Introduction
Essential vitamins and trace elements, which are globally known as micronutrients (MNs), are fundamental to metabolism ; they function as structures of enzymes or as their cofactors. After major burns, their requirements are influenced by the oxidative burst, metabolic state, and the additional nutritional needs linked to extensive skin repair. The first publications about elevated vitamin requirements go back to the 1940s and trace elements to the 1960s.
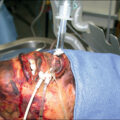
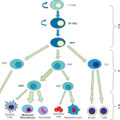
Oxidative stress characterizes major burns: it is defined as the imbalance between the production of reactive oxygen species (ROS) and reactive nitrogen species (RNS) and the antioxidant defenses, the latter being largely depending on MNs. , ROS are by-products of biologic systems and are required for numerous intramitochondrial and cellular processes. When ROS production increases beyond endogenous defenses, ROS start showing harmful effects on important cellular structures like proteins, lipids, and nucleic acids. In critically ill patients, this results in multiorgan failure ( Fig. 21.1 ).
Pathophysiology of oxidative stress in major burns.
The prooxidant and antioxidant balance may be disrupted and confer enhanced oxidative stress, which may result in organ failure.
Some MNs, such as ascorbic acid (AA) and α-tocopherol, act as direct antioxidants in the circulating compartment with plasma glutathione peroxidase (GPX3). The most important antioxidant enzymes include superoxide dismutase (SOD), catalase (CAT), the glutathione peroxidase (GPX) family, and the thioredoxin system: these enzymes depend on the trace elements copper, selenium, manganese, zinc, and iron. The B vitamins contribute to neutralization of reactive oxygen species in the mitochondria via nicotinamide adenine dinucleotide phosphate (NADP) and flavin adenine dinucleotide (FAD).
Thermal injury induces an intense and rapidly progressive oxidative stress that outperforms endogenous defenses. ROS are first generated from the burned skin but rapidly thereafter from the activated macrophages and neutrophils, as well as by the release of histamine, which activates xanthine oxidase. Oxidative stress aggravates the inflammatory response to injury by activating nuclear factor–kappa B : the control of this step involves several MNs, with selenium, AA, α-tocopherol, and zinc first in line. The resulting redistribution of the endogenous MNs further reduces antioxidant capacity. Already in 1975, Van Rij et al. showed in rats with 30% total body surface area (TBSA) burned that zinc-65 was rapidly taken up by liver, spleen, kidney, and wounds, with a decrease in the brain, muscles, and bone: this type of redistribution would later be called inflammatory-mediated redistribution of MNs because it also affects selenium and iron. This type of redistribution pattern has been confirmed by several authors. ,
Copper and zinc with selenium are linked in cytosolic defense against RNS and ROS: iron adds to the complexity as it is prooxidant. The plasma activity of copper-zinc-SOD is decreased after major burns. Furthermore, ceruloplasmin (Cp) plays a role as a neutralizer of ferrous entities. Selenium is mainly active through the antioxidant family of GPx enzymes, which depend on selenium for activity, but also through the large family of selenoproteins. Plasma GPX3 levels are the first to change, decreasing within hours after burn injury. α-Tocopherol also decreases rapidly, and in absence of supplements this decrease is associated with increased lipid peroxidation.
Antioxidant and immune defenses are tightly coupled, and copper, selenium, and zinc modulate both the innate and adaptive immune response through their availability. In particular, zinc deficiency alters the activity of monocytes and polymorphonuclear, natural killer, B, and T cells: the latter are particularly susceptible to changes in zinc status. Copper-dependent Cp is an acute-phase reactant protein, a ferroxidase that converts ferrous iron to its less reactive ferric form to facilitate binding to ferritin. Low Cp favors oxidative reactions and low iron levels and inflammation are tightly associated, as shown by Dubick et al. The body has developed strong defense mechanisms, including Cp, against this essential but potentially prooxidant trace element. Table 21.1 provides a summary of the most important functions of the MNs that are challenged by major burns.
Table 21.1
Summary of the Principal Trace Elements and Vitamin Functions Challenged During Major Burns
Completed functions are summarized in the guidelines. Berger MM, Shenkin A, Schweinlin A, et al. ESPEN micronutrient guideline. Clin Nutr. 2022;41:1357-1424.
| Most Challenged Functions in Burns | |
| Copper |
|
| Selenium |
|
| Zinc |
|
| Iron | Functional component of heme, participating in oxygen transport (hemoglobin, myoglobin), oxygen metabolism (catalases, peroxidases), cellular respiration, and electron transport (cytochromes) |
| Vitamin C |
|
| Thiamine—B 1 |
|
| Vitamin B family |
|
| Vitamin A |
|
| Vitamin D |
|
| Vitamin E |
|
| Vitamin K | Enzyme cofactor activity necessary for the activation of vitamin K-dependent proteins coagulation factor: C, S, M, Z, factors VII, IX, X and prothrombin |
Trace elements
Clinical importance of trace elements has been consolidated during the past decades. Among them, four have been shown to be of special importance in burns: copper, iron, selenium, and zinc, and possibly chromium. These elements are involved in antioxidant and in innate and adaptive immune defenses: their deficiency largely contributes to the classical complications observed after major burns, such as persistent inflammatory state, multiorgan failure, sepsis, and delayed wound healing. The trace element status alterations in major burns differ from other trauma and critically ill patients by the magnitude of the changes and their mechanisms. Here we address the changes affecting the blood compartment, exudative and urinary losses, their role in inflammation and antioxidant defenses, and, finally, some considerations about trace elements therapy.
Blood concentrations
Low blood concentrations (serum or plasma) of several trace elements have been repeatedly reported since the 1970s and support recommendations to determine and monitor blood levels after major burns and to orient repletion in cases of evident deficit. Trace element deficiencies arise primarily due to extensive exudative losses and repeated surgeries and burn baths commonly administered as part of burn injury management. ,
-
Copper: Very low levels of copper have been shown repeatedly after major burns. The circulating concentrations vary inversely with the size of burns. , Such low levels reflect deficiency because, different from all other trace elements which decrease with inflammation, copper and it carrier protein Cp increase during an inflammatory response, with Cp being upregulated by interleukin (IL)-1: this increase does not occur in major burns due to the acute exudative losses causing depletion. Further wound treatment is often carried out with silver products (silver sulfadiazine and silver-containing hydrofiber dressings): silver penetrates in the body and antagonizes copper, contributing to its decrease along with Cp. It is important to note that copper and iron metabolism are tightly linked.
-
Selenium: Blood levels of selenium decrease very early after major burns due first to an inflammatory redistribution and then to the depletion by the large exudative losses. Selenium remains low for several weeks. This is associated with a nearly immediate depression of the activity of GPX-3.
-
Zinc: Blood zinc levels decrease within the first hours after major burns and remain very low for weeks, also as the result of the inflammatory redistribution associated with inflammation and accompanying high losses.
-
Iron: After major burns, ferremia decreases nearly immediately and remains low for prolonged periods ; as for selenium and zinc, the initial drop results from acute inflammation and redistribution and is accompanied by an increase in ferritin. Thereafter, iron status is compromised by hemorrhagic losses during surgery but also with exudative losses. The iron depletion combined with inflammation causes persistent anemia.
-
Chromium: Animal studies show that chromium concentrations decrease in the livers of burned rats, becoming nondetectable after a few days, and in muscle very early on and for several days. Simultaneously, urinary chromium losses increase. The changes in chromium concentrations were associated in animals with early hyperglycemia, hyperinsulinemia, and increased secretion of stress hormones. Data from diabetic patients and patients on parenteral nutrition show that chromium deficiency contributes to insulin resistance. Data from the Lausanne lab confirmed that chromium is lost in exudates, along with molybdenum and manganese ; clinical significance must be confirmed.
-
Aluminum: The impact of this nonessential, potentially toxic element remains debated; investigations are few but indicate deleterious consequences on bone metabolism. Large aluminum intakes from albumin were a problem for several years. Aluminum loading has been reported in an adult burn cohort, which was investigated with bone biopsies. In severely burned pediatric patients, aurin tricarboxylic staining of bone biopsies for aluminum accumulation at the bone surface have been negative. The aluminum contamination of parenteral products has not been seriously addressed since the US Food and Drug Administration recommendation in 1986, and because there is no real treatment in case of toxicity, suspicion should be maintained and blood levels checked in cases of neurologic and bone pain, particularly in children. Data from the Lausanne lab confirmed that serum levels are above reference levels in adults, and aluminum is detected in the exudates.
Exudative and urinary losses
In healthy subjects, trace elements are lost through urine (selenium mainly) and/or feces (copper, iron, zinc), with extremely little being lost to sweat. Increased losses were suspected to occur after burns, but the demonstration of exudative losses from the burn wound is a two-step story in Lausanne first with balance studies in 1992 , and recently confirmed by a vacuum collection method.
-
Copper: Urinary losses were shown to be above normal in studies in the 1980s, , being particularly observed during parenteral nutrition, although excreted amounts were lower than the infused quantities. The main losses of copper have been shown to occur through exudates during the open wound phase after major burns; such losses occur similarly in children.
-
Selenium: The reduction of urinary excretion shown in burns already in 1984 reflect a deficiency, with selenium being retained. The selenium depletion was explained by significant exudative cutaneous losses, shown in the frame of a balance study and recently confirmed.
-
Zinc: Urinary losses of zinc are initially above normal, as in other major trauma, but then decrease. Significant losses occur through exudates, reaching about 10% of body content during the first week.
-
Iron: Recently, a study investigating a large palette of trace elements showed that, in patients with 27% TBSA burns, iron was lost in large amounts with exudates even in the absence of active bleeding.
It is important to note that, along with these four elements, others are also lost but have not been associated with clinically detectable alterations. Two important electrolytes, magnesium and phosphorus (Pi), are also lost with the exudates in substantial amounts, sufficient to explain the high requirements during the early phase of burns.
Vitamins
The first deficiencies described in major burns in the 1940s, were ascorbic acid (AA = vitamin C), and the B vitamins: later cholecalciferol (vitamin D), and alpha-tocopherol (vitamin E) were reported to be depleted in burned patients.
The most recent demonstration of higher vitamin needs comes from an industrial explosion in 2015 that injured 499 people: the 61 worst cases (burns >20% TBSA) were transferred to mainly to 2 burn units, one having a MN supplementation protocol and the other not (control) (see Table 21.2 ). In the ICU with micronutrient protocol, wound infections were significantly reduced (30.0% vs. 77.4%, P <.001), as was sepsis (13.3% vs. 41.9%, P =.021), and hospitalization days (52 vs. 77 days, P =.025). The supplement did not include all vitamins, but doses compare with those proposed by the European Society for Clinical Nutrition and Metabolism (ESPEN) guidelines for critically ill patients with high needs ( Table 21.2 ).
Table 21.2
Recommended micronutrient intakes for enteral nutrition (ESPEN standard and high requirements) , doses administered by Chen et al (color-dust explosion) , in CHUV protocol , and proposed intakes for the acute phase in major burns: these doses are intended for burns >20% during the first 2-4 weeks according to burn size.
| ESPEN enteral standard needs in 1500 kcal/d | ESPEN values for patients with high needs | Taiwan color dust | CHUV burns 2020 by IV and enteral routes | Proposed major burn micronutrient protocol | |
|---|---|---|---|---|---|
| TRACE ELEMENTS | |||||
| Copper | 1–3 mg | 1–3 mg | na | IV 4.77 mg | IV 4.5 mg |
| Selenium | 50–150 mcg | 200 mcg | na |
|
IV 300 mcg |
| Zinc | 10–20 mg | 20 mg | na | IV 45.5 mg | IV 40 mg |
| Iron | 18–30 mg | 30 mg | na | IV 1.10 mg (20 μmol) | IV 1.10 mg (20 μmol) |
| VITAMINS | |||||
|
900–1500 mcg (1500–2500 IU) | 1500 mcg (2500 IU) | 1980 mcg (6600 IU) |
|
2000 mcg (3300 IU) |
| D3—Cholecalciferol | 25 mcg | 30 mcg | 10 mcg (400 IU) | IV: 5.5 mcg (220 UI) | 4000 mcg (160,000 IU) |
| E—α -tocopherol | 15 mg | 40 mg | 20 mg |
|
EN: 100 mg |
| K—Phylloquinone | 120 mcg | 120 mcg | na | 10 mg/week | 10 mg/week |
| B 1 —Thiamine | 1.5 mg | 100 mg | 100 mg | IV: 3.5 + 100 mg | 200 mg |
| B 2 —Riboflavin | 1.2 mg | 10 mg | na | 4.14 mg | 10 mg |
| B 3 —Niacin | 18 mg | 40 mg | na | 46 mg | 40 mg |
| B 5 —Pantothenic acid | 5 mg | 7.5 mg | na | 16.15 mg | 20 mg |
| B 6 —Pyridoxine | 1.5 mg | 7.5 mg | 200 mg | 4.53 mg | 20 mg |
| B 7 —Biotin | 30 mcg | 75 mcg | na | 69 mcg | 75 mcg |
| B 9 —Folic acid | 330–400 mcg DFE | 500 mcg | na | 414 mcg | 500 mcg |
| B 12 —Cyanocobalamin | >2.5 mcg | 7.5 mcg | 2000 mcg | 6 mcg | 6 mcg |
| C—Ascorbic acid | 100 mg | 200 mg | 100 mg |
|
1 g |
The MNs from enteral feeding are not counted in the CHUV cocktail, but complete the daily supplements.
CHUV, Centre hospitalier universitaire vaudois; EN, enteral nutrition; RAE, retinol activity equivalent.
Vitamin C
In addition to its essential role in multiple metabolic pathways, AA is a potent antioxidant. Low AA plasma concentrations are present in all burn patients due to consumption during the antioxidant process but also to inflammation, which results in redistribution from the circulating compartment as soon as C-reactive protein (CRP) exceeds 10 mg/L. ,
The antioxidant properties of AA on the endothelium and impact on microcirculatory flow have been used to reduce fluid resuscitation requirements. In 2000, after animal testing, Tanaka et al. showed that megadoses of AA (66 mg/kg/h) during the first 24 hours significantly reduced fluid resuscitation volumes. This finding attributed was confirmed in an ovine model of 40% TBSA burn injury : AA prevented the 4-fold increase of plasma TBAR (thiobarbituric acid reactive substances) in burned sheep. Similar results were confirmed in a rat burn model in 2010. Studies in severely burned rats showed that high-dose AA normalized malondialdehyde (MDA) levels ( P <.01) and attenuated changes in the levels of CAT and SOD. Only one randomized controlled trial (RCT) has been conducted since these early results in India, including 30 patients who confirmed the 30% reduction in fluid resuscitation volumes. In 2019 a large retrospective Japanese cohort study confirmed the effect of high-dose AA on fluid resuscitation in severe burn patients. The study tested different thresholds of AA: out of 2713 eligible patients, n=157 were categorized into the vitamin C group, with the others serving as controls ( n = 2556). Propensity score matching (1:4) enabled comparing the 157 high-dose patients (>10 g/day threshold) with 628 control patients for analysis, and showed that high-dose AA was associated with reduced in-hospital mortality (risk ratio, 0.79; 95% confidence interval [CI], 0.66 to 0.95; P =.006). The minimum threshold for effect was 10 g within the first 2 days of admission. In 2022 a scoping review including 10 publications confirmed these positive effects, and encouraged continued research.
Vitamin C is a normal skin constituent that is found in high concentrations in the dermis and epidermis, stimulating collagen synthesis and assisting in antioxidant protection against UV-induced damage; keratinocytes have a high capacity for vitamin C transport. Higher than standard daily intakes of AA are essential for tissue repair, especially for the synthesis of collagen, as it is an essential cofactor for lysyl hydroxylase, i.e., for collagen biosynthesis and tissue repair.
Thiamine (B1)
Thiamine diphosphate (ThDP) is the active form of thiamine: it is an essential cofactor in the Krebs cycle; that is, it is essential for adenosine triphosphate (ATP) production and carbohydrate metabolism, but also for amino acid metabolism. Thiamine serves as a cofactor in the Krebs cycle and for the oxidation of glucose, thus its need is related to the energy intake.
A study including 20 patients with major burns with blood samples on admission and days 1, 3, and 7 showed that serum thiamine levels increased significantly with thiamine 100 to 200 mg/day delivered to 6 of them ( P <.001). Increasing serum thiamine levels were inversely related to pyruvate and lactate levels, with both decreasing with higher thiamine. This study suggests thiamine supplementation is associated with a decrease in pyruvate and lactate levels. Further metabolic flux studies associated with thiamine supplementation are required to establish the optimal dose. Thiamine is also necessary for the lysyl oxidase function to form collagen.
Vitamins B 2 to B 12 —the B family
Investigations conducted in Boston in the 1940s showed major alterations of blood levels of thiamine (B 1 ), riboflavin (B 2 ), and niacin (B 3 ) in patients with burns greater than 20% TBSA. The B-complex vitamins act mainly as cofactors, with a major function in the metabolism of carbohydrates, fats, and protein. Riboflavin is involved as a coenzyme in oxidation-reduction reactions. Blood riboflavin is decreased after burn injury, and an increased need for riboflavin in burn victims has been shown. Folic acid (B 9 ) is depleted after burns, which may impair synthesis of DNA and RNA. Inadequate supplies of vitamin B 12 and the indispensable amino acid methionine impair folate utilization. Thus a deficiency of either of these nutrients can produce signs of folate deficiency. Vitamins B 6 and B 12 serve as coenzymes in the energy and protein metabolic process. Vitamin B 6 is involved in amino acid metabolism and vitamin B 12 in the catabolism of long-chain fatty acids. Their vitamin B requirements are proportionate to the substrate intake.
Vitamin A (retinol)
Vitamin A is a prohormone that stimulates epidermal turnover, increases the rate of reepithelialization, and restores epithelial structure ; it increases proliferation of keratinocytes and fibroblasts and decreases levels of degrading matrix metalloproteinases. But despite being essential for anabolism, this vitamin has a narrow therapeutic window, and high doses are discouraged. Retinoic acid and retinal are the 2 active forms of retinol. Therefore, vitamin A needs should be expressed in retinol activity equivalents (RAE), where 1 RAE = 1 mg = 3.33 IU. Toxicity is observed with chronic administration of doses greater than 25,000 IU (7500 μcg) and generally linked with the preformed vitamin A (but not precursor). The evidence for higher doses of vitamin A is currently limited.
Indeed, high-dose vitamin A may result in hypercalcemia as shown by a recent case report. A patient burned 55% TBSA was receiving daily the unit’s standard multi-MN supplement consisting of vitamin A 10,000 IU (3000 μcg), oxandrolone, vitamin C, and zinc (220 mg zinc sulfate is 50 mg elemental zinc). On hospital day 33, serum calcium levels were elevated and increased to 13 mg/dL (3.25 mmol/L) a few days later. Parathyroid hormone (PTH) and vitamin D levels were within the normal range, and urine analysis showed normal calcium excretion. Subsequent assessment of vitamin A levels revealed very high levels at 93 μcg/dL. Supplementation was discontinued leading to normalization of vitamin A levels, and the patient could be discharged 10 days later.
Vitamin D
Vitamin D has pleotropic effects, being involved in skeletal muscle, bone health, cardiovascular health, immune system, and cardiac and lung function. Deficiency is common in the general population and in critically ill patients. Low 25-hydroxyvitamin D (25(OH)D) has been observed in nearly all pediatric and adult burn patients. In blood, vitamin D is mainly transported by its specific binding protein and by albumin. Hence, a blood concentration of 25(OH)D is strongly correlated with serum albumin level, even more than with TBSA and burned surface. Blood levels decreased with inflammation.
Bone metabolism abnormalities have been the trigger for vitamin D research in burned children who develop a progressive deficiency as measured by circulating levels of 25(OH)D and 1,25-dihydroxyvitamin D 3 . Serum 25(OH)D levels remain low for prolonged periods up to 2 to 7 years postinjury. Analysis of skin biopsy samples for vitamin D3 precursors after exposure to ultraviolet-B light showed that the conversion of 7-dehydrocholesterol to previtamin D3 was reduced in children a mean of 14 months after the burn. Low serum 25(OH)D concentrations were also found. Another major factor, however, is the profound change in skin structure and quality. Burn scar and adjacent areas of unburned skin can only convert roughly 25% of its 7-dehydrocholesterol precursor to vitamin D 3 on exposure to sunlight. Moreover, the amount of 7-dehydrocholesterol substrate is significantly reduced in both burn scar and adjacent unburned skin. This indicates that, after burn injury, the skin cannot synthesize normal amounts of vitamin D regardless of the amount of sun exposure received. Thus a progressive deficiency in vitamin D will result without supplementation.
A retrospective study in 107 adult burn patients showed that 59% have very low levels compatible with deficiency (25(OH)D below 20 ng/mL). Multiple regression analysis showed that adequate vitamin D concentration was associated with a reduction in the incidence of sepsis (odds ratio 0.10, 95% CI, 0.01 to 0.88). The same groups showed in a cohort including 412 patients that those with the very low values (<20 ng/mL) during the first week had more days on vasopressors and kidney failure, fewer ventilator-free days (by day 28), and prolonged hospital stay.
Rousseau et al. have shown that daily standard dietary reference intake (DRI) vitamin D doses (400–600 IU; 10–15 μcg/day) resulted in hypovitaminosis; this seemed linked to a reduction of fibroblast growth factor-23 (FGF-23) activity. Further, they showed in 15 adult burned patients randomized to quarterly intramuscular injections that a high dose (200,000 IU; 5000 μcg) followed by daily oral supplements was followed by improved quadriceps strength at one year, which may be important during rehabilitation. No change in bone health was observed between groups.
How much do burn patients need? A standard multivitamin preparation dose (400 IU/day) has been shown to be insufficient to restore normal blood levels in children, which was confirmed in the Belgian adult cohort, using 400 to 600 IU/day. The aforementioned trial of 200,000 IU vitamin D 3 with daily oral calcium versus placebo showed significantly higher calcitriol levels in the vitamin D group at 1 year.
There is still considerable debate about the optimal vitamin D dosing regimen in different population and patient groups as therapeutic benefit in relation to target serum concentrations of vitamin D is uncertain. Different meta-analyses of the effects of vitamin D supplementation have been conducted: high-dose bolus administration is not convincing, but the initial bolus followed by continuous administration might be the better option. For additional discussion of vitamin D in burns, please see Chapter 20 .
Vitamin E—α-tocopherol
Patients with severe burns are characterized by increased oxidative stress and free radical activity and very low blood levels of antioxidants. Vitamin E is a fat-soluble antioxidant that scavenges peroxyl radicals and prevents the radical-mediated chain reactions of polyunsaturated fatty acids. A study in 35 severely burned patients of whom 18 received 100 mg α-tocopherol daily showed that this intervention was associated with a reduction of lipid peroxidation. Recently, it has been shown that the tissue storage of vitamin E in burned children decreases by half as early as 3 weeks after injury. Burned patients were entering the operating room with consistently low vitamin E status. Furthermore, it has been shown in burned children that a combination of antioxidants (vitamin C, vitamin E, and zinc for 7 days; average doses of 900 mgU/day, 400 IU/day, and 7 mgU/day, respectively) increased circulating vitamin E and decreased malondialdehyde levels (a marker of oxidative stress) and reduced wound healing time (p <.001).
Mechanistic studies in the ovine model of burn and smoke inhalation using deuterium-labeled vitamin E showed that the burn increased depletion of liver vitamin E, suggesting the tissue mobilization of vitamin E. These studies suggested that, in addition to depletion of vitamin E from the lung and liver, other tissues were also depleted. Given the hypermetabolic and hypercatabolic state and altered lipid metabolism in patients with burn injury, there is concern that depletion of adipose tissue vitamin E levels may entertain a significant level of oxidative stress, which might cause secondary organ failure.
The inflammatory response resulting from the oxidative stress further impairs the healing process. The aforementioned RCT in 32 burned children randomized to a combination of vitamins E, C, and zinc showed a significant reduction in healing compared with unsupplemented children. Furthermore, vitamin E has been shown to be beneficial in the treatment of wounds in a variety of models, including scar formation from acute surgical wounds. Summarizing all the investigations ranging from in vitro bench work to clinical studies investigating the influence of vitamin E in vitro, in vivo, and in the clinical setting, a 2022 review concluded to the benefit of enteral or parenteral vitamin E supplementation in preventing, mitigating, and even reversing the effects of thermal burn injuries, infection, and sepsis; this warrants further research.
Vitamin K
This vitamin is mainly involved in coagulation, and clinicians are reluctant to deliver vitamin K as major burn patients tend to rapidly develop a procoagulation status. Nevertheless, the risk of deficiency in burns is real with limited enteral intake, antibiotic therapy, and multiple surgical procedures. In severely burned pediatric patients, Jenkins et al. reported that 91% of the 48 children they studied demonstrated low circulating levels in the first month postburn. However, there was no relationship between serum vitamin K levels and prothrombin time, raising the question of clinical significance.
But vitamin K is also involved in bone metabolism, as osteocalcin, a γ-carboxylated protein produced by the bone-forming osteoblasts, is vitamin K dependent. Investigations in children have reports low-circulating osteocalcin in the first month after burn injury. Osteocalcin is used as a standard index of bone formation; it also has been shown to stimulate pancreatic insulin production and peripheral insulin sensitivity. It is undercarboxylated osteocalcin and not total osteocalcin that increases insulin sensitivity.
Micronutrient therapy
MN needs are usually expressed as DRIs, a concept that includes the recommended dietary allowance (RDA) but also safety and toxicity issues. The DRIs must always be covered, and they usually are with the provision of enteral nutrition, but this paragraph addresses the administration of higher amounts delivered to treat with supplements the acute depletion and higher antioxidant and metabolic needs. Of note, DRI doses are higher than the parenteral nutrition doses due to the low absorption of MNs (limited bioavailbility by oral route: only selenium is well absorbed). Currently, the practice of supplementing patients with vitamins and trace elements has become popular among American burn centers, with adherence of 92%, and is practiced internationally based on results from the RCTs showing reduction of infectious complications (especially bronchopneumonia ), better wound healing, and shortened length of stay. When prescribing MNs, their combined effects on multiple functions of the body should be considered for an integrated prescription ( Fig. 21.2 ). The intravenous (IV) route should be privileged during the acute phase to ensure optimal bioavailability.