Key Words
autologous fat grafting, augmentation mammaplasty, reduction mammaplasty, mastopexy, breast reconstruction
Introduction
Achieving optimal symmetry is the primary goal of unilateral and bilateral breast reconstruction. In cases of unilateral breast reconstruction, which is the focus of this chapter, this often requires a secondary procedure on the ipsilateral breast and/or contralateral breast. It is estimated that up to 70% of women will undergo one or two procedures in an attempt to obtain symmetry. The primary operations utilized include augmentation mammaplasty, mastopexy, and reduction mammaplasty. Additionally, autologous fat grafting can further refine and correct contour deformities on both breasts, yielding a more natural and symmetric appearance.
The discussion of the likely need for such a symmetry procedure should occur at time of initial consultation with the patient, when breast reconstruction is discussed. The patient should be informed that both the need and desire for a contralateral symmetry procedure will be high. Furthermore, the timing of this procedure should also be discussed. In addition to discussing the likely procedures necessary, based on the patient’s goal size for the reconstructed breast, the different external scars that may result on both breasts should also be described.
The timing of secondary and symmetrizing operations remains an issue of debate. Proponents of simultaneous contralateral operations argue better aesthetics without an increased complication rate, and a reduction in the number of overall operations. However, opponents contend that immediate postoperative changes in the reconstructed breast, primarily swelling, are often unpredictable, and a more symmetric final result may be achieved by waiting until the reconstructed breast has reached its ultimate size and location on the chest wall prior to matching. Ultimately, either approach is acceptable, as long as the patient understands the benefits of each, and makes an informed decision.
In planning the approach, the plastic surgeon must also account for timing around any adjuvant oncologic treatment being delivered to the patient. If a contralateral operation is not done at the time of the patient’s initial reconstruction, it is preferable to delay until the patient has completed any adjuvant chemotherapy or radiation therapy. Because the reconstructed breast will often be operated on simultaneously, for aesthetic enhancement, such an approach will reduce complication rates, and improve symmetry.
Indications and Contraindications
It is the authors’ opinion that almost every patient undergoing unilateral breast reconstruction will be a candidate for some form of contralateral breast symmetry procedure. This is offered with the goal of achieving optimal aesthetic outcome. The key is selecting the appropriate procedure in each patient’s situation.
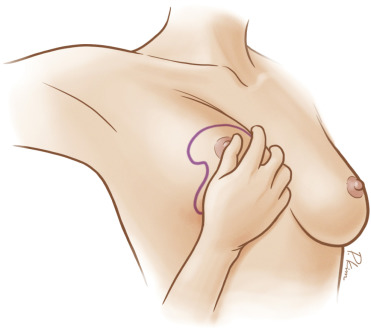
For those patients undergoing a large size increase from native to reconstructed breast, then a contralateral augmentation mammaplasty will usually be offered ( Fig. 18.1 ). This is the consistent method used for achieving volume symmetry in these patients. When offering this procedure, the surgeon must ensure the patient has appropriate soft tissue quality to support either a subglandular or submuscular implant placement. Furthermore, if greater than grade 1 ptosis exists on the breast, the need for a simultaneous mastopexy should be discussed.
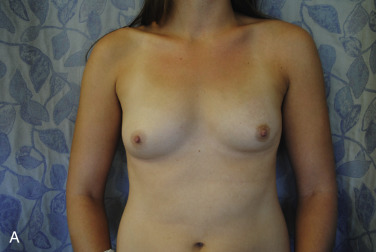
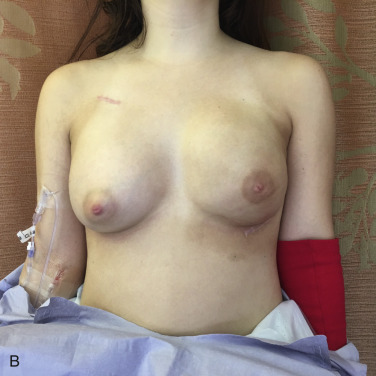
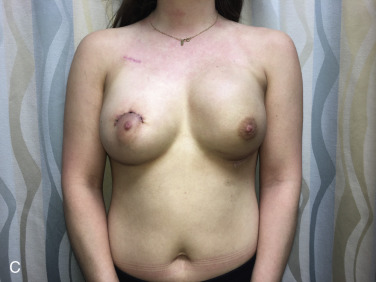
For those patients in whom a smaller reconstruction volume is achieved, relative to native breast size, a contralateral reduction mammaplasty is offered. The primary techniques considered for reduction include the classic inverted “T” inferior pedicle (Wise pattern), and the vertical pattern with medial or superior-medial pedicle. The Wise pattern reduction is reserved for patients with grade 3 breast ptosis, in need of significant skin resection, and greater than 800 g parenchymal resection. The vertical pattern is used for breasts with grade 2 ptosis, and anticipated parenchymal resection of less than 800 g. The authors’ preference is the vertical pattern, as it results in a breast with greater projection, and longer lasting result, due to the parenchyma reshaping involved; thus, this better matches a reconstructed breast.
In patients requiring correction of nipple–areola complex (NAC) position on the breast, without alteration of breast size, mastopexy is preferred. In the authors’ experience, when used for contralateral symmetry in breast reconstruction, mastopexy is often performed in conjunction with another procedure for symmetry on that breast. Most commonly, it accompanies an augmentation mammaplasty, for further correction of NAC height. Alternatively, it can be performed as a component of a reduction mammaplasty, which also elevates the NAC position, in conjunction with size reduction. All patients must undergo careful evaluation of changes in NAC position in the reconstructed breast, when nipple-sparing mastectomy (NSM) is performed, and allow this to guide the need for contralateral mastopexy. Oftentimes with NSM and prosthetic reconstruction, there is NAC elevation, due to skin and/or muscle contraction.
Autologous fat grafting is promoted by the author for almost all reconstructive patients, given that fat injection carries a multitude of benefits, both aesthetic and restorative. Most commonly, autologous fat grafting is performed on the reconstructed breast, for enhancing upper pole aesthetic symmetry with the native breast. In the reconstructed breast, upper pole parenchyma resection during the mastectomy results in tissue deficit and hollowing, and autologous fat grafting is an ideal correction. On the contralateral breast, fat grafting can similarly restore volume and enhance contour in specific, isolated areas of the breast. Furthermore, autologous fat offers restoration of tissue quality in the breast, due to its high stem cell concentration, and this benefits both breasts.
In all cases, the only absolutely contraindication to contralateral symmetry procedures is active smoking. In such cases, the elective procedures should be delayed until the patient has quit smoking for a minimum of 6 months. Relative contraindications to these procedures include a contralateral breast with a history of prior radiation therapy, obesity, or a preoperative breast shape/size that makes achieving reasonable symmetry unlikely.
Preoperative Evaluation and Special Considerations
During a patient’s initial preoperative evaluation, the surgeon must discuss patient-specific reconstructive options, while also addressing patient goals and expectations for both breasts. At this visit, a complete breast and oncologic history should be obtained, with particular emphasis on need for adjuvant treatment therapies including chemotherapy and radiation. While the ultimate goal of complete oncologic resolution should take precedence, the timing and coordination of reconstructive procedures can often impact reconstruction success and final cosmesis.
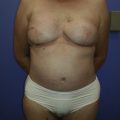
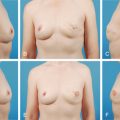
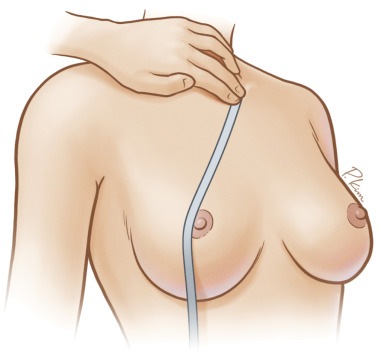
A careful examination and measurement of key landmarks on both breasts is critical, particularly breast base width, distance from nipple to inframammary fold, and distance from sternal notch to nipple ( Figs. 18.2–18.4 ). Any asymmetries must be noted, in both position and size of the NAC on both breasts. Furthermore, these measurements must be repeated on the reconstructed breast through the treatment, as the NAC position can change through mastectomy and reconstruction, and this must be accounted for when planning contralateral symmetry procedures.
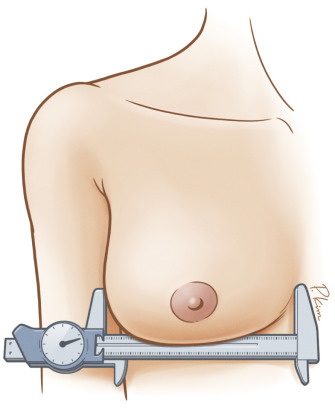
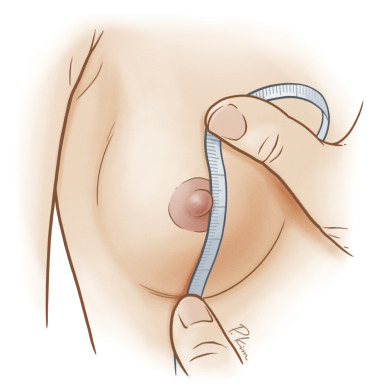
Finally, the projection of both breasts must be assessed carefully. The majority of prosthetic reconstruction is performed with high or enhanced high projection implants. This will often result in the need to either increase or decrease projection of the contralateral breast, which can be accomplished by accurately planning the augmentation mammaplasty or reduction mammaplasty, respectively.
Surgical Techniques
Augmentation Mammaplasty
Preoperative Markings
Key preoperative markings for landmarks in augmentation mammaplasty include the inframammary fold (IMF), the suprasternal notch to nipple distance, and nipple to IMF distance. If this is performed in conjunction with an expander–implant exchange, then markings for pocket dissection on the augmentation mammaplasty should mirror markings on the reconstructed breast for capsulotomy and pocket reshaping. The authors’ preferred incisional approach for augmentation mammaplasty is the lateral IMF incision. In most cases, this incision can be kept to 4 cm for the entire procedure. Other incisional approaches include the periareolar and the transaxillary approaches.
Details of Procedure
Based on upper pole parenchyma thickness, and type of contralateral reconstruction performed, the surgeon must first select the anatomic plane of implant placement for the augmentation mammaplasty. The authors’ preference is to perform subfascial augmentation, given the increased prevalence of prepectoral breast reconstruction procedures on the contralateral reconstructive breast. Subfascial augmentation offers advantages of less pain, lower risk of animation deformity, and low reported rates of capsular contracture. An upper pole pinch thickness of greater than 2 cm will allow for placement of a subfascial or subglandular breast implant for augmentation, without risk for visible implant edges in the upper pole.
When performing the augmentation at the time of expander-to-implant exchange on the contralateral breast, the reconstructed breast should be addressed first. Once this breast has been sized with the desired implant, and fat grafted, then the augmentation can be performed, and optimal aesthetic match can be attained.
When the IMF incision is chosen, this incision is marked 1 cm below the inframammary crease of the patient. Assuming the patient has a normal crease position preoperatively, this will result in the ability of the scar to lie behind the lower pole breast parenchyma, after the patient heals. When the incision is placed directly at the IMF or above, it will rise on the augmented breast, and will eventually sit on the visible portion of the patient’s lower breast.
Following incision through the IMF approach, careful dissection must proceed in a superior direction, such as not to lower or displace the IMF. Once the pectoralis fascia is reached, then the implant pocket can be elevated just below this layer. Dissection should always proceed approximately 1 cm above the IMF position. From this approach, once the correct anatomic plane is identified, the majority of the dissection can be performed bluntly. Once the pocket is elevated, and the eventual implant is placed, this will result in an implant sitting posterior to both the breast parenchyma and the pectoralis major fascia, but anterior to the pectoralis major muscle.
For those patients undergoing a submusclar implant placement, which is recommended in cases of breast deflation and reduced upper pole soft tissue coverage, the dual-plane approach is recommended. Following elevation of the pectoralis major muscle, the inferior insertion of the muscle is incised along its entire length, leaving a 1-cm cuff of muscle along the IMF. This will allow for NAC elevation and a more natural appearance of the augmentation mammaplasty. When the lower border of the pectoralis muscle is not released in this fashion, and the implant is placed in a complete submuscular pocket, the implant cannot descend to the native IMF, and this will likely result in implant malposition superiorly.
Following complete pocket elevation, the author promotes placement of all implants using a no-touch technique. Prior to implant placement, pockets are thoroughly irrigated with betadine and antibiotic-impregnated saline. Then the implant is placed in such a way that it does not contact the patient’s external skin.
When the periareolar approach to implant placement is selected, the previous steps for submuscular or subfascial implant placement remain the same. The primary difference is access to the pocket, from the anterior breast incision. While the dissection can be made in a transparenchymal manner, directly through the breast to the chest wall, this will expose the implant to bacteria present within the breast ducts. Thus, it is preferable for dissection to proceed along the lower pole breast fascia, inferiorly towards the IMF. Once the fold is reached, the dissection can then proceed superiorly in the desired plane to create the implant pocket.
Following completion of the augmentation, the patient must be placed in the sitting position in the operating room, to ensure symmetry between the breasts. Specifically, the surgeon must separately assess the following aspects on both the augmented and reconstructive breast: size, shape, base width, projection, NAC position. For the patient to be satisfied with the reconstructive outcome, all these factors must align.
Reduction Mammaplasty
Preoperative Markings
When marking a reduction mammaplasty, the first landmark to place is the postoperative NAC position. This is marked by transposing the IMF anteriorly onto the breast mound (Pitanguy’s point). This is then confirmed by matching sternal notch to nipple distance with the contralateral reconstructed breast NAC position, if matching a NSM.
Choosing technique for breast reduction often depends on the preoperative breast size and ptosis. When the breast has grade 2 ptosis, and a 150–800-g reduction is anticipated, a vertical breast reduction pattern is generally selected, with a superior or superior-medial pedicle. When the preoperative breast mound has grade 3 ptosis, and greater than an 800-g reduction is anticipated, an inverted-T “Wise pattern” technique is selected. This can be performed with an inferior pedicle, or a superior/superior-medial pedicle.
For vertical reduction patterns, the nipple position is marked at Pitanguy’s point, and is then placed 1 cm below this mark, to prevent a high-riding NAC. This is typically at a sternal notch to nipple distance of 22–23 cm. The remainder of the vertical reduction areola pattern is marked by planning the areolar circle with a 40–42-mm circumference. This is marked as a C-shaped incision, with the open area inferior. When this C-shaped dome is brought together at the two inferior edges, it creates a circle, with the stated circumference. Next, the vertical limbs are marked by displacing the breast medially and laterally, and with each, marking the vertical line from the upper point at the base of the new areola, to the inferior point just above the IMF ( Fig. 18.5 ). The amount of force used to displace the breast during these markings will determine the tightness of the inferior vertical closure, as more force results in a wider skin resection inferiorly.