Sommerlad Palatoplasty
T. Guy Thorburn
DEFINITION
Cleft palate repairs can be broadly classified into straightline repairs (such as the Sommerlad technique) vs Z-plasty repairs (such as the Furlow technique).
Otto Kriens proposed the intravelar veloplasty based upon his work on the anatomy of the cleft palate.1
Sommerlad then developed this dissection into a more radical procedure and popularized the technique.
The underlying principle is identification and retropositioning of the soft palate muscles, before connecting the levator muscle mechanisms from the two sides of the soft palate.
ANATOMY
The key functional issue in CP or SMCP is that the levator muscle mechanism is not in continuity on the two sides. In addition, the fibers become tethered to the posterior border of the hard palate.
Successful functional palate repair therefore requires repair of the “levator sling” as well as closure of the tissues across the cleft.
The tethering to the hard palate seems to be an equal problem in differing types of cleft: whether unilateral or bilateral cleft lip and palate, cleft palate only, or submucous cleft palate.
The key functional muscle is the levator palatini, but the surrounding muscle/aponeurotic tissue is kept in continuity to allow more reliable tissue handling and retropositioning and subsequent suturing.
Of note, the levator sits on the nasal aspect of the soft palate and so becomes visible only when the dissection is well underway.
PATIENT HISTORY AND PHYSICAL FINDINGS
The initial assessment of the newborn with a cleft involving a palate would usually be alongside a pediatrician and includes:
Pregnancy and birth history (including information from any antenatal testing), gestation, birth weight, and Apgar scores.
Initial assessment of cleft type and any related anomalies, including any airway concerns suggesting Robin sequence.
Medical, drug, and allergy histories.
Family history of clefts, other major health problems, or anesthetic problems and any genetic diagnosis.
Feeding history, including bottle type (eg, squeezy bottle, free flow, Haberman), current weight, maximum percentage weight loss and number of days to regain birth weight, and volume/duration/frequency of feeds.
Physical examination to assess the upper airways, cleft type, cleft width and how much deficiency there is of surrounding tissues, as well as any related anomalies or dysmorphic features. The pediatrician would then complete a fully newborn examination looking in particular for related health issues such as cardiac, respiratory, renal, or neurological signs.
IMAGING
No routine preoperative imaging is required for typical clefts. For older children presenting with SMCP or velopharyngeal incompetence (VPI), assessment with a speech lateral videofluoroscopy helps to evaluate the position of the velum during phonation and relative size of the soft palate to the size of the pharynx.
Standardized preoperative clinical photos should be taken as these are invaluable when assessing outcomes many years later.
SURGICAL MANAGEMENT
Preoperative Planning
A key aspect of successful cleft palate repair is optimizing the patient prior to surgery. A pediatrician is a crucial member of the cleft team.
Although there is much discussion of age at palate repair, different team protocols vary from around 3 months old to 15 months or more.
Very young babies will tend to be more susceptible to airway compromise around the time of surgery.
Delaying repair until much older and speech has developed has been associated with poorer speech outcomes, particularly related to articulatory errors.
Our team protocol is for palate repair around 8 to 12 months (corrected for prematurity), but our emphasis is much more on ensuring that the child is well and thriving as surgery approaches.
If the child is not growing along his or her expected centiles (with growth plotted on the appropriate chart for syndromic children), this should be addressed before surgery.
We routinely postpone for about 4 weeks if children have upper respiratory tract infections.
By following this approach, we have seen a significant reduction in fistulae and concerns with speech function.
Routine blood tests or cross match samples are not required, unless the child is known to have a specific risk factor.
For children with cardiac or respiratory problems, an up-todate echocardiogram or sleep study may be relevant.
Positioning
A Rae uncuffed or microcuffed tube is positioned in the midline and secured to the lower face.
The taping of the tube needs to be secure but avoiding taping the mouth closed or limiting access. Taping in a V shape along the line of the mandible avoids displacing the tapes when the mouth gag is opened.
The child is placed supine on a warming blanket, with the head at the very end of the operating table.
A large horseshoe gel head ring is placed under the shoulders and around the head to provide support without overextending the neck.
A head drape is applied, and the face is prepped.
The table is tilted to a slight head-up position.
An operating microscope is used for the procedure. The height of the table is adjusted once the microscope has been brought into place (adjusted according to whether the surgeon prefers to sit or stand).
A modified Dingman mouth gag is placed.
A throat pack is placed, and a marker sticker put across the drapes as a reminder to ensure it is removed at the end.
The sticker is placed so that the drapes cannot be removed without needing to disturb the warning sticker.
The throat pack is also included in the scrub nurse count as an additional precaution.
The nose and mouth are rinsed with aqueous chlorhexidine solution.
Approach
The width of the cleft is measured. The extent of the cleft and any unusual features are noted.
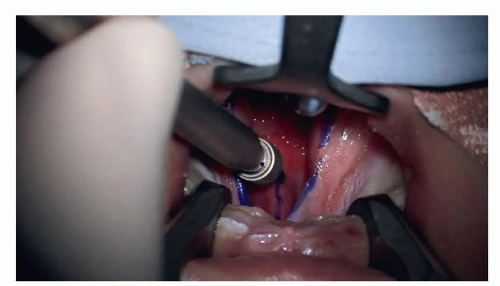
The incisions are marked with pen and ink (FIG 1).
Depending on the extent and shape of the anterior edge of the cleft, either a horseshoe shape or a triangular flap can be marked anteriorly.
The line of the incision in the soft palate can be identified by the pale line where the nasal mucosa meets the oral mucosa along the margin of the cleft.
For very wide clefts, lateral von Langenbeck incisions can be marked at the outset, or these can be decided later in the procedure after the closing tension around the hard palatesoft palate junction is apparent.
Tension is a factor of the soft tissue cleft width, the width of the lateral shelves of the palate, the elasticity of the tissue, and how vertical the shelves were sitting (which gives a “drawbridge effect”).
TECHNIQUES
▪ Hard Palate
Incisions and Dissection
Levobupivacaine or bupivacaine long-acting local anesthetic with adrenaline 1:100 000 is infiltrated and left about 8 minutes for vasoconstriction.
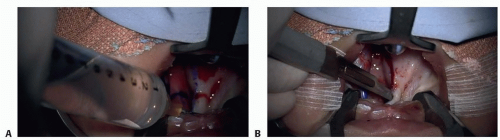
The injection is used to help hydrodissect the hard palate subperiosteal layer and the vomer flaps if these are being used (TECH FIG 1A)
The incision is begun along the cleft margin (or in the midline for a SMCP or rerepair).
For complete clefts of the palate, it is usually easier to start with the posterior two-thirds of the hard palate extending across the hard palate-soft palate junction, then to move on to the very anterior portion of the cleft, and finally to move on to the posterior soft palate and uvula (TECH FIG 1B).
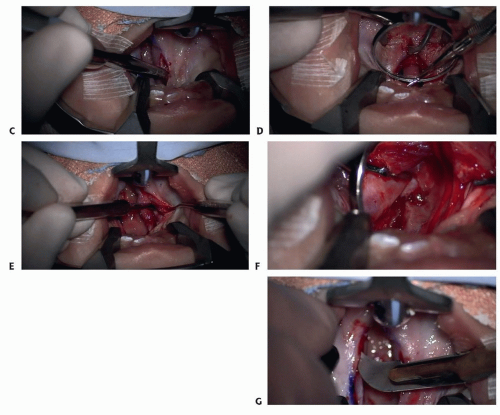
For clefts involving the hard palate, use a no. 15 blade to incise carefully down to the bone along the margin of the hard palate and 3 to 5 mm past the hard palate-soft palate junction and elevate subperiosteally with a periosteal elevator or Warwick-James elevator (TECH FIG 1C,D).
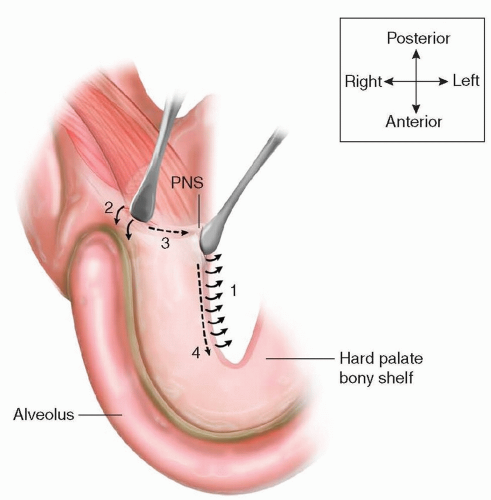
TECH FIG 2 • The stages of dissecting the nasal layer mucoperiosteal flap from the hard palate bony shelf. (1) Using a periosteal elevator with the spoon facing nasally, gently lift the periosteum off the margin of the bone with small movements. (2) Rotate periosteal elevator 180 degrees, so spoon faces orally, and insert it subperiosteally on nasal aspect of posterior edge of the bony shelf of the hard palate. (3) Wiggle and rotate spoon across the postnasal spine, the most adherent point. (Always return to position 2 if the periosteal elevator slips out of place.) (4) Continue to make wiggling and rotating movements with the periosteal elevator from the postnasal spine anteriorly.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree

 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access