Chapter 8 Ultrasound-assisted breast reduction
![]() For additional online content visit http://www.expertconsult.com
For additional online content visit http://www.expertconsult.com
Introduction
As is known, ultrasound energy was initially used by Zocchi1–6 to emulsify fat. A special instrument, composed of an ultrasound generator, a crystal piezoelectric transducer, and a titanium probe transmitter was utilized to target adipocyte cells. This new technology was first applied to body fat to emulsify only fat cells while sparing the other supporting vascular and connective components of the cutaneous vascular network. More recently, Goes,7 Zocchi,1–6 Benelli8 and di Giuseppe,9–12 have started to apply this technology to breast tissue to achieve breast reduction and correction of mild to medium-degree breast ptosis.
Preoperative Preparation
Preoperative Mammography
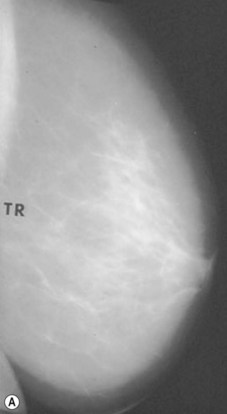
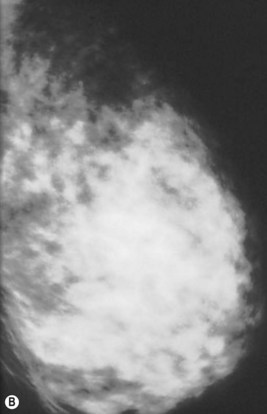
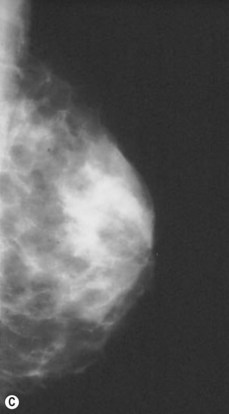
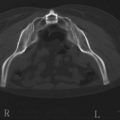
Preoperative mammograms (anteroposterior and lateral views), the so-called Ecklund view, are taken to evaluate the nature and consistency of the breast tissue (fibrotic, mixed or fatty parenchyma ), distribution of the fat, presence of calcifications, and areas of dysplasia or nodularity that might necessitate further studies (Fig. 8.1). The presence of fibroadenomas, calcifications, and other suspected or doubtful radiologic findings should be double-checked with ultrasound and a radiologist experienced in breast tissue resonance.
Contraindications
Furthermore, because the amount and distribution of the breast fat is variable, not all women are candidates for breast volume reduction with UAL. If fat and glandular tissue are mixed, penetration of the tissue may be impossible, as noted by Lejour13 and Lejour and Abboud.14 If the breast tissue is primarily glandular, the technique is not indicated.
Surgical Technique
Infiltration
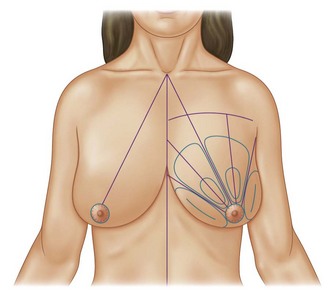
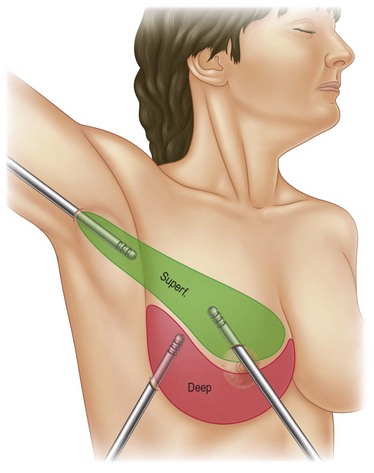
Infiltration should be divided into the three different layers of the breast: deep, intermediate, and superficial (Fig. 8.3).
In deeper and intermediate layers I expect a 1.5 : 1 ratio between infiltration and aspirate; in the superficial layer I normally infiltrate twice what I expect to extract (2 : 1 ratio). I use blunt infiltration cannulas, as described by Klein,15 15–20 cm long.
Probes
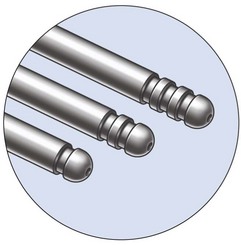
The Vaser system (Sound Surgical Technologies, Denver, CO, USA) provides different sizes and lengths of solid titanium probes (Box 8.1) expressly designed to fulfill all purposes in body contouring, as well as being capable of emulsification through the cavitation effect produced by the ultrasound energy. The piezoelectric transducer transforms electric energy into “vibration energy”, thus allowing the solid titanium probe to emulsify the target fat cells.
1. To enhance the efficiency of the emulsification, which is not limited to the tip, but extends to the last 1.5 cm of the shaft.
2. To allow a greater selection of options for targeting the various tissue types (purely fat, mixed, fibrotic), by utilizing different probes.
Technique
The Vaser surgeon may now utilize two further options:
1. The 4.5 mm large probe, for larger volumes, with a higher percentage of fat emulsification, for 1 minute,depending on the diameter of the probe.
2. The “cone” tip probe, which is very aggressive in fibrous tissue, and has been designed for male breast tissue (gynecomastia) destruction (Fig. 8.4).
Fat Emulsification
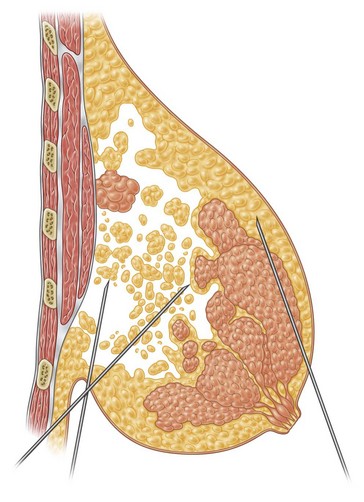
In breast reduction with UAL the duration of the procedure varies depending on the volume of reduction, the type of tissue encountered, and the amount of skin retraction required. A breast with purely fatty tissue is easier to treat than one with mixed glandular tissue, in which fat cells are smaller, stronger, and denser (Fig. 8.5).
The surgical planes, with good criss-cross tunneling and adequate undermining, are planned in the preoperative drawings. If large undermining is required for skin retraction, the superficial layers are treated initially. Then the deeper planes are reached, and more time is spent in thicker areas. Surgeons inexperienced in the procedure should be especially cautious when performing the technique, particularly in the subdermal planes.9–12,15–19
Subcutaneous UAL Undermining
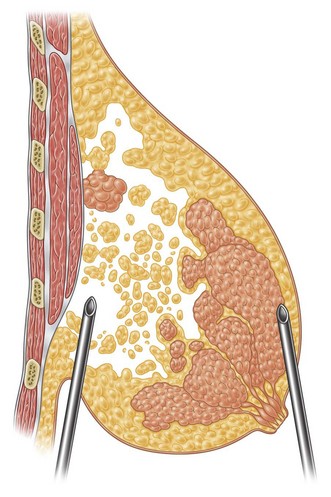
Together with UAL application to the fat layers, starting from the deeper layers and progressing to the more superficial ones, it is advisable to thin the superficial layer of the subcutaneous tissue of the upper and lower quadrants by using a different angle pattern, as in standard lipoplasty.20,21 This superficial undermining with low-frequency ultrasound energy helps to enhance the retraction of the breast skin and to redrape the breast skin to the newly shaped and reduced mammary cone (Fig. 8.6).
Optimizing Outcomes
Vaser is selective, and does not interfere with the vascular network of the dermal tissue, if properly made. It divides the connective and supporting structures of the skin. Rudolph (1991)22 showed the great potential of the dermal layer in wound contracture. As much as the dermis is thinned, so much contraction will result, providing the tissue vascularization is preserved.