syn (together) with mastos (breast) to describe a “presternal blending” of the breasts. 1 Symmastia more commonly occurs with the placement of large implants, overdissection of the pocket medially, and use of the subglandular plane (Fig. 14‑1). 2 Superior malposition leads to a “high-riding” implant, or “Snoopy nose” deformity (Fig. 14‑2). Snoopy nose deformity, also called double bubble type A or waterfall deformity, occurs when the implant is positioned cephalad to the glandular tissue. Inferior malposition may lead to the “double-bubble” effect, where the breast tissue is seen to lie superior to the implant (Fig. 14‑3). Lateral malposition (telemastia) is also observed and can create a wide separation between breasts.
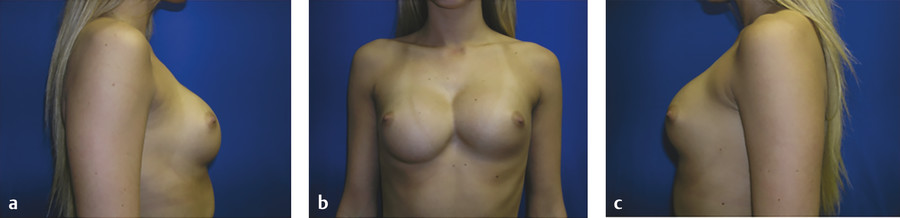
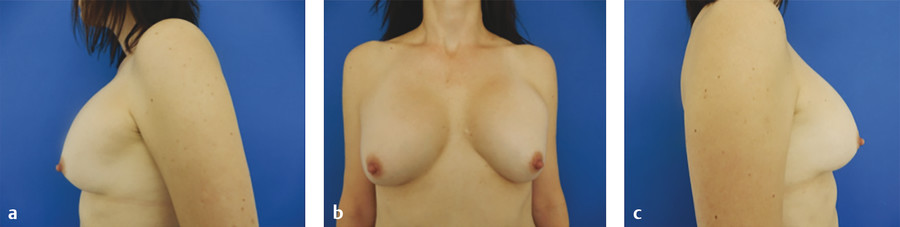
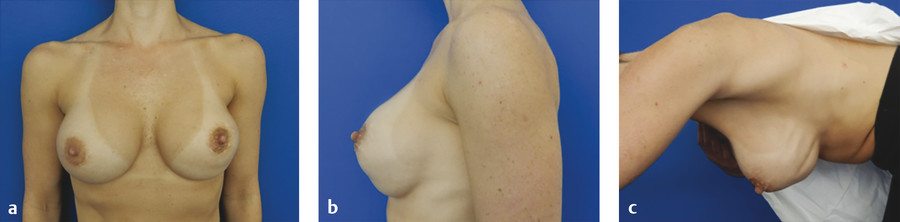
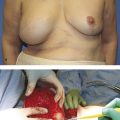
Inframammary fold (IMF) malposition manifests as one that does not maintain symmetry with the contralateral breast or when the implant migrates inferior to the proposed pocket. This is demonstrated in Case 1 in the Case Series at the end of this chapter.
Implant Rippling
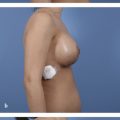
Implant rippling occurs where there is loss of the normal smooth curvature of the breast and, instead, wrinkles or ridges in the implant are transmitted to the skin, This is demonstrated in Case 2 in the Case Series at the end of this chapter.
14.1.2 Importance of These Complications
In the event of any of the complications in the preceding subsection occurring, patients may present for revision surgery with high expectations, given the emotionally charged nature of the operative journey they have likely endured. 3 Moreover, previous work has shown that breast augmentation is one of the procedures most commonly associated with aesthetic malpractice claims. 4 Undertaking revisionary breast surgery can be challenging and complex, even for the most experienced surgeons. In this chapter we outline the pathophysiology and etiology of implant malposition, including symmastia, implant lateralization and inframammary fold malposition, and rippling, in addition to discussing operative approaches to managing these findings.
14.1.3 Etiology of Implant Malposition
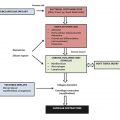
Implant malpositions may be multifactorial. However, as described by Brown et al, they can usually be ascribed to one or more of five categories: “patient factors, procedure selection, implant selection, surgical technique, and postoperative management.” 5 An understanding of these is crucial in determining the management strategy employed.
Patient Factors
Thin skin envelope and thin soft tissue overlying the implant are among the most frequently noted causes of implant malposition. This may be related to quality of the native tissue or to postoperative tissue atrophy. 6 A combination of poor-quality tissue and stretching over time can cause implant malposition, especially laterally and inferiorly. Small-breasted women of slight stature may fall into this category. It is recommended that the measured pinch-thickness of the upper breast pole coverage should be at least 2 cm for subglandular placement to be safe; otherwise deeper or dual-plane placement may be warranted to avoid implant rippling or palpability.
The Snoopy nose breast may occur in women with pre-existing ptosis. Ptosis of the glandular breast tissue relative to the implant and superior bulge caused by the implant are noted. The unsatisfactory look is further worsened by the ptotic appearance of the nipple areolar complex (NAC). Moreover, chest wall asymmetries and aberrant chest wall contouring, such as that present in pectus excavatum, may displace an implant. Vigorous contraction of the pectoralis major muscle in athletic individuals may lead to superolateral malposition. These factors must be observed or circumnavigated in any attempt at revision surgery.
Patients who present with tuberous breast deformity are at high risk of developing double-bubble deformity and high-riding implant.
Procedure Selection and Surgical Technique
The contribution of procedure selection and surgical techniqe to implant malposition primarily consists of the plane in which the implant was placed and the incisions used to approach the augmentation. For example, subglandular implant placement may more often predispose to medial displacement, because of lack of pectoralis support in that region. In contrast, subpectoral placement may lead to lateral displacement as a result of strong overlying muscle contraction. Symmastia can also occur in the subpectoral plane if the pectoralis major muscle is detached from the chest wall too aggressively. As discussed, implant malposition can be caused by technical error. Therefore, precise pocket dissection is important to avoid these complications.
Disruption of the native IMF may be more likely with inframammary incisions, leading to inferior malposition. Excessive IMF dissection may lead to caudal displacement of the implant with respect to the breast mound, creating a second, parallel IMF inferior to the native IMF and breast mound; this is known as the “double-bubble” deformity, as previously mentioned. 7 This may be unprecedented, when overdissection occurs in the context of hematoma evacuation; thus, it is important to minimize the risk of postoperative complications that may necessitate dissection. Meticulous hemostasis and minimization of surgical tissue trauma are essential. Where postoperative accumulation of fluid arises, early detection and prompt drainage are essential to avoid creation of a larger implant pocket.
Other situations may be anticipated, but tricky to avoid. For example, in women with particularly constricted breast bases, it may be necessary to lower the IMF in order to bring the NAC superiorly to a more central position. However, without particular attention to release of the tight IMF, it may often persist and form a second crease superior to the new IMF.
Another commonly encountered scenario is that of the patient who would have benefited from a combined augmentation–mastopexy but instead has an augmentation with a large implant. In this case, poor procedure selection may lead to the aforementioned complications.
Implant Selection
One of the most important considerations is that of implant size. While patients may desire large implants relative to their frame, it is important to respect the natural breast footprint. Rapid tissue expansion may also lead to stretching and thinning of the skin and overlying soft tissue, removing the supportive envelope required to maintain implant position. Horizontal displacement, vertical displacement, or a combination of these may result. Where vertical displacement occurs, a phenomenon known as “bottoming out” may be observed, where the nipple-to-IMF distance increases.
The surface of the implant is also important. Textured implants may lower capsular contracture rates and reduce the rate of implant migration. It has been suggested that this may be due to greater tissue integration or disruption of collagen deposition. However, textured implants have thicker shells and may be prone to traction rippling. This may be in part due to the heightened tissue integration.
Finally, but no less crucially, the choice of implant composition must be considered carefully. Because of concerns regarding the safety of silicone implants given recent reports of textured silicone–associated anaplastic large cell lymphoma (ALCL), saline implants represent a safer alternative. However, saline implants, despite the advantages of their lowered contracture rates and relative safety in the event of leakage, are more likely to exhibit rippling. Moreover, implants that are not filled adequately are also more prone to rippling.
Finally, capsular contracture is an important cause of implant malposition, as seen in Fig. 14‑2.
Postoperative Management
Adequate patient education, particularly regarding use of supportive clothing, is essential. Timely follow-up is important to enable early identification and treatment of complications that may predispose to implant malposition (such as infection, hematoma, and seroma development).
14.2 Management
14.2.1 Preoperative Evaluation
Having considered which category or categories of complication may apply to your patient, now you must consider how to move forward and address the issue. When faced with any breast augmentation revision surgery, a surgeon must return to basic principles: history and physical examination, in addition to elucidating patient expectations and setting appropriate goals.
History
This section covers three main themes: the operative course, the patient’s personal and breast-specific health, and the patient’s concerns and expectations.
It is important to elucidate the patient’s operative course up until the time of presentation. The first task is to note when the primary augmentation took place and what the specific indication was. Previous operation notes are useful in determining details about the implant itself, including composition, surface, shape, size, and fill. The use of adjunctive materials such as acellular dermal matrices (ADMs) must be noted. Ascertaining the location of the implant pocket is crucial, as is determination of the incisions used to access the pocket.
In taking the patient’s personal history, the surgeon asks questions to evaluate the patient’s general health, looking for risk factors that may affect any revisionary surgery undertaken. This includes wound healing problems, smoking, or steroid use. The surgeon ascertains any factors that may have influenced the development of implant malposition; for example, did the patient undergo massive weight loss or become pregnant?
In addition, it is important to characterize the patient expectations. What is she most dissatisfied by? This may include asymmetry, overall quality of life, and ill-fitting clothes. What does she hope to achieve? This is important, as it will not always be possible—or sensible—to attempt to correct all concerns.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree