Abstract
Posttraumatic nasal deformity is a complex problem that requires astute preoperative assessment and nasal analysis. A keen knowledge of the normal nasal anatomy and physiology is required to recognize abnormalities and to develop a treatment plan for each individual patient that appropriately addresses both cosmetic and functional concerns. The intraoperative techniques and maneuvers are many and vary according to the problem at hand. Following surgical treatment, an understanding of the postoperative healing process will help to increase patient understanding and satisfaction during recovery.
Keywords
rhinoplasty, nasal trauma, posttraumatic nasal deformity, facial plastic surgery, trauma
Background
Nasal bone fractures are the most common type of facial fracture, and the third most common fracture of the human skeleton. Nasal trauma is often the result of motor vehicle collisions, sports-related injuries, altercations, and falls. The annual incidence has been estimated to be 53/100,000 in the United States, with the incidence of post-traumatic nasal deformity ranging from 14% to 50% if such fractures are left untreated. Immediate fracture reduction in the acute setting can reduce the incidence of posttraumatic nasal deformity, but does not eliminate the risk entirely.
Nasal deformity following trauma is one of the most common reasons that patients seek evaluation by a rhinoplasty surgeon. Depending on the type of deformity, concerns may be aesthetic, functional, or a combination of the two. Surgical correction of the complex acquired deformities that occur after trauma requires a keen understanding of nasal anatomy and physiology and honed skills of nasal analysis and physical examination. Two of the most challenging problems to address are crooked nose and saddle nose deformities. These deformities often result in both cosmetic irregularities and nasal obstruction, which should be addressed simultaneously as a unified problem.
Surgical Anatomy
Normal Nasal Anatomy
When discussing nasal anatomy ( Fig. 3.6.1 ), the nose is typically divided into thirds. The upper third consists of the paired nasal bones and bony septum. The nasal bones articulate with the frontal bones superiorly, frontal processes of the maxilla laterally, perpendicular plate of the ethmoid medially, and upper lateral cartilages inferiorly. The nasal bones are thickest superiorly and become thinner inferiorly.
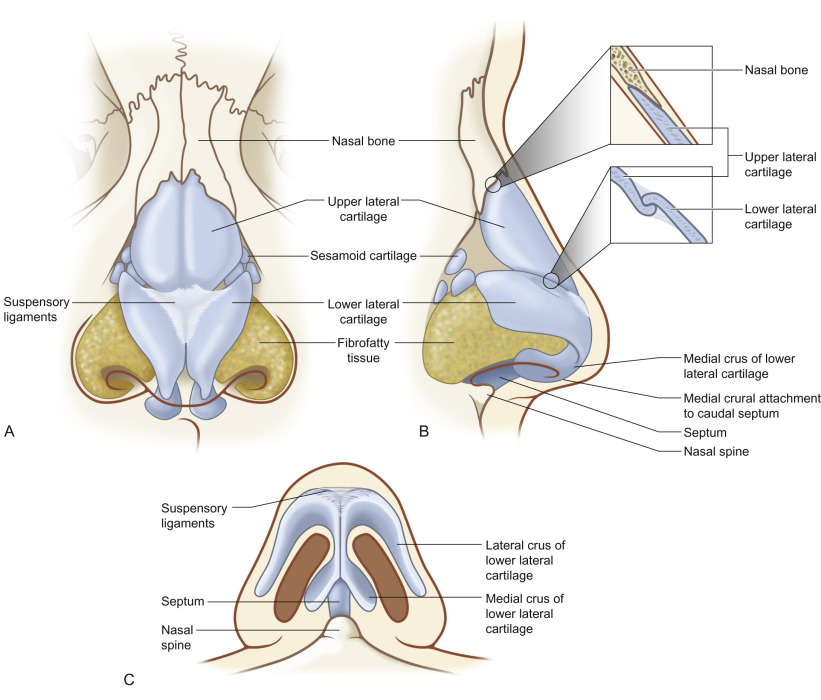
The middle third of the nose is composed of the upper lateral cartilages and the dorsal cartilaginous nasal septum. The upper lateral cartilages are fused with the nasal bones superiorly, dorsal cartilaginous septum medially, and lower lateral cartilages inferiorly. Externally, the shape of the middle vault plays a critical role in shaping the nasal dorsal aesthetic lines. Endonasally, the middle vault defines the internal nasal valve, which represents the narrowest portion of the nasal airway and the site of highest airflow resistance. The internal nasal valve is formed by the caudal edge of the upper lateral cartilage laterally, cartilaginous nasal septum medially, and head of the inferior turbinate posteriorly.
The lower third of the nose comprises the paired lower lateral cartilages, caudal septum, and bony nasal spine. Attachments of the lower lateral cartilages to the upper lateral cartilages in the scroll region and to the caudal septum and the strength of the lower lateral cartilages themselves are major determinants of tip support. Additionally, the position of the caudal septum relative to the nasal spine and the shape of the caudal septum itself play a key role in determining the shape and position of the lower third of the nose.
Crooked Nose
Asymmetry of the upper third of the nose results from fractures of the nasal bones with or without fracture of the bony septum. As deflections of the bony pyramid can be highly variable, it is important to determine the site of nasal bone fractures, contour of the nasal bones, and involvement of the bony septum. In simple cases, a single nasal bone is displaced medially by direct trauma. However, bilateral nasal bone fractures with involvement of the bony septum and subsequent deviation to one side is often the case.
Fractures of the bony pyramid are often accompanied by deviation of the middle third of the nose. Deviation to one side as a result of fractures of the bony pyramid often cause deviation of the cartilaginous septum to the same side superiorly, resulting in a “C-shaped” deformity ( Fig. 3.6.2 ). However, deformity of the middle vault can be seen without abnormality of the bony pyramid. Isolated cartilaginous septal involvement will result in deviation inferior to the nasal bones. If trauma results in disruption of the attachments of the upper lateral cartilage to the dorsal septum or caudal nasal bone, depression of the middle vault on that side will occur over time. If the attachments of upper lateral cartilages to the nasal bones in the keystone area are disrupted bilaterally, the upper lateral cartilages may become depressed over time, resulting in external visibility of the caudal aspect of the nasal bones (inverted-V deformity or saddle nose).
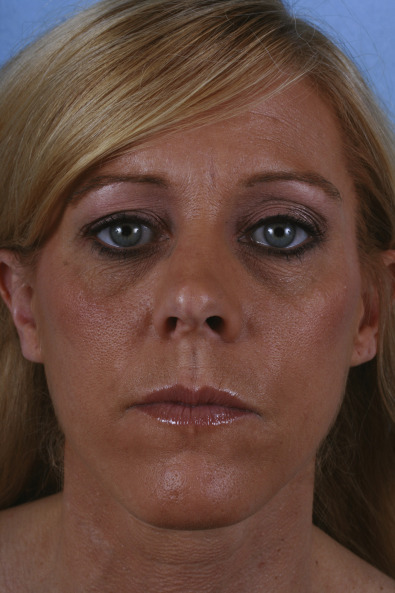
Post-traumatic deformity of the lower third of the nose often results from caudal septal fracture with subsequent deviation of the nasal tip to one side. Additionally, traumatic displacement of the caudal septum from the nasal spine results in potentially more severe tip deviation. An “S-shaped” deformity results from tip deviation to one side with contralateral deviation of the nasal bones and can result in significant cosmetic irregularity and nasal obstruction ( Fig. 3.6.3 ). This scenario is often associated with a high septal deviation, which can be challenging to repair.

Saddle Nose
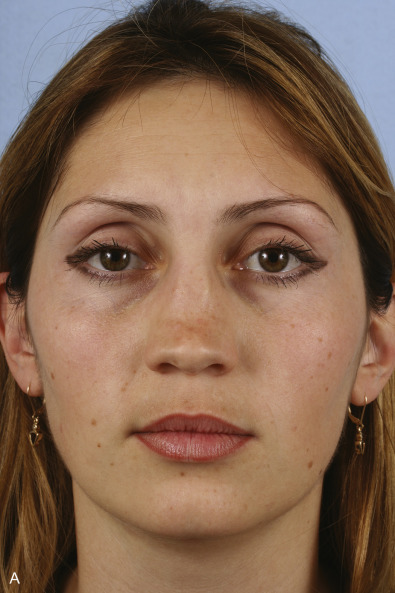
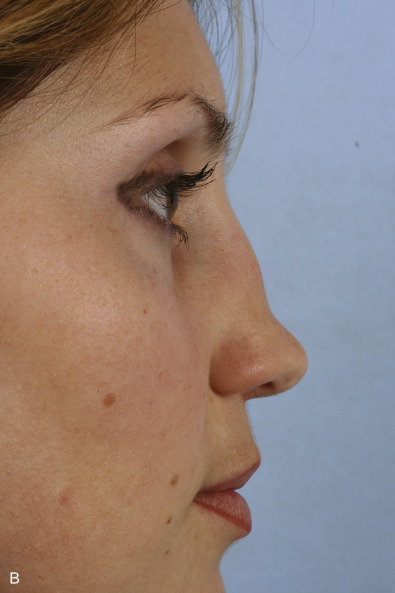
Saddle nose deformity results from the loss of integrity of the cartilaginous septum and results in loss of dorsal height and a scooped-out appearance ( Fig. 3.6.4 ). Following trauma, a saddle nose may develop from an untreated septal hematoma leading to infection and subsequent necrosis of the cartilaginous septum or from direct fracture of the septum. Various features may accompany the loss of dorsal height and include shortened vertical length, loss of tip support, tip overrotation, and columellar retrusion. The appearance and symptoms may be mild with a minimal supratip depression and slight widening of the nose to severe with complete loss of cartilaginous septal support, flattening of the nose, and nasal obstruction.
Clinical Presentation
History
A comprehensive history should include details of the timing and mechanism of injury and determination of the magnitude and vector of the traumatic force. High-velocity trauma resulting from motor vehicle collisions or similar mechanisms often causes significant comminution and septal injury, whereas low-velocity trauma resulting from personal assault and sports-related injuries often leads to less comminution and nasal deviation to one side. Cosmetic deformity and changes in breathing resulting from the injury must be evaluated in the context of preexisting aesthetic abnormalities and nasal obstruction. Preinjury photographs are helpful in establishing a baseline. The patient’s concerns regarding the appearance of the nose and patency of the nasal airway must be elicited to clearly establish goals of treatment.
Physical Examination
Determination of the anatomical cause of external deviation of the nose following trauma requires careful nasal analysis. In all cases, external examination should be accompanied by thorough endonasal examination. Determination of the nature and severity of nasal obstruction or subjective changes in nasal breathing are vital.
On inspection of the frontal view, symmetry and width of each third should be evaluated to elucidate any abnormalities of the bony pyramid, middle vault, and nasal tip. The brow–nasal tip aesthetic lines as determined by shadowing and transitions from the medial orbital rims, nasal root, middle vault, and nasal tip should be symmetric and smooth. On the lateral view, projection of the radix, bony dorsum, cartilaginous dorsum, and tip should be evaluated. The profile should be smooth with adequate relative projection at each level and appropriate rotation of the nasal tip. On the base view, columellar position and orientation, tip projection, and nostril symmetry should be evaluated. Any asymmetries or deviations should be noted and further evaluated.
Following inspection, careful palpation is required. Palpation of the nasal bones may reveal subtle bony step-offs or depressions even if not visible on inspection. Middle vault palpation may reveal loss of support or deficiency of the cartilaginous septum, separation of the cephalic edge of the upper lateral cartilages from the nasal bones, or asymmetric recoil, position, or strength of the upper lateral cartilages themselves. Downward and lateral pressure on the nasal tip can provide information on tip support and status of the relationship between the caudal septum and lower lateral cartilages.
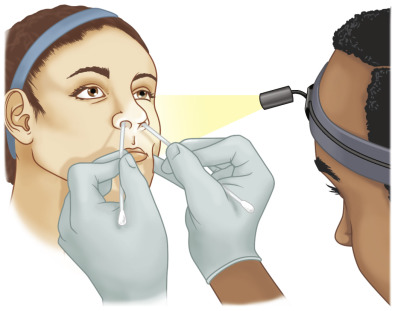
Endonasal and airway evaluation should include examination of the entirety of the nasal septum and static and dynamic evaluation of the external and internal nasal valves. Examination should be performed first without the use of topical decongestant and then performed a second time following adequate decongestion with a topical agent, such as oxymetazoline. Initially, the external nasal valves, which are formed by the columella, nasal floor, and nasal alar rim, should be evaluated for integrity. Movement and collapse at the level of the external valve should be evaluated during restful breathing and forced nasal inspiration. Function of the dilator naris muscle, which dilates the nasal vestibule, should also be evaluated. The internal nasal valves are then inspected using a nasal speculum for an appropriate valve angle of 10–15 degrees and stability during comfortable breathing and forced inspiration. A modified Cottle maneuver can then be performed to further evaluate support at the external and internal nasal valves ( Fig. 3.6.5 ). During the maneuver, a ring curette or other narrow instrument is used to support and/or elevate the lateral nasal wall at the level of the internal and external nasal valves to see if this prevents collapse and improves subjective breathing. An improvement with this maneuver may indicate amenability to surgical correction at the corresponding location. Following valve examination, a nasal speculum allows direct inspection of the anterior septum and potentially the posterior septum. If visualization of the posterior septum is difficult, a 0- or 30-degree endoscope can aid in septal examination. Any deviations or evidence of mucosal lacerations, which may indicate the site of septal fracture, should be noted. Additionally, the size and position of the inferior turbinates should be inspected as they can have a profound impact on patency of the nasal airway.
Photographic Documentation
High-quality photographic documentation should be performed for all patients seen for functional or cosmetic rhinoplasty consultation. Photographs are invaluable for preoperative surgical planning and patient discussion, intraoperative reference, and postoperative comparison. Standard photographic views for rhinoplasty surgery photos include frontal, base, “skyline,” bilateral oblique, and bilateral profile views ( Fig. 3.6.6 ). The “skyline” view of the dorsum is particularly valuable for visualizing the alignment of all three portions of the nose. A digital single-lens-reflex camera with a resolution of at least 1.5 megapixels is recommended. A camera lens with a focal length of 90–105 mm with macro capability is needed to minimize distortion and provide an adequate depth of field for the entire face to be in focus. Ideal lighting should be provided by two lights of equal intensity positioned at 45 degrees from the subject–camera axis to prevent shadowing and uneven lighting. A plain background devoid of shiny material or creases should be used. In terms of color, an electrochromic blue background is preferred for facial medical photography. A distance of 12–18 inches between the subject and background should be maintained to minimize shadowing by the subject on the background.




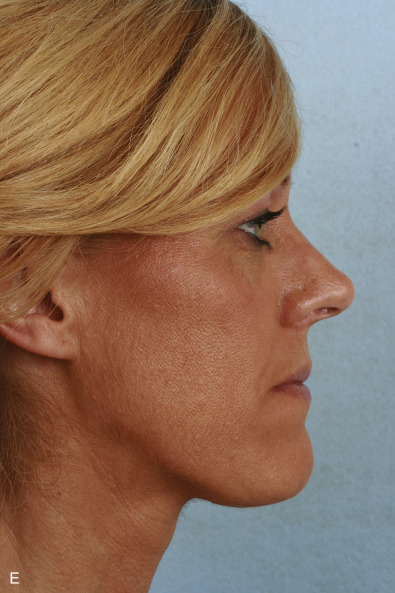
Radiological Evaluation
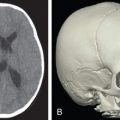
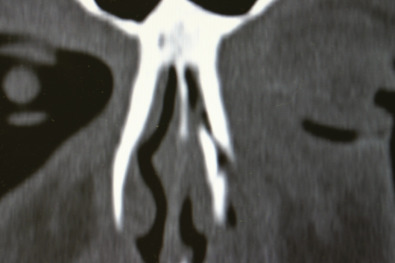
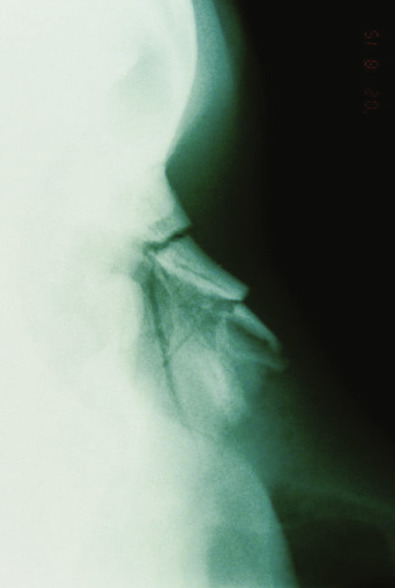
Computed tomography (CT; Fig. 3.6.7 ) may be useful in the acute setting to evaluate the nature and severity of facial fractures following severe trauma, but the majority of patients who subsequently follow up for correction of posttraumatic nasal deformity do not require imaging. However, if concomitant bony facial injuries are suspected, such as an untreated naso-orbital-ethmoid complex fracture, a CT scan can be considered. Plain radiographs taken at the time of trauma may provide information on the nature of nasal injury ( Fig. 3.6.8 ), but are often of limited value in the acute setting or upon planning for corrective surgery.
Surgical Techniques
Approach
The choice of surgical approach depends upon the type and complexity of the deformity to be addressed and experience of the surgeon. An endonasal approach may be preferred in patients requiring modest profile reduction, conservative tip management, or other minor modifications. Advantages of the endonasal approach include less tissue dissection, less postoperative edema, and more rapid postoperative healing; however, by its very nature the endonasal approach affords inferior visualization compared to the external or open approach. Indications for an open rhinoplasty approach include asymmetric nasal tip or middle vault, saddle nose deformity, and other complex nasal deformities requiring significant grafting or modification. Advantages of the open approach include excellent exposure allowing for precise tissue manipulation, suturing, and grafting. Disadvantages include an external transcolumellar incision, greater field of dissection that may disrupt some of the inherent nasal support mechanisms, and greater postoperative edema. In general, procedures that do not involve complex tip changes or grafting can be performed with endonasal approaches. When middle vault grafting or tip changes are necessary, an open approach offers distinct advantages.
Graft Material
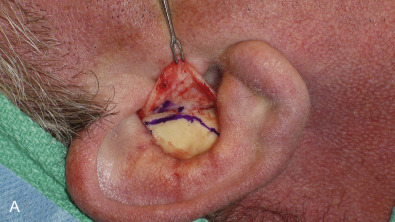
Surgical correction of nasal deformities often requires the use of grafting material. Autologous cartilage is the gold standard in rhinoplasty due to its effectiveness, similar biomechanical characteristics to the native nasal framework, and long-term safety profile. The primary sources for autologous cartilage grafts include septal, auricular, and costal cartilage. Septal cartilage is the preferred material for most rhinoplasty surgeons and is typically available in adequate quantity and quality unless the patient has a history of severe septal trauma or previous septoplasty ( Fig. 3.6.9 ). It can be easily harvested from the same surgical site through an endonasal or open approach, is generally straight, and provides strong structural support. It is highly versatile and typical uses include dorsal onlay, columellar strut, caudal septal extension, lateral crural strut, alar batten, alar rim, spreader, and tip grafts. Auricular cartilage is the second most commonly used graft in nasal surgery. It is more pliable and less rigid than septal cartilage, making it less ideal for (but not precluding) structural grafting, and is an excellent choice for most nonstructural applications when septal cartilage is inadequate or unavailable. A significant amount of the conchal bowl can be harvested en bloc without cosmetic deformity through an anterior or posterior approach with minimal donor site morbidity ( Fig. 3.6.10 ). When a significant amount of grafting material is required or when septal and auricular cartilage are unavailable or inadequate, costal cartilage can be harvested. Costal cartilage is strong, abundant, durable, and pliable and can be easily sliced, carved, and fashioned into essentially any graft. It is particularly useful when significant dorsal grafting or restoration of nasal structural integrity is required ( Fig. 3.6.11 ). Postoperative pain can be significant in some patients and there exists a risk of pneumothorax, although this risk is minimal if performed by an experienced surgeon. Crushed cartilage is an attractive option to conceal contour deformities and soften transition zones. Septal cartilage works best in this regard and can be lightly crushed without significant cellular loss. Diced cartilage wrapped in oxidized regenerated cellulose (Surgicel, Johnson & Johnson Medical, New Brunswick, NJ) or autologous fascia (typically the superficial layer of the deep temporal fascia) has been popularized in recent years and is an excellent tool to augment the dorsum and other areas of the nose while providing a smooth contour that is free of palpable edges.