Introduction
Burns of the shoulder and axillary region present a challenging task with respect to prevention and treatment. A proactive and multidisciplinary approach to burns of the axilla and shoulder can often prevent or minimize morbidity in this region. Such an approach requires early involvement from occupational and physical therapists to ensure proper positioning, splinting, and physiotherapy; early excision and grafting of deep partial- and full-thickness burn injuries to ensure rapid wound closure; and appropriate postoperative scar management including active and passive ranging exercises, splinting, and use of compression garments. Despite our best efforts, however, axillary adduction contractures will occur. In fact, a study published in 1978 retrospectively evaluated the incidence of burn scar contractures at major joints in 625 treated at Shriners Burn Hospital and the University of Texas medical branch hospitals in Galveston, Texas, between 1964 and 1975. Overall, the axilla had the highest incidence of contracture (57%); however, among those who had not received splinting or pressure dressings throughout their recovery, the rate was markedly higher (98%).
In a modern burn center with high-level care, the shoulder joint is still reported to be the most frequently contracted large joint postburn injury. Contractures at this joint are related to scarring within, and/or around, the axilla and have a reported incidence of 23% in the adult burn population. The incidence of this sequela is even higher in the pediatric burn population (28%) and can be more debilitating, as severity increases with the growth of the child. Limited range of motion (ROM) in the shoulder and arm as a result of these contractures can significantly impair quality of life by restricting the ability to perform daily activities and participate in rehabilitation.
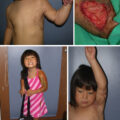
Once a burn scar contracture has developed, early surgical reconstruction leads to a faster return to normal ROM and function and prevents further involvement of the underlying structures such as bones, tendons, ligaments, and the neurovasculature. The posture, or position of comfort, for patients with axillary contractures is that of adduction of the shoulder with elbow and wrist flexion, which tends to worsen over time and complicate rehabilitation ( Fig. 63.1 ). Reconstruction of contractures involving additional joints and deeper structures is more complicated. In any case, however, reconstruction aims to correct the underlying scarring in a way that will allow for as much movement as possible while preventing contractures from recurring.
Position of comfort.
(From TBC Herndon)
General considerations
Early excision and grafting, and early mobilization, can help to reduce or minimize the formation of axillary contractures. Nevertheless, when an axillary contracture develops, it should be treated before it involves deeper structures and before the formation of secondary deformities. Initially, splinting and physiotherapy are performed. When nonsurgical interventions fail to make gains in ROM, surgical reconstruction is considered. It is not necessary to wait until the scar has matured; however, axillary contracture release is not typically performed during the acute phase of the burn and if initial wound closure has not been achieved.
Applied anatomy
The axilla is a pyramidal-shaped region located between the upper part of the arm and the side of the chest. It is a crucial anatomic area as it contains numerous important structures, including blood vessels, nerves, lymph nodes, and muscles. The axilla is defined by the anterior and posterior axillary folds ( Fig. 63.2 ). The anterior fold is composed of the pectoralis major, pectoralis major, and subclavius tendons and muscles. The posterior fold is composed of the teres major, subscapularis, and latissimus dorsi muscles and tendons. The medial extent of the axilla, between these folds, is the serratus anterior and the first four ribs; the lateral extent comprises the humerus, coracobrachialis muscle, and the short head of the biceps muscle. The superior aspect of the axilla is a hair-bearing dome shape, and the apex of this dome is referred to as the cupola. Beneath the skin, subcutaneous tissue, and axillary fascia of the dome lie major neurovascular structures. The first structure is the axillary vein, which is typically formed as the merger of the basilic and brachial veins at the inferior border of the teres major muscle. The axillary vein continues under the first rib, where it becomes the subclavian vein. The axillary artery, the primary blood supply to the axilla, lies superior and lateral to the vein and originates as it passes over the superior surface of the lateral border of the first rib. The axillary artery is typically divided into three anatomic segments (proximal, retropectoral, and distal) based on their relationship to the pectoralis minor muscle. The artery gives rise to several notable branches frequently useful in reconstruction: (1) the superior thoracic artery, which supplies blood to the upper part of the pectoral region and the first two intercostal spaces; (2) the thoracoacromial artery, which supplies blood to the pectoral muscles, the deltoid muscle, and the acromion; (3) the lateral thoracic artery, which supplies blood to the lateral and anterior chest wall, including the serratus anterior muscle; (4) the subscapular artery, which supplies the subscapularis muscle and other structures in the posterior axillary region; and (5) the anterior and posterior circumflex humeral arteries, which supply blood to the shoulder joint.
Axillary anatomy (Achauer’s burn reconstruction).
The majority of cutaneous sensation to the axilla is supplied by the intercostobrachial nerve, which emerges from the upper intercostal spaces and travels inferolaterally across the axilla. Relevant nerves include the medial brachial, medial antebrachial, and ulnar nerves, which may be encountered between the distal portions of the axillary vein and artery. Additionally, the lateral thoracic and thoracodorsal nerves can be found superficial to the serratus anterior muscle and course through the axilla.
Classification of axillary contractures
In general, contractures can be classified as broad and diffuse or as well-defined and linear. Their extent can be limited to skin/scar only or be complex with tethering of the underlining tissue such as fascia and muscle. For long-standing axillary contractures, it may be necessary to obtain multiple view radiographs of the shoulder to assess for subluxation, dislocation, or the presence of heterotopic ossification. Various classification systems have been described for postburn axillary contractures. Hanumadass et al. described four types of contractures based on anatomic considerations ( Table 63.1 ). Here, local tissue rearrangements are most applicable when adjacent scarring is minimal (types I and III), whereas incisional release and grafting or flaps are required when adjacent scarring is diffuse (types II and IV). Perhaps the most common classification is that described by Kurtzman and Stern 10 ( Table 63.2 ). This simple classification is also based on the anatomic location of the contracture; however it does not take into consideration the quality of the adjacent or surrounding skin. Finally, Ogawa et al. published a 25-year retrospective review of 124 axillary scar contractures treated in their department whereby contractures were classified into five types, each type with a suggested method for surgical correction ( Table 63.3 ). They also identified four key scar features to be considered when selecting an operative method: size, depth, location, and shape.
Table 63.1
Classification of Axillary Contracture
| HAIR BEARING | ANTERIOR OR POSTERIOR | ||
|---|---|---|---|
| Type | Area Involved | Axillary Fold | Adjacent Scarring |
|
|
|
|
Table 63.2
Kurtzman and Stern Classification of Postburn Axillary Contractures
| Classification | Location |
|---|---|
|
|
Table 63.3
Ogawa et al. Classification of Postburn Axillary Contractures
| Anatomic Location | Considerations For Surgical Correction | |
|---|---|---|
| Type I |
|
Skin graft |
| Type IIa | Anterior axillary line |
|
| Type IIb | Posterior axillary line | |
| Type IIIa |
|
Propeller flap |
| Type IIIb |
|
Flap design with donor site outside the axilla |
| Type IVa | Axilla, chest, upper arm |
|
| Type IVb | Axilla, back, upper arm | |
| Type IVc | Axilla, back, chest | |
| Type V |
|
|
The importance of this classification is to advocate for a universal approach to the correction of such contractures; however, each patient and contracture is unique. As is typical for postburn reconstruction, the surgical plan should be tailored to best meet the needs and expectations of a particular patient, and there is often more than one technique leading to a successful outcome. In general, options for surgical correction of axillary contractures include free skin grafts (with or without underlying skin substitute/dermal matrix), local flaps, regional flaps, free flaps, and scarring flaps.
Principles of management
Positioning and splinting
During the acute phase of the burn, appropriate positioning and splinting may help to prevent or minimize contracture formation. The shoulder joint is kept at 90 to 100 degrees of abduction, 15 to 20 degrees of flexion, and with some amount of external rotation. A bedside table or pillows are used with a conforming splint, foam wedge, or cushioned troughs. Extreme care should be taken to ensure the absence of pressure on bony prominences, such as the medial epicondyle and olecranon. This position is usually maintained during the day while in bed and at night and protects the brachial plexus from traction injury while maintaining the stability of the glenohumeral joint. Performing active and passive ROM during this phase is also critical. After skin grafting of the axilla during the acute or reconstructive phase, an open axillary type (airplane) splint or a figure-of-eight wrapping around the axilla with a foam wedge to keep greater than 90 degrees of shoulder abduction is frequently used.
Release and resurfacing
Surgical reconstruction of the axilla postburn injury should follow the general principle of replacing like with like. Therefore whenever possible, contracture release with nonburned full-thickness skin and subcutaneous tissue is preferable and typically results in the best outcome. In the absence of uninvolved skin or adjacent skin laxity, the use of free skin grafts is a viable option that has been well described in the literature. Advantages of free skin grafts include the ability to introduce a large amount of unburned, thin skin in a relatively simple procedure ( Fig. 63.3 ). The main disadvantage is that of recontracture, often requiring additional release, postoperative splinting, and immobility until graft adherence has been established, as well as the need for extensive physical therapy to further maximize ROM. The use of dermal matrices, such as AlloDerm, Integra, or BTM have been described to potentially reduce recontracture but require two stages with approximately 3 weeks in between to allow for integration and vascularization of the matrix , ( Fig. 63.4 ). Negative pressure wound therapy is frequently used to help bolster the matrix and may improve neovascularization; however, it still may be wise to splint the axilla during this period to maintain shoulder extension.
Complete axillary release with a split-thickness skin graft, postrelease days 5 (above) and 21 (below).
Staged release with BTM.
To release tension resulting from a contracture band, incisions should be oriented in a perpendicular fashion to the scar and should, optimally, extend onto unburned skin. Frequently, a fishtail extension is used at either end of the release. During the release, the shoulder should be mobilized and ranged under direct visualization to identify new points of tension and to ensure a complete release. As a postburn contracture represents a tissue deficit, we tend to avoid excision of scar whenever possible. Furthermore, over time the release of tension typically results in the normalization of surrounding hypertrophic scarring.
Local flaps
Adjacent tissue rearrangements
As there is frequently unburned skin within the axilla, adjacent tissue rearrangements are often used to lengthen a scar contracture band along the anterior or posterior fold. This technique is advantageous in that it uses full-thickness tissue resulting in less contracture, may stretch more over time, and does not require a prolonged period of immobilization. Potential disadvantages include a tendency for flap necrosis, depending on the vascularity of the flaps. A number of techniques have been described including Z-, V-W, or V-Y plasties. Multiple Z-plasties in series ( Fig. 63.5 ), four-flap Z-plasties, and double opposing (jumping man) Z-plasties may all be useful in the appropriate patient. Typically, a Z-plasty is best for a discrete, thin scar band with skin laxity on either side of the contracture. For a more broad-based contracture, or if there is skin laxity on only one side of the contracture band, a STARplasty or square flap may be more appropriate , ( Figs. 63.6 and 63.7 ). The choice of local tissue rearrangement should take into account the location of burned and unburned tissue, the size and width of the contracture band, and the location and amount of skin laxity.
Multiple Z-plasties for release and thin, linear, contracture band.
STARplasty. Note incorporation of perforating blood vessels to maximize perfusion.
Square flap.
Central axis flaps
The term propeller was introduced in 1991 by Hyakusoku et al. for reconstruction of contracture in cubital and axillary regions. Even extensively burned patients may have healthy skin in the axillary or cubital fossa because of joint flexion at the time of injury that may be used to break the scar contracture. The attraction of this technique lies in using the spared axillary fossa skin and rotating it 90 degrees to straddle the anterior and posterior axillary folds. The flap is based on a subcutaneous pedicle, is extremely simple to raise, and requires no microsurgical skills. If the donor area cannot be primarily closed, it may be covered with skin grafts and will provide excellent functional recovery within 6 months without splinting. The subcutaneous pedicle is very reliable, and minimal complications have been reported with this technique. Many innovative designs have been used (multilobed propeller flap, pinwheel flap, scarred propeller flap, zigzag modified propeller flap, multiple rhomboid flap) to enhance the aesthetic results or to minimize the need for skin grafting of the released raw areas.
Central axis flaps offer an option to use any amount of unburnt skin centrally or in the vicinity. Many broad-based or multiple linear contractures can be managed effectively with the use of these flaps, with better aesthetics and stable skin. The central axis flaps do not dislocate the hair-bearing skin of the axilla; however, many of these flaps are applicable only in mild to moderate contractures. These flaps are known to stretch over time, improving the functional outcome. There are no defined criteria for dimensions of these flaps that can be safely raised, but very long flaps have been elevated and rotated by 90 degrees without significant complications ( Figs. 63.8 and 63.9 ).
(A) A 32-year-old female with a postburn, type II, left axillary contracture with sparing of axillary dome and severe scarring of surrounding skin. (B) A quadrilobed flap is raised in the axillary fossa using a subcutaneous pedicle. (C) The flap is rotated 90 degrees to straddle the anterior and posterior axillary contracting bands, and the donor area is split skin grafted. (D) Excellent functional and aesthetic result at 30 months follow-up. The axillary hairs are well preserved, and the flap skin is fully stretched.
(From Karki D, Mehta N, Narayan RP. Post axillary burn contracture: a therapeutic challenge! Indian J Plast Surg. 2014;47:375–380.)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree