12
Transconjunctival Lower Blepharoplasty
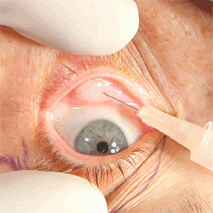
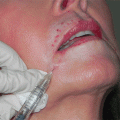
In the appropriate patient, transconjunctival lower blepharoplasty offers several advantages over transcutaneous lower blepharoplasty, including the lack of a skin incision, less ecchymosis, lack of orbital septum incision, and avoidance of denervation of the orbicularis oculi muscle. This technique, however, may be associated with increased incidence of postoperative chemosis and posterior lamellar cicatricial changes. Additionally, it must be modified to address lower lid laxity and midface descent and is not appropriate in patients with excess skin. As such, the transconjunctival approach to lower blepharoplasty is best performed in younger patients who do not have lower lid laxity, excess lower lid skin, or significant midface descent.
PREOPERATIVE EVALUATION
Evaluation of the lower eyelid blepharoplasty patient is of paramount importance. Those with unreasonable expectations or patients with whom the physician is not able to establish good rapport are poor surgical candidates. Patients with a bleeding diathesis or who take medications with anticoagulative properties are at higher risk for postoperative retrobulbar hemorrhage and possible irreversible vision loss. It is recommended that the patient consult with the prescribing physician regarding the safety of stopping anticoagulants. Poorly controlled hypertension also puts the patient at increased risk of a postoperative hemorrhage. A patient’s medical history will dictate whether he or she is a candidate for office-based surgery or requires monitoring by anesthesia personnel. General anesthesia is rarely indicated for lower blepharoplasty and is associated with vasodilatation and increased bleeding risk, but it may be an option in the rare patient with severe anxiety.
Patients with dry eye must be counseled that they are at increased risk of postoperative dry eye, particularly in the immediate postoperative period. This is especially important for post-LASIK patients, whose corneal sensory nerves have been transected, predisposing them to postoperative dry eye. It is recommended to wait a minimum of 6 months after LASIK surgery before performing blepharoplasty. Patients who have previously undergone LASIK should be counseled that blepharoplasty may also affect their refraction and lead to additional need for corrective lenses, contact lenses, or surgical enhancement.
Other medical conditions, such as thyroid disease, also need to be considered in evaluating patients for blepharoplasty. Patients with thyroid-associated orbitopathy should demonstrate stability of their ocular manifestations for 3 to 6 months before surgery.
Preoperative photos should be taken to document the patient’s preoperative appearance. Full-face and oblique photos are particularly useful. Side photos may also be taken. It is important to document the patient’s preoperative vision, in the event that the patient complains of decreased vision postoperatively. Slit-lamp examination should be performed to assess any corneal changes from dry eye. Although it is not always reliable, the basal secretion test may be used to document dry eye. Bell’s phenomenon (upward rolling of the eyes during forced closure) should be evaluated as this may provide additional protection against postoperative corneal exposure. The MRD2 (distance from the corneal light reflex to the lower lid margin) and preexisting lagophthalmos should also be documented.
Preoperatively, the surgeon should evaluate the amount of excess fat in each of the three lower lid fat pads. Occasionally, only the nasal fat pad will require debulking, but more frequently, debulking of the nasal and central fat pads is necessary. Some patients will require debulking of all three fat pads.
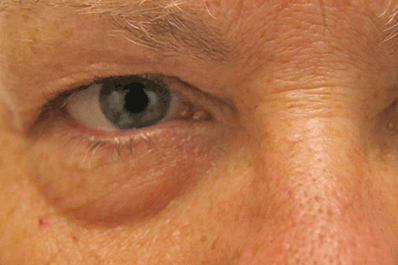
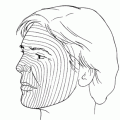
Figure 12-1. Ideal candidates for transconjunctival lower blepharoplasty should have lower lid fat prolapse with minimal lower lid laxity, lower lid excess skin, or midface descent.
Lower lid laxity may be evaluated by the lower lid distraction test. The lower lid is pulled away from the globe, and the distance from the globe to the lower lid margin is estimated. If the lid can be pulled 8 mm or more from the globe, lateral canthal tightening will likely be necessary. Patients with excessive lower lid skin may be better served by combining lower blepharoplasty with laser skin resurfacing or a pinch excision of lower lid skin, or by performing a transcutaneous blepharoplasty. Patients should also be examined for preexisting lower lid retraction. If sclera is visible between the limbus and the lower lid (scleral show), lower lid retraction is present. Patients with lower lid retraction may benefit from posterior lamellar grafting, as described in Chapter 16.
SURGICAL TECHNIQUE
Choice of instrumentation
Dissection may be performed with scissors/bipolar cautery, monopolar cautery, or CO2 laser depending on surgeon preference. Bipolar cautery is acceptable for use with pacemakers. Monopolar cautery offers the advantage of simultaneous cutting and coagulation, but it cannot be used in patients with pacemakers. The advantages of CO2 laser include compatibility with pacemakers and implantable defibrillators and decreased intraoperative bleeding, but it is associated with increased collateral tissue damage, which may cause increased incidence of wound dehiscence. Additionally, CO2 lasers require further preparation and equipment (covering of the OR windows, spectacle or goggle use by the OR team, laser masks to avoid plume inhalation, moist towels around the field to decrease the risk of fire, and antireflective instruments).
Anesthesia and skin marking
Transconjunctival lower blepharoplasty may be performed in the office setting with local anesthesia.
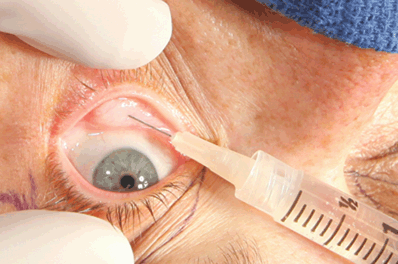
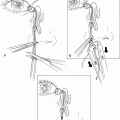
Figure 12-2. The transconjunctival approach is then used to inject approximately 1mL of lidocaine 2% with epinephrine into each of the nasal, central, and temporal fat pads on each side, after topical anesthetic drops are placed in both eyes.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree