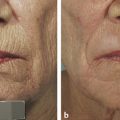
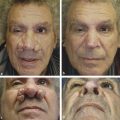
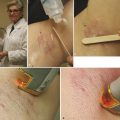
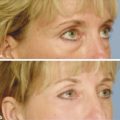
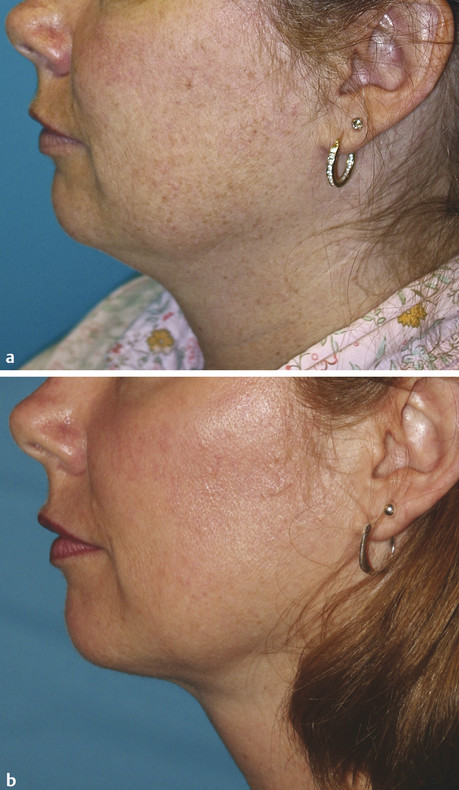
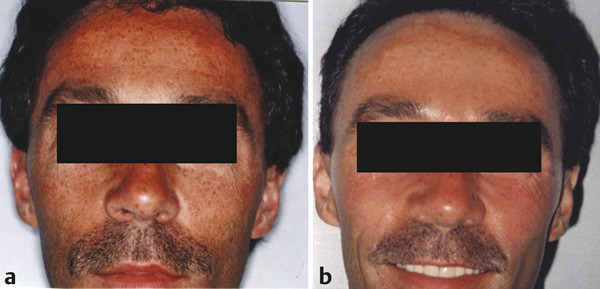
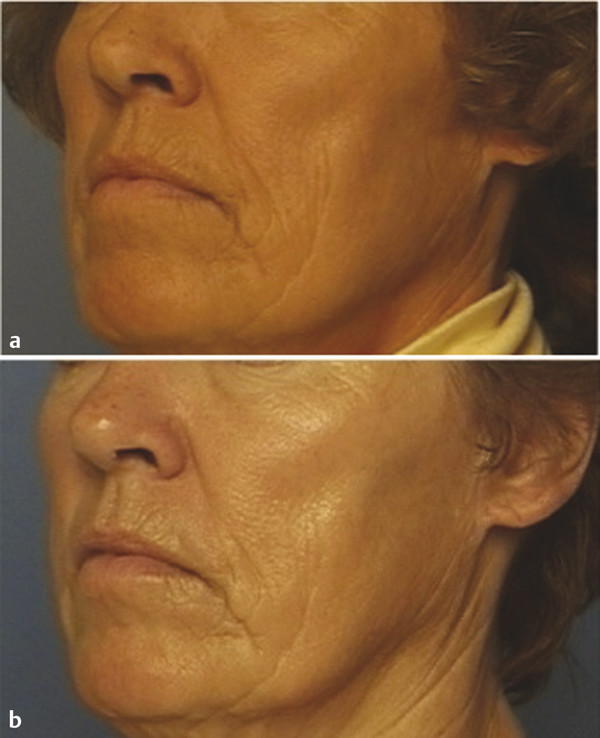
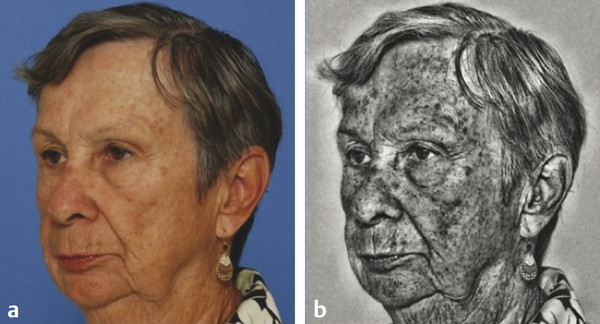
Indications for Superficial Peel and Patient Evaluation The primary clinical indications for superficial chemical peels are for the improvement of mild photoaging (Glogau types I and II), skin texture, acne, actinic keratosis and for improvement of fine rhytids. Superficial peels are ideal for patients whose lifestyles preclude the prolonged recovery required of medium or deep peels. Superficial peels are “patient friendly,” allowing patients to return to work the same day, are not painful, and are not associated with hypopigmentation. They are generally safe and rarely are associated with adverse sequelae. Often, superficial peels are performed 1 to 4 weeks apart (▶ Fig. 27.1, ▶ Fig. 27.2, ▶ Fig. 27.3). Maximal results are seen when a series of treatments (six to eight) are performed. Combining a series of peels with a home skin care regimen can result in optimal, long-term changes. Skin care regimens with use of topical vitamin C, retinoids, or low-concentration glycolic acid (GA) promote continued skin improvement and aid collagen production. Fig. 27.1 (a) Before a series of glycolic acid (GA) peels. (b) After a series of GA peels. Fig. 27.2 Patient is seen (a) prior to a series of glycolic acid (GA) peels, and (b) following a series of GA peels. Fig. 27.3 A woman is shown (a) before a series of glycolic acid (GA) peels, and (b) subsequent to a series of GA peels. A thorough patient history is important prior to any chemical peel regimen. A history of keloid formation, recurrent herpetic outbreaks, medication use such as oral isotretinoin, current use of skin care products, history of silicone injections, prior cosmetic procedures, and overall general health should be obtained. Background on a patient’s perceived skin sensitivity is meaningful because it may guide the clinician in choosing more or less aggressive treatments. Evaluations of Fitzpatrick skin type and the skin’s overall thickness and oiliness are helpful. Skin that is thicker and more sebaceous may require a pretreatment program with topical retinoids or alpha hydroxy acids (AHAs). Superficial peels can be used to treat all Fitzpatrick skin types (I–VI). The condition(s) treated by a superficial peel should ideally be limited to the epidermis. Examination of the skin with a Wood lamp will help to identify appropriate candidates (▶ Fig. 27.4). Wood lamp illumination enhances superficial dyschromias, whereas deeper dyschromias demonstrate minimal enhancement under illumination and require more aggressive therapies (medium- or deep-depth resurfacing).1 Fig. 27.4 A 70-year-old woman with marked rhytidosis and photodamage, comparing (a) standard photography with a (b) computer-generated Wood lamp depiction. (Reproduced with permission from Truswell WH, IV. Aging changes of the periorbita, cheeks, and midface. Facial Plast Surg 2013; 29(1): 3–12.) AHAs are weak acids that induce their clinical effects by either metabolic or caustic effect.2 At low concentrations, they reduce corneocyte cohesion, inducing exfoliation of the epidermis.2 At higher concentrations, their effect is mainly destructive; therefore, AHAs cannot neutralize themselves and need to be neutralized by water or a weak buffer.2 Superficial peeling primarily affects the epidermis and uppermost part of the dermis. The stratum corneum becomes thinner, more compact with desquamation.3 The inflammation stimulates the production of cytokines that in turn stimulate and activate fibroblasts that produce type I and type IV collagen and elastin fibers.4 Histological studies by Ditre et al5 showed an increase in collagen and glycosaminoglycans in the papillary and reticular dermis and increased elastic staining in the dermis.3,5 This increase in collagen and elastin translates into the clinical improvement seen postpeel. Chemical peels produce varying clinical effects to the skin depending on their depth of penetration. Chemical agents are classified as very superficial (removing stratum corneum) to deep (extending into reticular dermis) (▶ Table 27.1).6 Factors such as concentration, duration of contact with the skin, number of coats applied, as well as prepeel skin preparation may impact the depth of a peel and its subsequent clinical effect. Depth of penetration Peeling agent Very superficial (removes stratum corneum) Microdermabrasion Retinoic acid GA 30–50% (1–2 min) Jessner’s Solution (1–3 coats) Resorcinol 20–30% (5–10 min) TCA 10% (1 coat) Superficial (upper papillary dermis) GA 50–70% (5–20 min) Jessner’s Solution (5–10 coats) Resorcinol 50% (30–60 min) TCA 10–35% (1 coat) Solid CO2 slush Medium (papillary dermal) GA 70% (5–30 min) TCA 35% Modified Baker-Gordon w/2 drops of croton oil Deep (reticular dermal) Baker-Gordon phenol formula Hetter Peel Abbreviations: GA, glycolic acid; TCA, trichloroacetic acid. Superficial chemical peels penetrate the level from the stratum granulosum to the upper papillary dermis. Superficial peels are divided into two categories: very light and light. Very light peels exfoliate only the stratum corneum. The agents used include low-concentration GA, Jessner’s Solution, salicylic acid, and 10 to 20% trichloroacetic acid (TCA). Light peels injure the entire epidermis and will stimulate collagen deposition and promote epidermal thickening. Light peel agents include 50 to 70% GA, 10 to 35% TCA, and solid carbon dioxide slush (▶ Table 27.1).6,7 Preparation or “priming” of the skin prior to chemical peeling with topical agents may lead to improved and uniform results. This requires good patient compliance with the pretreatment program for consistent outcomes. Tretinoin applied 4 to 6 weeks in advance of initiating a peel program is commonly utilized. Tretinoin predominantly affects the epidermis with short-term use. Its epidermal effects (thinning and compaction of the stratum corneum and melanocyte suppression) make it an ideal pretreatment agent.1 Tretinoin enhances penetration of the peeling solutions and accelerates postprocedural epithelialization.1,7,8 Patients are instructed to apply the tretinoin as uniformly as possible to the face; uneven application can result in uneven or poor uptake of the peeling solution, limiting the effectiveness of the peel. Reduction in melanogenesis through the use of daily sunscreens is helpful to decrease incidence of postinflammatory hyperpigmentation (PIH). Application of hydroquinone 4% once or twice daily may be helpful to prevent PIH in Fitzpatrick skin types III through VI patients. Hydroquinone causes a reversible depigmentation through inhibition of the enzyme tyrosinase. This inhibits the enzymatic oxidation of 3,4-dihydroxyphenylalanine (dopa) to melanin, effectively suppressing melanin production.1,4,7 Although the likelihood of herpes simplex virus (HSV) reactivation with a superficial peel is low, antiviral prophylaxis should be considered because all resurfacing procedures have the potential to stimulate HSV. An active herpes infection is a contraindication to proceeding with a chemical peel. Most commonly used antiviral agents include acyclovir or valacyclovir 500 mg twice daily, started 1 to 3 days prior to procedure and continued for up to 10 to 14 days following the procedure.
27.3 Basic Chemistry and Histological Changes
27.4 Classification of Chemical Peels
27.5 Prepeeling Preparation
27.6 Postpeel Regimen
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree