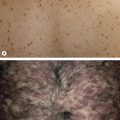
Abstract
Retinoids are analogs of vitamin A that exert multiple effects on cellular differentiation and proliferation, the immune system, and embryonic development. A thorough understanding of their mechanisms of action, formulations, administration, and potential adverse effects enables dermatologists to effectively and safely treat patients with a variety of cutaneous disorders. Topical retinoids are used to treat a number of conditions including acne, photoaging, and psoriasis, with skin irritation representing a limiting factor. Oral retinoids are the most effective drugs available for severe acne (isotretinoin) and many disorders of cornification (acitretin and isotretinoin), and they are also helpful in the management of inflammatory and neoplastic skin diseases; careful patient selection and monitoring are required due to their teratogenicity and other potential toxicities.
Keywords
vitamin A, retinoids, retinol, retinaldehyde, retinoic acid, isotretinoin (13- cis- retinoic acid), alitretinoin (9- cis -retinoic acid), acitretin, bexarotene, tazarotene, adapalene, tretinoin (all- trans -retinoic acid)
- ▪
Retinoids are structural and functional analogues of vitamin A that exert multiple effects on cellular differentiation and proliferation, the immune system, and embryonic development
- ▪
Retinoic acid receptors (RARs) and retinoid X receptors (RXRs) are ligand-dependent transcription factors belonging to the steroid–thyroid hormone nuclear receptor superfamily
- ▪
Topical retinoids are used to treat a number of conditions including acne, photoaging, and psoriasis; the limiting factor is dose-related skin irritation, and teratogenicity risk is very low to non-existent
- ▪
Oral retinoids are the most effective drugs available for severe acne (isotretinoin) and many disorders of cornification (acitretin and isotretinoin). They are also helpful in the management of psoriasis, especially pustular and erythrodermic forms (acitretin > isotretinoin), pityriasis rubra pilaris (acitretin and isotretinoin), cutaneous T-cell lymphoma (bexarotene), and chronic hand eczema (alitretinoin)
- ▪
Systemic retinoid therapy requires careful patient selection and monitoring due to associated teratogenicity and other potential toxicities; laboratory abnormalities (e.g. hypertriglyceridemia, elevated transaminases); ocular, musculoskeletal, and (primarily for bexarotene) endocrinologic or hematologic adverse effects
Introduction
Vitamin A (retinol) and related compounds with either structural (retinol derivative) or functional (vitamin A activity) similarities are known as retinoids ( Fig. 126.1 ). The importance of retinoids in cutaneous biology was first appreciated early in the twentieth century by Wolbach , who observed that vitamin A-deficient animals manifested altered keratinization, such as epidermal hyperkeratosis and squamous metaplasia of mucous membranes as well as certain precancerous conditions. The anti-keratinizing properties of vitamin A led von Stuettgen and Bollag to administer topical and systemic retinoids to treat disorders of cornification. In initial clinical trials with oral vitamin A, tolerable doses were ineffective but higher, potentially effective doses were too toxic. Because of this narrow therapeutic window, a program was launched to engineer synthetic retinoids with higher therapeutic activity and lower toxicity. Parallel to efforts with systemic agents, a growing interest in topical retinoids emerged.
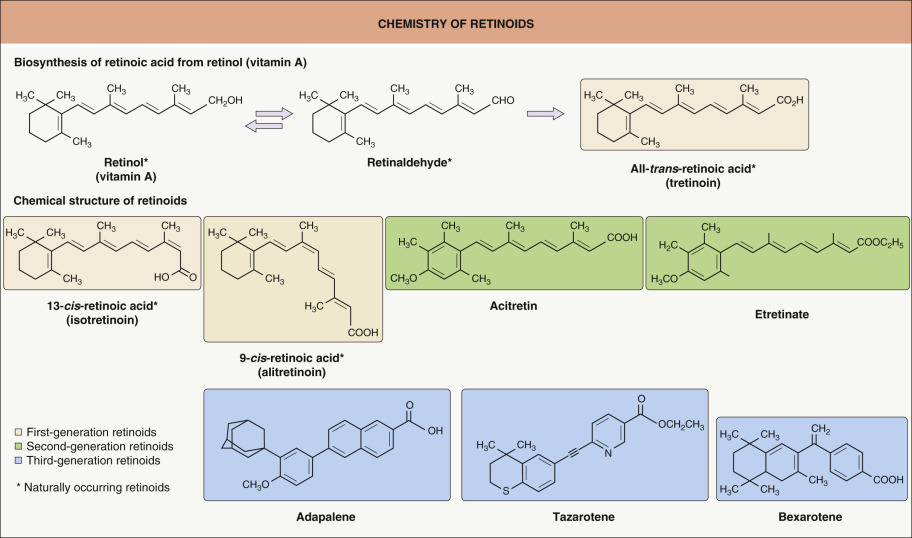
All- trans -retinoic acid (a t -RA; tretinoin), a naturally occurring metabolite of retinol (see Fig. 126.1 ), was the first retinoid to be synthesized. Orally, it did not have significant advantages over vitamin A, and, as a result, the primary dermatologic focus became its topical use, especially for acne vulgaris and photoaging. However, oral tretinoin is an important component of therapeutic regimens for acute promyelocytic leukemia, where its ability to promote cellular differentiation is utilized.
Initially synthesized in 1955, 13- cis -retinoic acid (13- cis -RA; isotretinoin) was first studied clinically almost two decades later. Its use was delayed by concerns regarding its teratogenicity, which were amplified because of the thalidomide tragedy. Results of isotretinoin treatment of psoriasis were equivocal, and etretinate was subsequently found to be more effective. In the mid to late 1970s, Peck and colleagues described the effectiveness of oral isotretinoin in the treatment of lamellar ichthyosis and other disorders of cornification as well as its ability to produce complete responses with prolonged remissions in patients with treatment-resistant nodulocystic acne. Topical isotretinoin has also been formulated and has efficacy similar to that of topical tretinoin for acne. In 1999, the US Food and Drug Administration (FDA) approved 9- cis -retinoic acid (9- cis -RA; alitretinoin) 0.1% gel for the topical treatment of cutaneous Kaposi sarcoma. To date, oral alitretinoin has been approved outside of the US to treat severe, recalcitrant hand eczema.
In 1972, Bollag developed two aromatic retinoids: etretinate and its free acid metabolite, acitretin. Both had a therapeutic index ten times more favorable than that of tretinoin in the chemically induced rodent papilloma test model. Etretinate and acitretin represent second-generation retinoids, and their development constituted a breakthrough in the systemic treatment of psoriasis and disorders of cornification.
A major advance in understanding the molecular pharmacologic features and mechanisms of action of retinoids came with the discovery of nuclear receptors known as retinoic acid receptors (RARs) and retinoid X receptors (RXRs). This allowed the development of new retinoids that target specific retinoid receptors. Third-generation retinoids include topical adapalene (acne), topical tazarotene (psoriasis and acne), and oral as well as topical bexarotene (cutaneous T-cell lymphoma [CTCL]). Lastly, topical retinol and retinaldehyde, the precursors of retinoic acid, are included in cosmeceutical products.
Mechanism of Action
Retinoids are involved in the regulation of diverse biologic functions ( Table 126.1 ). They affect cellular growth, differentiation and morphogenesis; inhibit tumor promotion and malignant cell growth; exert immunomodulatory actions; and alter cellular cohesiveness .
| BIOLOGIC FUNCTIONS OF RETINOIDS |
| Functions of vitamin A (retinol) * |
|
| Biologic effects of retinoids |
|
* Retinoic acid can substitute for retinol with regard to growth, morphogenesis, and epithelial differentiation; it cannot substitute completely for retinol in reproductive function, nor can it replace retinaldehyde in the visual system.
Vitamin A Metabolism
Vitamin A (retinol) must be acquired through the diet and is ingested as retinyl esters and provitamin A carotenoids; of the latter, beta-carotene is particularly efficient in its ability to be converted to vitamin A. Within the intestinal lumen, retinyl esters are hydrolyzed to retinol, which is then absorbed and stored in the liver in the ester form (especially retinyl palmitate; Fig. 126.2 ). Retinol and its esters represent the main dietary source, as well as transport and storage form, of vitamin A. Once inside the bloodstream, after release of the retinyl ester (storage form) from the liver, retinol is transported bound to a complex of retinol-binding protein (RBP) and transthyretin. The uptake of retinol from the RBP–transthyretin complex to target cells is mediated by STRA6 (stimulated by retinoic acid 6), a dimeric transmembrane protein that acts as an RBP–retinol receptor .
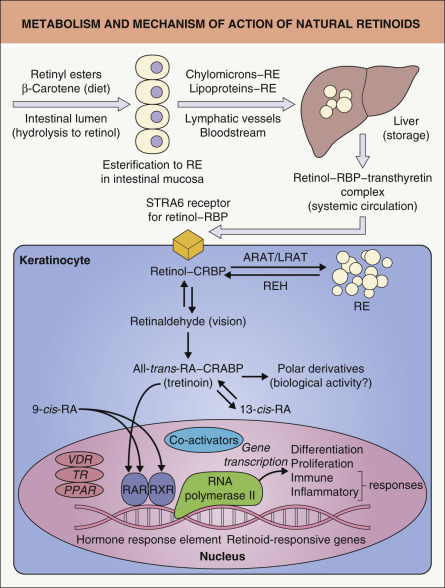
The cellular pathway leading to conversion of retinol to a t -RA, the biologically active ligand that binds to nuclear receptors, consists of a two-step process (see Figs 126.1 & 126.2 ). Retinol (vitamin A alcohol) is first reversibly oxidized to retinaldehyde (vitamin A aldehyde), which is then irreversibly converted to retinoic acid (vitamin A acid). Cellular RBP (CRBP-I) facilitates these enzymatic reactions by delivering retinol to appropriate enzymes.
Two additional intracellular carriers, cellular retinoic acid-binding proteins (CRABP-I and CRABP-II), are thought to function in transporting retinoic acid to the nucleus as well as buffering the level of free a t -RA in the cell. The latter is accomplished by sequestering a t -RA and by promoting metabolism of a t -RA by cytochrome P450 enzymes belonging to the CYP26 family (e.g. CYP26A1). CRABP-I regulates the metabolic fate of its ligands by directly affecting the activities of RA-metabolizing cytochrome P450 enzymes, while CRABP-II markedly stimulates the RA-induced transcriptional activity of RAR through protein–protein interactions .
Intracellularly, retinoic acid is found in both all- trans and 9- cis configurations (see Fig. 126.2 ). Physiologically, a t -RA is the predominant retinoic acid form, and only a very small fraction is isomerized into 13- cis -RA. a t -RA is the primary active ligand that binds to the three known nuclear RARs, which mediate, at least in part, the molecular and cellular effects of retinoic acid.
Retinoid Receptors
Retinoids exert most of their physiologic effects on DNA transcription by binding to two distinct families of nuclear receptors, RARs and RXRs. These receptor families belong to a superfamily of nuclear receptors that act as ligand-activated transcription factors and include the steroid, vitamin D 3 , and thyroid hormone receptors as well as peroxisome proliferator-activated receptors (PPARs). The RAR and RXR receptor families each contain three receptor isotypes (α, β and γ) encoded by different genes. a t -RA (tretinoin) binds only to RARs, whereas 9- cis -RA (alitretinoin) binds both to RARs and RXRs ( Table 126.2 ).
| KEY PHARMACOLOGIC FEATURES AND NUCLEAR BINDING PROFILE OF RETINOIDS | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Retinoid | Type | Systemic absorption or bioavailability * (% dose) | Elimination half-life | Metabolism | Excretion | Nuclear receptor binding affinity | |||||
| RAR | RXR | ||||||||||
| α | β | γ | α | β | γ | ||||||
| Topical retinoids * | |||||||||||
| Tretinoin ** (all- trans -retinoic acid) | Natural (1 st generation) | <2% in normal skin | Normally present in the skin | Isomerization to 13- cis -RA (epidermis) | Desquamation, biliary | + | + | + | – | – | – |
| Alitretinoin (9- cis -retinoic acid) | Natural (1 st generation) | Minimal | Normally present in the skin | Main metabolite: 4-oxo-9- cis -RA | Desquamation, biliary | + | + | + | + | + | + |
| Adapalene | 3 rd generation | Minimal | Unknown | Minimal biotransformation due to chemical rigidity | Desquamation, biliary | ± | + | + | – | – | – |
| Tazarotene | 3 rd generation | <1–6% in normal skin | 16 hours (tazarotenic acid) | Rapid (within 20 minutes) ester hydrolysis within the skin to form its active metabolite, tazarotenic acid; excreted metabolites: sulfoxides, sulfones | Desquamation, renal (within 3 days), biliary (within 7 days) | ± | + | + | – | – | – |
| Systemic retinoids | |||||||||||
| Tretinoin ** | Natural (1 st generation) | 50% | 1 hour | Hepatic; main metabolites: cis – and trans -4-oxo derivatives | Biliary, renal | + | + | + | – | – | – |
| Isotretinoin (13- cis -RA) | Natural (1 st generation) | 25% | 20 hours | Hepatic, endogenous concentration reached within 2 weeks; main metabolite: 4-oxo-isotretinoin | Biliary, renal | – | – | – | – | – | – |
| Alitretinoin | Natural (1 st generation) | Unknown | 2–10 hours | Hepatic; main metabolite: 4-oxo-alitretinoin | Renal, biliary | + | + | + | + | + | + |
| Acitretin (and etretinate) | 2 nd generation | 60% | 2 days | Hepatic, re-esterification to etretinate indirectly increased by alcohol consumption; main metabolite: cis -acitretin | Biliary, renal | + † | + † | + † | – | – | – |
| Bexarotene ‡ | 3 rd generation | Unknown | 7–9 hours | Hepatic | Biliary | – | – | – | + | + | + |
* Topical formulations have limited propensity for distribution to systemic tissues; oral bioavailability is highly variable and increases when administered with food.
** Also binds the cellular retinoic acid-binding protein (CRABP).
† Activate RARs despite binding poorly to them.
RARs function as heterodimers with RXRs, whereas RXRs may also act as homodimers or participate in the formation of heterodimers with a variety of other nuclear receptors, including vitamin D 3 , thyroid hormone, and PPARs. Such heterodimers provide a mechanism for cross-talk between nuclear hormone signaling pathways. Dimers of retinoid receptors (RAR/RXR or RXR/RXR) are localized to the nucleus and bind, even in the unliganded state, to specific DNA regulatory sequences called retinoid hormone response elements (RAREs) in the promoter regions of retinoid-responsive genes (see Fig. 126.2 ). Unliganded receptors bind to co-repressor molecules and repress transcription. However, when the receptor binds its ligand, it undergoes a conformational change resulting in the release of co-repressors and recruitment of co-activators. These molecules include histone acetylases that change the conformation of chromatin and allow access to DNA by transcriptional machinery. The retinoid–receptor complex thereby modulates the transcription of specific sets of genes, and it is likely that many of the differentiation-inducing actions of retinoids are mediated by this mechanism.
In addition to direct upregulation of gene transcription via binding of retinoid–receptor complexes to RAREs, retinoids can have indirect effects on gene transcription that result from the downregulation of genes that do not contain RAREs in their promoter region. The retinoid–receptor complex is thought to antagonize transcription factors such as activator protein-1 (AP1) and nuclear factor-interleukin-6 (NF-IL6) by competing for the same set of required co-activator proteins, thereby leading to decreased expression of AP1 and NF-IL6-responsive genes; expression of the latter genes promotes cellular proliferation and inflammation. The antiproliferative and anti-inflammatory actions of retinoids are believed to be mediated by this type of indirect negative gene regulation. In particular, retinoic acid has important roles in inhibiting IL6-driven induction of proinflammatory Th17 cells and in promoting differentiation of anti-inflammatory regulatory T cells. The anti-inflammatory effects of a t -RA (tretinoin) have also been associated with its ability to regulate the expression and activation of Toll-like receptors (TLRs), especially TLR2. The biologic relevance of non-genomic effects of retinoids (e.g. phosphorylation, membrane effects) remains under investigation.
The existence of several types and varied distributions of receptors, dimers, hormone response elements, and regulatory proteins shows that retinoid action is mediated via multiple pathways and results in a complex process of activation or inhibition of a large set of coordinately regulated genes However, the exact mechanism of retinoid action in many dermatologic conditions is still unknown, and, so far, the nuclear receptor concept does not fully explain the biologic diversity of retinoid effects.
Retinoids in the Skin
Vitamin A and its bioactive metabolites play a major role in promoting the keratinocyte differentiation that occurs from the epidermal basal layer to the stratum corneum . Retinyl esters and retinol are the major retinoids found in the skin, with the former reaching a concentration of >1000 pmol/g in the epidermis. Epidermal retinoids can absorb UVB radiation and have ~2–3% of the UVB-filtering capacity of the melanin in phototype II/III skin . The UVB absorption process results in dramatic depletion of epidermal retinoids, which can be prevented by application of topical retinoids . Nutritional deficiency, aging, and oxidative stress can also lead to lowered retinoid levels in the skin . There has been an ongoing debate regarding possible generation of reactive oxygen species upon the interaction of UVA radiation with retinyl esters (e.g. retinyl palmitate) present in cosmetics and sunscreens, but the theoretical potential for photocarcinogenicity has not been shown to be clinically relevant.
Synthetic Retinoids
Three generations of synthetic retinoids have been developed (see Fig. 126.1 ). The first-generation non-aromatic retinoids (tretinoin, isotretinoin, alitretinoin) are produced by chemically modifying the polar end group and the polyene side chain of vitamin A. Second-generation mono-aromatic retinoids (etretinate, acitretin) are formed by replacing the cyclic moiety of vitamin A with different substituted and unsubstituted ring systems. The third-generation poly-aromatic retinoids (adapalene, bexarotene, tazarotene), called arotinoids, are produced by cyclization of the polyene side chain.
Commercially available retinoids differ not only in their spectrum of clinical efficacy but also in their observed toxicity and pharmacokinetics. Each retinoid should be investigated as a unique drug, and the lack of disease response to one retinoid does not necessarily signify unresponsiveness to other retinoids.
The oral bioavailability of all retinoids is considerably enhanced when administrated with food, especially with a fatty meal, due to their lipophilic properties. Retinoid metabolism is predominantly hepatic; it involves oxidation and chain shortening to biologically inactive and polar metabolites, facilitating biliary and/or renal elimination. The oxidative metabolism is induced by the retinoids themselves and possibly also by other agents known to stimulate hepatic cytochrome P450 isoforms. Table 126.2 summarizes the key pharmacologic features and nuclear binding profiles of retinoids used in dermatology.
Adapalene
Adapalene is a photostable, rigid, and highly lipophilic synthetic retinoid with higher affinity for RAR-β/γ than for RAR-α. Since RAR-β is not expressed in keratinocytes, RAR-γ is the primary target receptor for adapalene in the epidermis. Adapalene does not bind to cellular retinoic acid-binding proteins (CRABPs) but does induce expression of CRABP-II. Its lipophilic properties may contribute to better pilosebaceous uptake and anti-acne activity. Given its negligible transdermal absorption, the teratogenic risks of topical adapalene appear to be minimal. While adapalene affects the cellular differentiation, keratinization, and inflammatory processes that are abnormal in acne, it has no sebostatic effect.
Tazarotene
Tazarotene is a prodrug that is rapidly converted by cutaneous esterases to its free carboxylic acid (tazarotenic acid), which is the active metabolite. It has a higher affinity for RAR-β/γ than for RAR-α and no affinity for RXR. Because of its rapid metabolism, systemic exposure is low. Tazarotene appears to modulate the pathogenesis of psoriasis by regulating expression of retinoid responsive genes, including those involved in cell proliferation, cell differentiation, and inflammation.
Acitretin
Acitretin is the major metabolite and the pharmacologically active form of etretinate. Although acitretin and etretinate are equally effective, acitretin has much more rapid elimination. Etretinate is approximately 50 times more lipophilic than acitretin and binds strongly to plasma proteins, particularly lipoproteins and albumin. Etretinate is stored in adipose tissue (including subcutaneous fat), from which it is released slowly, with a long terminal half-life of up to 120 days. Under identical conditions, acitretin carries a negatively charged group that makes it much less lipophilic than etretinate. As a result, acitretin does not accumulate in adipose tissue and is eliminated from the body more rapidly, with a half-life of 2 days.
The major serious adverse effect of oral retinoids is teratogenicity, and, therefore, the length of time that these drugs are present in the body is of great importance. Re-esterification of acitretin to etretinate may occur when acitretin is taken simultaneously with alcohol. This finding prompted the manufacturer to extend the time of contraception for female patients with childbearing potential taking acitretin to 2 years after its discontinuation, as it is for etretinate. The FDA advises a contraceptive period of at least 3 years for acitretin, based on the pharmacokinetics of acitretin and etretinate observed in clinical trials and on previous safety experience with etretinate. However, acitretin retains its shorter half-life in women who strictly avoid alcohol during treatment and for 2 months thereafter . Because of its improved risk–benefit ratio, acitretin was approved by the FDA in 1996 as a substitute for etretinate, which is no longer commercially available .
Acitretin’s mechanism of action is still not clearly understood. Paradoxically, it activates all three RAR subtypes despite binding poorly to them. Evidence supports a normalization of differentiation and proliferation as well as a modification of inflammatory responses and neutrophil function.
Isotretinoin (13- cis -retinoic acid)
Isotretinoin is a naturally occurring retinoid resulting from the metabolism of vitamin A (see Fig. 126.2 ). 13- cis -RA and a t -RA are two physiologically interconvertible isomers that differ in their elimination half-lives: approximately 20 hours and 1 hour, respectively. Isotretinoin undergoes first-pass metabolism in the liver and subsequent enterohepatic recycling. In plasma, more than 99% of isotretinoin is protein-bound, mainly to albumin. There is neither liver nor adipose tissue storage, in contrast to vitamin A. The major metabolite of isotretinoin, 4-oxo-isotretinoin, is produced by oxidation. Isotretinoin and its metabolites are excreted in the urine and feces. After discontinuation of isotretinoin, physiologic concentrations of the drug and its major metabolites are reached within 2 weeks, ranging from 2 days for a t -RA to 10 days for 4-oxo-isotretinoin. Therefore, 1 month of post-therapy contraception provides an adequate safety margin to avoid teratogenicity.
Among natural and synthetic retinoids, only oral isotretinoin and its 4-oxo-isotretinoin metabolite significantly suppress sebum production, which explains their dramatic effects on acne. Isotretinoin-induced seboatrophy is unlikely to be RAR/RXR-mediated since isotretinoin has no clear affinity for any known retinoid receptor , and potent RAR/RXR ligands such as tretinoin and alitretinoin do not lead to seboatrophy. The mechanism of isotretinoin-induced seboatrophy is thought to involve sebocyte apoptosis , but inhibition of either sebocyte progenitor differentiation or the genes encoding sebogenic enzymes represent two other possible pathomechanisms.
Bexarotene
Bexarotene, an RXR-selective retinoid (rexinoid), is FDA-approved in oral (1999) and topical (2000) forms for treatment of CTCL. This compound is about 100-fold more potent at binding to RXRs than to RARs. In plasma, bexarotene is highly bound (>99%) to various proteins that have yet to be characterized. Bexarotene has a clearance profile similar to that of isotretinoin, with a terminal half-life of between 7 and 9 hours . Bexarotene is metabolized by CYP3A4 and generates its own oxidative metabolites via hepatic CYP3A4 induction. Neither bexarotene nor its metabolites are excreted in the urine; their elimination is thought to occur primarily via the hepatobiliary system . The exact mechanism of action of bexarotene in CTCL is still unknown, but it probably acts through regulation of cellular differentiation and proliferation, as well as by induction of apoptosis.
Alitretinoin (9- cis -retinoic acid)
Alitretinoin is a naturally occurring pan-agonist retinoid that binds to both RARs and RXRs , representing the endogenous ligand for the latter. Topical alitretinoin 0.1% gel is indicated for the treatment of cutaneous Kaposi sarcoma and oral alitretinoin therapy is currently utilized outside the US for refractory chronic hand eczema. The absorption of oral alitretinoin from the gastrointestinal tract is variable and dose-proportional over the therapeutic range of 10–30 mg daily; the absolute bioavailability of alitretinoin has not been determined. Alitretinoin is metabolized via oxidation by CYP3A4 enzymes of the liver into 4-oxo-alitretinoin, and both the parent drug and its metabolite also undergo isomerization into a t -RA and 4-oxo-a t -RA, respectively. Elimination is primarily renal, with the half-life of unchanged alitretinoin ranging between 2 and 10 hours. Alitretinoin concentrations return to normal within 1–3 days after treatment cessation.
The mechanism of action of alitretinoin in chronic hand eczema is unknown. Alitretinoin has immunomodulatory and anti-inflammatory effects that include suppressing the expansion of cytokine-activated leukocyte subsets and antigen-presenting cells.
Retinoic acid metabolism blocking agents
R etinoic a cid m etabolism b locking a gents (RAMBAs) inhibit catabolism of a t -RA by P450 enzymes in the CYP26 family, thereby raising the intracellular levels of endogenous a t -RA in the skin and other targeted tissues . This limits systemic exposure and the potential for toxicity, and a t -RA levels return to the physiologic range within 24 hours of discontinuing these medications. Liarozole, an imidazole derivative without antifungal properties, is a RAMBA with low isoenzyme specificity that also inhibits P450-mediated pathways of steroid biosynthesis whereas talarozole, a triazole derivative, is a more selective and highly active CYP26 enzyme inhibitor. Liarozole has been granted orphan drug status for congenital ichthyosis by the European Commission and the FDA. In a recent randomized, placebo-controlled phase II/III trial in 64 patients with moderate-to-severe lamellar ichthyosis, a 41–50% response rate was observed in patients receiving liarozole, compared to 11% with placebo, with borderline statistical significance (p = 0.056) .
Indications ( Table 126.3 )
Topical Retinoids
The most important element in topical retinoid therapy is patient education. Local skin irritation can be expected, and noticeable beneficial effects may take weeks or months to appear. Administration of topical retinoids should be titrated depending on cutaneous irritation, which may mean decreasing the concentration or the frequency of application. It is generally wise to begin with a low-strength formulation and then increase the concentration as tolerance builds. Another tactic is to start by applying a given concentration every other day. Daytime moisturizers with sunscreen are important components of any topical retinoid regimen.
| CLINICAL INDICATIONS FOR RETINOIDS IN DERMATOLOGY | |||
|---|---|---|---|
| Topical retinoids | FDA-approved indications | Acne vulgaris (tretinoin, adapalene, tazarotene) Photoaging, e.g. wrinkling, mottled pigmentation, facial roughness (tretinoin, tazarotene) Psoriasis, <20% of body surface area (tazarotene * ) Cutaneous T-cell lymphoma (bexarotene) Kaposi sarcoma (alitretinoin) | |
| Selected non-FDA-approved indications | Some disorders of cornification (ichthyoses) Darier disease Pityriasis rubra pilaris Rosacea Pigmentary disorders, e.g. melasma, postinflammatory hyperpigmentation Lentigines Actinic keratoses Striae Wound healing Lichen planus (oral and cutaneous) Verrucae planae (flat warts) Corticosteroid-induced atrophy Therapy and prevention of skin cancer (basal cell carcinoma; xeroderma pigmentosum) | ||
| Systemic retinoids | FDA-approved indications | Psoriasis (acitretin) | Pustular psoriasis (localized and von Zumbusch) Erythrodermic psoriasis Severe and recalcitrant plaque-type psoriasis * |
| Acne (isotretinoin) | Nodulocystic acne Recalcitrant acne with tendency for scarring | ||
| Cutaneous T-cell lymphoma (bexarotene) | Resistant to at least one systemic therapy | ||
| Selected non-FDA-approved indications | Rosacea and acne-related disorders | Hidradenitis suppurativa Eosinophilic pustular folliculitis (Ofuji disease) AIDS-associated eosinophilic folliculitis Pyoderma faciale (rosacea fulminans) Acne with solid facial edema Dissecting cellulitis of the scalp | |
| Disorders of cornification and related conditions | Ichthyoses, various forms (see Ch. 57 ) Darier disease Keratoderma Papillon–Lefèvre syndrome | ||
| Inflammatory disorders | Chronic hand eczema (alitretinoin, acitretin) Pityriasis rubra pilaris Lupus erythematosus Lichen planus | ||
| Chemoprophylaxis of neoplastic processes | Xeroderma pigmentosum Basal cell nevus syndrome Skin cancer in solid organ transplant patients | ||
| Treatment of neoplastic processes | Epithelial precancerous conditions Basal cell carcinoma Advanced squamous cell carcinoma Keratoacanthoma (including those induced by BRAF inhibitors) Kaposi sarcoma Sebaceous hyperplasia Muir–Torre syndrome Leukoplakia Langerhans cell histiocytosis | ||
| Miscellaneous conditions | Atrophoderma vermiculatum Ulerythema ophryogenes Confluent and reticulated papillomatosis Bazex syndrome (paraneoplastic acrokeratosis) Follicular mucinosis Sarcoidosis Granuloma annulare Lichen sclerosus (genital or extragenital) Subcorneal pustular dermatosis Graft-versus-host disease (chronic sclerodermoid) Verruca vulgaris, condyloma | ||
* Combination therapy, e.g. with a topical corticosteroid or photo(chemo)therapy, is often required.
Acne
Topical retinoids, of which tretinoin is the prototype, are mainstays in the treatment of comedonal and inflammatory acne vulgaris . The primary mode of action in acne is thought to be the normalization of differentiation and proliferation of the follicular epithelium (see Ch. 36 ), which leads to the loosening and unseating of microcomedones, thereby preventing obstruction of the pilosebaceous unit. In addition, topical retinoids may have anti-inflammatory activity. The mechanism of action of topical isotretinoin (not available in the US) is similar to that of topical tretinoin because of intraepithelial isomerization of isotretinoin to tretinoin. In contrast to oral isotretinoin, topical isotretinoin fails to suppress sebum production; it is less irritating and probably also somewhat less effective than tretinoin. The topical synthetic retinoids, adapalene and tazarotene, have comparable or (for adapalene) improved tolerability while maintaining efficacy similar to that of topical tretinoin .
Topical retinoids should be applied to the entire face or all acne-prone areas once a day as tolerated, with tretinoin applied in the evening to prevent inactivation by UV light. Application of these medications to dry skin minimizes dermal absorption, which correlates with skin irritation. Patients should be advised that beneficial effects do not become evident for 6–8 weeks or longer. An apparent exacerbation may occur during the first month of therapy, representing the externalization of deeper-seated acne lesions as the follicular epithelium is loosening. With the exception of mild, primarily comedonal acne, topical retinoids are typically used concomitantly with benzoyl peroxide products and antibiotics (oral or topical) that target Propionibacterium acnes and inflammatory processes that contribute to acne (see Ch. 36 ).
Psoriasis
Topical application of tretinoin or isotretinoin has limited efficacy in psoriasis. Although topical tazarotene was shown to be effective in treating mild to moderate plaque-type psoriasis affecting ≤20% of the body surface area, irritation limits its use as monotherapy. A combination of tazarotene and a mid-potency topical corticosteroid can improve efficacy and reduce the likelihood of both irritation and corticosteroid-induced atrophy.
Photoaging
Several controlled studies have clearly demonstrated that topical retinoids, including tretinoin and tazarotene creams, can improve fine wrinkling and lighten uneven pigmentation . It generally takes 3–6 months of daily applications to see significant clinical improvement. Cutaneous irritation is usually the limiting factor. Retinaldehyde was found to be as effective as tretinoin in treating photodamage in less extensive trials , and it had a better tolerance profile that may reflect more controlled delivery of retinoic acid to target cells.
Photoaging is the consequence of UVR-induced damage to the skin, which is characterized by decreased vitamin A content as well as lower expression of RXR-α and RAR-γ (the major retinoid receptors in keratinocytes) in the acute setting and then later by upregulation of AP1-driven matrix metalloproteinases (MMPs). Topical retinoids promote cellular differentiation and extracellular matrix synthesis, including an increase in hyaluronic acid via a CD44-mediated mechanism in addition to decreased MMP production . Histologic findings after repeated topical application of tretinoin include compaction of the stratum corneum, epidermal hyperplasia (acanthosis), correction of atypia (e.g. actinic keratoses), dispersion of melanin granules, increased dermal collagen synthesis, and angiogenesis. These findings explain the reported smoother skin, rosy glow, decrease in blotchy pigmentation, and diminished fine lines and wrinkles.
Other indications
Other FDA-approved indications for topical retinoids include alitretinoin 0.1% gel for cutaneous Kaposi sarcoma and bexarotene 1% gel for CTCL . There are also numerous “off-label” uses for topical retinoids (see Table 126.3 ).
Systemic Retinoids
Psoriasis
Several randomized, controlled, multicenter trials have been performed to ascertain the efficacy of acitretin in plaque-type and pustular psoriasis, with similar results to prior studies of etretinate . Guidelines for use of acitretin in psoriasis are summarized in Tables 8.13 and 8.14 . The best results have been obtained in acral or generalized (von Zumbusch) pustular psoriasis, in which acitretin is considered to be a first-line therapy. The various forms of pustular psoriasis, as well as erythrodermic psoriasis, tend to clear relatively rapidly with acitretin monotherapy. Rebound does not usually occur after stopping treatment, and reintroduction produces a beneficial response.
Plaque-type psoriasis responds variably to these drugs. Although complete clearance of plaques is achieved in only about 30% of treated patients, a significant improvement is obtained in an additional 50%. The mean decrease in the Psoriasis Area and Severity Index (PASI) score is approximately 60–70%, depending on the dosage and duration of treatment. Many of the plaques may remain, but they are thinner with less scale and erythema. Approximately 20% of patients may be considered treatment failures.
An initial worsening with increased erythema and/or extent of involvement of plaque-type psoriasis may occur within a few days of starting acitretin therapy at a dosage of 0.5–1 mg/kg per day (~25–70 mg/day in adults). Utilization of a lower dose (10 mg/day) initially, followed by a progressive increase, helps to avoid this complication. At the end of an 8-week treatment period in two studies, acitretin monotherapy at doses of 25–75 mg/day, but not 10 mg/day, was superior to placebo .
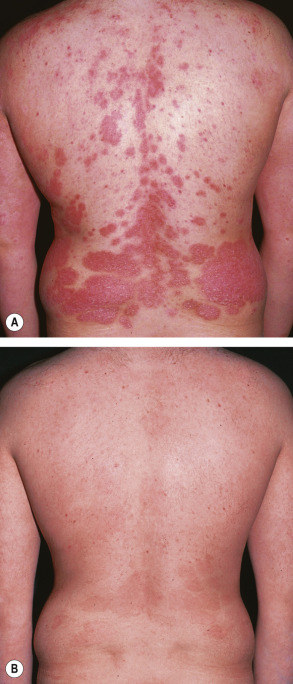
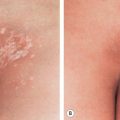
Total clearance of psoriatic plaques usually requires that oral retinoids be combined with other treatments such as topical corticosteroids, topical vitamin D derivatives, anthralin (dithranol), or photo(chemo)therapy (narrowband UVB or psoralen plus UVA [PUVA]). The “Re-PUVA” combination, in which retinoids are given for 14 days before starting PUVA, can produce an accelerated response rate and resolution of lesions that would not clear with a retinoid or PUVA alone ( Fig. 126.3 ). The cumulative UVA exposure required to produce a remission is also significantly lower with Re-PUVA, reducing the risk of UVA-induced carcinogenesis. Oral retinoids can also be combined with bath PUVA. Lastly, the combination of acitretin with UVB phototherapy has been shown to be more effective than retinoid or UVB phototherapy alone in patients with psoriasis .