Key Points
- •
Lymphedema (surgical) treatment is nowadays tailored to the patient’s needs and even more specifically to the local needs in one affected limb.
- •
Lymphoscintigraphy and near-infrared fluoroscopy are baseline imaging techniques for lymphedema, but both have limitations, especially for surgical planning in more advanced cases.
- •
Magnetic resonance (MR) lymphography permits us to have a full mapping of the lymphedematous limb as to the local needs, differentiating edema of the different layers, fatty deposition, or fibrotic changes.
- •
The gadolinium-based contrast injection of MR lymphography gives us a mapping of the functional lymphatic channels and good differentiation with venous structures. The crossing points of functional lymphatics and veins of a similar caliber with exact coordinates are obtained and can be used for planning of lymphovenous anastomosis (LVA), minimizing the length of incisions and making LVA surgery faster and more predictable.
- •
For the planning of vascularized groin lymph node flap, a computed tomography scanner can be used in order to map the groin (number and position of the lymph nodes and relationship to vascular structures).
Introduction
Lymphedema is caused by insufficient lymphatic drainage or blockage of the lymphatic system leading to an abnormal accumulation of a protein-rich interstitial fluid within the soft tissues. Primary lymphedema results from a structural defect of the lymphatic system (congenital or clinically seen later in life). However, most cases in developed countries are secondary lymphedema with an iatrogenic cause (cancer surgery, radiotherapy, surgical trauma, etc.). The diagnosis of lymphedema can be made by taking the patient’s history and performing a physical examination and may be confirmed by imaging studies. The most widely used studies are lymphoscintigraphy, magnetic resonance (MR) lymphangiography, and indocyanine green (ICG) lymphography. Nonsurgical treatment is still the core of lymphedema management. However, advances in microsurgical techniques have opened up surgical treatment options, which are now part of the international consensus for lymphedema treatment.
Imaging Techniques in Lymphedema
Several techniques are advocated in order to map the lymphatic anatomy of an affected limb, each with its advantages and disadvantages.
It is not in the scope of this chapter to go into the details of each technique, but we will give a general overview of the information that can be extracted from each imaging technique.
Lymphoscintigraphy
Lymphoscintigraphy is still considered by many as the baseline gold standard examination for the diagnosis of lymphedema. It gives general information about the lymphatic system, both functional and structural, and can confirm lymphedema with certainty. Determination of the velocity of the tracer uptake and quantification of tracer uptake are done at the end of the examination, giving a general functioning rate of the system and showing potential asymmetries. Routes of lymphatic drainage can be seen with shunting from the superficial to the deep system (recruitment of deep nodes), aberrant lymphatic pathways, dermal backflow, and so forth.
Standardization of the protocol seems to be a problem especially when comparing images and following up on the evolution of the pathology. The omm protocol is described by Bourgeois in three phases.
Advantages:
- •
Confirmation of lymphedema
- •
Lymphatic velocity quantification
- •
Tracer-uptake quantification
Disadvantages:
- •
Long examination (3 hours!)
- •
Poor anatomic and spatial resolution (planar images)
- •
No information about tissue status (fibrosis/fat)
- •
Difficult correlation between images and surgical decision-making
Near-Infrared Lymph Fluorescence Imaging
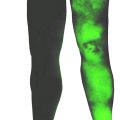
Lymphatic fluorescence imaging using indocyanine green (ICG) was a breakthrough in the imaging of the superficial lymphatic system. It provided a new way of visualizing the lymphatic channels under the skin and made preoperative localization and visualization of functional lymphatic channels in real time possible. Staging systems have been described for the upper and lower limbs, giving us indications for potential surgical treatment. A similar severity staging has been described for the genitalia. However, this examination is time-consuming and operator dependent, and if performed by an inexperienced operator, much useful information could be lost. Moreover, it maps only lymphatic vessels with a maximal depth of 10–12 mm under the skin surface even in good circumstances. Although relatively rare, adverse effects to ICG injections exist (ranging from mild reactions to anaphylactic shock).
Advantages:
- •
Fast
- •
More spatial resolution (360 degrees around the limb)
- •
Gives indication for potential lymphovenous anastomosis (LVA)
- •
Allows staging of severity
Disadvantages:
- •
Operator dependent
- •
Maximum depth 10–12 mm
- •
No information about tissues (fibrosis/fat) or veins
- •
Adverse effects
The use of magnetic resonance imaging (MRI) and computed tomography (CT) will be discussed extensively in the next paragraphs.
General Assessment of the Limb Using MR Lymphography
Imaging Protocol
The protocol described in this section is our protocol for the upper limbs, but exactly the same principles are applied for the lower limbs.
We performed our MRI studies using gadobenate dimeglumine 529 mg/mL (MuliHance, Braccor, Germany). This contrast agent has a high transient protein binding capacity as compared to other gadolinium-based contrast agents. Local anesthesia is added to the solution (0.2 mL Linisol 1%–lidocaine hydrochloride) as contrast agents in extravascular spaces cause a burning sensation.
The injection is given in the webspaces, with 0.5 mL of the solution injected per webspace. Incidences of allergic reaction to gadobenate dimeglumine are very rare, unlike other contrast agents.
Patients are placed in a supine position in the MR scanner. To avoid artifacts in imaging of the arm, the patients are placed eccentric in the bore so that the arm is as much in the homogeneous magnetic field as possible. The thumb is placed in a pro-supination position (pointing ventrally). To avoid trembling or movements during the scanning, the arm is slightly supported at the level of the distal arm and wrist.
The examination starts with a dynamic three-dimensional (3D) T1 series of the region of the wrist to the elbow (one station—5 minutes). This series is performed 15 minutes after the start of the injection of contrast. Next, T2-weighted imaging of the same region and the upper arm is requiring two scan ranges. The images of the two scan ranges are stitched together resulting in an excellent overview of the whole arm (15 minutes). Then, the 3D T1 series is repeated. Our MR examination was performed on a 3 T system (Skyra, Siemens Medical Systems, Erlangen, Germany). Image analysis of the 3D T1 series was performed with Philips Intelligence (Philips, Best, the Netherlands). Displayed images are the maximum intensity projections (MIPs) in the axial, coronal, and sagittal planes between 3 and 10 mm thickness (MIP-thin) that are recognizable for surgeons.
Using this protocol, a single contrast injection is ideal, showing all necessary structures without the need for a venous contrast agent (e.g., ferumoxytol), as advocated by some authors.
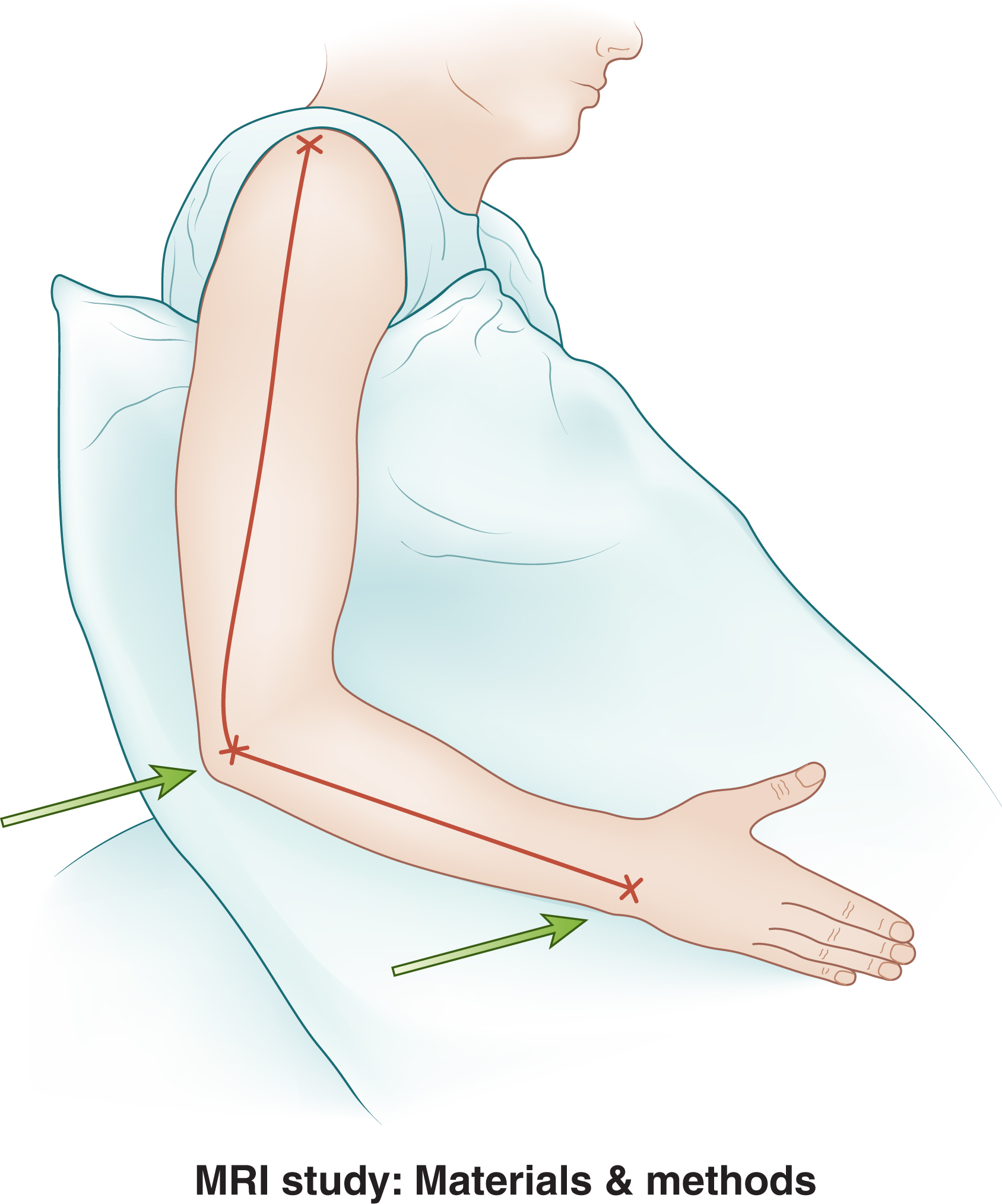
Coordinate System in MR Lymphography
In a similar manner to how perforator mapping is performed in a standardized way in order to be reproducible, we describe a coordinate system for MR lymphography in the limbs. As reference points, we use the lateral humeral epicondyle for the elbow and, for the wrist, the mid-dorsal part of the radio-carpal joint measured when metacarpal 3 is in the longest axis of the arm. For the shoulder, the acromio-clavicular joint is used as a reference point. Functional lymphatic channels will be seen draining contrast in a linear pattern. Those are mapped with precise localization and are described in a coordinate system compared to predefined standardized anatomical landmarks.
The depth of the functional lymphatics is described, as is description of small veins in the neighborhood of described lymphatics.
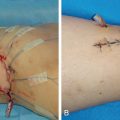
In this way, for every limb, the mapping consists of exact locations where lymphatics cross with the veins. Obviously, the lymphatic channel can be used on different levels in order to perform the LVA, but with this particular mapping method, surgery is more predictable, swifter, and without any sham incisions (as was sometimes the case in the early experience).
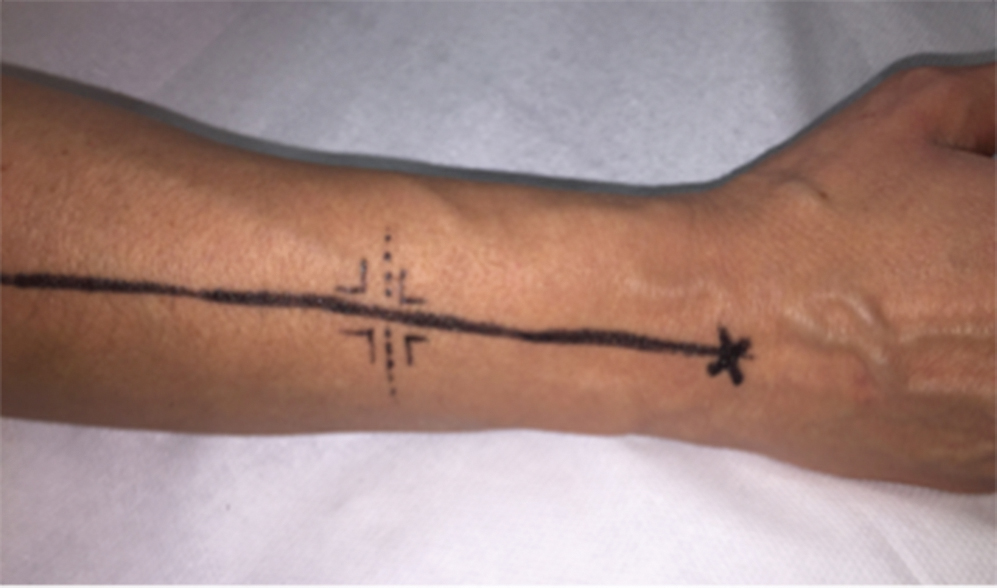
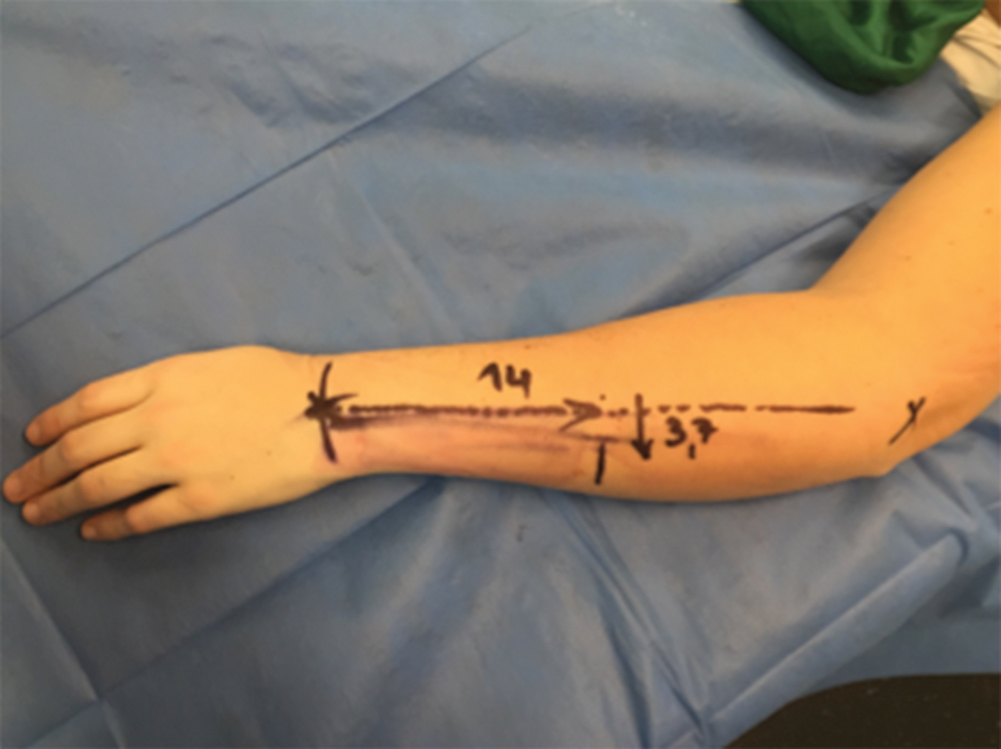
For the coordinate system, lines are drawn between the anatomic landmarks, and all further coordinates are given relative to those points and lines ( Fig. 8.1 ). Distances on the axes are given by the radiologist (×cm proximal/distal to the landmark), followed by another measure (×cm) in a right angle departing from the axis. At the end point (the crossing of a functional lymphatic and a vein), a depth of the lymphatic is given (× mm) ( Figs. 8.2 and 8.3 ).