13 The Process for Flap Selection by Region of the Lower Extremity
We restore, rebuild, and make whole those parts which nature hath given, but which fortune has taken away. Not so much that it may delight the eye, but that it might buoy up the spirit, and help the mind of the afflicted.
—Gaspare Tagliocozzi (▶ Fig. 13.1)1
Summary
A wound requiring repair, or a defect that must be restored, may often be solved even without the need for a vascularized flap. The exact solution indeed must be a process requiring first a careful preoperative analysis of the complexity of the patient’s problem and any rate-limiting comorbidities, and by having an astute awareness of the given institution’s technological capabilities and also that of the reconstructive surgeons themselves. The completion of every such assessment after scrutinizing all these parameters will thus always be unique for that individual patient. For the same reason, if the planned optimum strategy requires a flap, that too must be individualized. Whether muscle, integument, bone, or perhaps some other soft tissues are required as a flap, the exact choice must not only best fit the requirements of the recipient site but also simultaneously minimize donor site deformity. The expanded lower extremity zone concept, unlike traditional dogma, knows no arbitrary boundaries and tailors a flap selection process to be determined by specific factors such as recipient site size and complexity, whether function must be restored, what choices are available, and a realization that the final appearance may be just as important a factor for the patient who seeks as close as possible the restoration of normalcy.
Keywords: reconstructive ladder, reconstructive elevator, reconstructive matrix, expanded zone concept, chimeric flap
13.1 Introduction
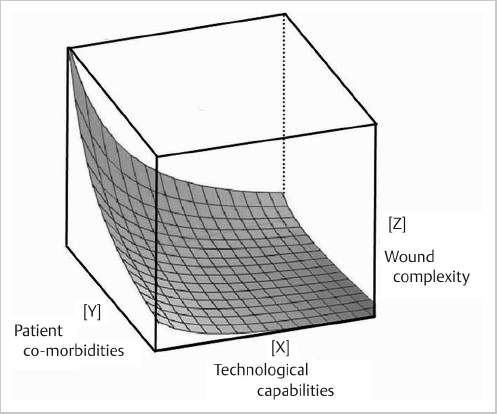
The correction of any wound involving the lower extremity requires repair of disrupted parts, while a defect will always require the restoration of missing components.2 Traditionally, the method to accomplish either of these objectives adhered to the reconstructive ladder, beginning in the basement with the simplicity of a secondary closure, then stepwise in a sequential fashion proceeding upward with increasing complexity through skin grafts and dermal matrices until reaching the available assortments of flaps.2,3 Levin expanded his orthoplastic ladder to also include the appropriate steps for management of bone injury or gaps.4 Gottlieb and Krieger5 challenged this conventional approach with their reconstructive “elevator” that allowed them to jump at will to whatever level they considered the best solution not only for the immediate problem but also for the long term. The reconstructive matrix may be the best model of all as it emphasizes all aspects of the critical preoperative decision-making analysis necessary to provide the best overall result6; that will be unique in the lower limb, as this must assure not only bony stability and adequate soft-tissue coverage but also, most importantly, the maintenance of function and mobility.7 Closer inspection of this matrix reveals a three-dimensional structure with its axes corresponding to the technological capabilities available at the given institution, which may somewhat correspond to the rungs of the reconstructive ladder, patient surgical risk factors such as comorbidities, and the complexity of the problem that needs to be solved (▶ Fig. 13.2).6 A simultaneous assessment of how all of these parameters interconnect will be essential for each individual patient to permit formulation of their optimal reconstructive strategy.8 Thus, if a vascularized flap is indicated, the exact choice will never be the same for every patient, as the product of all these parameters will have an infinite variability necessitating that the final selection always be individualized so that the best outcome can be anticipated.
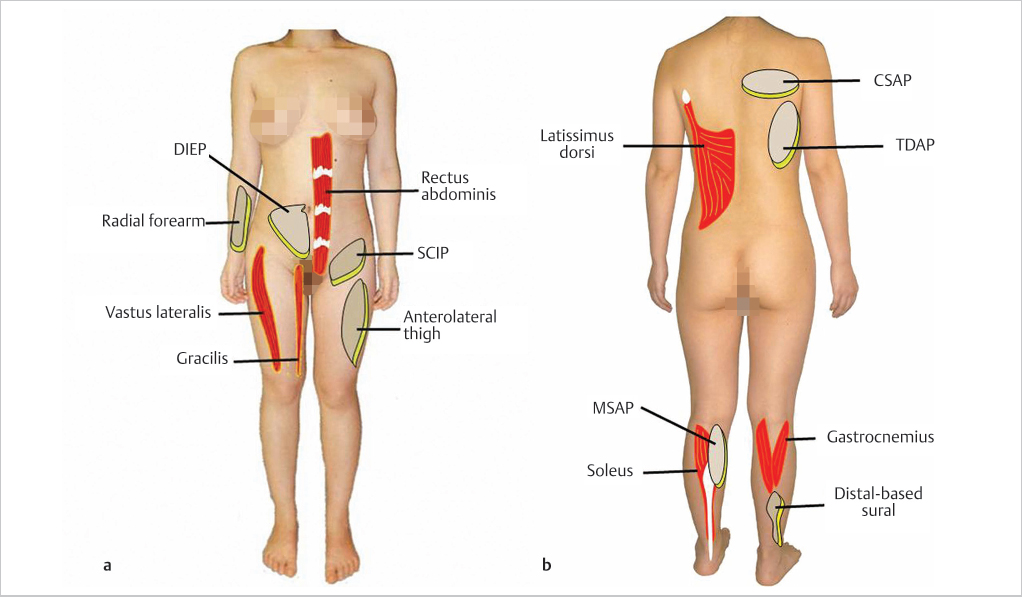
Rausky et al9 believed that the goals of lower limb reconstruction must include timely intervention to better ensure function preservation, creation of no impediment in the use of shoe wear, and the provision ultimately of a reasonable appearance, while causing minimal donor site morbidity. A properly selected flap may be the only alternative that is possible to fulfill all these prerequisites. The possible options for bone deficits will be better discussed in Chapter 23. Soft-tissue requirements are the more common need anyway in this region, and hereafter the most practical or workhorse flaps will be emphasized (▶ Fig. 13.3), recognizing that a “laundry list” of all available flaps would be an impossibility and that notable satisfactory exceptions exist that may rely instead on a surgeon’s familiarity and particular preferences.10
Fig. 13.2 The optimal reconstructive strategy must be individualized for each patient using the reconstructive matrix. This requires that the surgeon assess the complexity of the wound or defect, then consider all possible modalities including flaps needed for restoration, while also considering the limitations of the patient’s inherent risk factors. The three-dimensional hyperbola within this matrix represents the optimal outcomes possible after consideration of the individual components of these three variable parameters. (Following the guidelines of Erba et al.6)
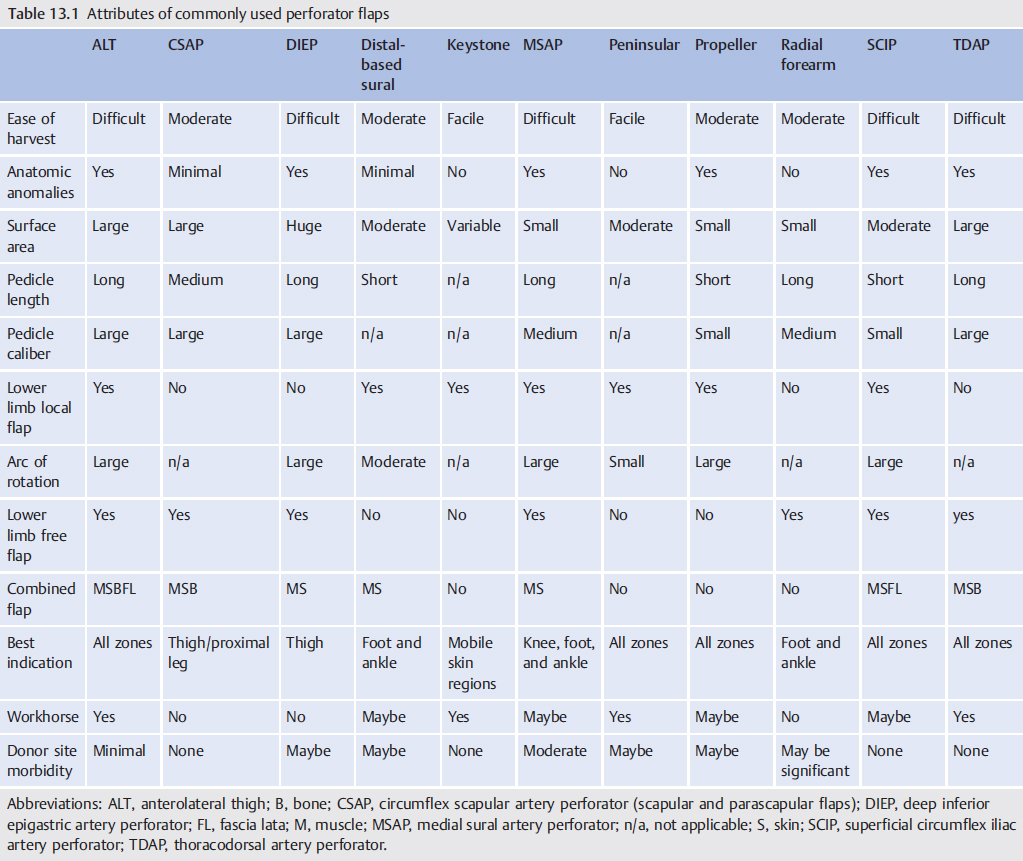
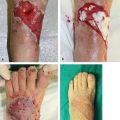
Comparable rates of primary fracture and skin healing, time to ambulation, and thus limb salvage are similar regardless of whether a muscle or fasciocutaneous flap is used.11,12 The latter includes the genre of perforator flaps, which many consider provide a superior aesthetic result, the potential for later elevation to allow secondary procedures as a better option than a muscle flap, and, since no muscle is included, minimize function loss at the donor site (▶ Table 13.1). The adoption of this concept of perforator flaps has rapidly seen an increase in the use of local or so-called freestyle13,14 flaps throughout the lower extremity in lieu of free flaps, perhaps a consequence of the fact that the latter may be riskier, especially in patients with multiple comorbidities, and certainly require a greater allocation of resources and time as well as technical expertise that may not be universal. However, even a small defect may still be better resurfaced with a microsurgical tissue transfer if adjacent tissues have been damaged and perforators are unavailable or unreliable15; and it certainly will always be a solution for all zones of the lower extremity even if some might think that choice inappropriate (▶ Fig. 13.4).
Fig. 13.3 The named pragmatic and workhorse flaps commonly used in the lower extremity. (a) Anterior donor sites. (b) Posterior donor sites (CSAP, circumflex scapular artery perforator; DIEP, deep inferior epigastric artery perforator; MSAP, medial sural artery perforator; SCIP, superficial circumflex iliac artery perforator; TDAP, thoracodorsal artery perforator).
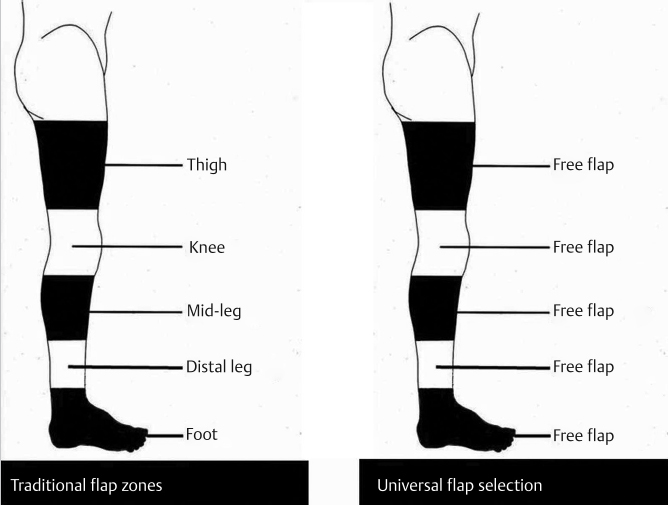
Fig. 13.4 With the lower extremity divided into the traditional zones, selection of a “free flap” can be a universal, if not unrealistic, solution for all regions if a flap is needed.
13.2 Selection According to the Recipient Site
Formerly, the lower extremity was divided into regional zones (▶ Fig. 13.4) where the flap choice would be either a pedicled flap available from that zone or a free flap.16 Mathes and Nahai17 in their original book on muscle flaps listed some 22 available muscles in the lower limb as possible local flaps, but most were too diminutive or had an unreliable pattern of circulation. Those still commonly in use include the vastus lateralis or tensor fascia lata18 muscle for the trochanteric area; gracilis and rectus femoris19 for the groin, or occasionally also the sartorius,8 but its vascular supply may be unreliable; gastrocnemius for the knee and proximal third of the leg; and soleus for the middle third (see Chapter 14; ▶ Table 13.2). The rectus abdominis muscle, although a distant flap, can still reach the upper thigh and groin, but at the potential price of causing abdominal wall incompetence.20 A paradigm shift has recently evolved for the utilization of local cutaneous flaps instead throughout the lower limb, whether based on perforators or not (▶ Fig. 13.5).21 These have included propeller, peninsular, island, or advancement flaps including keystone flaps (see Chapter 15). Many would consider the distal-based sural flap, which many prefer for more acral defects as a substitute for a free flap, to be a peninsular flap or even a propeller flap, depending on the method of elevation.22,23
A better way to evaluate lower limb soft-tissue requirements has been proselytized by Lachica24 who has introduced an “expanded zone concept” (▶ Fig. 13.6). Again, because of the advent of perforator flaps, the traditional zone idea has become too restrictive as it lacked specificity with regard to wound size and complexity as well as type of tissue loss.24 The “expanded lower extremity zones” are not restricted by arbitrary boundaries, and are differentiated according to soft-tissue anatomical and functional requirements throughout this region, which in turn determines appropriate flap selection (▶ Table 13.3).24 Areas densely surrounded by muscle such as the thigh and calf have no functional restrictions, and, although a skin graft or muscle flap would suffice, a thin perforator flap would give a superior aesthetic result,20,24 replacing “like with like.”25 Most of the rest of the leg also requires soft-tissue replacement only, and that usually best as a perforator flap (▶ Table 13.3). Any flap in the knee area must allow unrestricted motion and the patella, since pressure bearing, must also have a more durable, resilient coverage.24,26 Following the subunit principle for foot and ankle soft-tissue restoration,27,28 all areas are similar in that a thin flap is mandatory to allow proper fit of shoes, while the plantar heel and forefoot differ in that any flap must be durable as these will be subjected constantly to weight bearing and the strains of ambulation.24
If for any reason a local flap is not available, a free flap may be the next option. Restricting the donor site to the same extremity if possible will minimize the overall scarring and burden on the rest of the body. The anterolateral thigh flap has become the “ideal” soft-tissue free flap to fulfill these requirements29 (▶ Table 13.1), as this donor site can be prefabricated,30 can undergo thinning to the proper contour,31 can have gigantic dimensions or split into multiple smaller flaps,32 has a long and reliable vascular pedicle, and can even be used in combination with other adjacent tissue components such as fascia lata or muscle if desired.33 The medial sural artery perforator free flap is another option specifically for smaller defects, as it also has a potentially long pedicle to reach any available recipient vessels to thereby avoid use of vein grafts, with still moderately large caliber vessels.34 The radial forearm flap similarly has a long pedicle, and may be the only thin cutaneous flap in the obese patient encountered most often in the western hemisphere, albeit sometimes this can create significant donor site compromise.20,23,35 As an alternative for the morbidly obese, muscle flaps may still be preferable for proper contour and logistical reasons, with the “workhorse” flaps being the latissimus dorsi (LD) for large defects or the gracilis for smaller ones (▶ Table 13.2). Other cutaneous flaps from the dorsal thoracic fascia such as the circumflex scapular artery perforator flaps (also known as the scapular36 or parascapular flaps37) or the thoracodorsal artery perforator (TDAP) flap may be just as versatile as the LD muscle, but the former offers function preservation if important. Note also that many prefer the TDAP flap over the scapular or parascapular flap, as the vascular pedicle is easier to dissect and can be longer (see Chapter 16).