Key Points
- •
Precise knowledge about normal lymphatic anatomy in the upper and lower extremities can empower practitioners to distinguish structural changes occurring in lymphedema.
- •
Lymphatic anatomy in lymphedema changes substantially with the deterioration of superficial lymph collecting vessels.
- •
Lymphedema can be caused by restriction of outflow from the original pathway through the axilla or inguinal region and is not always associated with changes in lymphatic drainage pathways to other regions.
Introduction
A better understanding of the anatomy of the lymphatics equips practitioners with the fundamental information required to accurately diagnose lymphedema and select the appropriate surgical option for each patient. Therefore, surgeons working with the lymphatic system need to understand normal lymphatic anatomy, as well as the changes that occur in lymphedema.
The lymphatic system is distinctly different from the vascular system, and our conventional knowledge about the vascular system does not help to understand it. For example, the lymphatic system does not have a pumping organ like a heart. Rather, lymph fluid is propelled extrinsically by muscle movement and intrinsically by peristaltic contraction of the lymph collecting vessels. Blood is circulated through the arterial and venous systems and perfused throughout the body, whereas lymph fluid is produced in the peripheral tissues and transferred via the lymphatic system to return to the blood circulatory system.
Starling’s Law is the basic principle governing the regulation of fluid exchange in the body. The traditional Starling’s Law was recently modified due to new understanding of the function of the endothelial glyocalyx layer. The revised Starling Equation Law suggests that filtered fluid returns to the circulatory system primarily via the lymphatics because there is no reabsorption possible through the blood capillaries and venules. Hence, the main cause of tissue edema is considered to be a result of lymphatic dysfunction.
Normal anatomy of the lymphatics has been investigated over three centuries since the development of the Mercury method in the 17th century. Its use in anatomical preparations and its perception as an anatomical material evolved with the understanding of the circulatory and lymphatic systems. However, mercury was later abandoned for use in anatomical studies due to its toxicity. The author (HS) developed the microinjection technique to demonstrate the lymphatics in cadaveric specimens. This method uses hydrogen peroxide to inflate the lymphatic vessels to identify them, after which a fine needle is cannulated into the vessels and a dye or radiocontrast medium is injected to allow their visualization. In recent times, indocyanine green (ICG) fluorescent lymphography has been used to demonstrate the lymphatics not only in patients with lymphedema but also in cadavers. This new imaging method provides increased imaging data and promotes further understanding about the anatomical changes that occur in lymphedema. Based on the authors’ anatomical findings, ICG lymphography data, and archival diagrams from historical materials, we proposed a new anatomical concept called the “lymphosome,” which demarcates the skin into separate lymphatic territories. Each lymphatic territory is defined by the notion that several superficial lymphatic vessels form a group that connects to first-tier (sentinel) lymph nodes ( Fig. 2.1 ).
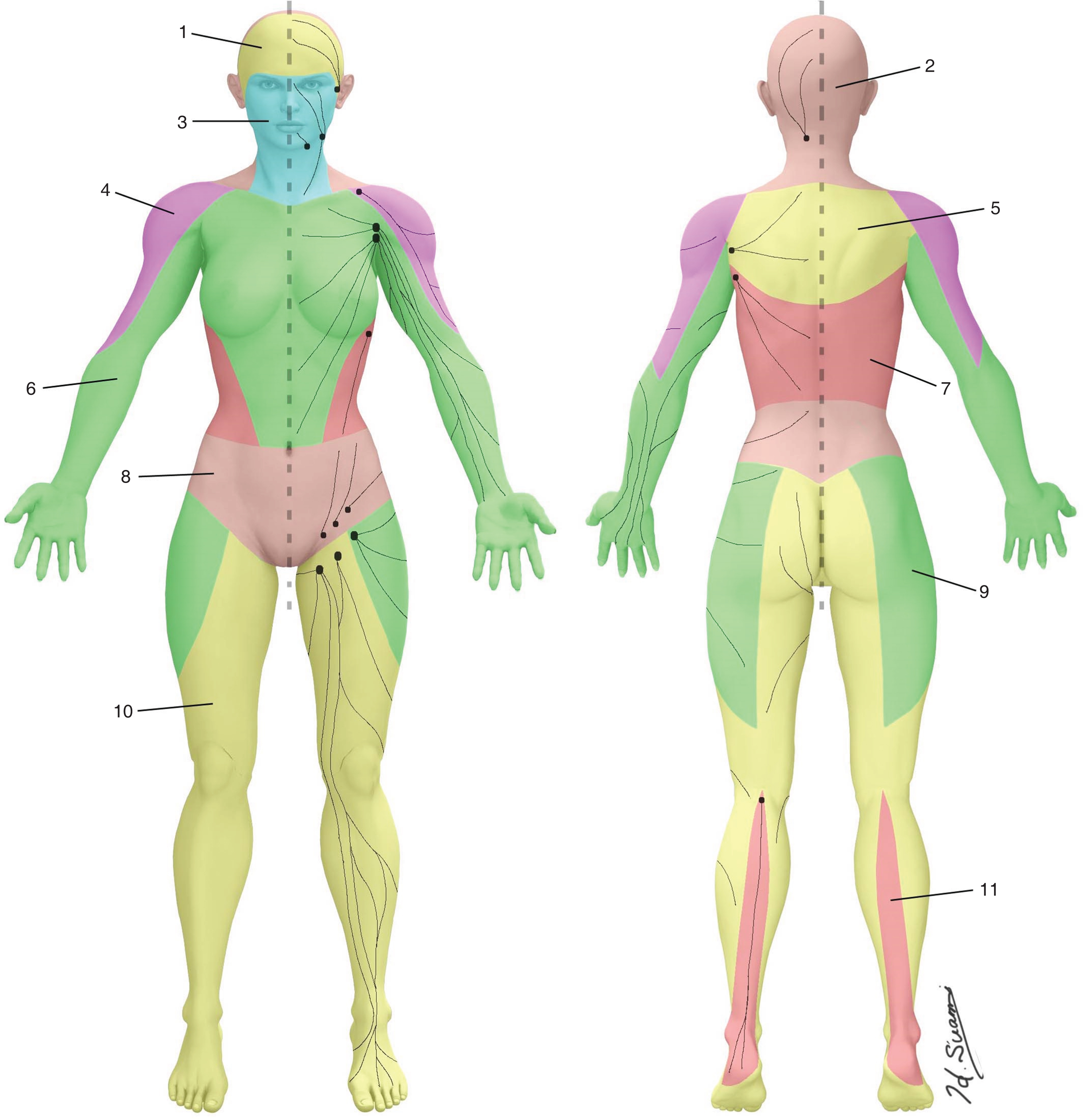
An understanding of normal lymphatic anatomy is vitally important for practitioners because it provides the baseline imaging data required to distinguish the altered anatomical structures that occur in lymphedema. However, normal anatomy itself is not enough to interpret imaging data in lymphedema because other factors such as lymphangiogenesis, dermal reflux (dermal backflow), and other structural changes are always associated with lymphedema. The lymphatic anatomy changes after lymph node dissection, and the body attempts to maintain lymph drainage in several different ways. The anatomical changes do not occur only at the surgical site but may also occur in any areas downstream of the lymphatic vessels that connect to the removed nodes. In this chapter, we describe normal lymphatic anatomy in the limbs and introduce the anatomical changes that occur in lymphedema.
Normal Lymphatic Anatomy in the Upper Extremities
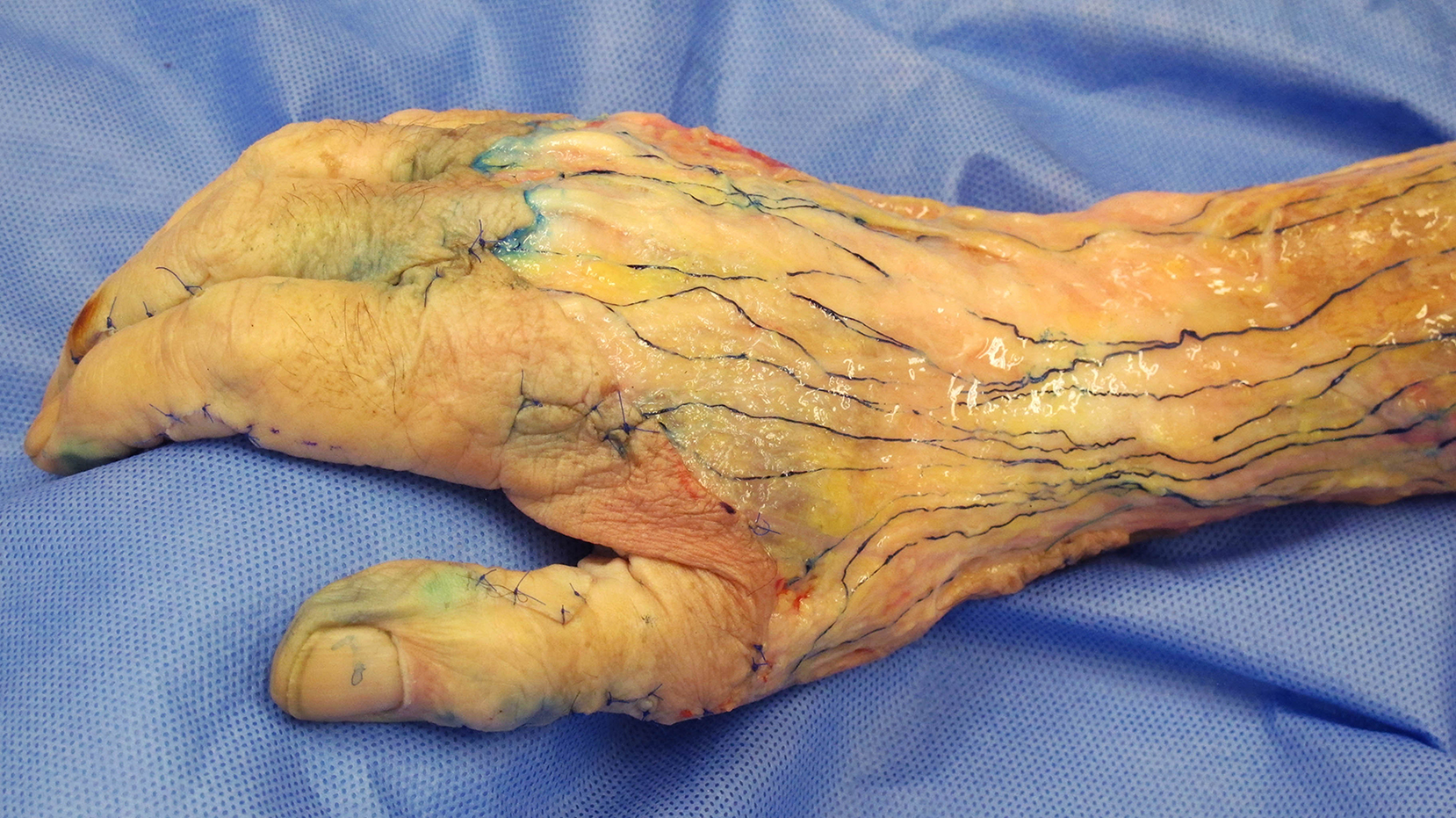
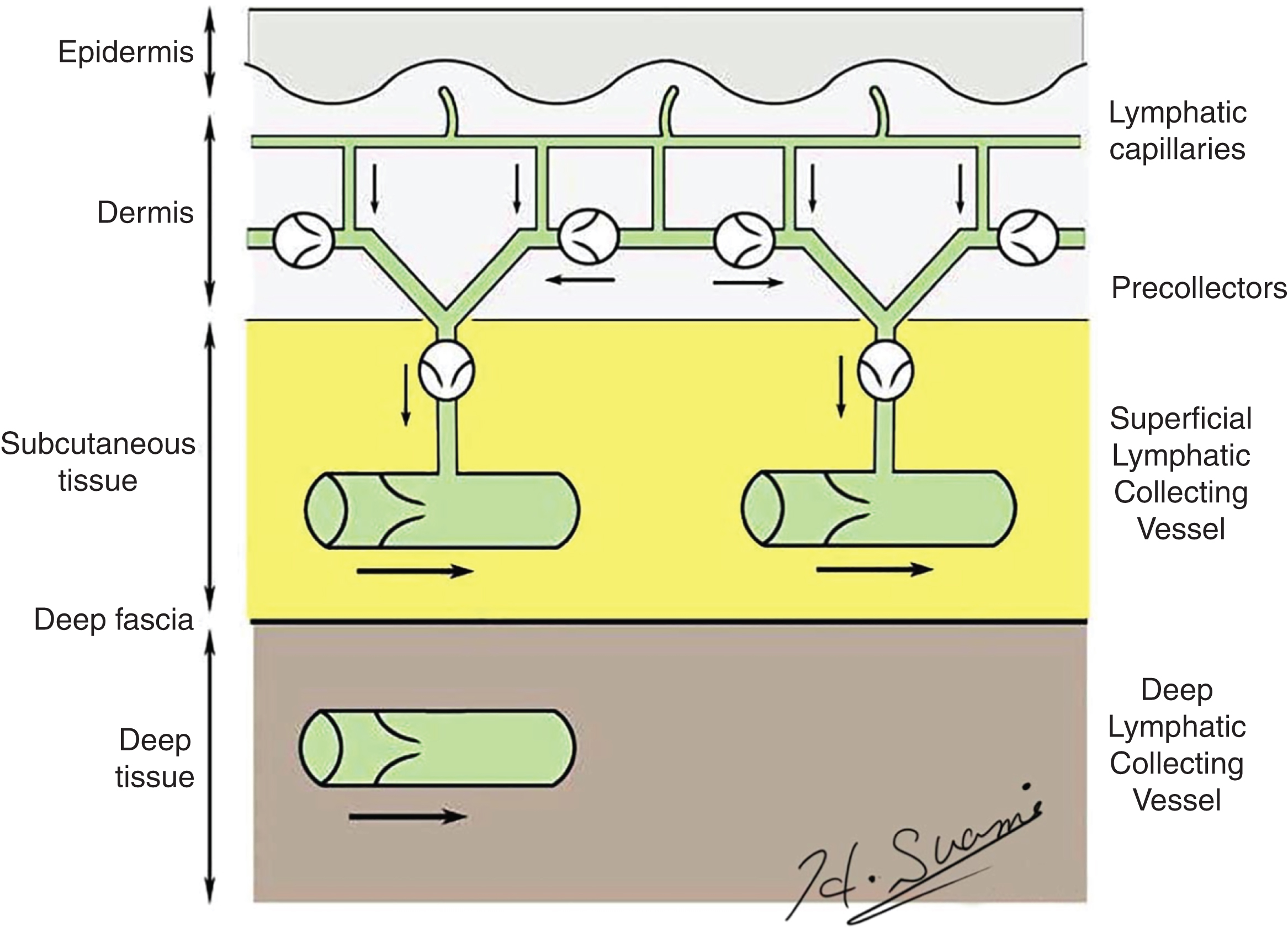
The lymphatics in the upper extremity originate in the fingers and palm ( Fig. 2.2 ). The lymphatic capillaries and precollectors within the skin merge to form the lymph collecting vessels in the subcutaneous tissue ( Fig. 2.3 ). As Kubik explained, each collecting vessel has an independent narrow strip of skin territory. Thus, the lymphatic imaging tracer must be injected at multiple circumferential sites if a comprehensive view of the lymphatics is to be captured. If only one or two sites are selected for tracer injection, the operator may miss identifying affected lymphatic vessels originating from other aspects. It was previously said that the lymphatics differ substantially between individuals, but there is no anatomical evidence to support this statement and it is not accurate. There are some anatomical variations between people, but normal lymphatic anatomy is uniform with regard to the relationship between the collecting vessels and their corresponding lymph nodes.
The lymphatics in the upper extremity primarily drain to one of two pathways: to the axilla or to the clavicular nodes. The lymphatic system is separated into superficial and deep lymphatics by the deep fascia. The superficial lymphatics connect to one or two dominant lymph nodes in the axilla (arm sentinel node/s). The deep lymphatics run along the major arteries and connect to the axillary nodes. The lymph collecting vessels connecting to the clavicular nodes were separately described by Mascagni and Sappey. More recently, Kubik named this pathway “the lateral bundle.” He described the potential importance of the lateral bundle in the prevention of lymphedema because this pathway is independent from the axillary pathway and can be preserved after axillary node dissection. The cadaver dissection study of Leduc et al. found that the lateral bundle existed in the upper extremity in 36% of subjects.
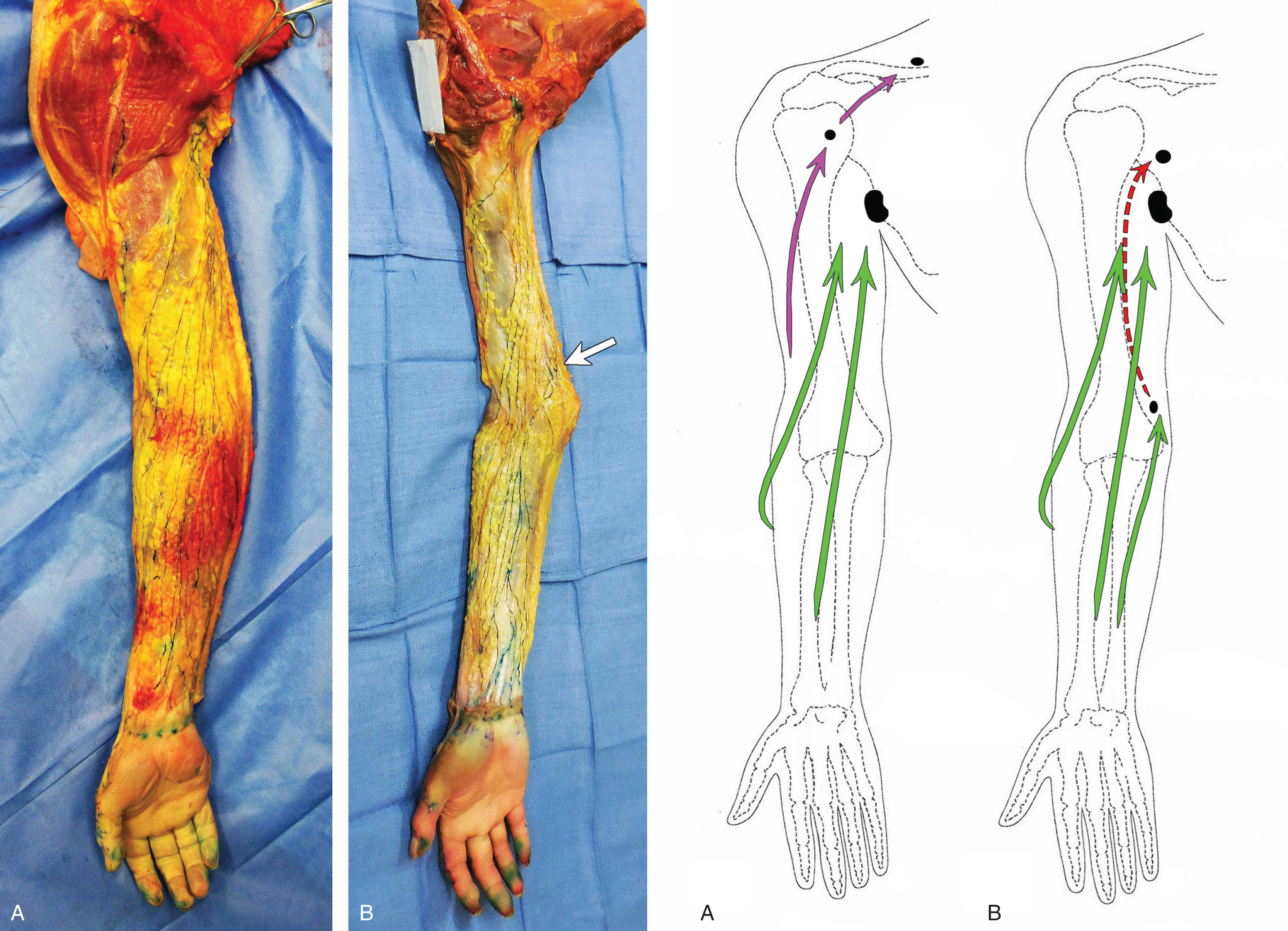
Dissection photos and schematic diagrams of lymphatic drainage pathways in the upper extremity are shown in Fig. 2.4 . The superficial and deep systems are independent of each other in most areas, but one anatomical variation has a natural connection between them at the medial elbow. The basilic vein runs along the medial front forearm, penetrating the deep fascia at the medial elbow on its way to connecting to the brachial vein in the upper arm. A few superficial collecting vessels sometimes run along the basilic vein and become deep lymph collecting vessels in the upper arm ( Fig. 2.4B ). These vessels commonly pass through the epitrochlear lymph nodes—small interval lymph nodes in the cubital fossa. If the epitrochlear nodes are identified with lymphatic imaging, the operator should consider that the efferent vessels from the nodes have transformed into deep lymphatic vessels. This anatomical variation may serve as a bypass pathway when a sentinel node biopsy or level 1 node dissection is performed for breast or skin cancer treatment. The deep lymphatic vessels run along the axillary vein, and oncologic surgeons commonly do not skeletonize the axillary vein to avoid disturbing them. Their corresponding lymph nodes are located more centrally in the axilla, away from the arm sentinel node/s.
Anatomical Changes of the Lymphatics in the Arm in Lymphedema
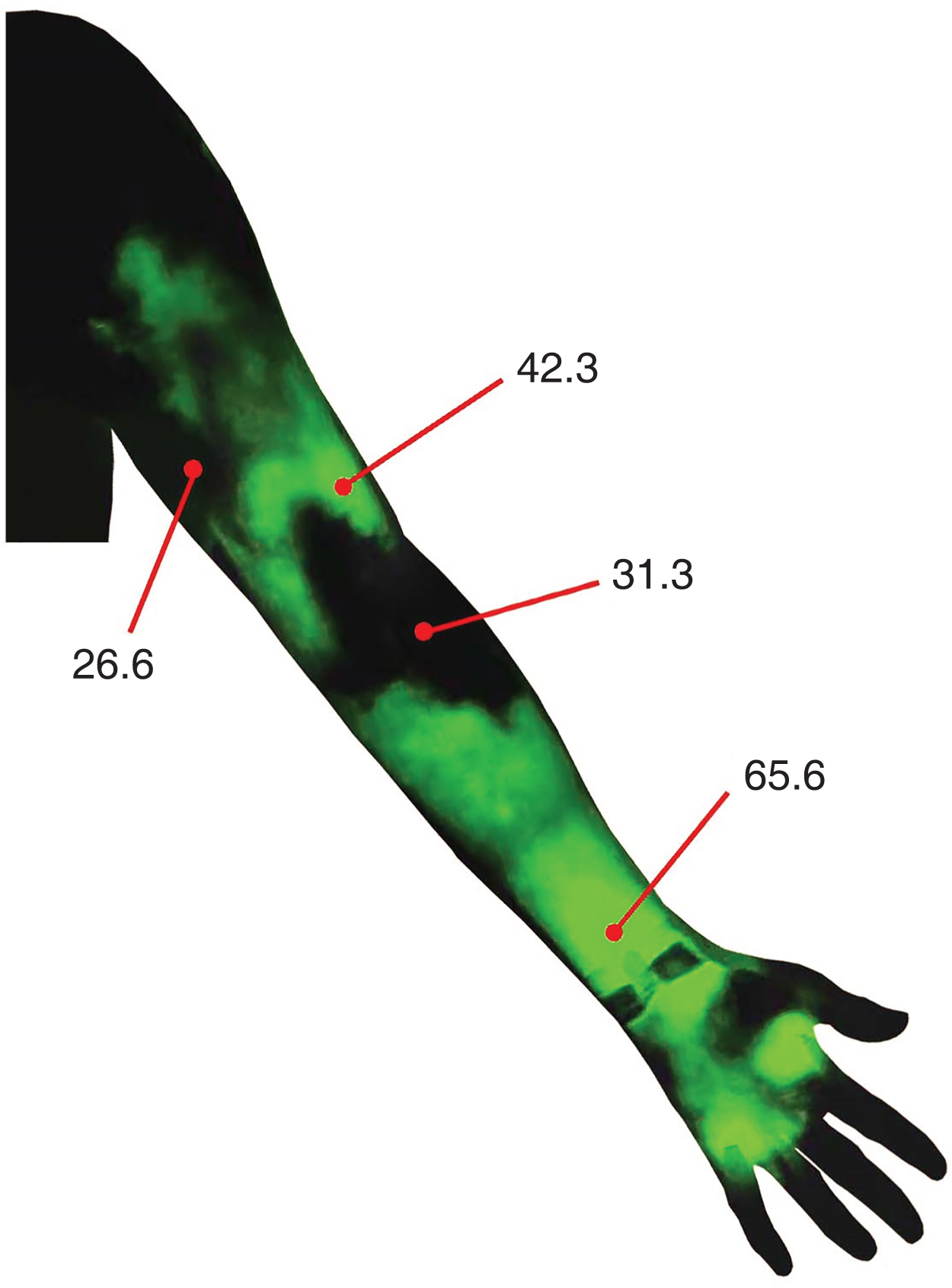
The presence of dermal backflow is a key imaging indicator to diagnose lymphedema. Dermal backflow is caused by restriction of upstream flow in the lymph collecting vessels. It is characterized as reflux of lymph fluid from the lymph collecting vessels into the skin and dilatation of the lymphatic capillaries and pre-collectors within the skin. Skin water content in the dermal backflow area is higher than in unaffected skin, so this anatomical change can be noninvasively determined by measuring skin water content ( Fig. 2.5 ). Although lymphedema patients report the discomfort and fullness in the dermal backflow areas as adverse symptoms, dermal backflow plays an important role by creating alternative functional routes to transfer lymph fluid when the superficial lymphatic vessels become restricted. Dermal backflow forms a bridge between obstructed and patent lymphatic vessels in mild to moderate lymphedema (e.g., International Society of Lymphology [ISL] stage I or II) and serves as a substitute route for transporting lymph fluid when the majority of the lymph collecting vessels have deteriorated (e.g., ISL stage III) ( Fig. 2.6 ).