11 Preoperative Evaluation of the Breast Augmentation Patient
Summary
This chapter serves to outline the preoperative evaluation of a breast augmentation patient. Patients are divided into three categories: hypomastia, involutional atrophy, and developmental asymmetries with hypomastia. Each category is carefully evaluated for surgical planning.
Key Teaching Points
The patient’s goals require careful analysis and appreciation.
The breast should be carefully analyzed in terms of morphology and its relationship to underlying muscular structures.
The anatomy of the patient’s cleavage should be evaluated as it may impact the approach to breast augmentation technique selection.
Significant ptosis will require a combination mastopexy augmentation.
Nipple sensation should be assessed preoperatively as it may be impacted by surgery.
Suspicious masses should be evaluated preoperatively with a full breast work-up to exclude cancer.
Asymmetries should be pointed out and carefully evaluated for correction.
Women presenting to plastic surgeons for breast augmentation usually fall into one of the three major categories:
Patients with hypomastia desiring augmentation alone.
Patients with involutional atrophy postlactation, who may be candidates for either augmentation alone or augmentation mastopexy.
Patients with asymmetry and hypomastia.
Each category requires careful clinical evaluation with an assessment of the patient’s desires and expectations before developing an operative plan. Failure to appreciate subtle differences in best shape and location can lead to undesirable postoperative complications and patient dissatisfaction.
Before examining these patients, a thorough general and breast history should be taken, including an evaluation of breast development in other members of the family as well as cancer history. Patients with a strong family history of breast cancer and ovarian cancer may be carrying the BRCA oncogene and require genetic testing. They may well require prophylactic mastectomy and reconstruction rather than consideration for an augmentation given that mastectomy would be an inevitable long-term requirement as a lifesaving procedure. Careful consideration should also be given to the patient’s expectations and body image. Patients desiring exceptionally large and unrealistic augmentations are a particular cause of concern, and body dysmorphic disorder should always be considered in such patients. Surgery should never be performed in patients suspected of having body dysmorphic disorder.
Similarly, it is important to understand the patient’s desires and expectations in terms of overall breast anesthetics. When the discussion first begins regarding ultimate breast size, the patient should be made aware of the ideal proportions of the normal breast. Malucci’s description of the 45:55% ratio of upper pole to lower pole fullness is a good starting point for this discussion.
11.1 Breast Examination
When evaluating a patient with hypomastia for breast augmentation, it is helpful to consider four important parameters as the basis for decision making in order to achieve the best aesthetic outcome. These are listed below:
Footprint of the breast.
Conus of the breast mound.
Quality of the overlying skin and parenchyma.
Ratio of breast tissue above and below the nipple equator (45:55%).
11.2 Hypomastia
Nulliparous patients with hypomastia are typically younger women whose breasts have simply failed to develop to a volume that is aesthetically pleasing for them. Frequently, these patients are thin with a small breast volume and varying degrees of separation of their breasts in the midline. If they have had children, breast-feeding may have exacerbated the problem. Occasionally, one sees the patient who is heavier in terms of body weight, but who simply has small breasts, which may appear even smaller due to their heavier body proportions.
When examining such patients several clinical features need to be evaluated.
Key Clinical Features
Nipple to notch measurement.
Nipple to inframammary fold distance.
Intermammary distance.
Length and breadth of the chest wall.
Presence or absence of pectus deformities.
Volume of breast tissue.
Medial and lateral pinch test.
Level at which the pectoralis major muscle arises from the sternal border.
Nipple–areola diameter and nipple prominence.
Presence or absence of breast herniation into the areola suggesting tuberous deformity and the degree of definition of the inframammary crease.
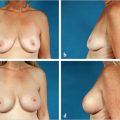
Nipple to Notch Measurement: The average nipple to notch measurement in the virginal breast is 19 to 21 cm. Patients with long thin chests may have greater nipple to notch measurements, but still appear to have a proportional looking chest. The longer the distance to the nipple, the greater the tendency for the patient to appear to have low slung breasts at the completion of breast augmentation. Similarly, if the patient has a very short distance from the nipple to the notch with a short vertical length to her chest wall, it is imperative not to give the patient the appearance of excessively high breast augmentation with fullness below the clavicles (▶Fig. 11.1, ▶Fig. 11.2).
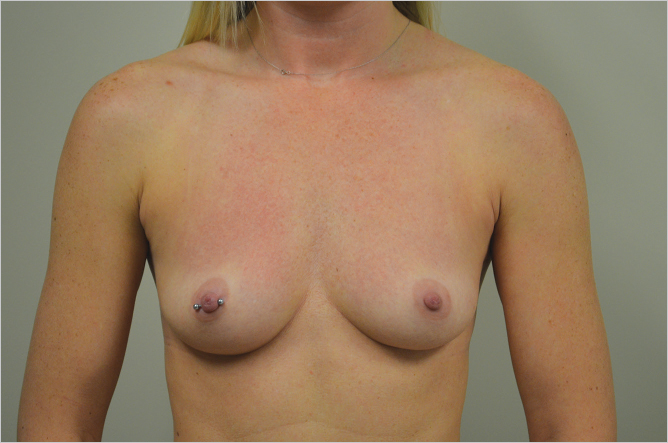
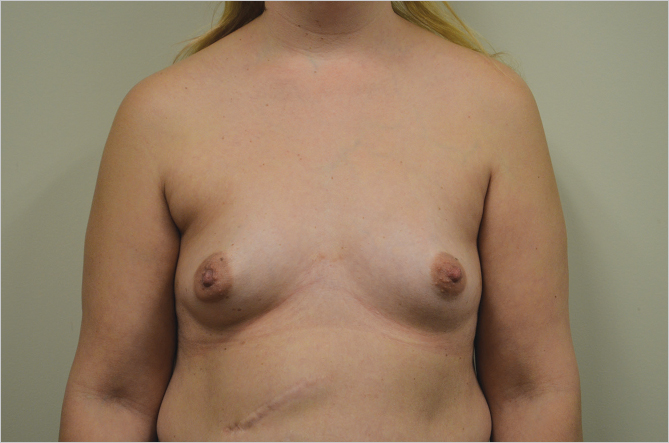
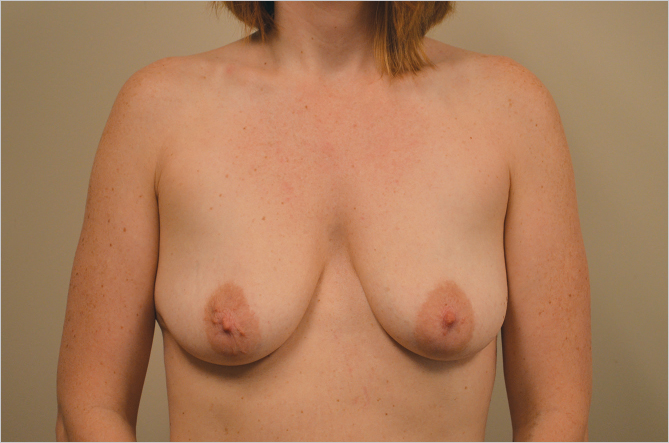
Nipple to Inframammary Fold Distance: The nipple to inframammary fold distance is an important determinant of aesthetic success in breast augmentation. This is particularly true of the patient who has an excessively short distance between the fold to the nipple, particularly if that crease is tethered to the chest wall. An inability to release the inframammary fold and create natural lower pole fullness will accentuate the tendency to double bubble formation. This is an extremely unattractive deformity following breast augmentation and can be difficult to avoid or correct. Although inframammary radial scoring can be helpful in eliminating a tight short breast crease to achieve lower pole natural contours, it is often an indication for me to perform subfascial augmentation by which means I can really achieve consistent aesthetic results in these patients. Similarly, in excess of the long inframammary fold to nipple distance in patients with pseudoptosis of the lower pole of the gland can create unattractive glandular ptosis over the lower pole of the implant, which can give the augmentation a very unbalanced appearance (▶Fig. 11.3).
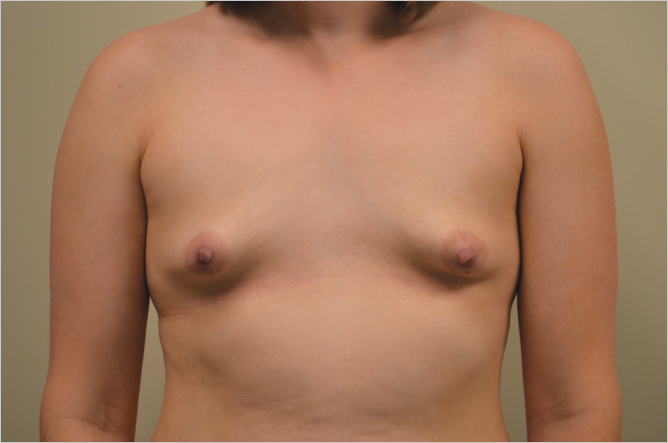
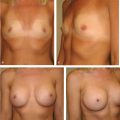
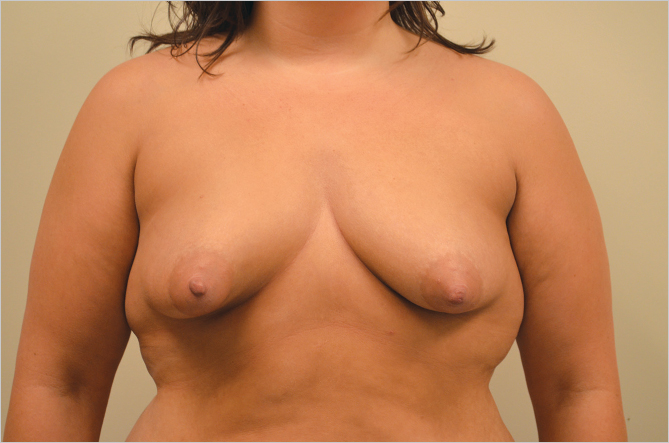
Intermammary Distance: The distance between the breasts will determine how much cleavage the surgeon is likely to achieve when performing augmentation. Two factors determine cleavage. The first is the level at which the pectoralis major muscles arise from the lateral portion of the sternum. In some patients, the medial borders the pectoralis muscles are almost touching in the midline which allows a subpectoral implant to be placed medially to enhance cleavage. In other patients, the pectoralis major origins may be so lateral that the muscles act as a barrier to medial implant placement, resulting in a very wide-spaced augmentation, with an area of flatness appearing between the breasts. Many patients find this distasteful and unattractive. The second factor affecting cleavage is the origin of the breast gland itself in relation to the sternum. If the gland itself is located immediately over the pectoral muscles, the patient is more likely to have attractive cleavage fullness after an augmentation than if the breasts are very widely spaced in relation to the muscles. In patients with widely separated breasts desiring cleavage, I find it preferable to perform a substantial augmentation, as this allows me to place the implants more medially on the chest wall without having to be concerned about the level of origin of the pectoralis major muscles in relation to the sternum (▶Fig. 11.4, ▶Fig. 11.5).
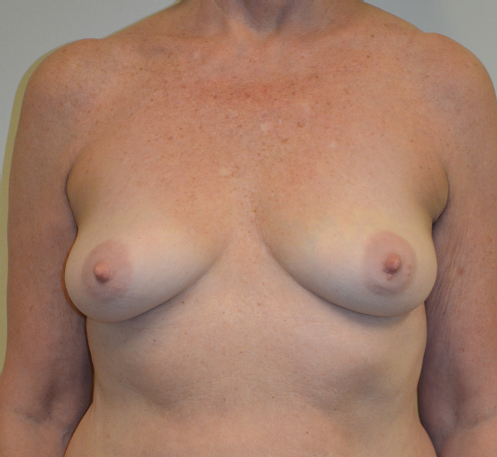
11.2.1 Chest Wall Length and Breadth
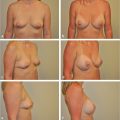
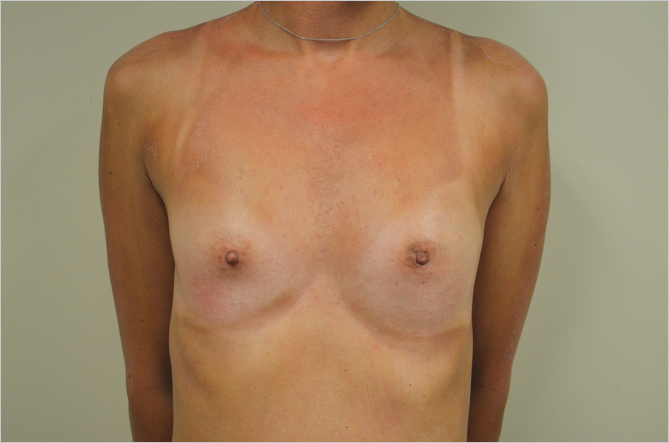
Measurements of the chest wall vary enormously in terms of body habitus, patient height, and transverse diameter of the thoracic cavity. Tall asthenic individuals tend to have narrow chest diameters with long vertical length while mesomorphic individuals often have wider transverse diameters to the chest wall all of which can have an impact on breast location. Implant-based diameter should be carefully assessed in such individuals, as a very wide implant in a narrow-chested patient may create excessive lateral fullness, while a narrower implant in a broad-chested woman may not fill the base diameter of the breast adequately. Additionally, some patients have lateral chest wall fullness, which may detract from the overall result of an augmentation and may require suction reduction in order to achieve a pleasing aesthetic result (▶Fig. 11.6, ▶Fig. 11.7).
11.2.2 Chest Wall Deformities
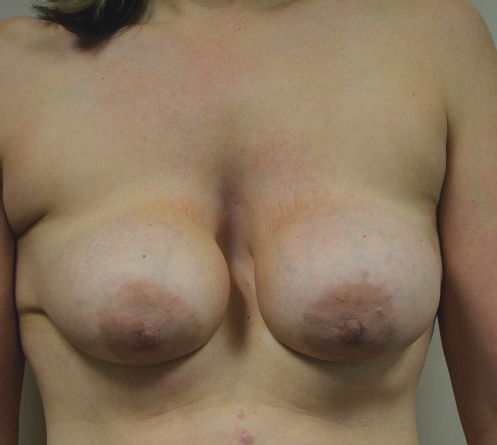
Patients presenting for breast augmentation should have a careful examination of the sternum and adjacent chest wall, in order to evaluate the potential impact of deformities of the structures on the final outcome. Patients with pectus excavatum deformities often have a medial tilt of the breast into the deformity and the nipples may point medially creating a “squinting” type appearance. Rotation of the breast laterally can correct this bizarre appearance. In addition, the medial pectoralis major muscles may be poorly developed in these patients as may be the intercostal muscles, rendering the patients more at risk of accidental penetration of the pleural cavities during dissection. Subpectoral dissection should be undertaken with great care in these patients and it is my preference to perform a subfascial augmentation in this clinical setting. Conversely, pectus carinatum deformities tend to push the breasts laterally and result in a tendency for implants to slide laterally off the chest wall toward the axilla (▶Fig. 11.8, ▶Fig. 11.9).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree