Tumors
Ed Athanasian
I. Benign Soft Tissue Tumors
Ganglion cysts
Definition
Ganglion cysts are the most common soft tissue masses in the hand. These lesions can be thought of in simple terms as a herniation of joint or tendon sheath synovial fluid outside the normal confines of the articular capsule or tendon sheath. These balloonlike structures are attached to the capsule or tendon sheath by a stalk. This can be narrow or broad based. The “stalk” can behave as if it has a one-way valve or a two-way valve. This concept helps to explain the variation in the size of ganglion cysts. At times, these lesions progressively enlarge in size. At other times, they can enlarge and then decrease in size. The cyst wall is comprised of fibrous tissue and does not have a true endothelial lining. Some ganglion cysts may arise from degenerated ligament as can be seen with dorsal carpal ganglion cyst arising from the scapholunate interosseous ligament. Common types of ganglion cysts include dorsal carpal ganglion cysts, volar carpal ganglion cyst, retinacular cyst arising from tendon sheath, and mucous cysts, which represent a specialized form of ganglion cyst arising from the distal interphalangeal (DIP) joint. Ganglion cysts can arise from any joint in the hand.
Pathogenesis
Mucous cysts arise at the DIP joint and extend dorsally or peripherally. On occasion they can be subungual. These are felt to arise in association with osteoarthritis, and osteophytes have been felt to be a significant factor contributing to their development. The excision of associated osteophytes is important during treatment in an effort to reduce recurrence risk.
Retinacular cysts may arise spontaneously, following tendon sheath injection, and following repetitive digit flexion against resistance. These cysts most commonly arise in close proximity to the A1 pulley but can be seen further distally.
Dorsal carpal ganglion cysts commonly arise in association with the scapholunate interosseous ligament. Mucoid degeneration of the ligament has been implicated as a source for the cysts.
Volar carpal ganglion cysts tend to arise radially in association with the extrinsic radio carpal ligaments or the scapho-trapezialtrapezoid ligament and can abut or even surround the radial artery.
Physical examination
Each type of ganglion cyst tends to arise in a common and predictable location. When suspected ganglion cysts are seen in unusual locations, the
initial differential diagnosis should include alternate lesions including solid neoplasms.
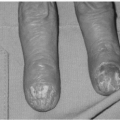
Mucous cysts tend to arise dorsally at the level of the DIP joints. This is usually seen in the setting of osteoarthritis and Heberden nodes may be present. The overlying dorsal skin may be thinned. There can be spontaneous clear drainage. Nail deformity can be seen in the form of grooving if the lesion affects the germinal matrix or dorsal nail fold. The lesions are firm and usually not tender. Infection can be seen following spontaneous drainage.
Retinacular cysts tend to arise palmarly in line with the proximal aspect of the flexor tendon sheath. These lesions are firm. They tend to be relatively small and often less than 5 mm. They can be central or eccentric. These lesions can be tender on deep palpation and patients frequently report pain with direct contact when gripping such as when holding a hammer.
Dorsal carpal ganglion cysts tend to arise somewhat radial to midline in the region of the lunate capitate articulation or scapholunate articulation. These lesions are variable in size. Wrist flexion may assist in the identification of lesions and allow easier palpation. Pain may radiate distally along the course of the finger extensors and symptoms can be accentuated by resisting digit extension. Pain may be made worse with active wrist extension and on occasion there may be limitation of active and passive wrist extension. These lesions typically transilluminate. If transillumination is not possible, alternate diagnoses should be considered. A positive Watson scaphoid shift test is usually present on examination.
Volar carpal ganglion cysts tend to arise in close proximity to the radial artery just proximal to the volar wrist flexion crease. These lesions are usually firm. Transillumination will help delineate the lesion and identify the course of the radial artery. Aspiration typically yields thick gelatinous clear or straw-colored fluid, which on occasion might be blood tinged.
Radiographs
Plain x-rays of mucous cysts will frequently demonstrate dorsal osteophytes and osteoarthritis. Radiographs of retinacular cysts as well as dorsal and volar carpal ganglion cysts are most commonly normal. On occasion arthritis can be seen in association with these lesions. MRI is generally not indicated when history and physical examination are consistent with ganglion cyst. On occasion occult dorsal carpal ganglion cysts can be better delineated by MRI or ultrasound. If a solid lesion is suspected, MRI may be useful.
Treatment
Mucous cysts
When lesions are small, asymptomatic, and not spontaneously draining observation is reasonable. Many patients simply wish to be assured that they do not have a solid tumor or malignancy. Large or symptomatic lesions may be aspirated; however, recurrence is frequent. Mucous cysts may be excised surgically although there is a substantial risk of recurrence as the underlying cause (osteoarthritis) remains. While marginal excision with debridement of osteophytes may be effective, simple excision of the base of the lesion at the level of the joint with joint debridement is also a very effective means of treating these lesions and appears to have a lower risk of skin and wound healing problems. Skin coverage is typically not required with the latter method.
Retinacular cysts
Small asymptomatic or minimally symptomatic lesions may be observed as long as physical examination findings are characteristic. Symptomatic central lesions may be aspirated in the office under local anesthesia with occasional recurrence. Eccentric lesions may be in close proximity to the digital vessels and nerves and may not be amenable to aspiration in the office. These lesions may be excised under local anesthetic in the form of marginal excision.
Dorsal carpal ganglion cysts
Asymptomatic lesions may be observed assuming physical examination findings strongly support the diagnosis of dorsal carpal ganglion cyst. These lesions should clearly transilluminate on examination. If this is not the case, further evaluation is necessary. Treatment alternatives include aspiration either in the office floor under ultrasound guidance. Recurrence may exceed 50% following aspiration. There is no clear benefit to the injection of corticosteroid, which on occasion may be associated with skin depigmentation and fat atrophy. Open marginal excision may be considered for multiple recurrent lesions with anticipated recurrence risk of approximately 5%. Recent studies have suggested that arthroscopic excision of dorsal carpal ganglion cysts may be an alternative effective means of treating these lesions.
Volar carpal ganglion cysts
Asymptomatic lesions can be observed. Symptomatic lesions can be treated similar to the dorsal counterpart, although the close proximity of the radial artery increases the risk of complications, including the development of a psuedoaneyrysm if the radial artery is injured. Open excision with identification of the radial artery generally results in low recurrence and minimal complications. Prior to excision, an Allen test should be performed to determine patency of the radial artery and arterial filling of the hand through the ulnar artery.
Giant cell tumor of tendon sheath
Giant cell tumor of tendon sheath is the most common soft tissue solid neoplasm that arises in the hand. Its pathogenesis has not been clearly defined. Multinucleated giant cells and hemosiderin laden macrophages are typically seen on histological assessment. These lesions arise in close proximity to joints. There can be direct extension into adjacent joints and ligaments. This may play a role in local recurrence following marginal excision. Most commonly, these lesions are firm and nodular. There is also a diffuse variant, which tends to spread proximally along flexor tendon sheaths and appears to be associated with a higher risk of local recurrence.
Physical examination
These lesions arise in close proximity to the proximal interphalangeal (PIP) and DIP joints but may be seen anywhere in the hand. Lesions may arise in association with the flexor tendon bursa in the palm. Rarely symptoms of nerve compression can be seen. The nodules can be quite firm and are typically not tender. The nodule may move with digit motion when adherent to tendons. These lesions do not transilluminate.
Radiographs
Giant cell tumor of tendon sheath is most commonly not visible on x-ray. Approximately 5% of lesions can cause a pressure erosion and sclerotic reaction
on adjacent bone. There are rare but well-described examples of direct bony invasion mimicking a more aggressive process. MRI typically demonstrates a nodular lesion with decreased signal seen in association with hemosiderin. The diffuse variant may mimic a proliferative synovitis with decreased signal. On ultrasound, they appear as solid, homogeneous hypoechoic masses with detectable internal vascularity
Treatment
The standard treatment for giant cell tumor of tendon sheath is marginal excision. The potential for a different neoplasm including a malignant tumor must be considered prior to proceeding with marginal excision of these lesions. This is particularly true for lesions arising in the carpal tunnel. The risks of soft tissue contamination in the event of a diagnosis of malignancy are great. During excision of a giant cell tumor of tendon sheath most commonly the lesion will have a Brown/yellow xanthomatous appearance, which is characteristic. If the lesion is in close proximity to a joint, careful inspection of the joint may demonstrate extension deep to the volar plate or in the region of the collateral ligaments. Local recurrence can be seen in approximately 30% of patients with reports of recurrence ranging from 5% to 50%.
II. Benign Bone Tumors
Enchondroma