Introduction
Burn-related injury to the trunk is common in both pediatric and adult populations. The prominent anatomical location of the breast and the nipple-areola complex (NAC) within the anterior trunk makes these structures vulnerable to all mechanisms of burn injury. Survival from large total body surface area (TBSA) burns has improved in modern times. The improvement in survival have led to increased long-term morbidity among burn survivors. The goals of acute and reconstructive surgery for breast and NAC burns are to preserve and restore functional and cosmetic appearance to the highest possible level. Of paramount importance during any acute or reconstructive procedure involving the breast and NAC is the preservation of as much viable tissue as possible and the prevention of injury to the underlying breast bud that is responsible for the growth of the breast mound that begins when the child begins puberty.
It is important to recognize that deep partial- and full-thickness burns that heal without surgery may develop long-term complications related to breast function and aesthetics. Superficial breast and NAC burns are unlikely to cause significant postburn functional or cosmetic deformities. However, deep partial- and full-thickness burns to the breast and NAC in pediatric patients can lead to significant functional and cosmetic deformities, including distress related to loss of femininity. In the pediatric female patient, breast and NAC burns can cause functional impairments related to mammary development and lactation, as well as cosmetic deformities related to scar hypertrophy and contracture, which can contribute to the displacement of the NAC, breast asymmetry, hypoplastic breast tissue, and/or amastia ( Fig. 62.1 ). The functional, cosmetic, and psychological effects of the burn injury may not become apparent for many years after the initial burn injury. Although both males and females sustain burn injuries to the breast and NAC, the treatment of the injury in the male patient is less complex.
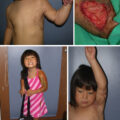
Postburn hypertrophic scarring of the left breast, anterior torso, left axilla, and left upper extremity in a pediatric, prepubescent female (left). The second image reflects postburn contractures of the neck and anterior torso with displacement of the left breast mound, nipple-areola complex, and inframammary fold (right).
Superficial partial-thickness burns to the anterior torso, breast, and NAC are often treated with local wound care alone and generally heal in 1 to 2 weeks. Small, deep second- and third-degree burn wounds to the breast can be treated with early excisional debridement and primary closure. Early excisional debridement and split-thickness skin grafting are recommended for larger surface areas and deep second- and third-degree burns to the breast ( Fig. 62.2 ). Burns to the trunk are not often immediately life threatening, except for respiratory compromise secondary to deep second- and third-degree circumferential burns that inhibit oxygenation and ventilation of the patient. Regardless of the size and depth of the burn injury, an emphasis is placed on promoting adequate pain control, nutritional support, and the prevention of infection by providing adequate local wound care and surgical excision when indicated. It should be noted that deep second- and third-degree burns to the NAC should be treated conservatively rather than by excisional debridement, as this structure can heal from the deep glandular breast bud, which is often spared. Breast contour deformities can also develop in the breast, regardless of the method of acute closure, and can be addressed during the reconstructive period. This chapter fully discusses the surgical management of deep second- and third-degree burns in the acute and reconstructive stages.
Early excision and autografting of deep second- and third-degree burns to the anterior torso. Also note that the severity of the anterior torso burns required tracheostomy to maintain a patent airway during the acute phase of the patient’s burn care and reconstruction.
Breast anatomy and sequelae of burn injury
Mature female breasts are specialized apocrine sweat glands that are responsible for lactogenesis. Each breast mound overlies the pectoralis major muscle of the anterior torso, as well as the upper portion of the rectus abdominus muscles inferiorly. The breast mound is secured in its medial aspect at the sternum and runs laterally, where it then inserts at the middle axillary line. The exterior surface of the mammary gland is covered with epidermis, including the nipple, areola, and general surfaces of the breast. It is important to remember that the breast is firmly fixed to the chest wall throughout the entire circumference of its perimeter. The underlying dermis of the breast is connected to a network of collagen and elastin fibers interwoven within the breast’s deeper fibroadipose and fibroglandular tissues to provide the general contour and shape of the breast within its overlying skin envelope. Of note, the ratio of fibroadipose tissue to fibroglandular tissue in breasts varies with age, body mass, hormonal status, and pregnancy status. Interconnected collagen and elastin pass from the dermis through the mammary tissues and secure the breast to the underlying superficial fascia of the anterior trunk muscles. ,
The glandular breast bud is a circular disk of tissue immediately posterior to the NAC responsible for the development of the breast under the influence of circulating hormones. The glandular tissues of the breast are organized into a series of lobules and ducts that connect to the NAC. The glandular breast bud in children is located 4 to 8 mm below the NAC; therefore it is relatively protected even in severe injury to the skin of the chest wall. The glandular ducts are lined with epithelial cells that can allow the NAC to regenerate the epidermis after severe injury if the glandular breast bud remains viable. McCauley et al., in a review of 28 pediatric female patients with chest wall burns, found that all patients developed breast tissue, even in the absence of NAC. Therefore clinical evidence of severe NAC injury, or complete absence of NAC after burn injury, does not necessarily equate to underlying glandular breast bud injury. In the pediatric and adult nonlactating breast, there is little distinction between the superficial fat plane immediately anterior to the breast bud and the glandular tissue of the breast bud itself. Iatrogenic injury to the glandular breast bud should be avoided. ,
Thelarche (or breast budding) is defined clinically as Tanner stage II. It represents the onset of the hormonal factors that cause the breast, NAC, and underlying fibroadipose and fibroglandular tissues to mature. Female breast development typically occurs between 11 and 15 years of age and is completed by 21 years of age. Breast skin is thinner in its superior and lateral quadrants (1.38 ± 0.24 mm) and thicker in the medial and inferior quadrants (1.97 ± 0.26 mm). In females, beginning in the mid-40s, the skin of the breast thins; the lateral and inferior quadrants thin the most with age, possibly because of decreased circulating estrogens during menopause. Breast maturation requires an unrestrictive skin envelope to allow expansion of the underlying breast tissue; therefore a prior burn injury can affect maturation at this stage. Scar contracture bands and deformation of the natural breast often occur during this period. Although lactation can still occur, hypertrophic scar contractures of the burnt breast often cause displacement of the NAC, which must be surgically corrected to achieve adequate function to facilitate breastfeeding, as well as general aesthetics of the breast. ,
Epidemiology
Significant improvements in burn survival have occurred over the last few decades and can be attributed to (1) implementation and increased adherence to standardized acute burn resuscitation protocols; (2) early excisional debridement and autografting of burn wounds; (3) improvements in the treatment of inhalational injuries and the prevention and treatment of multiorgan failure; (4) improved nutritional support, including modulation of the hypermetabolic and catabolic responses to burn injury; and (5) reduced frequency of large TBSA burns in recent years. Because of the decrease in mortality among those afflicted with devastating burn injuries, requests from patients to restore the functional and aesthetic components of their burn injuries have increased in modern times.
The trunk is the second-most common location for burn-related injury in both pediatric and adult populations after extremity burns. Breast and NAC burns are most commonly due to accidental pediatric scalds that occur in the domestic environment. The most common unintentional mechanism for pediatric scalds is related to the child accidentally pulling a container of hot water down onto their bodies, which has a characteristic splatter distribution of burn injuries that most commonly injure the face, bilateral upper extremities, and anterior torso. In a review of 704 pediatric patients treated in the emergency department over 6 years, Drago et al. demonstrated that 66% of burn injuries were due to scalds. Furthermore, Burvin et al. evaluated 421 female patients with breast burns over 3 years and found that of the 138 breast burns, 66% were secondary to scald injury. In this study, scalds were responsible for most first- to second-degree burns, whereas most second- to third-degree burn wounds occurred in those injured by cooking oil, fire, or flame injuries. Fire, flame, and cooking oil–related burns are more likely to occur in older children and adults; however, their mechanism of injury tends to cause a more serious burn injury. , Although flame burns are less common, their mechanism tends to cause deep second- and third-degree wounds that require excisional debridement and autografting to obtain wound closure. Regardless of the mechanism of the burn injury, deep second- and third-degree burns to the breast and NAC can injure the glandular breast bud, the mammary tissue responsible for normal breast development. McCauley et al., in a review of 28 pediatric female patients with chest wall burns, found that 71% of patients required surgical release of anterior torso contractures to facilitate breast maturation and development.
Acute management
Initial care of burns to the anterior torso, breast, and NAC begins with a global trauma assessment according to the Advanced Trauma Life Support guidelines established by the American College of Surgeons. Early prophylactic endotracheal intubation may be necessary for patients who undergo large-volume fluid resuscitation because of the potential for increased airway edema. One must remember that in determining the TBSA of a burn wound, the size of the breast can contribute a significant percentage that is not represented on the typical Lund and Browder chart; therefore, in patients with large burns to the anterior torso, the burn injury often underestimates the true percentage of TBSA of the overall burn injury. The underestimation of TBSA can reach 10% in those with large breasts, compared with 5% for males and 7% for females with a smaller breast size.
During large-volume crystalloid resuscitation, patient respiratory mechanics must be frequently reevaluated, especially in those patients with deep circumferential second- and third-degree burns to the torso, as these patients may require emergent thoracoabdominal escharotomies if ventilation becomes compromised. , During escharotomies of the anterior trunk, great care must be taken not to incise directly through mammary tissue. When performing an escharotomy on the anterior trunk, it is important to preserve as much viable tissue as possible and design escharotomy incisions in such a way that they do not negatively affect breast cosmesis and cause iatrogenic injury to the breast tissue, the breast bud, or the NAC. Even for those who do not require an anterior chest wall escharotomy during resuscitation, these patients can develop long-term restrictive disease related to postburn contracture.
Superficial second-degree burns to the anterior torso, breast, and NAC are treated with pain control, mechanical debridement of denuded epithelium, daily cleansing of the burn wound, and application of dressings—with or without topical antimicrobial agents. The epithelium regenerates from uninjured hair follicle remnants and generally heals in 1 to 2 weeks. During this period, an emphasis is placed on promoting adequate nutritional support to facilitate wound healing and infection prevention by providing adequate local wound care. It is important to recognize that second-degree burn wounds that heal without surgery may still develop long-term complications related to breast function and aesthetics.
The management of deeper second-degree burn wounds follows a similar algorithm; however, one must remember that deeper second- and third-degree burn wounds heal by secondary intention, a process of epithelization and contraction. A daily clinical evaluation of the burn wound is performed with the recommendation that any burn wound to the anterior torso undergo early excision and autografting if it is not expected to heal within 3 weeks. A large TBSA burn wound to the anterior chest with deep second- to third-degree burn wounds throughout must be treated with early excision and autografting, with preservation of as much viable tissue as possible, and with great care to avoid injury to the underlying breast bud in the pediatric patient. In the pediatric patient, if the glandular breast bud is spared, there will likely be normal parenchymal development of the breast in the future. , Some authors support the preservation of the cosmetic units of the breast during the debridement process followed by split-thickness autografting. Large sheets of narrowly meshed autograft (1:1 or 1.5:1) with the interstices closed compactly should be used to appear as if it were a sheet graft. In our experience, seams between grafts are best placed along Langer’s lines whenever possible to minimize future bands of contracture.
Once adequate healing is achieved for both second- and third-degree burns, the burn wound must undergo long-term surveillance, especially in the pediatric patient and those expected to reach childbearing age, as deep second- and third-degree burns to the breast may develop thick scar contractures that prevent the normal skin envelope from expanding as the breast matures. , , Patients should enroll in a scar management program that can facilitate close follow-up and initial treatment of healing burn injuries with the use of pressure garments and silicone therapy and frequent massage and moisturization of the healing burn wound to optimize scar maturation and prevent sequelae of burn injury to the anterior torso. The follow-up for pediatric patients is important as the reconstruction of any postburn deformity is typically delayed until thelarche or at least 1 year after the burn injury if significant contracture bands prevent normal breast maturation or NAC.
Postburn reconstruction and techniques
Current surgical procedures include a combination of contracture release with full- or split-thickness skin grafting, local tissue flaps, tissue expansion, autologous fat grafting, and rare occasions of pedicled or free-flap reconstruction. Given that one breast may be relatively uninjured, treatment may also include symmetrizing procedures, such as reduction mammoplasty or mastopexy, to address a more ptotic or unburned contralateral breast. Most importantly, treatment plans must be tailored to the unique breast deformity and may need to include a combination of modalities.
Scar contractures
The key to successfully reconstructing the burned breast is to replace all structures to their original anatomic position and fill the resulting defects with tissue. The “Reconstructive Ladder” concept is an appropriate framework for conceptualizing breast and/or NAC reconstruction after burn injury. This concept arranges reconstructive options in order of increasing complexity. The ladder, beginning with the least complex or “bottom rung” to the most complex, contains the following components:
-
■
No treatment
-
■
Skin graft
-
■
Tissue expansion
-
■
Skin substitutes
-
■
Local flap
-
■
Regional flap
-
■
Free flap
-
■
Transplant
A risk/benefit analysis must be undertaken by evaluating the proposed procedure and the potential for donor site morbidity or failure. It is important to recognize that the simplest reconstructive option may not be appropriate for the individual patient. For patients with complex contracture deformities or those who undergo staged reconstruction, a more complex reconstruction may be chosen if the perceived cosmetic and functional outcome will have benefits over a simpler procedure.
Scars may be modified in situ to improve contour, decrease hypertrophic scarring, and ameliorate contracture bands. Recent advances in burn scar care include the use of fractional CO 2 and pulsed dye lasers as an adjunct to traditional treatments, including pressure garments, silicone, and intralesional injection of high-potency steroids and/or fluorouracil to modify existing scars ( Fig. 62.3 ). , In many cases, adding these low-risk regimens can improve softness while decreasing contracture bands or hypertrophy to the point where the healed scar no longer requires excision and autografting, or more complex adjacent tissue transfer procedures.
Postburn intramammary scarring in a prepubescent female (left). Softening of the contracture bands are noted after fractional CO 2 laser and intralesional Kenalog therapies (right).
Scar contractures resulting from severe burn injuries to the breast can be a challenge for both the patient and the surgeon. Severe burns negatively affect the patient’s sense of attractiveness and quality of life and contribute to lower self-esteem. , The precise timing of reconstruction can be challenging to decide in the case of burn injuries to the breast, especially in cases of young female patients who have not yet reached adolescence. To minimize overtreatment, adult patients should wait for scar maturation (typically 6–12 months). If the contracture is severe and the symptoms are significant, it may be necessary to release the contracture before full maturation. For patients who have not yet reached puberty, most authors advocate waiting until the first signs of breast development and operating once the contracture of breast tissue significantly impairs normal breast development. ,
Once a decision is made to treat a symptomatic contracture, an assessment should be made of the type and location of the contracture. Some authors have proposed a classification system for postburn breast deformities. We have modified this excellent classification to account for the fact that many of these patients require not only the release of the inframammary fold (IMF) but also the release of the lateral fold, medial fold, or even the entire breast circumference ( Table 62.1 ). Once the contracture has been classified, a treatment strategy can be made based on the donor sites available. Reconstruction of the burned breast can be a multistage process. Therefore the patient’s priorities must match the treatment plan the surgeon believes is feasible. As always, longitudinal and multidisciplinary care is important in burn care.
Table 62.1
Modified Classification System of Postburn Breast Deformities
| Location | Unilateral |
| Bilateral | |
| Extent | Total |
| Subtotal | |
| Anatomical | Breast mound |
| Nipple-areola complex | |
| Inframammary fold | |
| Deformity | Contracture—intrinsic/extrinsic |
| Hypoplasia | |
| Aplasia | |
| Symmetry | |
| Releases | Inframammary fold |
| Interbreast (webbing or synmastia) | |
| Lateral mammary fold | |
| Medial mammary fold | |
| Circumferential | |
| Lateral, superior, or inferior displacement |
Breast asymmetry
Breast asymmetry is a common complication of chest burns in female patients. Treatment of these contractures with release and grafting, local flaps, or tissue expansion can reduce these differences. If one of the breasts is spared from burn injury, symmetrizing procedures are often required. As with radiation injuries, thermal burn injury can result in tightening of the skin on the affected side. Macromastia and breast ptosis, common diagnoses in both burned and unburned patients, can exacerbate these asymmetries and subsequently require reduction mammoplasty or mastopexy on the uninjured side ( Fig. 62.4 ). , In the case of symptomatic macromastia of the burned breast, reduction mammoplasty may be used safely. Previous authors have suggested that even burn-injured skin can be used as a pedicle for the NAC if the tissue is carefully deepithelialized and the subdermal plexus is maintained. In our experience, maintaining thick medial and lateral flaps of at least 2 to 3 cm ensures adequate blood supply to injured tissue. In many cases, after the scars of the burned breast are released, the burned area contains almost the same tissue volume as the nonburned contralateral side.