div class=”ChapterContextInformation”>
10. Surgical Reconstruction of Penile Urethral Strictures: Single-Stage Procedures
Keywords
Penile strictureOne-stage urethroplastyOral mucosal graftGlue10.1 Introduction
The aetiology of penile urethral strictures include many causes, with a significant differences between developing and developed countries. In developing countries, post-infectious (Neisseria gonorrhoea) strictures still represent the cause of the majority of penile strictures, but post-instrumentation/catheter related strictures are increasing [1–3]. Developed countries showed a decrease in infective aetiology and an increase of catheter, instrumentation, idiopathic causes, lichen sclerosus (LS) and failed hypospadias repair (FHR) related strictures [4–6].
Penile urethral strictures are managed by using a one or two-stage repair. Complete obliteration of the external urethral meatus with wood-hard fibrosis extending into the penile tract or complex strictures associated with fistulae, scarring, chordee, abnormal meatus, small glans and deficiency of the dartos layer are better managed by using a staged reconstruction [7–9]. In one-stage penile urethroplasty the use of a flap or graft is still a debated issue [10]. In recent years, the use of a graft for anterior urethroplasty has become the most popular option for any augmentation tissue repair [10]. However, the current literature is too limited to answer the question of whether a flap or graft is superior for one-stage penile urethroplasty, including only a collection of retrospective series of patients or meta-analysis studies with a variable definition of the stricture recurrence and successful outcomes [10]. The success rates of penile urethroplasty using a flap or graft are reported to be similar [10].
The aim of this chapter is to describe the history and evolution of the surgical reconstruction of penile urethral strictures using single-stage procedures, including the new surgical innovations.
10.2 Historical Background
10.2.1 History and Evolution of Penile Skin Flap Urethroplasty
In 1968, Orandi described a new one-stage urethroplasty utilizing the principles of pedicled skin grafting for repair of penile and bulbar urethral strictures [11]. A skin incision is made at the level of the stricture, the urethra is ventrally opened in the midline and the desired penile skin graft is tailored according to the stricture length and inverted and sutured over the urethral defect [11]. The inverted skin graft will have ample mobility despite its long and wide attachments to the dartos fascia [11]. In 1972, Orandi reported the results of this original technique on 14 patients showing that one patient developed stricture recurrence and two patients grew hair and formed stones over the grafted area, requiring transurethral removal and revision [12].
However, the technique described by Orandi is not completely original because in 1962 Leadbetter et al. referred to a method of letting in an island of skin based on a pedicled dartos fascia to repair penile strictures in children [13].Turner-Warwick in 1972 and Blandy in 1975 described some important changes to Orandi’s technique [14, 15]. In 1985, Webster et al., reported the results on 11 patients treated by using vascularized island skin flap urethroplasties suggesting that the results appear to be excellent when the procedure is used for penile stricture repair, but the use of vascularized skin flap urethroplasties for repair of bulbar and membranous strictures has been complicated by pseudodiverticula and stone formation [16]. Anyway, for many years, the Orandi’s technique represented the milestone for treatment of penile urethral strictures.
In 1983, Quartey described an original technique for a single-stage urethroplasty using a transverse distal penile-preputial cutaneous island flap, similar to the technique described by Duckett for hypospadias repair [17]. In 1985, Quartey reported the results of this technique in 27 patients with stricture recurrence in six patients and diverticulum formation in five [18]. In 1997, Quartey fully described the microcirculation of penile and scrotal skin as anatomical basis of this technique [19]. The Quartey’s technique become one of the most popular procedures for urethral stricture repair used in African countries.
In the 1980s and 1990s, the use of a penile skin flap for single-stage penile urethroplasty was the most commonly used technique and Hinman Jr. fully described the anatomical and vascular basis of these techniques [20].
In 1993, McAninch described a new technique for one-stage repair of long penile and peno-bulbar urethral strictures using a circular fasciocutaneous penile skin flap based on Buck’s fascia as the major vascular supply [21]. The surgical anatomy and the harvesting flap technique was fully described by McAninch and Morey in 1997 and 1998 [22, 23]. In 2008, Whitson et al. reported the long-term efficacy of distal penile circular fasciocutaneous flap for one-stage repair of complex anterior urethral strictures [24]. A total of 124 patients were included in the study with a median follow-up of 7.3 years (range 1 month to 19.5 years), median stricture length was 8.2 cm (range 0,5–24), and at 1, 3, 5 and 10 years the overall success rates were 95%, 89%, 84% and 79%, respectively [24]. Smoking, failed hypospadias repair and stricture length >7 cm were predictive of failure [24]. Hematoma, urinary extravasation, penile skin necrosis, decrease in penile sensation were the most frequent reported complications [24].
The McAninch’s technique , even now, represents one of the most popular procedures for the repair of long complex penile or peno-bulbar urethral strictures.
10.2.2 History and Evolution of Penile Graft Urethroplasty
The use of free skin grafts for single-stage anterior urethroplasty was reported many years before the use of pedicled skin flaps. In 1953, Presman and Greenfield described the use of a free skin graft for reconstruction of the perineal urethra in one patient, with successful outcome [25].
In 1963, Devine et al. started in popularizing the use of free full-thickness skin grafts for penile and bulbar urethroplasty, describing original techniques [26–29]. The Devine and coworker’s articles represent a milestone in the history and evolution of the use of penile free skin grafts for anterior urethroplasty.
In 1984, Webster et al. reported excellent results in 18 cases in which a penile skin donor site was.
used and three failures in which the full thickness grafts were raised from the inner aspect of the upper arm, and suggested caution when extra penile skin is used for such repairs [30].
For many years, penile skin was the preferred tissue suggested for single-stage urethroplasty.
A great evolution in the techniques using free grafts was in 1993, when El-Kassaby et al. reported the first series of 20 adult patients with penile (12) or bulbar (8) urethral strictures treated by transplanting an oral mucosa graft, with high success rate [31].These authors reported that they started using this technique in 1975, without suggesting why they decided to use the oral mucosa, but they had known and reported an article on the use of oral mucosa in ophthalmology [31]. We can suppose that this article was the first after the pioneering report from Kirill Sapezhko in 1894 [32]. However, it would be interesting to know why these authors started using this innovative surgery in 1975 and only described it in 1993, 18 years after their first application [31]. Nevertheless, this report represents a milestone in the history of the use of oral mucosa for urethroplasty. In 1996, Wessells and McAninch, reported the outcomes on 35 patients who underwent penile or bulbar urethroplasty using free grafts (penile skin, oral mucosa, bladder mucosa) and suggested that oral mucosa provided higher success rate when compared to penile skin [33].
A great evolution on the use of oral mucosa graft for penile urethroplasty started in 1996, when Barbagli et al. first described a dorsal approach to the urethral lumen for reconstruction [34]. As far as the penile urethroplasty is concerned, the most important improvement of the Barbagli’s dorsal approach was suggested by Asopa et al. in 2001 [35]. These authors described a new fascinating penile single-stage reconstruction utilizing the Snodgrass, Hayes and Malone techniques used for hypospadias repair [35–37]. On this technique, the penile urethra is fully exposed, and the urethral plate is longitudinally incised to create a wide window for oral mucosal graft placement [35]. In 2016, Barbagli et al. described a new modification of the Asopa’s technique for penile urethroplasty using a new glue for graft fixation inside the incised urethral plate, reporting an 85.7% success rate [38].
10.3 Single-Stage Penile Skin Flap Urethroplasty
The decision to perform a penile pedicled skin flap urethroplasty or free oral mucosal graft is based on surgeon preference and background.
The use of pedicled vascularized penile skin flap is mainly suggested in patients with penile urethral strictures showing a narrow and fibrous urethral plate not ideal for a transplant of free graft. In patients who developed recurrent stricture after Asopa’s free graft urethroplasty , the use of a vascularized penile skin flap should be the preferred choice. In patients with LS genital skin disease the use of a penile flap should be avoided. In patients with failed hypospadias repair, the dartos fascia will be fibrous, thin and not adequate for vascular support to the skin island flap.
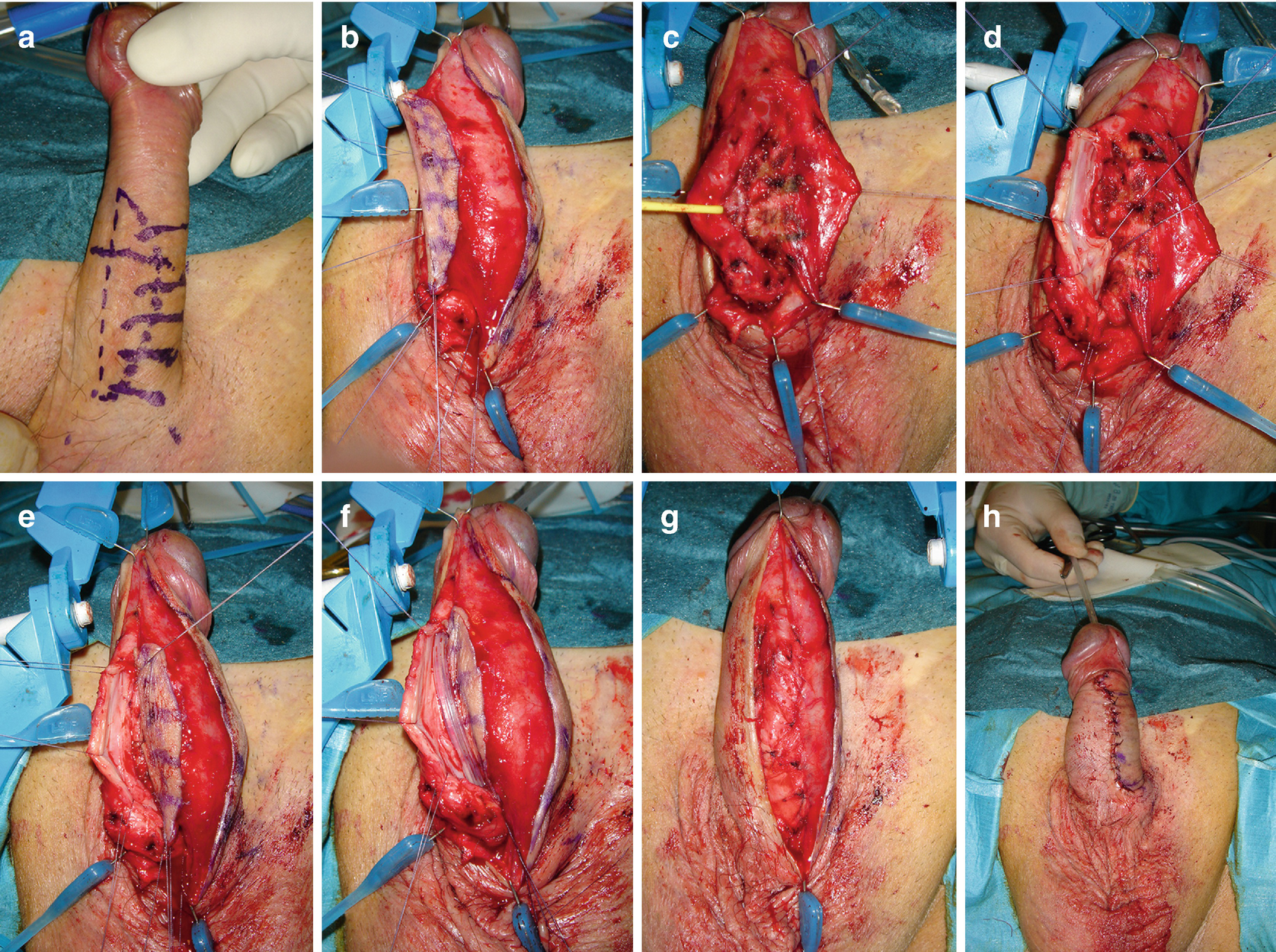
(a) The site of stricture is identified and the penile skin incision is outlined showing the skin flap and it vascular support. (b) The penile skin island is developed based on dartos fascia. (c) The penile urethra is fully dissected form the corpora cavernosa. (d) The urethra is rotated to expose the dorsal surface and fully opened. (e) The penile skin island is moved over the corpora cavernosa, next to the urethral mucosa. (f) The penile skin island is fixed to the corpora cavernosa and sutured to the urethral mucosa margin. A Foley 12 Ch. silicone catheter is inserted. (g) The urethra is fully rotated over the skin flap and sutured to the corpora cavernosa. (h) The penile skin is closed over the urethra

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree