, Julie Karen1 and Perry Robins1
(1)
New York University School of Medicine, New York, NY, USA
Flap Overview
Classified Based on Primary Tissue Movement or Vascular Supply
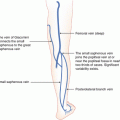
Axial Flap: axial cutaneous flaps include a named artery within the flap’s longitudinal axis, used to repair larger defects (commonly nasal defects). Examples include median and paramedian forehead flaps (supratrochlear A.), the dorsal nasal flap (angular A.), and the Abbe cross-lip flap (labial A.)
Random Pattern: geometrically designed surgical repair based on either deep or adjacent vascular pedicles without named arterial blood supply, the elevated portion of the flap is perfused by the highly anastomotic subdermal and dermal vascular network.
Interpolation: staged flap in which base of flaps pedicle is noncontiguous with surgical wound, can be axial (e.g., paramedian forehead flap, and Abbe cross-lip flap) or random pattern (e.g., melolabial). Division of the pedicle is typically done at approximately day 21 but varies with surgeon preference and type of repair.
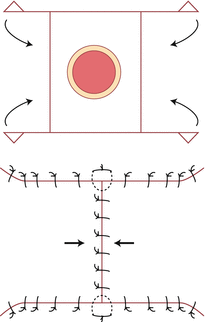
Single Advancement Flap
When/Where
To cover a defect where adequate tissue on one side is available to slide over the defect to facilitate good closure. Especially useful in areas where the parallel lines of the flap will fit into normal wrinkle lines such as those on the forehead and eyebrow. Patients with good laxity of skin (e.g., the elderly) are suitable candidates.
How
Parallel lines are cut, tissue and flap are freed from their base and slid over the defect to join with adjacent tissue. Small Burow’s triangles may be necessary to remove bulging at the base of the flap.
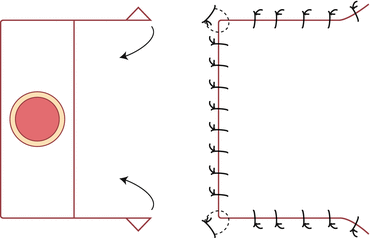

Figure 3.1
Single advancement flap
Bilateral Advancement Flap (H-Plasty)
When/Where
Where it is more judicious to slide tissue from both directions to achieve good closure. Frequently used on the scalp and the upper lip.
Z-Plasty
When/Where
Mainly used to change the direction of a scar that is deforming (e.g., a long scar line) or to elongate a scar that is constricting (redirect tension vectors). Common sites for usage are the medial canthus, side of the face, and forehead.
How
Incise a Z-plasty using 60° angles; the limbs of the Z should be of equal length. The amount of tissue available on either side will determine how long the common limb of the Z (and thus, the size of the Z-plasty) can be.
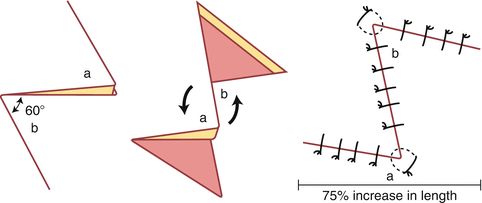

Figure 3.3
Z-plasty
M-Plasty
When/Where
When it is desirable not to extend an ellipse into a nearby structure or to avoid cutting across relaxed skin tension lines (reduce scar length). Figure 3.5 shows suggested placement sites on the face (e.g., eyebrow, outer canthus, nasolabial fold, and lips).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree