Abstract
Bony defects of the frontocranial skeleton are commonly the result of traumatic, ballistic, neoplastic etiologies. The three-dimensional structure of this region can sometimes make satisfactory reconstruction a complicated task. A number of alloplastic implant materials have been, and still are, used in the search for a simple and reliable solution to this problem. While surgeons may experience short-term successes with titanium mesh or polyetheretherketone (PEEK), long-term results with regard to implant exposure and infection may vary. In the authors’ experience there is no adequate substitute for the use of autogenous bone graft – split calvarium, split rib, or iliac crest – in reconstructing full-thickness cranial defects. With adequate training there are minimal donor site complications, and there is rarely, if ever, long-term failure of the grafts.
Keywords
frontocranial reconstruction, full-thickness cranial defects, autogenous cranial reconstruction
Background
Paul Manson, Bill Crawley, and Jack Hoopes in 1986 published a paper entitled “Frontal cranioplasty: risk factors and choice of cranial vault reconstructive material.” In that paper they examined their series of 42 cranioplasties, 25 of which were treated with methylmethacrylate (MMA), and 17 with autogenous bone. Both groups had about 60% preexisting infections.
In the MMA group, there were no infections, and in the autogenous bone group there were four infections (23%). One would draw the conclusion from their data that an acrylic cranioplasty would be the treatment of choice.
I [S.A.W] was asked to write the commentary for their paper, and I said that my experience with 73 autogenous cranioplasties differed from theirs: there were no infections. I had no experience with MMA to compare, since I did not use alloplastic materials, but still felt that autogenous bone grafts were the material of choice.
As of 2017, our series of autogenous cranioplasties had grown to 176, including 72 preexisting defects, and 104 “primary cranioplasties” wherein a large parietal bone flap was removed, split through the diploic space, and half replaced as a cranioplasty, and the other to serve as a large autogenous bone graft. In 23 cases, split rib was used, in 6 cases iliac bone, and the remainder were split calvarial. In this entire series, there have been no infections, and no complications associated with the harvesting of the bone grafts.
Since our series extends over a time period of 42 years (1975–2017), I think we can confidently support the assertion made in 1986 that autogenous bone grafts are indeed the material of choice, the “gold standard.”
Hydroxyapatite/Methylmethacrylate
Methylmethacrylate is an alloplastic substance that has long been used to reconstruct small to moderate cranial defects. It is mixed prior to use to form a moldable putty, and has a substantial exothermic reaction while hardening which must be taken into account when applying the material to tissue in situ . It has substantial tensile strength and compression resistance, is cheap, and relatively easy to use. However, as a foreign substance, it provides a nidus for infection, and even those surgeons with extensive experience using MMA for cranioplasty procedures recommend against its use in proximity to the frontal sinus due to unacceptably high risk for infection.
Hydroxyapatite is an inorganic phosphate-based compound that forms a hard cement after it is cured, similar in that with regard to MMA. This material, too, has limitations with regard to the size of the defect it is reliably able to reconstruct. It demonstrates superior osseointegration relative to MMA, a minimal inflammatory response, as well as some degree of osseoconduction that would theoretically mitigate some of the infection risk associated with alloplastic materials. A distinct advantage is that there is no associated exothermic reaction, and associated risk of thermal damage to surrounding tissue. However, as with MMA, there is compelling evidence that hydroxyapatite should never be used in close proximity to the frontal sinus due to significantly increased risks of bacterial seeding and subsequent infection.
In 2003 Moriera-Gonzalez et al. conducted a large study analyzing the clinical outcomes in long-term follow-up between autogenous bone, methylmethacrylate, and hydroxyapatite. Infection and implant exposure were the most common complications seen in those patients treated with methylmethacrylate and hydroxyapatite, and occurred in 13.3% and 22.4% of these cases respectively. In comparison, the rate of infection and exposure seen with autologous bone was significantly lower, at 7.1% and 1.3% respectively.
Titanium Mesh
Titanium is a commonly used material in the fixation of bony fractures and reconstructions, and is reasonably well tolerated by the body. Typically, for cranioplasty procedures, it is used in the form of a moldable mesh, which can be cut, bent, and fitted to cover the relevant defect. In this form it has been used successfully (particularly in conjunction with free tissue transfer for improved soft tissue coverage) for reconstruction of large frontocranial defects. It is, however, still a foreign substance, and thus prone to the complications inherent to such materials. Infection risk remains higher than that of autogenous bone, there is an ever-present risk of attenuation of the overlying native soft tissue envelope (especially in large reconstructions), and when used in context of irradiated tissue the results will be predictable and poor.
Polyetheretherketone (PEEK)
Polyetheretherketone (PEEK) is biocompatible, inert, and reported to have similar mechanical properties to bone. Importantly, it can be formed to precisely fit frontocranial defects preoperatively based off 3-dimensional CT scans. For these reasons PEEK has been growing in popularity, based on the arguments that these implants save operative time, prevent donor site morbidity, and result in improved aesthetic outcomes. While early results seem to indicate better outcomes relative to other alloplastic materials, clinical series are limited in scope (between 5 and 38 patients), and follow-up times are probably inadequate at this point (from 6 to 24 months) to provide an accurate representation of the potential for long-term success. There does appear to be an implant failure rate of up to 27% reported with PEEK, typically due to exposure and/or infection. A few direct comparison studies with PEEK cranioplasties have suggested a lower complication rate relative to autogenous bone, however these were small series with short follow-up times, and this was clearly not consistent with our experience.
Autogenous Nonvascularized Bone
Through our experience over the past 41 years, autogenous bone grafts are generally the most appropriate material with which to reconstruct the frontocranial region. Grafts can be readily harvested from split calvarium, split rib, or iliac crest cortical bone. The ability of these grafts to revascularize and consolidate after reconstruction allows them to become resistant to infection over the long term. While other published experiences vary in their quality and results, we have experienced zero graft failures as a result of infection or extrusion. The notion is commonly put forth that these nonvascularized grafts are prone to significant resorption, but again, this has not been the case in our experience.
The most comprehensive recent investigation to date regarding the use of autogenous bone for cranioplasties was published by Fearon et al. Their 14-year series of 96 patients had zero incidences of postoperative infections resulting in loss of the cranioplasty graft, all of which were performed with split calvarium. Only one patient experienced clinically significant graft resorption that required operative revision. Additionally, their extensive review of the literature concluded that alloplastic cranioplasty grafts demonstrated a nearly fivefold higher infection rate relative to autogenous bone grafts. They also noted that should infection occur with an autogenous graft, it can often be treated with drainage alone, as opposed to the near universal need to remove an alloplastic implant under similar circumstances.
Free Tissue Transfer
Rodriguez, and a number of other craniofacial microsurgeons, have used the fibula extensively to reconstruct limited frontal and zygomatic defects (the scapula has been used to a lesser degree as well), but there is no vascularized bone flap that can be used for the repair of a large defect. The latissimus flap is an excellent option to provide well-vascularized muscle capable of nourishing free bone grafts for reconstructing larger bony defects, and several fasciocutaneous perforator flaps have been used in this regard with good success as well. For patients with suspect soft tissue coverage, particularly the irradiated, free flaps must be used preliminarily in order to prepare the recipient site for the bone graft. This can also be performed concomitantly with a bone graft dependent upon the specific clinical scenario, however we have preferred to stage these procedures in order to allow the sometimes very significant swelling of the free flap to resolve prior to placement of the graft.
Case Examples
Case 1
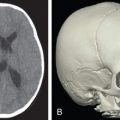
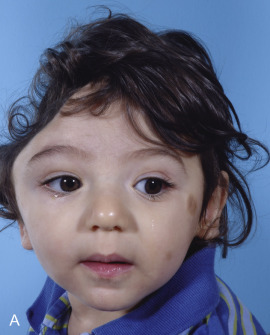
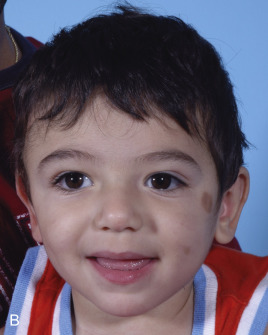
Just before his first birthday this boy was bitten by a Boxer dog and sustained a loss of most of his right parietal bone, dura, and a good bit of parietal lobe ( Fig. 3.1.1 ). Excellent neurosurgical care debrided nonvital brain and repaired the dura with an artificial dural substitute. Because of the lack of native dura, spontaneous regeneration of the bone was unlikely. Three months later, at 14 months of age, a switch cranioplasty was performed, taking the entire left parietal bone to replace what was missing on the right. This left the left side devoid of bone, but with healthy dura and pericranium. Several fragments of his skull, which had been saved and frozen from the original operation, along with a large segment of rBMP-2 impregnated in collagen sponge, were placed between the dura and the pericranium. At 2 years of age the boy had an intact skull and only a mild left hemiplegia.
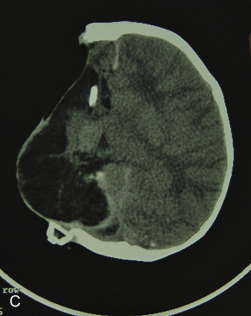
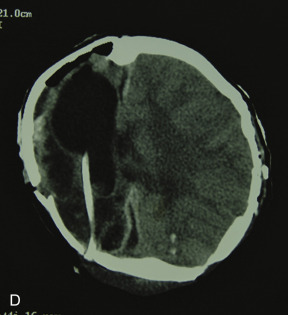
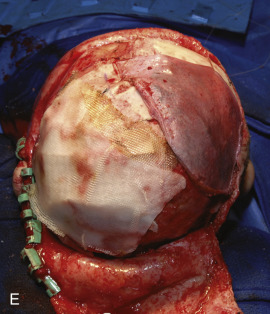
Case 2
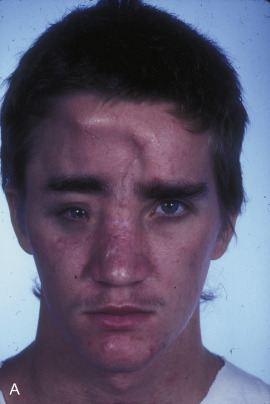
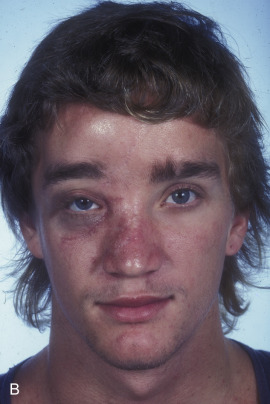
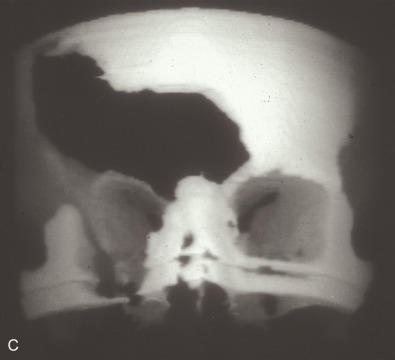
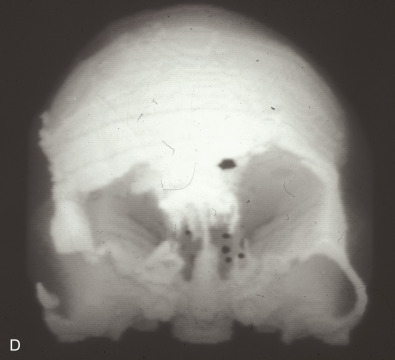
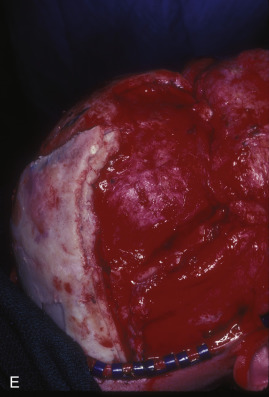
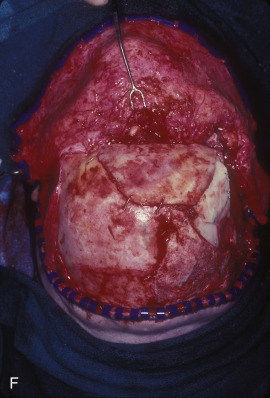
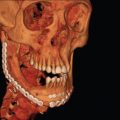
This 19-year-old male lost control of his bicycle on a wet bridge and was run over by a truck ( Fig. 3.1.2 ). After debridement of his compound right fronto-orbital defect, along with complete removal of the remnants of his frontal sinus (proper neurosurgical treatment), he was left with the defect shown, which was easily repaired with split calvarial bone from adjacent parietal bone.