| Symptomatic conjunctivochalasis affecting tear film and lacrimal outflow |
| Non-resolving chemosis after eyelid surgery |
| History of cicatrizing conjunctivitis (Stevens–Johnson syndrome/toxic epidermal necrolysis, mucous membrane pemphigoid, linear IgA disease, drug-induced) |
| History of any lower eyelid surgery (functional or cosmetic with details of the surgical approach) |
| History of thyroid-related orbitopathy or any orbital process causing proptosis |
| History of previous ocular medications used |
| Evaluation of ocular surface and tear film |
| Snap-back and eyelid distraction tests to assess lower eyelid laxity |
| Presence of punctal ectropion and stenosis |
| Lacrimal irrigation to rule out outflow obstruction |
Introduction
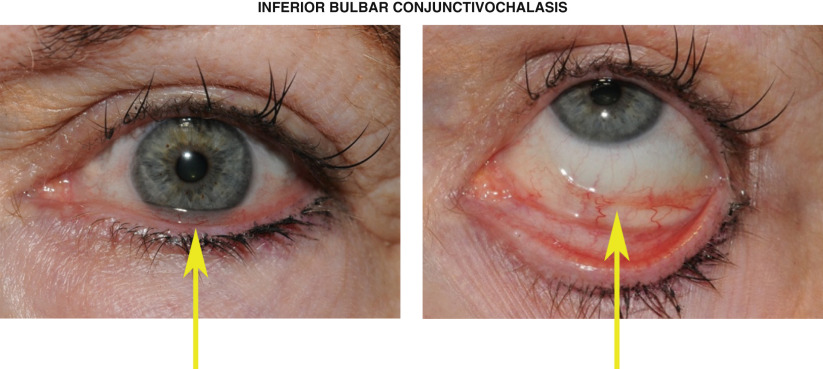
Conjunctivochalasis is characterized by redundant conjunctival tissue analogous to dermatochalasis of the eyelids. This condition is generally benign and age-dependent. Advanced conjunctivochalasis of the inferior bulbar conjunctiva can rest on the lower eyelid margin, cause ocular discomfort, tear film instability and obstruct lacrimal outflow ( Figure 52.1 , left panel). With blinking, the redundant inferior bulbar conjunctiva is continually chafed by the lower eyelid margin and becomes hyperemic ( Figure 52.1 , right panel). Conjunctivochalasis should be distinguished from chemosis, which is swelling of the conjunctiva associated with exudative fluid.
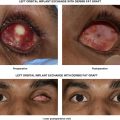
In the preoperative evaluation, diseases associated with cicatrizing conjunctivitis should be ruled out and, if appropriate, referred to an ocular surface specialist. Redundant conjunctiva of the caruncle and inferior bulbar conjunctiva can be seen with thyroid-related orbitopathy as well as any condition that causes proptosis. Lower eyelid surgery, in particular transconjunctival blepharoplasty, can be complicated by persistent chemosis. This condition is usually self-limited as the exudate resolves as the postsurgical inflammation diminishes. In a lax lower eyelid where tightening has been performed with undiagnosed conjunctivochalasis, this redundant conjunctiva may spill over onto the eyelid margin, causing ocular surface symptoms. Epiphora may be the result of conjunctivochalasis obstructing the inferior punctum. Canalicular irrigation should be performed to rule out lacrimal outflow obstruction even in the presence of conjunctivochalasis. Corneal examination may show inferior staining from irritation by the redundant conjunctiva with blinking.
There are numerous techniques that have been described for the treatment of conjunctivochalasis. Medical management consisting of ocular lubrication is the initial treatment. Topical antihistamines, cyclosporine and steroids may be used judiciously. For refractory cases of conjunctivochalasis, our preferred treatment is thermal conjunctivoplasty. This technique uses a hand-held, battery-powered, high-temperature cautery tip to thermally contract the redundant conjunctiva. Treatment at the limbus is spared to avoid damage to the stem cells. Refractory chemosis after eyelid surgery can also be treated with thermal conjunctivoplasty. Performing cauterization on the palpebral conjunctiva is avoided as symblepharon may result. Finally, this procedure should not be carried out in patients with a history of cicatrizing conjunctivitis.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree