div class=”ChapterContextInformation”>
61. Surgical Treatment of Male Stress Urinary Incontinence: An Overview
Keywords
Stress incontinenceProstatectomyMale slingArtificial urinary sphincter61.1 Introduction
The most common cause of male stress urinary incontinence (SUI) in patients who seek treatment is prior prostate treatment, particularly radical prostatectomy [1, 2]. The fact that these patients have already suffered an adverse event is an important factor to consider when offering surgical treatment for incontinence. Therefore, patient counseling and managing patient expectations is nearly as important as outcome in the traditional sense after surgery for SUI. All patients should be told about the natural history of urinary function recovery, ideally prior to prostate cancer treatment, and then undergo conservative measures to hasten urinary continence. About 10% of patients will, unfortunately not regain continence and about half of these will seek treatment [3].
All patients should have already undergone a course of pelvic floor muscle exercises or physical therapist-direct pelvic floor muscle therapy . Prior to offering surgical therapy, patients should be beyond an appropriate period to make sure continence will not return (usually 6–12 months) and continence level should be at a plateau. Furthermore, other pathology including overactive bladder or anastomotic stenosis should be ruled out or treated. Once it is determined that the patient is suffering from intractable SUI or stress-predominant SUI and is significantly bothered, surgical management should be offered to the patient.
61.2 Surgical Management
After surgical treatment for stress urinary incontinence is chosen by the patient and his provider, the patient must be counselled on the myriad of treatments available, their risks, outcomes, complications, and alternatives available [4]. Furthermore, some surgical modalities are better suited for specific patients based on the degree of incontinence, history of radiation therapy, history of anastomotic stenosis – treated or not, and the quality of the bladder. Another consideration is the general health of the patient because most surgical procedures require regional or general anesthesia .
61.3 Urethral Bulking Agents
The least invasive treatment for SUI consists of urethral bulking agents [5]. Urethral bulking consists of injecting bulking material via an injection needle introduced though a cystoscope. The injections are typically sub-epithelial near the location of the bladder neck. Multiple types of injectable material have been used. Collagen was one of the first materials used, but because it is absorbable, multiple treatments were needed over time to maintain efficacy. Unfortunately, efficacy was only seen in less than 20% of patients with a large proportion of the responders needing retreatment [6].
Subsequently, non-absorbable agents have been used (eg. Carbon-based gels) for urethral bulking [5, 7]. The rationale for these was to decrease the number of times that patients would need to be retreated. No large series exist, but the consensus among those that perform these procedures is that these agents also need to be retreated and their results are essentially the same as that with collagen.
Urethral bulking agents are not considered durable treatment for SUI, but they can be used if patients are aware of their low efficacy and their high rate of retreatment. They can also be used in patients who are not candidates for regional or general anesthesia or as a bridge to definitive treatment. Furthermore, the use of bulking agents does not preclude the use of other surgical procedures.
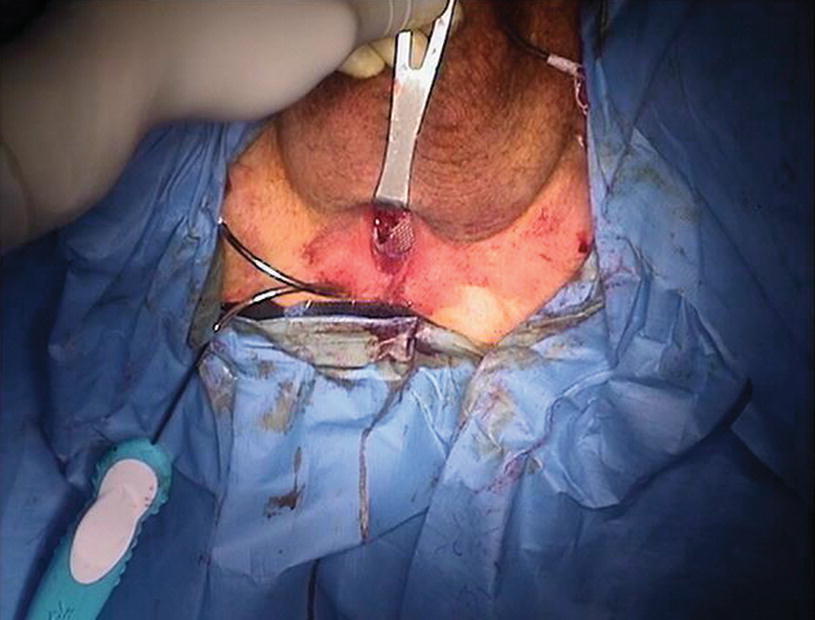
61.4 Male Slings
Male slings are treatment for SUI that consists of placing a mesh underneath the urethra usually though a perineal incision [5, 8]. Male slings are generally either fixed, with transobturator or quadtratic slings being the most common current variants, or adjustable. The most common male sling, the transobturator male sling consists of mesh “arms” that become embedded in native tissue and are therefore considered fixed. Adjustable male slings are those that contain mechanisms that allow the slings to be tightened after initial placement. These slings, in theory, allow for better efficacy because they can be tightened in patients who are unhappy with continence results after the procedure. Mesh material is generally large-pore polypropylene but can also be silicone or other materials.

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree