Abstract
Correction of secondary deformities of the midface can happen even for the most experienced surgeons due to inadequate reduction. This chapter categorizes the correction of secondary defects based on the initial fracture patterns and deformity of midface caused by medial canthal deformity, orbitozygomaticomaxillary complex (OZMC) fractures and Le Fort fractures. The secondary correction of the central midface will be covered briefly in the context of Le Fort II and III fractures. Medial canthal correction can be done by osteotomy or epicanthoplasty techniques. Complications of OZMC fractures include poor 3-dimensional reduction resulting in residual cosmetic deformities and an increase in orbital volume with subsequent enophthalmos or dystopia. This can be corrected by onlay of bone or other materials if there are no associated ocular findings and reconstruction of the internal orbit. OZMC osteotomy is the optimal technique to address orbital volume, dystopia and projection, and width of the face. The key fit of the bony fractures at the zygomaticofrontal sutures, orbital rim, and lateral buttress of the maxilla are lost in delayed repair due to bone remodeling. Hence techniques such as intraoperative navigation, imaging, preoperative surgical cutting, and repositioning guides are of value. The most common maxillary defects encountered after Le Fort fractures are midface retrusion, decreased midfacial height, and anterior open-bite. Patients with Le Fort II or III fractures would benefit from reestablishing the old fractures and mobilization to help correct the orbital rim position and the malocclusion at the same time. Often recreation of the Le Fort II or III fractures may not help obtain the desired occlusion due to remodeling and associated soft tissue changes. In such situations, the Le Fort I osteotomy should be completed at the same time. The technique is similar to that of the Le Fort I osteotomy performed in orthognathic surgery, utilizing dental models and surgical splints.
Key Words
secondary midface deformity, zygoma malunion, zygoma osteotomy, onlay grafting, navigation, intraoperative imaging, medial canthal deformity, orbital dystopia, Le Fort fractures, dental malocclusion, anterior open-bite
Background
Secondary deformities resulting from complications in treating craniofacial injuries, specifically the midface, occur even when treated by experienced surgeons. Following proper surgical principles and recognizing the potential functional and aesthetic sequelae limits many complications. Ideal primary reconstruction is not always achieved. Displaced or missing bony segments result in an inadequate infrastructure, which interferes with the balance of the associated soft tissues. Lack of underlying support leads to loss of proper soft tissue dimensions and results in further reconstructive difficulty. The main focus of this chapter is the assessment of secondary deformities of the midface, specifically maxillary, zygomatic, and naso-orbito-ethmoid (NOE) fractures, and techniques for restoring both form and function are reviewed. Return of symmetry and function are the fundamental bases for reconstruction. An organized evaluation of facial structures including orbital position, bizygomatic width, and occlusion are crucial. The surgeon’s goal when addressing the midface is restoration of appropriate facial height, width, and projection ( Fig. 3.8.1 ).
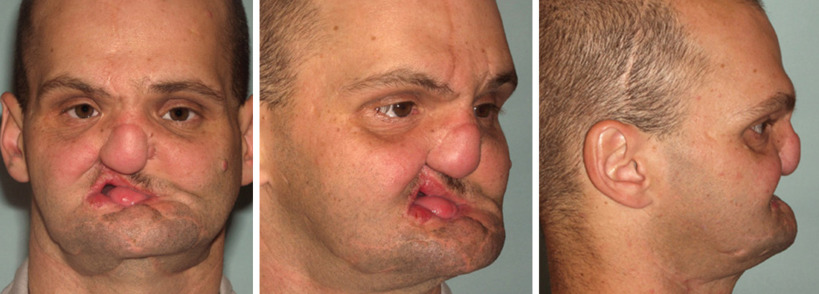
There are multiple reasons for requiring a secondary correction. These include poor reduction, inadequate stabilization, and delayed treatment or nontreatment. When insufficient closed reduction or fixation means are applied, loss of skeletal and soft tissue support occurs. It is also important to understand that the first operation provides the best opportunity for a good outcome. Primary restoration of proper skeletal framework and immediate placement of grafts in areas of bone loss provides the necessary structure needed to maintain soft tissue contour. This reduces the severity of complications requiring secondary management. Operative correction of established traumatic deformities with associated soft tissue changes and permanent disfigurement poses a formidable challenge. The important aspects in reconstruction are a detailed assessment of the patient including a thorough history and physical examination, and adequate imaging studies, such as a computed tomography (CT) scan. The early correction of midface fractures yields better facial form than the treatment of established deformities. Beyond one year, the timing of repair of these defects has less influence on eventual esthetic and functional outcome.
In order to plan for secondary revision, sufficient assessment of the bone and soft tissues must be achieved. Minor distortions may be managed by more conservative options, whereas gross deformities will likely require aggressive treatment such as osteotomy and repositioning. Therefore, proper presurgical evaluation is the most important initial step when addressing secondary deformity. For this chapter, we will categorize the correction of secondary defects based on the initial fracture such as the central midface and medial canthal deformity associated with NOE fractures, orbitozygomaticomaxillary complex (OZMC) fractures and Le Fort fractures.
The functional deficits due to midfacial deformities can be grouped into ophthalmological, sinonasal, and masticatory issues. The most common ophthalmological deficit is diplopia and this is due to globe malpositioning and from adaptive changes within the extraocular muscles. The inferior rectus and superior oblique muscles are frequently involved with posttraumatic and postsurgical scarring. The secondary correction typically involves creation of stable and anatomical orbital architecture followed by delayed extraocular muscle surgery. Secondary repositioning of periorbital bony segments may further exacerbate diplopia.
Functional problems of the sinonasal system include obstruction of the nasal airway and paranasal sinuses. Septorhinoplasty and endoscopic sinus procedures can be performed at a later time. The masticatory dysfunction is primarily due to malocclusion. This will be discussed further in the section on Le Fort fractures.
Central Midface and Medial Canthal Deformity
The central midface consists of the paired nasal bones that form the nasal sidewalls and medial orbital rims conjointly. This region is common to NOE fracture, Le Fort II and III fractures. If uncorrected or inadequately treated, the secondary deformity is extremely difficult to correct. The pivotal structure that is present in this region is the medial canthal tendon. This tendon supports the canthus, enables proper apposition between the eyelid and the globe, and includes the lacrimal canaliculi. In order to have acceptable functional and esthetic outcomes, the surgeon must restore nasal projection, intercanthal width, orbital volume, and a functional lacrimal system.
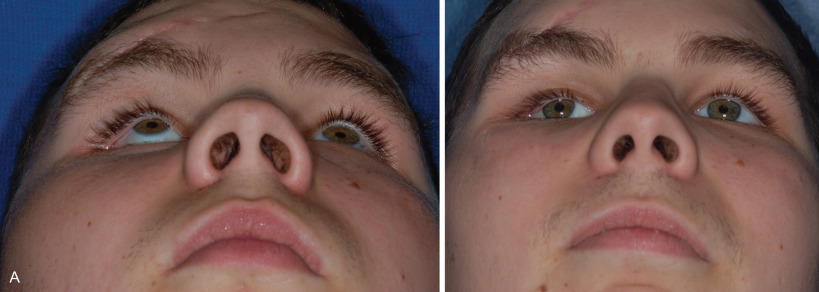
The majority of late complications resulting from inadequate management of medial canthal tendons are cosmetic in nature. Late deformities include a shortened palpebral fissure, telecanthus, enophthalmos, ocular dystopia, and a shortened nose with saddle deformity of the nasal dorsum. The main components involved in NOE deformities are the medial canthal area, the nose, and the medial internal orbit. There is often significant scar contracture and soft tissue thickening ( Fig. 3.8.2 ).
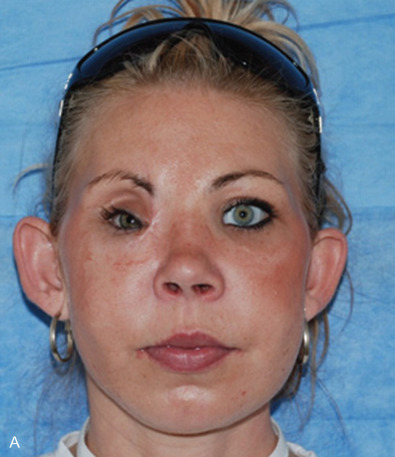

The secondary correction of the medial canthal tendon-bearing fragment in the central midface is managed similarly for NOE fracture and comminuted Le Fort II and Le Fort III fractures. In this chapter we will briefly discuss the management of the deformity surrounding the medial canthus. NOE fractures are discussed in detail in other chapters.
Medial Canthal Correction
Telecanthus can be corrected by re-osteotomy and repositioning medially of the old fracture site containing the medial canthal attachment. The transnasal wire when placed anterior to the medial canthal attachment will widen the posterior portion of the segment and thus laterally displace the medial canthal tendon. If one canthus is superior to the other, the inferior canthus should be elevated to achieve symmetry.
If the medial canthal tendon is detached during previously operated NOE fracture, Le Fort II or Le Fort III, the medial canthal tendon itself must be found and engaged with a wire. In this situation, a small incision can be used directly over the tendon area in the skin to locate and secure the medial canthal tendon. Engaging the tendon alone tends to produce a “bow-string” appearance and also has the propensity to drift laterally over time. When absent or deficient bone is present, a calvarial graft can be placed and then the transnasal wire can be pulled through the graft and secured with a transnasal wire or perhaps a mini bone anchor.
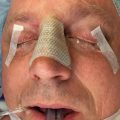
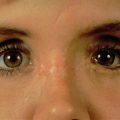
Medial canthal tissue thickening due to hematoma formation and scarring can be encountered if the medial canthal tendon is not addressed previously. The oblique transnasal wiring technique with Y–V epicanthoplasty incision is adequate and would assist in minimizing unsightly scar formation ( Fig. 3.8.3A–B ). Masking of telecanthus can be done by dorsal nasal augmentation to increase the nasal profile and decrease the appearance of telecanthus. This technique will also lengthen the nose and raise the radix.


Medial Wall Osteotomy
When the medial canthal tendon is displaced laterally with the bony medial orbital wall, either due to NOE or Le Fort III fracture with comminution, this results in medial orbital wall hypertelorism. Poor frontonasal angle and poor nasal projection combined with associated telecanthus or traumatic orbital hypertelorism compound the severity of the apparent deformity making the patient look worse ( Fig. 3.8.4A–C ).


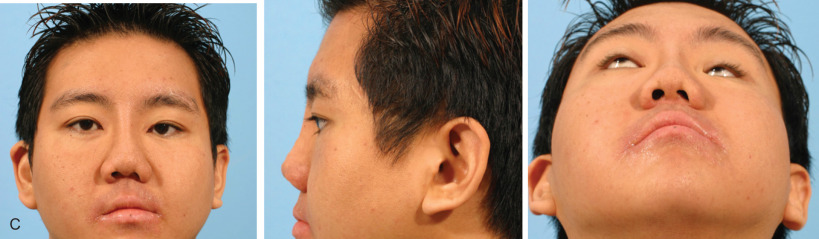
Zygoma Fractures Secondary Deformity
The zygomatic bone is an anatomical structure that determines the outer shape of the midface. It constitutes the lateral two-thirds of the orbital floor and lateral wall. Secondary deformities can occur due to delay in diagnosis, inability to correct in an appropriate time period or poor reduction of the zygoma. The majority of unfavorable outcomes relate to improper orientation of the zygomatic complex in three dimensions, which leads to failure to restore the facial dimensions and contour. The most common complications relate to poor cosmetic results, abnormalities in globe position, and malpositioned lateral canthus position. The common abnormal globe position is enophthalmos and inferior displacement. This is due to persistently increased orbital volume and inadequate correction of internal orbital defects. The meridian of the globe is at the lateral rim. A small external rotation of the lateral orbital wall often results in an increased intraorbital volume. Late enophthalmos may also result from scarring or atrophy of orbital soft tissues despite attempts at adequate reconstruction. Successful reconstruction of zygoma fractures is dependent on the correction of midface height, width, and projection. Recent emphasis is placed on the zygomaticomaxillary buttress (as opposed to the zygomaticofrontal region), not only because it is typically the mobile area but also because of its importance in restoring facial height.
As malar projection decreases, facial width tends to increase. Restoring facial balance thus requires understanding ideal zygomatic positioning and returning displaced segments to these dimensions. Complications of zygomatic fractures include poor 3-dimensional reduction resulting in residual cosmetic deformities and an increase in orbital volume with subsequent enophthalmos or dystopia.
A displaced zygoma typically results in facial widening and inadequate malar projection. Severe cases will likely require osteotomy and repositioning as well as bone grafting to achieve proper aesthetic balance ( Fig. 3.8.5 ).

ZMC Secondary Correction
The goals of secondary surgical correction are the same as primary treatment. The surgical treatment of ZMC fractures is organized into two goals: (1) restoration of facial projection and facial symmetry and (2) restoration of orbital volume, globe position, and shape of the affected palpebral fissure. Delayed repair of greater than 4 months after injury commonly requires not only osteotomy of the segments but also bone grafting. This is due to osseous healing and bone resorption that has occurred. For cases requiring refracture with osteotomies, mobilization of the ZMC can be challenging due to the scar contractures of adjacent soft tissues. In order to gain sufficient mobility, all attachments should be released, including the masseter.
Facial symmetry is achieved by restoring the 3-dimensional position of the malar prominence and orbital volume is restored by alignment of the zygoma with its internal and external articulations such as the sphenoid. The secondary correction of the zygoma deformities can be done by reosteotomy, onlay grafting techniques, soft tissue fillers (autogenous fat or fillers) or a combination of techniques. The minor deformities are managed with augmentation or reduction procedures to camouflage the asymmetry. The larger corrections would typically require reosteotomy, repositioning, and supplemental bone grafting. Adjunctive soft tissue resuspension is often helpful. This can be done with lower eyelid incisions of endoscopic midface lift.
Onlay Grafting
The minor secondary deformity from zygoma malposition can be managed by onlay grafting and bony recontouring. This is especially the choice when there is good orbital volume restoration and no enophthalmos or dystopia. Due to irregular remodeling and resorption in older fractures, when repositioning segments, overcorrection as well as onlay grafting is needed. Overcorrection of the onlay graft is an important consideration because there will likely be some resorption of this bone over time. The onlay graft’s site and extent of augmentation should be established preoperatively. Intraoperative judgment of the extent of necessary augmentation to achieve symmetry is extremely difficult, due to distortion of overlying soft tissues as a result of the surgical access, edema, and presence of an endotracheal tube.
In minor deformities, masking with fat injections or high-density polyethylene/silicone malar implants and soft tissue resuspension will be pursued. The “ideal” characteristics of onlay grafts include the following: biocompatible, no risk of disease transmission, resistant to infection, dimensionally stable, easy to shape or mold, amenable to skeletal fixation, and long shelf-life. More recently, customized polyetheretherketone (PEEK) implants are more frequently utilized. With the advances of 3D imaging and advancement in biocompatible alloplastic materials, there has been a recent shift to consideration of patient-specific implants created using 3D CT scans. These implants have the distinct advantage of being tailored precisely to the exact size and contour of the defect, thus reducing intraoperative time and adjustment. Other advantages of PEEK implants include excellent chemical resistance (corrosion and acid), biocompatibility, ideal imaging properties (X-ray and CT translucency with no artifacts, and magnetic resonance imaging compatibility with no magnetic interferences), and a modulus that can be tailored by adding reinforcing fibers that enable their mechanical properties to be increased significantly ( Fig. 3.8.6A–C ).