Viral Exanthems
Kenneth Howe
 Varicella (chickenpox)
Varicella (chickenpox)
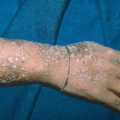
 Hand-foot-and-mouth disease
Hand-foot-and-mouth disease
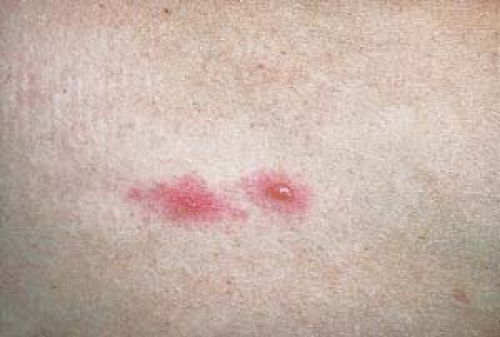
 Erythema infectiosum (fifth disease)
Erythema infectiosum (fifth disease)
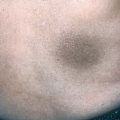
 Roseola infantum
Roseola infantum
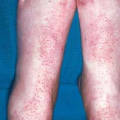
 Rubella (german measles)
Rubella (german measles)
 Rubeola (measles)
Rubeola (measles)
Overview
Viral exanthems are the cutaneous manifestation of an acute viral infection. In most exanthems, viral particles are present within the visible lesions, having reached the skin through the bloodstream. It is unclear whether the observed exanthem results from active viral infection of the skin, the immune response to the virus, or a combination of these two.
Most common in children, viral exanthems may present as distinct, clinically recognizable illnesses such as measles or chickenpox. More frequently, however, a nonspecific eruption is seen that makes an exact diagnosis elusive. More than 50 viral agents are known to cause exanthems, and many of these rashes are indistinguishable from one another. Because most viral illnesses are benign and self-limited, a specific diagnosis is often not made.
In some situations, however, determining the precise etiology may be of vital importance. Examples include the appearance of a viral exanthem during pregnancy or in an immunocompromised patient. It is also important to distinguish viral exanthems from rashes caused by treatable bacterial or rickettsial infections and from hypersensitivity reactions to medications.
Varicella (Chickenpox)
Basics
Varicella, or chickenpox, is an infection caused by the varicella-zoster virus (VZV). Transmission occurs by aerosolized droplet spread, with initial infection occurring in the mucosa of the upper respiratory tract. Traveling through the blood and lymphatics (primary viremia), a small amount of virus reaches cells of the reticuloendothelial system, where the virus replicates during the remainder of the incubation period. Nonspecific host defenses contain the incubating infection at this point, but in most cases these defenses are eventually overwhelmed, and a large secondary viremia results. It is through this secondary viremia that VZV reaches the skin. The viremia occurs cyclically over a period of approximately 3 days and results in successive crops of lesions.
Most cases occur during childhood, and half of the patients are younger than 5 years of age.
Epidemics have a peak incidence during late winter and spring.
Description of Lesions
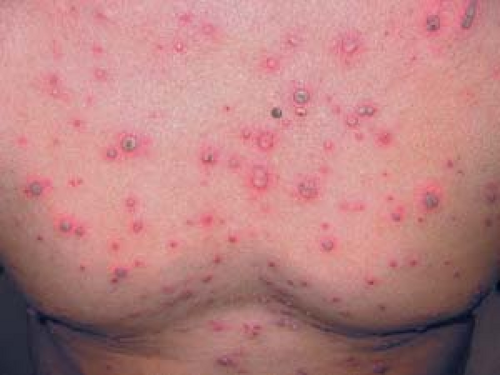
The characteristic lesions begin as red macules and progress rapidly from papules to vesicles to pustules to crusts. The entire cycle may occur within 8 to 12 hours. The typical vesicles are superficial and thin walled, and they are surrounded by an irregular area of erythema, giving them the appearance of “a dewdrop on a rose petal” (Fig. 8.1).
The lesions are usually pruritic.
Involvement of the oral mucous membranes (enanthem) occurs as well, most commonly on the palate. Because vesicles in these sites quickly rupture, it is common to observe shallow erosions.
Because the lesions appear in successive crops, a characteristic feature of varicella is the simultaneous presence of lesions in varying stages of development. In any given area, macules, vesicles, pustules, or crusts may be seen.
Crusts usually fall off within 1 to 3 weeks, depending on the depth of involvement.
Large blisters can also be seen in varicella, often resulting from superinfection with Staphylococcus aureus. Hemorrhagic lesions may occur in patients with thrombocytopenia.
Scarring is not unusual in uncomplicated varicella. Facial “punched-out” scars are common.
Distribution of Lesions
The eruption typically begins on the face, scalp, and trunk and then spreads to involve the extremities.
Successive crops appear over 3 to 5 days, resulting in a diffuse, widespread eruption of discrete lesions (Fig. 8.2).
Clinical Manifestations
Incubation Period
The duration typically is 2 weeks (range, 10 to 21 days).
During this period, children are usually asymptomatic, with the onset of the rash being the first sign of illness.
In older children and adults, symptoms are typically more severe. The rash is frequently preceded by 2 to 3 days of fever and flulike symptoms, which often persist during the acute illness.
Complications
Complications in healthy children are rare; complications are more common in infected adults.
Varicella pneumonia is a relatively uncommon complication that usually occurs in adults and immunocompromised children. It begins 1 to 6 days after onset of the rash, with pulmonary symptoms such as cough, dyspnea, and pleuritic chest pain. The severity of the symptoms is out of proportion to the findings on physical examination. Chest radiographs typically reveal diffuse nodular densities.
Diagnosis
The diagnosis of varicella is usually straightforward, based on the characteristic presentation and clinical findings.
A Tzanck smear can be helpful in confirming the diagnosis (see Chapter 6, “Superficial Viral Infections”). When the test is positive, it reveals characteristic multinucleated giant cells. Identical findings are seen in herpes zoster virus or herpes simplex virus (HSV) infections.
Laboratory Testing
Smears obtained from active lesions can be tested by the direct immunofluorescence technique, which uses fluorescent-labeled antibodies to detect the presence of VZV. This technique has a sensitivity and specificity nearly equal to those of culture, with the advantage of providing rapid results.
Active lesions can also be cultured for VZV. Culturing of the VZV virus is technically difficult and positive less than 40% of the time.
Other Viral Exanthems
Vesicular exanthems of coxsackievirus and echovirus infections may be mistaken for varicella.
These exanthems may show a characteristic distribution, as in hand-foot-and-mouth disease.
Disseminated Herpes Zoster
See Figure 24.6.
Patients have a previous history of primary varicella.
There is often a typical vesicular eruption accentuated in one unilateral dermatome in a typical “zosteriform” pattern. This is seen in addition to a widespread rash that is indistinguishable from varicella.
The patient is generally immunocompromised, secondary to medications, malignant disease, or human immunodeficiency virus infection.
Eczema Herpeticum (Kaposi’s Varicelliform Eruption)
See Figure 6.29.
Preexisting skin disease such as atopic dermatitis becomes secondarily infected with HSV.
Direct immunofluorescence or culture results indicative of HSV infection.
Atypical Measles
This occurs in adults who received killed measles virus vaccine between 1963 and 1967.
The eruption begins on the palms and soles and then spreads proximally.
Pneumonia is a common feature.
The diagnosis can be confirmed by a rise in measles antibody titers.
Impetigo
The patient generally feels well.
Typical moist, honey-colored crusts are present, often in a periorificial distribution (See Chapter 5, “Superficial Bacterial Infections”).
Acute Varicella
Uncomplicated varicella in otherwise healthy children is generally treated with supportive care such as antipruritics and antipyretics. Aspirin should be avoided because of the risk of Reye’s syndrome.
Oral acyclovir is warranted in patients who are at an increased risk of complications, and, in general, it should be started within 24 hours of the onset of the rash. These patients include:
Otherwise healthy, nonpregnant patients 13 years of age or older.
Children older than 12 months of age with chronic skin or pulmonary conditions or who are receiving long-term salicylate therapy.
Children receiving short, intermittent, or aerosolized courses of corticosteroids.
Intravenous acyclovir is indicated in immunocompromised patients or in patients with virally mediated complications of varicella.
Varicella Vaccine
The VZV vaccine (Varivax) is recommended for universal immunization in all children.
It is optimally given between 12 and 18 months of age; it may be administered in a single dose at any time before 13 years of age.
In older adolescents or adults, two doses of vaccine should be administered 4 to 8 weeks apart.
The appearance of breakthrough varicella, seen in previously immunized persons, has indicated that the effectiveness of the vaccine wanes over time. Consequently, a revaccination booster immunization is now recommended for children between 4 and 6 years of age.
Varicella and Pregnancy
Peripartal maternal varicella poses a particular risk to the newborn. Neonates born 2 days before or 5 days after the onset of maternal varicella should be given varicella immunoglobulin (VZIG). Those newborns who develop varicella should be treated with intravenous acyclovir.
Oral acyclovir is not recommended in pregnant women with uncomplicated varicella because the risks and benefits to the fetus are unknown.
Pregnant patients who develop varicella in the first trimester have a 2.3% to 4.9% risk of delivering a child with the fetal varicella syndrome.
This syndrome is a congenital malformation complex with features such as intrauterine growth retardation, prematurity, cicatricial lesions in a dermatomal distribution, limb paresis and hypoplasia, chorioretinitis, and cataracts.
It is not known whether the administration of acyclovir prevents these complications.
Patients remain contagious until all cutaneous lesions are crusted.
Hand-Foot-and-Mouth Disease
Basics
Hand-foot-and-mouth disease is an acute viral infection that manifests as a vesicular eruption with a characteristic distribution. The infection is caused by enteroviruses, most commonly coxsackievirus A16. The virus is spread from person to person by the fecal-oral route.
Outbreaks are typically in the summer or early fall, and epidemics may occur. Transmission is more likely in crowded environments.
Young children (1 to 5 years of age) are most commonly infected.
The incubation period ranges from 4 to 6 days.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree