Thermal Injuries
Kodi K. Azari
Christine Fisher
Galen S. Watchman
I. Definition/Introduction
Thermal injury to the upper extremity and hands remains a common clinical event. The severity of injury ranges from mild to catastrophic, and recovery from burn injuries must take into consideration functional as well as aesthetic outcomes. The cornerstones of upper extremity burn care are early excision and stable soft tissue coverage, splinting, early mobilization, and concerted rehabilitation.
II. Epidemiology
The upper extremity is involved in 89% of burns, with 1% of the population of Western countries sustaining a burn injury each year. One fourth of these patients will require medical care.
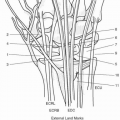
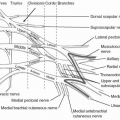
III. Anatomy
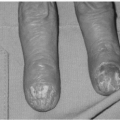
The dorsum of the hand is more likely to be involved in explosive or flame injuries while the palmar surface is more likely to be involved in friction burns and electrical injuries. The location of the burn wound is significant in the severity of the injury. The thin and mobile skin on the dorsum of the hand facilitates direct thermal effects on the tendons, blood vessels, and joints directly below the surface. The glabrous skin on the palmar surface of the hand has a thick epidermis and subcutaneous fat layer with a dense arrangement of fibrous septa connecting to the deep fascia to provide shock absorption and frictional stability.
IV. Pathophysiology
The duration of heat exposure and the temperature of the heat source determine the severity of a burn.
Thermal injury to the skin leads to protein denaturation, blood vessel coagulation, and increased capillary permeability, thus creating zones of necrosis, stasis, and impaired circulation.
Burns of 20% or more total body surface area (TBSA) result in generalized edema and swelling of nonburned tissues.
Fluid shifts from the intravascular to interstitial spaces cause edema, which can decrease perfusion.
Inadequate fluid resuscitation can lead to the conversion of zones of stasis to necrosis. Elevated tissue pressures due to swelling or constriction by circumferential full thickness burns can cause neurovascular injury to a limb.
Approximation of surface area of body burned: Head 9%, anterior chest and abdomen 18%, posterior chest and abdomen 18%, each arm 9%, each leg 18%, and genitalia 1%.
V. Evaluation
The evaluation of thermal injuries is based on the extent and severity of soft tissue injury. The extent of the injury may not be clear early as it is often difficult to determine the depth of the burn. All burned patients must be fully evaluated for concomitant systemic injuries and aggressively resuscitated. Referral to a specialized burn center has been well defined by the American Burn Association.
American burn association criteria for transfer
Partial thickness to full thickness burns greater than 20% TBSA in patients 10 to 50 years old.
Partial thickness to full thickness burns greater than 10% TBSA in patients less than 10 years of age or greater than 50 years of age.
Full thickness burns greater than 5% TBSA in patients of any age.
Partial or full thickness burns to hands, feet, face, eyes, ears, perineum, genitalia, and major joints.
High-voltage electrical injuries, including lightning.
Chemical burns.
Any patient with burns or concomitant trauma (e.g., fracture) in which the burn injury poses the greatest risk of morbidity or mortality. When the trauma poses a greater immediate risk, the patient may be treated initially in a trauma center until stable before transfer to a burn center.
Inhalational injury.
Circumferential burns to extremities or chest.
Patients with preexisting medical conditions that make burn resuscitation and recovery more difficult or present a risk of mortality (diabetes, chronic obstructive lung disease, and coronary artery disease).
Hospitals without qualified personnel or equipment for care of burn-injured children.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree