| Implant extrusion, not amenable for repair with patch graft |
| Enophthalmos and superior sulcus deformity from insufficient orbital volume |
| Socket contracture |
| Primary implant in the growing orbit of a child |
| History of socket irradiation |
| Details about enucleation/evisceration; type of implant used |
| Depth of fornices and presence of socket contraction |
| Implant motility (suggests extraocular muscle attachment) |
Introduction
A healthy anophthalmic socket consists of an intact conjunctival surface with deep fornices that allows for retention of an ocular prosthesis, symmetric upper and lower eyelid positions, and a buried orbital implant of sufficient volume. Socket complications can result from deficiencies of any of these features.
A detailed history of the events leading up to the anophthalmic socket is important. The type of surgery (enucleation vs. evisceration), implant used, and any intraoperative findings should be elicited from the patient and the operative report if available. Enucleation for intraocular tumors may be associated with irradiation, which can result in socket contraction and/or ischemia. A phthsical eye resulting from multiple surgeries may have conjunctival shortening. Trauma and loss of the globe may be associated with occult orbital fractures and lost extraocular muscles during surgery. The prosthetic should be evaluated for size, fit, and surface irregularities. With the prosthetic in place, evaluation is directed towards: position of the upper and lower eyelids, vertical excursion of the eyelids, volume of the superior sulcus, presence of lower eyelid malpositions, and exophthalmometry. After removal of the prosthetic, the socket should be evaluated for: depth of the fornices, conjunctival shortening/symblepharon, signs of breakdown of the conjunctiva/exposure of the orbital implant, and signs of infection or inflammation of the conjunctival surface.
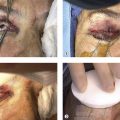
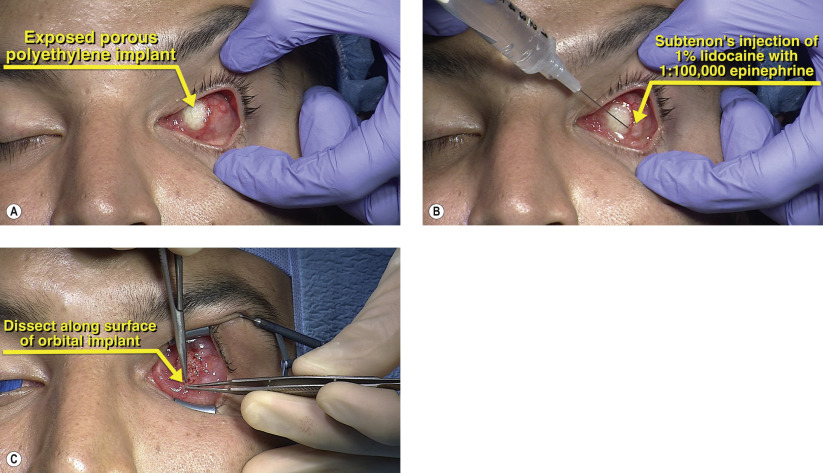
Implant extrusion can be a consequence of multiple factors including: insufficient coverage of the implant with Tenon’s capsule, placement of too large an orbital implant, implant infection, a poorly fitting prosthetic causing pressure necrosis of the conjunctival surface, after placement of a peg for improved motility, and a complication related to the type of orbital implant used. Medical management consists of antibiotic therapy, but implant extrusion is managed definitively with surgery. Small and early extrusions can be managed with a patch graft over the exposed implant with autologous temporalis fascia or donor sclera, provided sufficient conjunctiva is present to completely cover the exposure. The success rate of patch grafts is variable and depends on several factors including: size of the defect, degree of microbial contamination of the implant, and viability of the conjunctiva. For larger and late extrusions with possible infection of the implant, our preference is to remove the infected orbital foreign body implant and replacement with an autologous dermis fat graft.
A dermis fat graft has many advantages including that it: is an autologous tissue with no risk of extrusion, provides surface area for contracted sockets, and can grow in the developing child. The main disadvantages are: donor site morbidity and the variable rate of absorption of the fat component.
Surgical Technique

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree